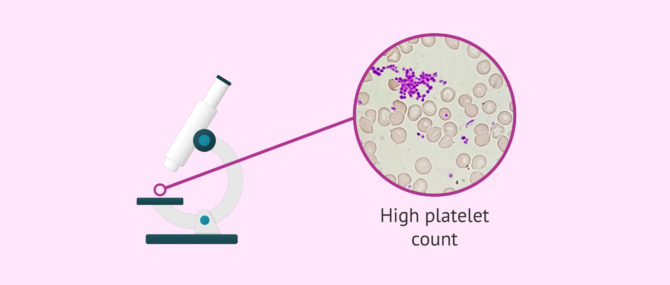
Essential thrombocythemia is a pathology included in the Myeloproliferative Syndrome (MPS) that presents with thrombocytosis (high number of platelets in blood) and hyperplasia of mature megakaryocytes in bone marrow. This is the most common PMS, with thrombocythemia occurring in 2 to 3 persons per 100,000 population per year.
Normally, values above 600,000 platelets/ml usually determine the diagnosis, although currently this limit has been lowered to 400,000 platelets/ml.
Although thrombocythemia is a more frequent alteration in middle-aged people, there are 15-20% of patients under 40 years of age and there is even a second peak of incidence in patients around 30 years of age, predominantly in women. For this reason, the effect that the disease may have on pregnancy is being studied.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 2.
- 3.
- 4.
- 4.1.
- 5.
- 6.
- 6.1.
- 6.2.
- 7.
- 8.
What symptoms does essential thrombocythemia cause?
Essential thrombocythemia is a hematological pathology characterized by elevated platelet levels, which leads to an increased predisposition to thrombosis or blood hemorrhages.
At the onset of the disease, patients usually have no symptoms. However, as the number of platelets in the blood increases, people begin to show symptoms of essential thrombocythemia. These include the following:
- Functional and transient microcirculation disorders (vasomotor disorders).
- Thrombotic complications.
- Hemorrhagic symptoms.
In addition, thrombocythemia often leads to an enlarged spleen, known as splenomegaly. Generally, one of the symptoms predominates, although two complications may also occur at the same time or sequentially.
However, only a small proportion of patients suffer serious, life-threatening complications.
There is no correlation between the occurrence of hemostatic complications and the degree of thrombocytosis. In fact, there are patients with platelet levels close to normal who show more or less severe thrombohemorrhagic complications.
Other symptoms of thrombocythemia
Although the clinical manifestations mentioned above are the most common, thrombocythemia can also cause other signs. Some of them are listed below:
- Weakness.
- Headaches.
- Skin burning.
- Tingling.
- Redness of the hands and feet.
However, many patients suffering from essential thrombocythemia are asymptomatic and are aware that they have this alteration in the number of platelets through a blood test or a medical check-up for any other pathology.
Why does essential thrombocythemia occur?
One of the possible causes of essential thrombocythemia are mutations in genes such as JAK2. It is a gene that encodes proteins responsible for the growth and division of blood cells, especially platelets.
Another gene whose mutation is associated with this blood disorder is CARL. This gene is involved in the functioning of the immune system and helps to heal wounds. However, the mechanism by which genetic changes would cause an increase of platelets in the blood is not known.
Although the most frequent causes of thrombocythemia are mutations in the genes, it is not an inherited disorder. Normally, thrombocythemia occurs due to somatic mutations, i.e. changes in the blood cell-forming cells after conception.
Diagnosis
The basic diagnostic test to detect essential thrombocythemia is a blood test where a platelet count is performed. In addition, ferritin, folic acid, uricemia and vitamin B12 levels will be determined.
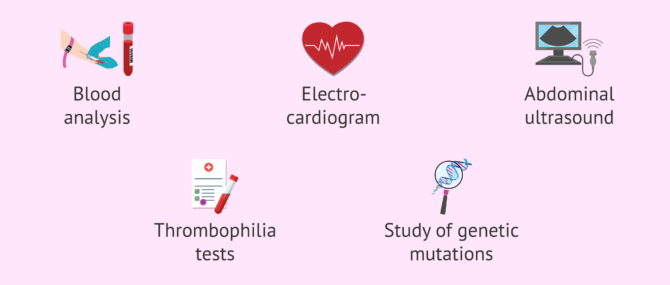
Other complementary tests that help in the diagnosis of essential thrombocythemia are:
- Electrocardiogram.
- Abdominal ultrasound.
- Biopsy and bone marrow aspiration.
- Tests for thrombophilias.
- Study of genetic mutations.
Although the bone marrow study is one of the additional tests, it is not essential for the diagnosis of essential thrombocythemia. However, it is quite common to do so to confirm the diagnosis of essential thrombocythemia.
Treatment
The main objective of treatments for essential thrombocythemia is to maintain the platelet count in the normal range, i.e. below 400,000 platelets/ml. Once treatment is started, it should be maintained for a period of time until platelet levels are reduced. Among the most commonly used treatments for thrombocythemia are the following:
- Hydroxyurea
- is a myelosuppressive drug, i.e. it blocks the production of red blood cells
- Anagrelide
- its trade name is Agrylin and effectively lowers platelet levels. This drug is usually used in cases where hydroxyurea has not been effective.
- Interferon
- although this type of drug is not one of the most widely used due to its adverse effects. However, interferon is safe in pregnant women with high platelet levels.
- Aspirin
- low doses of aspirin help to thin the blood, which reduces the formation of blood clots.
As an alternative to these medications and in emergency situations, the specialist may recommend apheresis or plateletpheresis. This is a procedure in which platelet levels are very rapidly reduced by drawing the patient's blood and passing it through a machine that separates the platelets. The blood without the platelets is then returned to the body.
Tips for essential thrombocythemia
One of the general recommendations of specialists for people suffering from high platelet levels is to take aspirin on a regular basis. However, there are other home remedies that improve essential thrombocythemia.
For example, it is important to follow a healthy lifestyle to avoid disorders such as diabetes or high blood pressure that would increase the risk of clot formation. In addition, eat a varied diet and avoid trans fats.
It is also advisable to exercise or walk for half an hour every day, as well as to stop smoking.
How does it affect pregnancy?
There are cases in which the diagnosis was known before pregnancy and other patients who discover their condition after routine pregnancy blood tests.
Pregnancy in itself does not pose an added danger to essential thrombocythemia, since when the disease affects young women, its development is usually benign. Although pregnancy does not aggravate or adversely affect the disease, there is an opposite risk, i.e. pregnancy does adversely affect essential thrombocythemia.
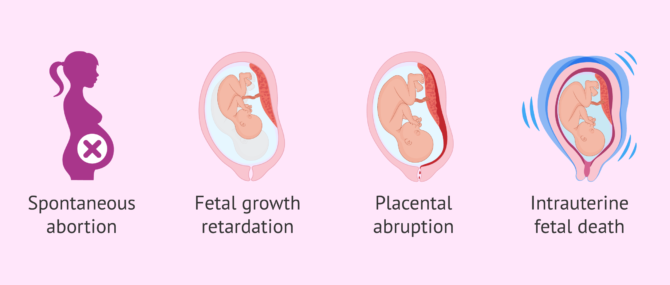
Thrombocythemia during pregnancy is associated with thrombosis of the placental vessels and can lead to multiple infarctions and secondary placental insufficiency. The latter carries a risk of first trimester miscarriage. In addition, the risk of fetal growth retardation may be increased.
Other consequences during pregnancy associated with this pathology are placental abruption, preeclampia or intrauterine fetal death.
It is important to note that, as with symptoms, there is no direct correlation between the consequences of the pathology on the pregnancy and the value of the mother's platelets.
FAQs from users
What are the possible complications of thrombocythemia?
When platelet levels in the bloodstream are too high and proper treatment is not carried out in time, acute leukemia or heavy bleeding may develop.
In addition, other possible complications of thrombocythemia include stroke, heart attacks or the formation of blood clots.
Are all cases of recurrent miscarriages due to coagulation problems?
No. Repeated miscarriages can have different reasons and it is thought that one of them could be thrombophilias or blood clotting problems.
This is why many specialists recommend specific tests in case there could be a link. However, conclusions about this association are limited.
We make a great effort to provide you with the highest quality information.
🙏 Please share this article if you liked it. 💜💜 You help us continue!
References
Ayalew Tefferi, Tiziano Barbui. Polycythemia vera and essential thrombocythemia: 2021 update on diagnosis, risk-stratification and management. Am J Hematol. 2020 Dec;95(12):1599-1613. doi: 10.1002/ajh.26008. Epub 2020 Oct 23 (View)
Maria Caterina Putti, Irene Bertozzi, Maria Luigia Randi. Essential Thrombocythemia in Children and Adolescents. Cancers (Basel). 2021 Dec 6;13(23):6147. doi: 10.3390/cancers13236147 (View)
Spivak JL, Silver RT. The revised World Health Organization diagnostic criteria for polycythemia vera, essential thrombocytosis, and primary myelofibrosis: an alternative proposal. Blood. 2008 Jul 15;112(2):231-9 (View)
Vannucchi AM, Guglielmelli P, Tefferi A. Polycythemia vera and essential thrombocythemia: algorithmic approach. Curr Opin Hematol. 2018 Mar;25(2):112-119 (View)
FAQs from users: 'What are the possible complications of thrombocythemia?' and 'Are all cases of recurrent miscarriages due to coagulation problems?'.





I don’t think you could’ve explained it better! I know about ET very well, since I was diagnosed with it a year ago after having 3 miscarriages. Later, I started a treatment to fight against ET and now I’m pregnant! 😀 But it’s very surprising that I didn’t experience any symptom of ET until very late… Has anybody experienced this too? Have a nice day!