In most in vitro fertilization (IVF) cycles, either with your own eggs or with egg donation, there are embryos left over at the end of the treatment. This is due to the improvement of assisted reproduction techniques and the tendency to transfer a single embryo to the patient's uterus.
The embryos left over from an assisted reproduction treatment, if they are of good quality, are vitrified to preserve them. The destiny of these frozen embryos depends both on the legislation that regulates assisted reproduction techniques in your state and/or country and on the decision of the couple or patient.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 2.
- 3.
- 3.1.
- 4.
- 5.
- 5.1.
- 5.2.
- 5.3.
- 5.4.
- 6.
- 7.
- 8.
What is the origin of the surplus embryos?
When a couple undergoes in vitro fertilization (IVF) reproductive treatment, either conventional IVF or intracytoplasmic sperm injection (ICSI), the aim is to obtain as many good quality embryos as possible. The aim of this is to increase the chances of success of the cycle.
However, it is not possible to transfer all the embryos obtained in the cycle to the patient's uterus in a single attempt. The two main reasons are:
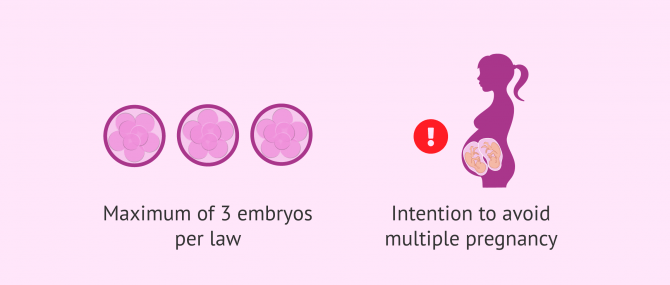
- The advice or legislation of the governing body in your particular area. Usually guidlines limit the transfer to one or perhaps two embryos, with a maximum of three.
- The intention to avoid multiple pregnancy. In this way, a single embryo will be transferred whenever possible, i.e. without compromising the chances of success.
It should be noted that the optimization of embryo freezing techniques that has taken place in recent years makes it possible to cryopreserve leftover embryos without compromising their survival rates. In addition, the quality of the treatments and embryo selection techniques has also increased.
Considering undergoing a fertility treatment? By getting your individual Fertility Report your will see different clinics especially selected for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
All these advances allow more single embryo transfers to be performed without decreasing the pregnancy rates per ovarian stimulation cycle. However, these improvements in turn lead to an increasing number of surplus embryos.
How many embryos to transfer?
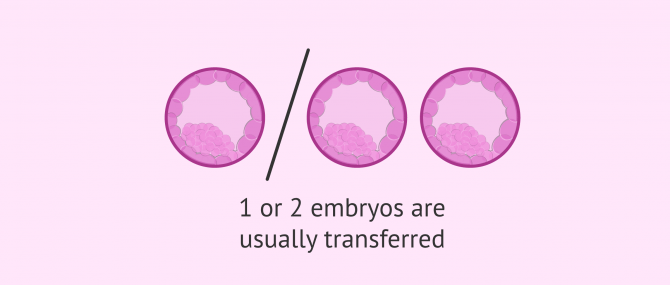
The couple or single woman who undergoes the reproductive treatment is the one who decides, together with the medical recommendations of the specialists, the number of embryos to be transferred. Currently, it is most common to transfer one or two embryos per transfer.
Only in cases with poor prognosis are three embryos are transferred. If this is the case, it is important that specialists inform the patients about the advantages, risks and effects of transferring one, two or three embryos depending on the characteristics of the woman and the specific medical situation.
Fate of frozen human embryos
The choice of the number of embryos to transfer is not the last important decision to be made. After the embryo transfer, a decision must be made about what to do with the untransferred embryos.
In Spain, the cryopreservation of embryos is regulated by article 11 of Law 14/2006. Among other things, this article states:
Pre-embryos left over from the application of in vitro fertilization techniques that are not transferred to the woman in a reproductive cycle may be cryopreserved in banks authorized for this purpose.
Law 14/2006 also specifies the options regarding the destination of frozen excess embryos:
- Own use, either because the first attempt has failed or because a second child is desired. This option allows another embryo transfer without the need to undergo ovarian stimulation or follicular puncture. In this way, the most inconvenient stages of IVF treatments are avoided.
- Donation for reproductive purposes. Patients, in this case, must meet the same requirements stipulated for donors. The recipient couple will perform what is known as an embryo adoption.
- Donation for research purposes. The couple will be informed of the specific project for which their embryos will be used and must sign a specific consent form stating the project in question.
- Cessation of their conservation without any other use.
This last option can only be used when the medical authorities consider that the woman no longer meets the appropriate requirements for the assisted reproductive technique. Furthermore, as stipulated by law, this must be decided by specialists outside the centre where the embryos are kept.
Renewal of consent
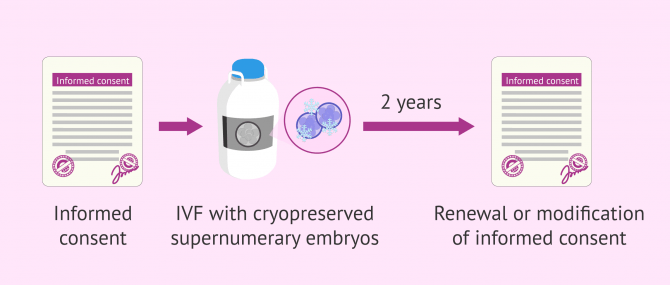
Once the centre has explained in detail the four possible alternatives to the woman or couple, the woman or couple must sign an informed consent form authorising the destination chosen. This consent is signed prior to IVF treatment, but must be renewed (or modified to give another destination to the embryos) at least every two years.
It is common that the first option chosen is cryopreservation for later use by the woman or couple, either because of failure of the first IVF cycle or because they want to give a sibling to the child already born. However, after several years, the couple or woman may decide to change the fate of the cryopreserved embryos.
The donation of pre-embryos for adoption by other couples is an option that is rarely chosen. Furthermore, the requirement that the woman must not be over 35 years of age to be able to donate is an impediment, since most patients who undergo IVF are over this age.
Donation for research purposes is also not very popular. The truth is that, at present, many couples do not care for their embryos and do not respond to the renewal or modification of the consent.
What happens to abandoned embryos ?
One of the problems that assisted reproduction clinics currently suffer is that many patients with frozen embryos do not renew their consent. This means that they do not communicate that they wish to continue with the maintenance of these cryopreserved embryos nor do they indicate a new destination.
This is a controversial topic in the US as clinics are experiencing increasing numbers of abandoned embryos. It has been suggested that new legislation is needed to keep up with the current developments in assisted reproductive treatments.
UK law requires that if more than 5 years have passed without any communcation or consent from the parents of the embryos, the embryos must be destroyed.
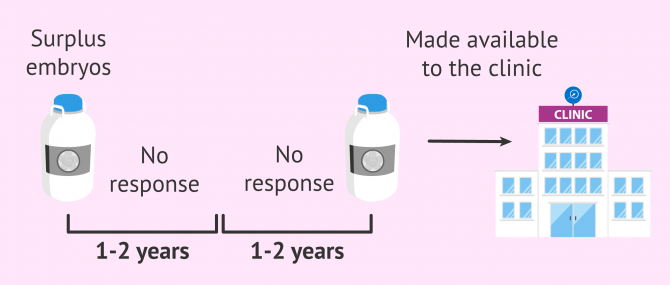
In Spain, if after two consecutive renewals, the centre where the embryos are stored does not manage to obtain the signature of consent from the woman or couple, and is able to demonstrate the actions carried out to obtain the renewal without obtaining a response, the embryos will remain at the disposal of the clinic.
Therefore, in this case, the clinic will be able to choose the destination of the abandoned embryos as long as it maintains the conditions of confidentiality and anonymity and free of charge.
Video on what happens to the excess embryos after IVF
Michelle Lorraine Embleton, biochemist at inviTRA, talks to us in this video about why there are leftover, surplus embryos after an IVF cycle and their fate.
In an IVF treatment, fertilization of the egg with the sperm takes place outside the body, the embryos are grown in the laboratory and then the best embryo(s) transferred into the womans body. The embryos that are not transferred can be preserved cyrogenically for future use, donated for other treatments or research, or destroyed.
FAQs from users
What are abandoned embryos from IVF treatment?
In Assisted Reproduction clinics, when IVF treatment is performed, a number of embryos is obtained that may be more than the number of embryos that the woman or couple needs to have the number of children they want. These embryos are kept cryopreserved in the banks of the clinics until the patients decide what fate they want to give them, since they will not need them.
It may happen that a woman or couple does not want to maintain their embryos, ignoring the requirements of renewal of the destination that the clinic must make at least every 2 years (the woman or the progenitor couple is asked to renew or modify the signed consent). In this case we would be talking about abandoned embryos.
The solution that the law established to dispose of these embryos is that, if during two consecutive renewals it is impossible to obtain the signature of the corresponding consent from the woman or the progenitor couple, and the actions carried out with the aim of obtaining said renewal without obtaining the required response can be demonstrated in a reliable manner, the embryos will remain at the disposal of the clinic, the embryos shall remain at the disposal of the centres in which they are cryopreserved, which may use them according to their criteria for any of the purposes established by Law 14/2006, of 26th May, on assisted human reproduction techniques, maintaining the established requirements of confidentiality and anonymity, as well as being free of charge and non-profit-making.
Can I know which woman or couple my embryos go to if I donate them to other patients?
One of the possibilities within the Informed Consent is to donate your embryos to another patient/s for reproductive purposes. These embryos become part of the Centre's own embryo bank. The donation of embryos will be made by the Centre to the recipient patient/couple, who will be reminded of the free, secret and anonymous nature of embryo donation and its nature as a voluntary, altruistic and disinterested act. Likewise, in your case, you will not be able to know to whom the embryos have been donated.
If artificial insemination is performed instead of in vitro fertilisation, are there also supernumerary embryos?
No. In assisted reproduction treatments in which artificial insemination is performed, fertilisation takes place in the woman's uterus. Therefore, neither eggs are extracted nor embryos are generated in the laboratory.
Are better results achieved with a second IVF than with the transfer of frozen embryos?
One of the factors that most influences the results of in vitro fertilisation (IVF) treatments is the quality of the embryos.
Thanks to advances in cryopreservation, we can now vitrify (freeze) embryos without altering their quality.
Therefore, if the embryos are of good quality, the results of vitrified embryo transfer (VET) are practically the same as if we transfer fresh embryos from a second ovarian stimulation.
However, it must be considered that it is much more comfortable for the patient to transfer frozen embryos than to have to undergo ovarian stimulation and follicular puncture again. For this reason, it is most common to transfer all the cryopreserved embryos before starting another ovarian stimulation cycle.
Recommended reading
If you want to know more details about UK Law, we recommend reading the following article: Egg Donation & UK Law - What Does the HFE Act 2008 Say?
On the other hand, if you wish to know what the transfer of frozen embryos consists of, you can find more information here: How Does the Frozen Embryo Transfer (FET) Procedure Work?
We make a great effort to provide you with the highest quality information.
🙏 Please share this article if you liked it. 💜💜 You help us continue!
References
Berrocal Lanzarot, A. I. (2007). Análisis de la nueva Ley 14/2006, de 26 de mayo sobre técnicas de reproducción humana asistida. Una primera aproximación a su contenido. Revista de la Escuela de Medicina Legal de la U.C.M.
Comisión Nacional de Reproducción Humana Asistida (CNRHA) (2015). Aspectos legales y éticos de la donación. En: Registro Nacional de Donantes de Gametos y Preembriones. Ministerio de Sanidad, Consumo y Bienestar Social de España.
Ley 14/2006, de 26 de mayo, sobre técnicas de reproducción humana asistida. Jefatura del Estado «BOE» núm. 126, de 27 de mayo de 2006 Referencia: BOE-A-2006-9292. (view)
FAQs from users: 'What are abandoned embryos from IVF treatment?', 'Can I know which woman or couple my embryos go to if I donate them to other patients?', 'What is the origin of the surplus embryos after IVF?', 'In IVF, how many embryos are transferred?', 'What is the fate of unused human embryos after an IVF treatment?', 'How long can IVF embryos be stored?', 'Are any surplus embryos formed after an artificial insemination?', 'Should I use my frozen embryos or repeat the whole IVF cycle?', 'If artificial insemination is performed instead of in vitro fertilisation, are there also supernumerary embryos?' and 'Are better results achieved with a second IVF than with the transfer of frozen embryos?'.
Authors and contributors


More information about Michelle Lorraine Embleton




Hi, I have some left over embryos in cryo. I have two heatlhy sons from previous IVF cycles and I don´t intend on having any more children. I want to stop the storage of the embryos and donate them, but my husband thinks we should keep them in storage in case we change our minds. Not sure what to do.
Hi IsabellaStar10
It is an interesting question that you pose and one that can be both delicate and contraversial. In your case it is a good idea to communicate well with your husband and draw up a plan for what happens to the embryos after a few more years. It also depends on the consent forms that you signed when starting the treatment and the legislation in your state or country.
Embryo donation is a possibility and if you are interested in reading more about it then please have a look at the following page: What is embryo adoption and donation?.
I hope this information helps. Best wishes!