Seminal plasma allergy or hypersensitivity is a rare disorder whose prevalence is unknown. Itching and burning in the vaginal area are the most common local symptoms of this allergy, but it can also cause systemic reactions.
The best way to prevent an allergic reaction to semen is to use a condom during sexual intercourse. However, this is not the right choice if you are looking to have a baby.
Therefore, achieving pregnancy naturally in women allergic to human seminal plasma can be difficult. However, thanks to seminal lavage, it is possible to achieve pregnancy through artificial insemination (AI) or in vitro fertilization (IVF).
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 3.
- 3.1.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 5.
- 6.
- 7.
- 8.
What is seminal plasma allergy?
Ninety percent of the semen content is seminal fluid, while the remaining 10% is spermatozoa. The liquid phase of sperm or seminal plasma is composed of minerals, sugars, hormones, cholesterol and proteins such as prostate-specific antigen or PSA.
Semen allergy, also known as semen allergy, also known as seminal plasma hypersensitivityis a rare condition caused after contact with the proteins that are part of semen. Therefore, it is an immune response to seminal plasma and, generally, to PSA.
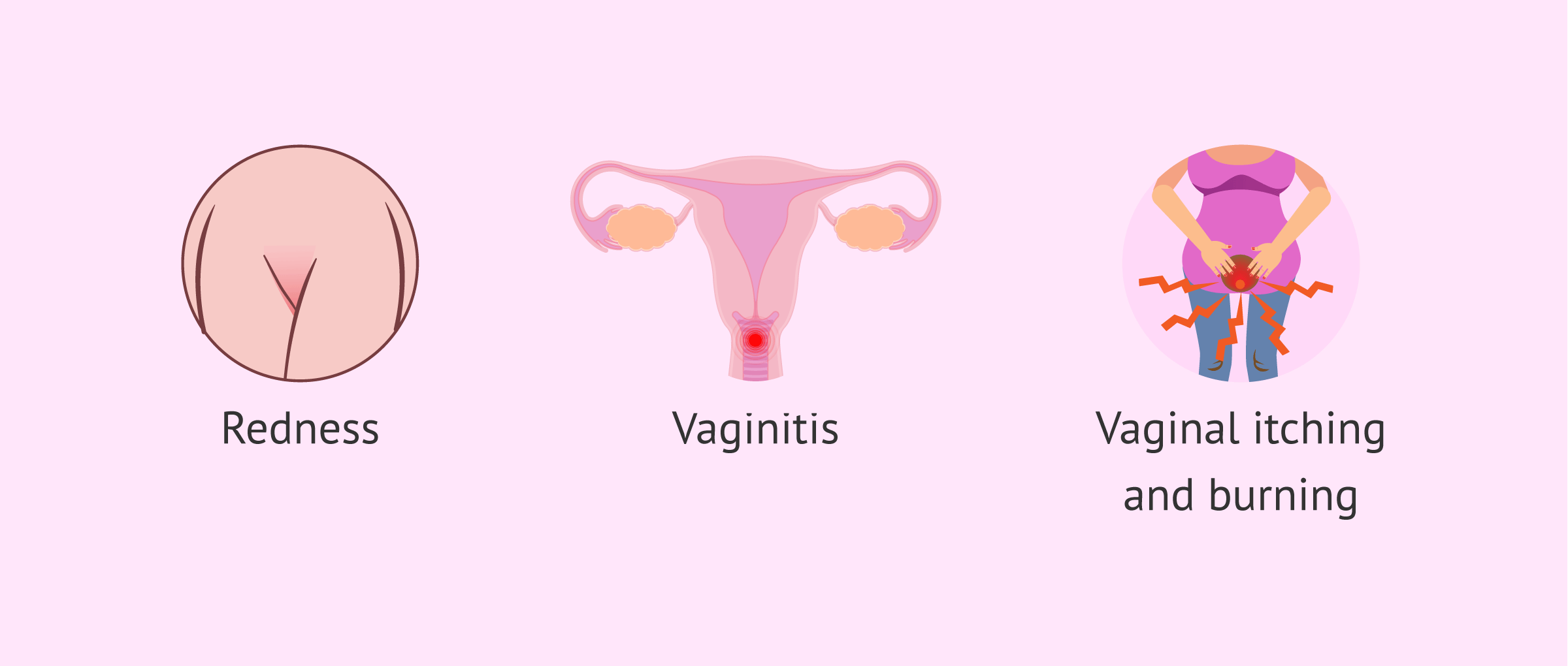
This type of allergy can occur locally or systemically and can manifest with different conditions, from vulvovaginitis to anaphylactic reaction.
In typical cases of semen allergy, patients have an IgE antibody-dependent immune reaction(type I hypersensitivity) and show symptoms during or shortly after intercourse.
Some of the risk factors are:
- Prolonged time without sexual intercourse.
- Menopausal stage.
- Use of the intrauterine device or IUD.
- Sexual intercourse with vasectomized males.
Most women suffering from semen allergy also present type I hypersensitivity to other substances, as well as asthma, allergic rhinitis, atopic dermatitis, etc. However, there are times when this is not the case.
Symptoms of semen allergy
Redness, vaginitis, pain, itching and burning sensation in the vaginal area are usually the most common clinical manifestations of sperm allergy. These symptoms usually appear shortly after contact with the ejaculate and their duration is variable.
In addition to local discomfort due to semen allergy, systemic disturbances such as angioedema or wheezing may also occur. Rarely, semen allergy causes difficulty breathing.
In any case, if you have any of these symptoms, it is best to inform the specialist as soon as possible so that he/she can establish the most appropriate treatment.
Treatment of seminal plasma allergy
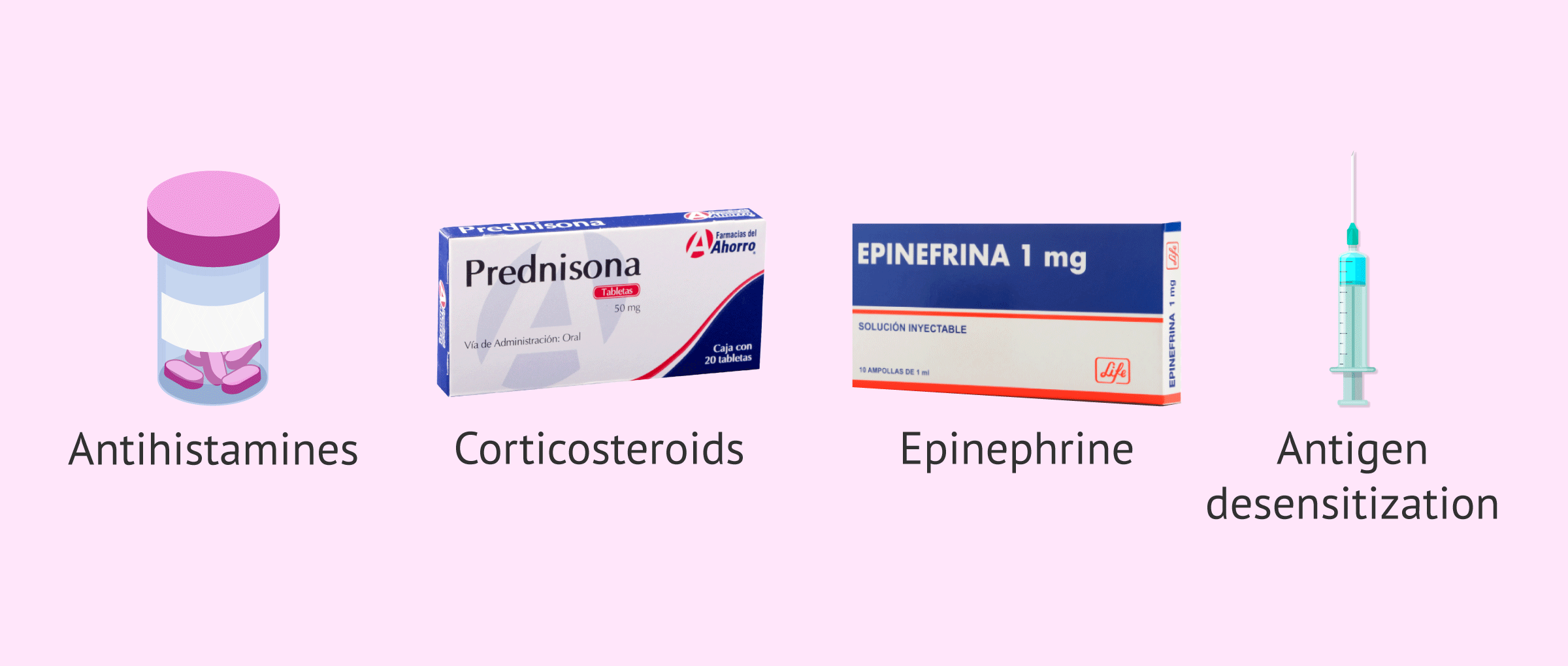
Many of the symptoms caused by semen allergy disappear on their own or with the use of antihistamines. However, at other times, the administration of corticosteroids, epinephrine or other antihistamines is necessary.
The use of condoms seems to be the best and simplest method to prevent allergy to seminal fluid, but it is unfeasible for couples who wish to conceive.
For these couples, the therapeutic alternative for semen allergy would be desensitization of the antigen responsible for the allergy.
Semen allergy and fertility
Allergy to semen can cause problems when trying to conceive, which can lead to frustration for the couple. However, allergy to seminal fluid is not equivalent to infertility.
Women with semen allergy who wish to become pregnant can do so through assisted reproductive techniques such as artificial insemination (AI) or in vitro fertilization (IVF). In particular, if the semen allergy is severe, it is best to attempt pregnancy by IVF-ICSI.
It should be noted that these reproductive treatments can cause serious problems if seminal lavage is not performed correctly. This is the reason why multidisciplinary teams must follow these patients with special care to avoid unwanted side effects.
FAQs from users
Is semen allergy synonymous with infertility?
No. Seminal plasma hypersensitivity or semen allergy is not a cause of infertility in women. However, it is true that it can cause greater difficulty in achieving pregnancy naturally, but assisted reproductive techniques can be used.
What is the composition of semen?
Sperm is formed from different secretions produced by the glands of the male genital tract. There are two types of components in semen:
- Seminal plasma: is the liquid phase of semen and is composed of secretions from the seminal vesicles, prostate, epididymis, vas deferens and adnexal glands.
- Cellular: spermatozoa are the spermatozoa and account for about 10% of the seminal content.
What causes semen allergy?
Semen allergy or hypersensitivity is an immune reaction that develops against the proteins that are part of the seminal plasma. Generally, the most common cause is allergy to prostate-specific antigen or PSA, a protein that is secreted by the prostate.
Suggested for you
As mentioned above, it is important to perform an adequate seminal lavage in order to carry out a fertility treatment in women with semen allergy. Therefore, we recommend that you read the following article to learn more about it: What does the sperm capacitation process consist of?
In addition, we have said that seminal plasma allergy For this reason, you may find it interesting to visit the following link: Immunological infertility: types, causes and treatments.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Babula O, Bongiovanni AM, Ledger WJ, Witkin SS. Immunoglobulin E antibodies to seminal fluid in women with vulvar vestibulitis syndrome: relation to onset and timing of symptoms. Am J Obstet Gynecol. 2004;190(3):663-7 (View)
Frapsauce C, Berthaut I, de Larouziere V, d'Argent EM, Autegarden JE, Elloumi H, Antoine JM, Mandelbaum J. Successful pregnancy by insemination of spermatozoa in a woman with a human seminal plasma allergy: should in vitro fertilization be considered first? Fertil Steril. 2010;94(2):753.e1-3.
Lee J, Kim S, Kim M, Chung YB, Huh JS, Park CM, et al. Anaphylaxis to husband's seminal plasma and treatment by local desensitization. Clinical and molecular allergy: CMA. 2008;6:13 (View)
Mari Tanaka, Yukinobu Nakagawa, Yorihisa Kotobuki, Ichiro Katayama. A case of human seminal plasma allergy sensitized with dog prostatic kallikrein, Can f 5. Allergol Int. 2019 Apr;68(2):259-260. doi: 10.1016/j.alit.2018.08.003 (View)
M.M. Sánchez Sánchez, A.I. Teijelo, R.M. García Robles, A. Leiva, J.M. Benavente, J.A. Pérez Escanilla, F. Corredera, A. Tejerizo García y L.C. Tejerizo LópezServicio de Obstetricia y Ginecología. Hospital Virgen de la Vega. Salamanca. España.Aceptado para su publicación el 23 de agosto de 1999 (View)
FAQs from users: 'Is semen allergy synonymous with infertility?', 'What is the composition of semen?' and 'What causes semen allergy?'.