Male infertility plays a very important role in the sterile couple. When problems arise in getting pregnant, around 30% of them are due to a male factor.
A sterile man usually presents with low semen quality in most cases. This which means that their sperm are not able to fertilize the egg which would result in a pregnancy.
Depending on the cause of this male sterility, it can be possible to find a specific treatment to allow these couples to become parents.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 1.3.
- 1.4.
- 2.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 4.7.
- 4.8.
- 5.
- 6.
- 7.
- 8.
Reasons for infertility in males
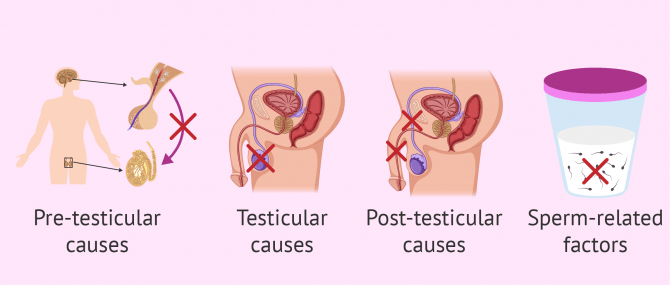
Male sterility can be caused by a series of factors that we can classify into four groups:
- Pre-testicular or endocrine factor: hormone imbalances affecting the development and/or testicular function.
- Testicular factor: direct involvement of the testicles.
- Post-testicular factor: problems with the ejection of sperm.
- Sperm abnormalities: issues directly linked to the quality of the sperm produced.
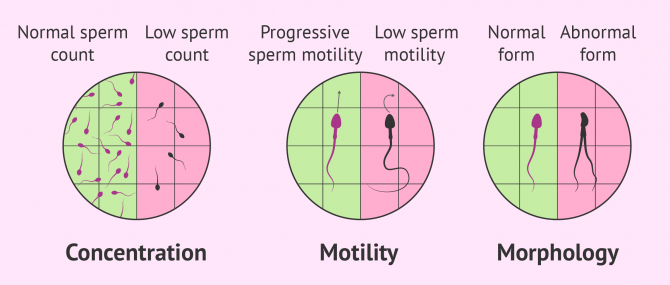
Despite the wide range of causes leading to male sterility, the quality of the ejaculated sperm is affected to some extent in each case. For a semen sample to be considered to be of good quality, it should meet certain parameters. These include sperm concentration, sperm motility, sperm morphology, and sperm vitality.
In order to diagnose the possible cause of male sterility, it is necessary to perform some diagnostic tests, starting with a spermogram. If you would like more information about this, we recommend visiting following page: Male Fertility Testing.
Below, we discuss the different types of male infertility in more detail:
Pre-testicular or endocrine causes
This type of male infertility is caused by problems with the hormonal regulation of the spermatogenesis, in other words, the sperm production.
The hormones secreted by the pituitary gland, LH and FSH, which act on the male reproductive function, may be altered for any of the following reasons:
- Unhealthy lifestyle habits
- Diabetes
- Hypothyroidism and hyperthyroidism
- Hypogonadism hypogonadotropic
- Hyperprolactinemia
These alterations can be due to congenital problems or be caused by external factors such as some substances or drugs (e.g. the use of anabolic steroids), which can affect the entire hormonal regulation system, causing fertility problems.
You can learn more about this subject reading this post: Pre-testicular causes of male infertility.
Testicular causes
When we mention testicular causes of male infertility, we refer to any factor affecting directly the testes.
Male infertility due to a testicular factor can be congenital or acquired, that is, caused by external agents at any point in the patient's life:
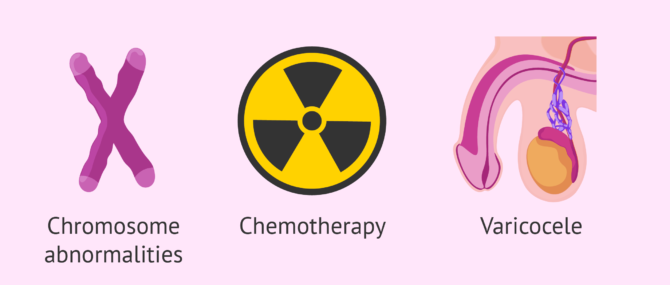
- Congenital anomalies or abnormalities
- caused by genetic alteration the chromosomal level (i.e. the Klinefelter Syndrome), or a faulty gene, for example in Noonan syndrome. Diseases can also be caused by defects in the genes of the male Y chromosome.
- Acquired disorders
- In this group, we find those problems caused as side effects or adverse reaction of certain drugs, e.g. chemotherapy, drug use, radiotherapy, trauma, infections, etc. The most known pathologies are varicocele, cryptorchidism, orchitis and hydrocele.
If you are interested in more detailed information on this subject, we invite you to continue reading here: Testicular Disorders & Infertility.
Post-testicular causes
The post-testicular causes of male infertility are a set of complications derived either from a blockage or an abnormality in the seminal ducts.
The seminal ducts consist of the epididymis, the vas deferens and the urethra, which the sperm must travel through once they have been produced in the testicles.
There are various causes of obstruction, such as infections, trauma, antisperm antibodies, hypospadias or cystic fibrosis.
The inability to ejaculate is also considered a post-testicular alteration.
If you are interested in this topic, you can read on in the following article: Post-Testicular Factors of Male Infertility.
Sperm abnormalities
Sperm abnormalities are the leading cuase of male infertility. This includes alterations in the sperm that directly affect their morphology, motility, vitality, or number.
In order to evaulate sperm quality, the diagnostic test of choice is a a semen analysis. A sperm analysis allows the specialist to determine the presence of the following alterations:
- Oligospermia or oligozoospermia
- low sperm count.
- Asthenozoospermia
- poor sperm motility.
- Teratospermia or teratozoospermia
- large amount of sperm with an abnormal morphology.
- Necrospermia or necrozoospermia
- large amount of dead sperm in the ejaculate.
- Azoospermia
- zero sperm count.
You can find information about Each of these spermatozoan abnormalities in this article: can List of Sperm Disorders that Cause Male Infertility.
Symptoms of male infertility
In most cases, the man will not experience any obvious signs of infertility. In almost all cases, the only sign of male infertility is the inability to conceive a child after one year of trying to conceive.
However, if the man has already been diagnosed with another disease such as hypogonadism, he may already suspect that he will have difficulty having children.
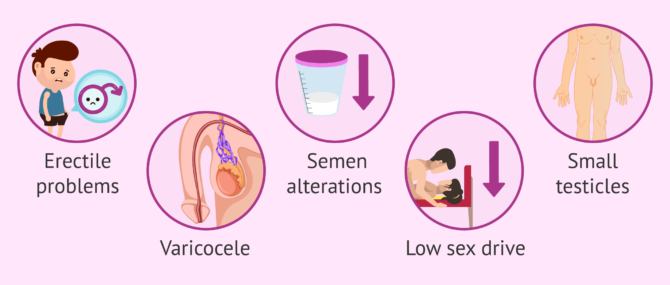
Other signs and symptoms commonly associated with male infertility include:
- Low libido and erection problems.
- Altered semen with an abnormal color, strong odor, very watery, very thick, etc.
- Smaller than normal testicles.
- Changes in voice, hair loss or decreased muscle mass that indicate possible hormonal changes.
- Alterations in the urine or pain when urinating that alerts of a possible infection.
- Appearance of varicose veins in the testicles.
If these symptoms appear when trying for pregnancy, the man should have a study with the necessary tests to confirm whether it is a case of male infertility.
What is the treatment
To deal with male infertility, we need to know the cause that is preventing pregnancy occuring. In some cases, it is possible to recover male fertility after pharmacological treatment or surgery. In the most severe cases, the only option will be assisted reproduction.
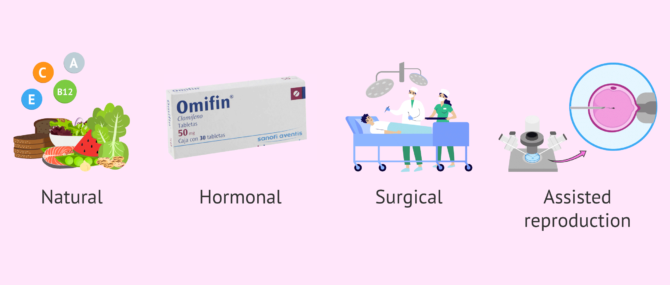
Below, you will find some possible treatments for male infertility:
- Natural treatment
- A healthy lifestyle with a balanced diet combined with vitamin supplements can help improve seminal quality in less severe cases. Above all, antioxidants such as selenium, carnitine and vitamins E, A, C and B12 are very important.
- Hormonal drugs
- gonadotropins and clomiphene citrate, for example, are given to men with hypogonadotropic hypogonadism.
- Surgical intervention
- for testicular conditions such as cryptorchidism or varicocele.
- Assisted Reproduction
- when the previous options cannot be applied or have not been successful. In the face of a severe male factor, the technique that offers the best success rates is ICSI (Intracytoplasmic sperm injection).
We recommend visiting the following post in order to get more information about this subject: Treatments for Male Infertility.
Do you need donor sperm for your fertility treatment cycle? Then we recommend that you get your Fertility Report now to find the most suitable clinic for you. Our thorough selection criteria when it comes to recommending clinics plus your particular needs equal the best fertility center for you. You will receive in your inbox a detailed report with the clinics that we recommend for your particular treatment, as well as the conditions that they offer for each program.
FAQs from users
What are the main symptoms of male infertility?
Male infertility is usually asymptomatic and the causes are diagnosed after taking a thorough clinical history of the patient with personal and family history, and requesting the indicated complementary tests.
What hormones are analyzed to determine the cause of male infertility?
Among the multiple causes of male sterility are those that depend on the interaction between the brain and the testicle, and it is in these cases where it is of interest to request a hormonal study, through the FSH (follicle stimulating hormone) and LH (luteinizing hormone). Their determination will indicate the state of the pituitary-testicular axis.
Does age influence male fertility?
Male age can affect sperm quality, but there is not as marked a decline in fertility as in the case of women. After the age of 40, male fertility decreases. It has been observed that with age there is a slow but progressive reduction in seminal volume, a decrease in sperm concentration and an increase in oxidative stress.
In addition, the likelihood of sperm having genetic alterations also increases. Nevertheless, a man can still be fertile in his 50s, 60s and even 70s.
In the following article there is more information on the effect of age on men: What is Andropause / male menopause
Can infertility in males be temporary?
Yes, there are cases in which the male goes through periods of stress or anxiety that can cause temporary infertility. The same happens with flu-like processes with fever, since the increase in body temperature affects the production of spermatozoa. In these cases, fertility can recover after 3 months once the stage that causes infertility is over. This is because a complete process of spermatogenesis lasts 3 months.
Can male infertility be cured with diet?
A balanced diet, rich in antioxidants such as vitamin supplements or omega 3, can boost sperm quality in certain cases. However, improvement is not possible in the most severe cases of infertility. In such cases, fertility treatments are the only solution to achieve pregnancy. The following post may be of interest: Foods to boost sperm quality.
If I have received chemotherapy, am I sterile?
The effect of chemotherapy on sperm quality depends on the drug used for treatment, since not all of them affect spermatogenesis in the same way. In addition, each patient may be more or less affected by the treatment. To find out whether a patient's testicular function has been altered, it will be necessary to perform a fertility study.
This article explains more about the effect of chemotherapy drugs: Cancer and fertility
The result of the seminogram indicates that I have azoospermia. Will I not be able to be the biological father of my children?
Azoospermia is the absence of sperm in the ejaculate, but it can have different causes. Depending on the reason for the azoospermia, the prognosis will be one or the other.
If it is due to a posttesticular factor (obstructive azoospermia), sperm production is not altered and sperm can be obtained directly from the testicle. However, if it is an alteration in sperm production (secretory azoospermia), it is very unlikely that sperm will be found in the testicle.
For more information on this male fertility problem, you can read the following article: Azoospermia
What are the main causes of male infertility?
About 30% of sterility cases are due to problems in the male. These problems can be found at the pretesticular, testicular, posttesticular or even semen level.
For example, leading an unhealthy lifestyle or having diabetes would cause alterations in the hormonal axis and could be the cause of male sterility. In addition, genetic alterations, varicocele, oncological treatments or obstruction of the seminal ducts, among others, would also be a cause of male infertility.
Therefore, when a couple hasbeen trying pregnancy for some time and it does not come, the best thing to do is to begin with fertility studies in both the woman and the man.
Recommended reading
If you are interested in learning more about the male reproductive system and how it works when a man becomes fertile, we recommend the following article:Male fertility: the male reproductive system
There are multiple diseases or alterations that can cause male sterility. For details about each them, we have the following page for you: Illnesses that cause male infertility
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
G.R. Dohle, T. Diemer, A. Giwercman, A. Jungwirth, Z. Kopa, C. Krausz (2010). Guía clínica sobre la infertilidad masculina. European Association of Urology 2010 (actualización en abril de 2010) (view)
Griffin DK, Finch KA (2005). The genetic and cytogenetic basis of male infertility. Human Fertil;8(1);19-26
Guzick DS, Overstreet JW, Factor-Litvak P, Brazil CK, Nakajima ST, Coutifaris C, et al. (2001). Sperm morphology, motility, and concentration in fertile and infertile men. N Engl J Med; 345: 1388-1393 (view)
Juárez de Diego JF (1999). Principales causas de infertilidad masculina. En: Arrondo JL. Actualización en Andrología. Publimed Comunicación SL. Pamplona.
Male infertility best practice policy committee of the American Urological Association (AUA) (2010). The optimal evaluation of the infertile male. AUA Best Practice Statement. Revised,.
Matorras R, Hernández J (eds.) (2007): Estudio y tratamiento de la pareja estéril: Recomendaciones de la Sociedad Española de Fertilidad, con la colaboración de la Asociación Española para el Estudio de la Biología de la Reproducción, de la Asociación Española de Andrología y de la Sociedad Española de Contracepción. Adalia, Madrid (view)
Pierik FH, Van Ginneken AM, Dohle GR, Vreeburg JT, Weber RF (2000). The advantages of standardized evaluation of male infertility. Int J Androl; 23(6): 340-6 (view)
Sociedad Española de Fertilidad (SEF) (2011). Manual de Andrología. Coordinador: Mario Brassesco. EdikaMed, S.L. ISBN: 978-84-7877 (view)
World Health Organization (WHO) (2000). WHO Manual for the Standardized Investigation, Diagnosis and management of the infertile male. Cambridge: Cambridge University Press.
FAQs from users: 'What are the main symptoms of male infertility?', 'What hormones are analyzed to determine the cause of male infertility?', 'Does age influence male fertility?', 'Can infertility in males be temporary?', 'Can male infertility be cured with diet?', 'If I have received chemotherapy, am I sterile?', 'Can problems with sperm cause miscarriage?', 'The result of the seminogram indicates that I have azoospermia. Will I not be able to be the biological father of my children?', 'Does sperm quality decrease as a man ages?', 'What are the main causes of male infertility?', 'Can HPV cause infertility in males?', 'Does mumps cause infertility in males?', 'Can Chlamydia cause infertility in males?', 'Does testicular trauma affect fertility?', 'Are there any Ayurvedic treatments or remedies to cure male infertility?' and 'Are men with Cystic Fibrosis sterile by default?'.
Authors and contributors


More information about Michelle Lorraine Embleton






Hello Sandra F… my husband is infertile, what are our options? Just wondering now on my own because I’m still young and would love to have children… if this is our situation, I’m considering the possibility of divorcing…