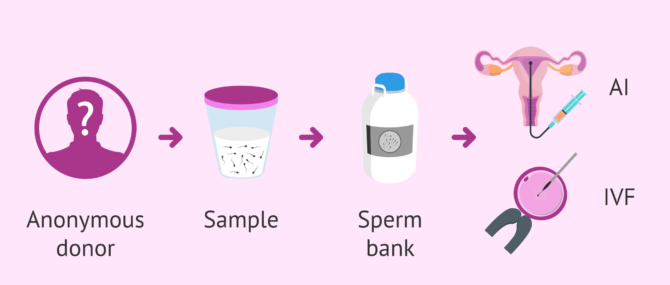
Sperm donation is an act of solidarity that allows many people to become parents, either through artificial insemination (AI) or in vitro fertilization (IVF).
Potential sperm donors must meet certain requirements in order to guarantee the success of these treatments. As such, sperm donor candidates will have to undergo a series of tests to be accepted. In addition, donors receive financial compensation for the inconvenience caused, despite the fact that the donation process is an altruistic and voluntary act.
For all these reasons, the price of assisted reproduction treatments in which a sperm donor is used to achieve pregnancy increases by about 200-500€.
Provided below is an index with the 12 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 4.
- 5.
- 6.
- 7.
- 8.
- 8.1.
- 8.2.
- 8.3.
- 8.4.
- 8.5.
- 8.6.
- 8.7.
- 8.8.
- 8.9.
- 8.10.
- 8.11.
- 9.
- 10.
- 11.
- 12.
Do I need a sperm donor?
In recent years, the use of sperm from sperm banks in assisted reproduction treatments has increased considerably. This is because more and more people require these techniques to have children, especially lesbian couples and women who want to be single mothers. Mainly, donor sperm is used in the following cases:
- Very severe male infertility, when the partner's sperm cannot be used. For example, in the case of secretory azoospermia.
- To avoid a genetic disease transmissible by the male of the couple, especially in cases where it cannot be detected by preimplantation genetic diagnosis (PGD).
- Absence of male partner.
Thus, we see that sperm donation is used when the partner's sperm cannot be used, for whatever reason.
What does it involve?
Sperm donation is a relatively simple act, consisting simply of donating ejaculated semen. The difference with respect to egg donation in the case of women is that sperm donation does not require any surgical intervention.
Once the donation procedure has been performed, the semen is frozen in a sperm bank for later use by a woman or couple in need of assisted reproduction treatment.
These semen samples from donors cannot be used until they have been verified that they are completely free of sexually transmitted diseases. Therefore, it is necessary that at least 6 months have passed after the donation of the sperm, for the sperm to be assigned to a recipient.
As a result, it is not necessary for the donor to synchronize with the partner in order to donate, but can donate when it suits him/her best. This also makes the process more comfortable for the male.
Legal aspects of sperm donation
Sperm donation in Spain is completely anonymous and altruistic. The reproduction center is provided with all the information and the donation process is recorded, but the parents cannot know the identity of the donor or choose the donor's characteristics.
Recipients of donor sperm will only receive general information about blood type, hair color, height, etc., but under no circumstances will they receive any identifying information about the donor.
Accordingly, the sperm donor is also not provided with the identity of the recipient partner or woman or any information about the patients using the sperm.
Law 14/2006 on assisted human reproduction techniques states that only in the case of a serious disease that may endanger the health of the child or for criminal matters, the identity of donors may be disclosed.
However, the release of identity would be done through the center's physicians and through a court order, and only if it is indispensable to avoid danger or for a legal purpose. Otherwise, no one outside the center can have access to the donor's information.
Who can be a sperm donor.
Any man who is fertile, in good physical and mental health and has optimal semen quality can be a sperm donor. In order to donate sperm, as we will see below, you need to meet a series of requirements and follow a few simple steps.
Requirements to donate sperm in Spain.
Spanish law requires the donor to:
- Be between 18 and 50 years old.
- Not suffer from any infectious disease transmissible to offspring, such as HIV, hepatitis B and C or syphilis.
- Not have any genetic disease or family history of hereditary disorders.
- Be in good physical and mental health This will be verified by medical and psychological tests.
- Have excellent quality semen to ensure a high success rate and that the sperm survive the freezing process.
Furthermore, it is important to ensure that the sperm donor candidate has no more than 6 children in the national territory at the time of donation. This to avoid possible consanguinity problems (colloquially known as in-breeding).
If the male does not meet all of the above mentioned requirements, he cannot be accepted as a sperm donor in any clinic in Spain.
How do you donate sperm?
In order to donate sperm, the potential donor should go to an assisted reproduction center. The center's staff will perform the preliminary tests to check if he can be admitted. Once accepted into the donor program, the male must come into the clinic to to provide donations. The elegibility tests performed on donors are as follows:
- Seminogram (semen analysis).
- Semen test freeze.
- Genetic study.
- Study of infectious diseases.
- Psychological test.
If the tests are all passed and the man is admitted as a donor, he must then proceed as follows, and according to the center´s instructions:
- The donor needs to maintain a period of sexual abstinence of 3 to 5 days prior to donation, for optimal semen quality.
- In a private room at the center, the ejaculate is deposited in a jar and delivered to the laboratory.
The donation process takes between 3 and 9 months, depending on the center, although it usually takes about 6 months. A sample must be deposited weekly, so the donor must agree on the days and times when he/she can come to the center to do so.
All semen samples deposited by the donor are frozen and kept in a sperm bank. The samples can remain frozen for years, as they are stored in liquid nitrogen. When they are to be used, they are thawed and the spermatozoa maintain their functional and morphological characteristics properties.
Financial compensation to donors
In many countries it is important to understand that semen is not paid for: it is not a sale of gametes. It is illegal to sell sperm according to certain laws, depending on where you live. The money received is a form of compensation from the clinic to the donor, for the inconvenience of coming to the center, undergoing the tests, the loss of work hours that may be involved, etc. Therefore, it is compensation for the time and effort spent.
The financial reward is about €30 to €50 for each donation. The amount varies depending on the length of time you donate for.
The usual process is 25 donations, so about €1,200 can be obtained. This amount is usually given in weekly or monthly installments, depending on the clinic.
How to choose the sperm donor?
In Spain it is not possible to choose a sperm or egg donor, so prospective parents will not see a catalog of sperm donors as is the case in some countries. It is the assisted reproduction clinic itself that assigns a donor to the woman or couple in need. The center's staff will always look for the greatest possible similarity between the donor and the recipient couple or woman.
Under no circumstances may parents indicate their preferences or choose certain physical or personality traits. The choice will be made taking into consideration the characteristics of the couple or woman:
- Physical characteristics
- race, skin, eye and hair color, height, etc.
- Immunological characteristics
- blood group and Rh factor.
Thus, if a heterosexual couple has Caucasian traits, they will be matched with a donor who also has Caucasian traits; they will never be matched with a donor of another race or with traits representative of another race or nationality.
In addition, an attempt should be made to have as much physical similarity as possible to the female recipient of the sample.
If you want to know more about how the sperm donor is chosen, you will find more information in this article: Sperm donor selection
Pregnancy from sperm donation
There are two assisted reproduction techniques that can be performed with donor sperm:
- Artificial insemination (AI)
- this is the simplest technique, whereby the donor's sperm is introduced directly into the woman's uterus through a cannula.
- In vitro fertilization (IVF)
- this technique requires the extraction of eggs directly from the ovary in order to fertilize them in the laboratory with donor sperm.
In both cases the semen used comes from a sperm bank, where the sperm remain frozen to preserve their characteristics and functionality intact until the moment they are needed.
Children born thanks to a sperm donor in Spain cannot know their biological father, since, as we have indicated above, anonymity must be maintained. Donors have no rights over the children born as a result of their donation.
Prices of treatments with sperm donation
The price depends on the treatment, the clinic where it is performed, the number of attempts needed to achieve pregnancy and whether any additional technique is needed for the particular case.
In general, in Spain, artificial insemination with donor sperm can cost between €800 to €1500. In the UK the price is between £700 - £1600.
The price in the United states can vary greatly, since the sale of sperm is permitted, and can range from $300 to over $4000.
To this sum, you must also add the cost of the necessary hormonal medication to gently stimulate the maturation of the eggs. This is not usually included in the price. The cost of this medication is around €300
In vitro fertilization (IVF) has a higher cost, since it requires more manipulation and instrumentation. In Spain, the price of IVF with donor sperm is around €3,200-€5,000.
In the UK this process can cost between £5000 and £8000 depending on the clinic and techniques used.
A cycle of IVF with donor sperm in the US can typically cost around $13,000 - $17,000, and will vary greatly between location, clinic, techniques and the cost of the donor sperm.
Again, the price of any medication needed is not usually included. This can cost around 1000-1200€, as a higher dose is needed than for insemination.
Success rates with donor sperm.
Because donors are subjected to strict testing and the criteria they must meet are very demanding, success rates are higher when donor samples are used compared to the results obtained with the partner's sperm.
However, the probability of achieving pregnancy will also depend on the patient's age and the cause of infertility. These factors directly influence the quality and quantity of eggs available in the ovary and, therefore, the probability of pregnancy. The hormonal medication used for treatment and the endometrial receptivity achieved are also relevant points.
The probability of pregnancy varies, depending on the age of the woman between approximately 13 and 22% in each attempt. When a woman is 40 or older, the probability of pregnancy is considerably lower if her own eggs are used.
From the age of 35-37 years the ovarian reserve (number of eggs in the ovary) decreases drastically, hence, the probability of pregnancy by artificial insemination is low. Therefore, in vitro fertilization (IVF) is directly recommended.
In the case of IVF, the probability of pregnancy with donor sperm can be approximately 40-45% in each cycle.
In this article you will find all the information about the probability of pregnancy in the different treatments: Success in assisted reproduction
FAQs from users
Are there sperm banks in Spain and do clinics use sperm from these banks or also from overseas?
Yes, there are sperm banks in Spain. Usually, the assisted reproduction clinics themselves have their own bank, so that donors come to the clinic to make the donation. There is also an independent Spanish bank, which does not depend on any clinic and supplies those centers that need it.
If a patient has unusual physical characteristics and no compatible donor can be found, the clinic can request samples from a foreign bank.
Can the same sperm donor be used for a second pregnancy?
In Spain, it is possible to use the same sperm donor for a second pregnancy, provided the requirements established by Law on Assisted Human Reproduction Techniques are met.
Spanish legislation sets a legal limit of six children born in Spain per donor. As long as this limit has not been reached and the clinic (or donor bank) still has available samples from that donor, the same donor may be used for a subsequent pregnancy.
When is the use of donated sperm required?
The use of banked sperm is required in situations of severe male infertility: very low semen quality or with parameters well below normal and/or poor results in previous in vitro fertilization cycles.
In addition, the use of donor sperm is also indicated in situations where there is an absence of sperm in the ejaculate and in testicular biopsy (secretory azoospermia) or when the man is a carrier of a hereditary genetic disease.
Other indications for the use of donor sperm are when there is no male partner, such as women who choose to become single mothers or for female couples who wish to have a child together.
Are there any risks associated with assisted reproduction treatments using donated sperm?
If the regulations established by the Spanish law of assisted reproduction are complied with, the use of donor sperm for reproductive purposes can be considered as "highly safe". In fact, the tests carried out on the donor will entail a lower risk of transmission of genetic or infectious diseases, than couples seeking pregnancy who have not been previously tested, having unprotected sex.
In spite of all the studies that are carried out, there will always be what we call a "residual risk", which is linked to diseases that have not yet been studied or diseases that we do not know how to study.
Where can I find a known donor for sperm?
Known sperm donation is allowed in countries such as the United States or the United Kingdom. For instance, in the UK a friend or family member could be your sperm donor, although the HFEA recommends to draw up a donor co-parenting agreement in order to set out the intentions of each party.
How is donor sperm frozen? How long does it last?
The semen is frozen at the assisted reproduction center or sperm bank where the sample is delivered. For this purpose, the sample is placed in containers (straws or cryotubes) and immersed in liquid nitrogen at -196°C.
Semen samples frozen in liquid nitrogen can be stored for years without any problem. The sperm do not suffer any damage and remain with practically the same characteristics as the moment when they were frozen.
Is sperm donor treatment availble through social security? (Spain)
Yes, if the couple needs sperm donation due to poor semen quality of the male partner, donor sperm can be used. However, treatment with donor gametes is not available in all communities and centers, so you should enquire about the specific conditions of your assigned center.
In the case of women without a male partner (single women or female couples), the treatment can be performed only in those autonomous communities and centers where they are allowed to receive said treatments. Therefore, they should also request information about the specific conditions in their medical center or hospital.
How much does sperm donation pay in Spain?
Sperm donors are given money as compensation for their trouble, time and effort, but it is not payment per se, as it is not a sale. The compensation is usually between €30 and €50 per sample donated.
Can you buy sperm over the internet?
Yes, it is possible to buy sperm from a sperm bank online. The assisted reproduction centers themselves do this when they need a sample from a donor with unusual physical characteristics.
If the semen is to be purchased by an individual user, it must be purchased from a foreign bank, since in Spain sperm banks can only supply assisted reproduction clinics. In fact, in recent years, a sperm bank in Denmark is gaining a special reputation among women and couples who wish to opt for home artificial insemination.
Does a catalogue of sperm donors exist so I can choose my donor?
In Spain there is no donor catalog available for patients because the donation must be anonymous by law. However, there are catalogs of foreign banks in which it is possible to choose the donor according to the desired characteristics.
If the maximum number of offspring per donor is 6, why is there a Dutch sperm donor who has fathered over 150 children?
The regulation of gamete donation depends on each countries legislation. In Spain, the maximum number of children per donor is six. In addition, it should be noted that this maximum refers to the offspring in national territory, so in some cases it may be that the same donor has more than six children in other countries, despite making the donation in Spain.
Recommended reading
As we have seen, banked semen is used for both artificial inseminations and in vitro fertilization (IVF) treatments. If you want to know in more detail what these techniques consist of, we recommend reading the following articles:
- Donor Artificial Insemination or DAI
- IVF with sperm donor: process and results.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Andrade-Rocha FT (2003). Semen analysis in laboratory practice: an overview of routine test. J Clin Lab Anal 2003; 17: 247-258 (view)
Ballesteros A, Castilla JA, Nadal J, Ruiz, M. Manifiesto de la SEF sobre la donación de gametos en España. Publicado a través de la Sociedad Española de Fertilidad (SEF) (view)
Comisión Nacional de Reproducción Humana Asistida (CNRHA) (2015). Aspectos legales y éticos de la donación. En: Registro Nacional de Donantes de Gametos y Preembriones. Ministerio de Sanidad, Consumo y Bienestar Social de España (view)
Kvist U, Björndahl L. ESHRE Monographs: Manual on Basic Semen Analysis. Oxford: Oxford University Press, 2002.
Ley 14/2006, de 26 de mayo, sobre técnicas de reproducción humana asistida. Jefatura del Estado «BOE» núm. 126, de 27 de mayo de 2006 Referencia: BOE-A-2006-9292 (view)
Matorras R, Hernández J (eds): Estudio y tratamiento de la pareja estéril: Recomendaciones de la Sociedad Española de Fertilidad, con la colaboración de la Asociación Española para el Estudio de la Biología de la Reproducción, de la Asociación Española de Andrología y de la Sociedad Española de Contracepción. Adalia, Madrid 2007 (view)
O'Brien P, Vandekerckhove P. Intra-uterine versus cervical insemination of donor sperm for subfertility (Cochrane Review). In: The Cochrane Library, Issue 1, 2001. Oxford: Update Software.
Sigman M, Zini A. (2009). Semen analysis and sperm function assays: what do they mean? Semin Reprod Med; 27: 115-123.
Sociedad Española de Fertilidad (SEF) (2011). Manual de Andrología. Coordinador: Mario Brassesco. EdikaMed, S.L. ISBN: 978-84-7877 (view)
FAQs from users: 'Are there sperm banks in Spain and do clinics use sperm from these banks or also from overseas?', 'Could I enter into a co-parenting agreement with a known sperm donor?', 'Can the same sperm donor be used for a second pregnancy?', 'When is the use of donated sperm required?', 'Are there any risks associated with assisted reproduction treatments using donated sperm?', 'Are there any celebrity who has used donor sperm to get pregnant?', 'Where can I find a known donor for sperm?', 'How is donor sperm frozen? How long does it last?', 'What are the benefits of using donor sperm for male infertility?', 'Is sperm donor treatment availble through social security? (Spain)', 'How much does sperm donation pay in Spain?', 'Can you buy sperm over the internet?', 'Does a catalogue of sperm donors exist so I can choose my donor?' and 'If the maximum number of offspring per donor is 6, why is there a Dutch sperm donor who has fathered over 150 children?'.
Authors and contributors




More information about Michelle Lorraine Embleton










Can you guys kindly show me how to donate (sell) my sperm as I am a healthy and agile 23 year-old-boy desperately in need of money?
Dear Stephen,
Where are you from? The requirements for potential sperm donors vary from country to country. Anyway, perhaps any of the threads in our forum could be helpful, so my advice is that you visit our Sperm Donation Forum.
Should you have any further questions, do not hesitate to Ask Our Specialist.
Best wishes
I am a Nigerian currently in North Cyprus. I neither drink nor smoke, and I’m 23 years old. So is it possible I donate here?
Hello again Stephen,
We are not a clinic, but my advice is that you visit our Clinic Directory to see in which clinics from Cyprus you could donate. Just follow this link: Best clinics for egg donation in Cyprus.
I hope this helps,
All the best
Hi, I live the in UK. I really want to be a mum but I don´t have a partner so I am thinking of using a sperm donor. I understand that I can´t buy sperm in the UK but can I buy it from the USA. Any help appreciated thanks.
Hi Tamara,
You have a variety of options to become a mum using donated sperm. There are UK sperm banks that supply hospitals and clinics, and you can find many of these on the internet.
If, for whatever reason you require sperm from outside the UK, you can also buy it directly from an overseas sperm bank. The sample will be shipped to a UK licensed fertility clinic, where you can also have the treatment you require.
I hope this answers your question and good luck!