Azoospermia, commonly referred to as zero sperm count, is described as the absence of measurable sperm in the ejaculate (semen). Depending on the cause, it can be classified into two types: secretory or non-obstructive azoospermia, and obstructive azoospermia.
The chances of achieving pregnancy with azoospermia are dependent on the type, too. If it is obstructive azoospermia, sperm can be collected with a testicular biopsy to be used for ICSI. However, in cases of secretory azoospermia, retrieving sperm is more complicated, and the man might need to use donor sperm to have a baby.
Provided below is an index with the 10 points we are going to expand on in this article.
- 1.
- 1.1.
- 2.
- 2.1.
- 2.2.
- 3.
- 4.
- 5.
- 6.
- 6.1.
- 6.2.
- 6.3.
- 6.4.
- 6.5.
- 6.6.
- 6.7.
- 7.
- 8.
- 9.
- 10.
Definition of azoospermia
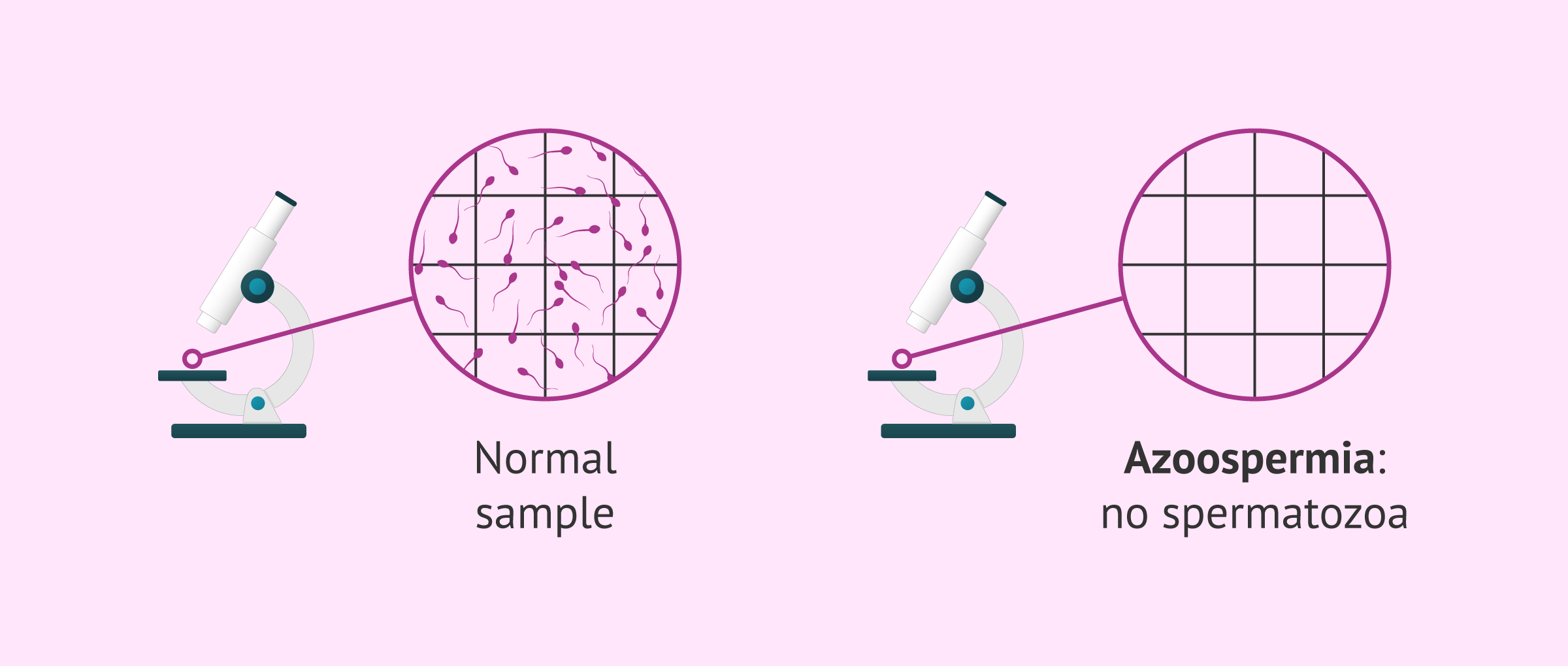
The concept of azoospermia refers to a sperm disorder characterized by the total absence of spermatozoa after ejaculation. For this reason, it is not possible to establish levels of azoospermia according to its severity, unlike what happens, for example, with oligospermia. In this case, the concentration of spermatozoa in the ejaculate is lower than normal, but not null as in azoospermia.
Azoospermia is the cause of approximately 3% to 10% of male infertility cases. As there are no sperm in the ejaculate, natural pregnancy is not possible. Therefore, men with azoospermia will have to resort to assisted reproductive techniques.
However, azoospermia does not cause clinical manifestations in men, so they will know that they have this seminal alteration after undergoing a seminogram.
What is azoospermia and how is it diagnosed?
As mentioned above, azoospermia is a disorder that has no noticeable symptoms for the male, so for its diagnosis it is necessary to perform a spermogram. This test consists of collecting a sample of the ejaculate after masturbation and with a period of abstinence of 3-5 days. The semen sample obtained will be examined in the laboratory to check, among other things, the concentration and motility of the spermatozoa.
If you need to undergo IVF to become a mother, we recommend that you generate your Fertility Report now. In 3 simple steps, it will show you a list of clinics that fit your preferences and meet our strict quality criteria. Moreover, you will receive a report via email with useful tips to visit a fertility clinic for the first time.
When the semen analysis report is available, sperm count is compared with the diagnostic reference values provided by the World Health Organization (WHO):
- Azoospermia
- No sperm in the semen.
- Cryptozoospermia
- Less than 100,000 sperm per milliliter of semen.
- Oligozoospermia
- Less than 15 M/ml.
- Normozoospermia
- All sperm parameters are normal.
Azoospermia is a medical condition that has no noticeable symptoms. This is the reason why, for its diagnosis, it is necessary to perform a semen analysis.
Determining FSH hormone levels might be useful as well. This hormone is produced by the brain and is responsible for spermatogenesis (production of spermatozoa) in the testes. If FSH levels are too high, it translates into a decreased level or the absence of stem cells in the sperm sample. A testosterone and fructose test is advisable, too.
What are the causes of azoospermia?
The fact that the man has no sperm in the semen can be due to two main causes:
- Secretory or non-obstructive azoospermia
- The testes are incapable of producing sperm.
- Obstructive azoospermia
- Sperm are produced, but the cannot be expelled with the ejaculate due to an obstruction in the ejaculatory ducts.
Carrying out a testicular biopsy is necessary in order to determine the type of azoospermia. It consists of taking a tissue sample from each testicle in order to check if it produces sperm (obstructive azoospermia) or not (secreting azoospermia). Getting your hormones tested might also help to determine the type of azoospermia. If the levels of hormones that play a role in spermatogenesis are altered, the diagnosis will be secretory azoospermia. However, this method is not so accurate as a testicular biopsy to determine whether a few sperms could be retrieved and used during fertility treatment.
Secretory azoospermia.
Secreting or non-obstructive azoospermia is the most severe, frequent type of azoospermia, being present in 70% of cases. It can be congenital (condition existing at birth) or acquired (due to an illness or treatment with toxic medicines). These are the most common causes:
- Undescended testicles
- Exposure to toxic substances: drugs, radiotherapy, and chemotherapy.
- Genetic disorders such as alterations in genes related to spermatogenesis.
- Hormonal imbalances such as hypogonadotropic hypogonadism (deficiency of the hormones released by the pituitary gland and responsible for stimulating sperm production in the testicles)
- Testicular diseases: mumps, trauma, inflammations, and severe varicocele.
If you are interested in the subject, we recommend you visit the following article: What is secretory azoospermia? - Causes and treatments.
Obstructive azoospermia
Obstructive azoospermia is due to a problem in the sperm ducts which transport the sperm from the testicles to the urethra, in which the ejaculate occurs. The most common causes of this type of azoospermia are:
- Absence of vasa deferentia, owing to either congenital reasons or after a surgical procedure.
- Inflammations or trauma in the testes, epididymis, vasa deferentia, or prostate.
For more details, keep on reading here: Obstructive Azoospermia - Causes & Treatment Options.
Azoospermia and varicocele
The relationship between azoospermia and varicocele is rather common since 5% of varicocele cases end up developing azoospermia. However, this only occurs among the most severe cases of varicocele.
Want to learn more about your options of conceiving with varicocele? Read more: Achieving Pregnancy with Varicocele.
Varicocele is defined as the dilation of the veins that form the spermatic cord and directly affects spermatogenesis, that is, the production of sperm. The more severe the dilation of the veins, the more affected the production of sperm and the higher the risk of azoospermia.
Patients with secretory azoospermia who undergo surgery for correcting varicocele (varicocelectomy) usually recover 50% of their testicular tissue. In addition, sperm motility after ejaculation is recovered in 55% of cases.
Is azoospermia by vasectomy possible?
Vasectomy is a method of male sterilization with which the absence of sperm in the ejaculate is achieved. It involves inducing obstructive azoospermia voluntarily through the cutting of the vas deferens, thus preventing the passage of sperm from the testicle to the urethra.
Since the vas deferens are blocked, the sperm will be stored in the epididymis and eventually reabsorbed by the body itself.
Vasectomy does not affect sperm production, although it is true that, over time, the body may decrease sperm production or it may be slightly altered.
Treatments
To be able to start treatment it is essential to know the type of azoospermia, that is if it is secretory or obstructive azoospermia. In addition, it should be noted that some types of azoospermia have no solution and it will not be possible to obtain any sperm.
In those males diagnosed with obstructive azoospermia, performing a testicular biopsy could be a solution for obtaining sperm. Furthermore, microsurgery by removing the obstruction and joining the ducts, epididymovasostomy, or vasovasostomy would also make it possible to treat the azoospermia and obtain sperm in the male.
On the contrary, patients with secretory azoospermia will be given hormonal treatment.
If you want more information about the different treatments, visit the following link: Treatment for Non-Obstructive & Obstructive Azoospermia.
FAQs from users
Is there any preventive treatment for azoospermia?
Most of the times the problem of azoospermia is due to a constitutional cause, either by genetic failure or congenital affection, the male is born without germ line. In these cases, azoospermia cannot be prevented.
Other causes of azoospermia occur as a consequence of testicular damage (trauma, radiation, surgery, toxins, tumors...). In these situations, healthy lifestyle habits (balanced diet, non-extreme sport, avoidance of toxins) can prevent azoospermia. Likewise, the male testicle should be protected in procedures that involve the absorption of ionizing radiation in the area.
Read more
Is it possible to be a father with secretory azoospermia?
Yes, it is possible. Secretory azoospermia is the absence of spermatozoa in the ejaculate. When we refer to secretory azoospermia it is when this absence is due to the lack of sperm production in the testicles (spermatogenesis). This sperm alteration can be reversible or irreversible.
In the case of obstruction of the vas deferens it is possible to recover spermatozoa by testicular biopsy so that the male germ cells can be rescued and an ICSI (Intracytoplasmic Sperm Injection) can be performed.
What are the symptoms of azoospermia?
Men with azoospermia will not show any noticeable symptoms such as pain, swelling, etc. Therefore, the only way to diagnose azoospermia is when the male has a semen analysis.
For this reason, many patients do not know they have azoospermia until they try to become fathers naturally and do not succeed. At this point, they go to a specialist and, after performing a seminogram, the absence of spermatozoa in the ejaculate is detected.
However, there are cases in which azoospermia can be accompanied by erection problems or sexual alterations related to some hormonal irregularity, which has led to secretory azoospermia.
It is also possible, although complicated, for the male to intuit azoospermia by a change in the color or appearance of the semen, since the absence of spermatozoa can make it somewhat more watery, light and transparent.
In any case, changes in the semen are not a determining symptom of azoospermia, since they can also be due to other reasons such as prostate or seminal vesicle alterations, eating habits, testicular pathologies, etc.
Which type of azoospermia is more serious in relation to infertility?
Secretory azoospermia is more serious. It prevents the production of spermatozoa and, therefore, it is not possible to have biological children even by applying assisted reproduction techniques. As we have already mentioned, the only option to achieve pregnancy if you suffer from this type of azoospermia is sperm donation.
Can natural pregnancy be achieved with secretory azoospermia?
Any form of azoospermia, secretory and obstructive, prevents natural pregnancy, since the ejaculate does not contain spermatozoa. As for secretory azoospermia, it will not be possible to achieve pregnancy through assisted reproduction either, since there is no sperm production.
Depending on the cause of the azoospermia, it will be possible to administer a hormonal treatment capable of restoring spermatogenesis to achieve pregnancy with secretory azoospermia, even with in vitro fertilization (IVF). If it is not possible to restore sperm production, gestation can be achieved by sperm donation.
Is azoospermia the same as aspermia?
No. Azoospermia is the absence of sperm in the ejaculate, but the man has no problems ejaculating. On the other hand, the term aspermia refers to the absence of ejaculation. Therefore, these are two different seminal disorders.
Is pregnancy possible with IUI in cases of azoospermia?
No, it is not. The main requirement for IUI to be possible is to have a normal sperm count. Unfortunately, azoospermia patients have no sperm in the ejaculate.
Suggested readings
If you wish to learn more about all the types of sperm disorders that may occur in males, my advice is that you visit this comprehensive guide to all of them: Sperm Disorders that Cause Male Infertility – Causes & Treatment.
Throughout this post, we have mentioned that IVF with ICSI is the only treatment option for males with secretory azoospermia wishing to have children. Want to get more info on this technique? Read: What Is ICSI Technique? – Process, Success Rates & Cost.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Andrade DL, Viana MC, Esteves SC. Differential Diagnosis of Azoospermia in Men with Infertility. J Clin Med. 2021 Jul 16;10(14):3144. doi: 10.3390/jcm10143144. (View)
Andrology-Male Reproductive Health and Dysfunction. Nieschlag E, Behre HM (eds). Berlin: Springer Verlag, 1997.
Cioppi F, Rosta V, Krausz C. Genetics of Azoospermia. Int J Mol Sci. 2021 Mar 23;22(6):3264. doi: 10.3390/ijms22063264. (View)
Comhaire FH, De Kretser D, Farley TMM et al. 1987 Towards more objectivity in diagnosis and management of male infertility: results of World Health Organization multicentre study. International Journal of Andrology 10, 1–53.
Cooper TG, Noonan E, von Eckardstein S, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update 2010;16:231-45.
Fogle RH, Steiner AZ, Marshall FE, et al. Etiology of azoospermia in a large nonreferral inner-city population. Fertil Steril 2006;86:197-9.
Jarow JP, Espeland MA, Lipshultz LI. Evaluation of the azoospermic patient. J Urol 1989;142:62-5.
Krausz C, Genetic Aspects of Male Infertility, European Urological Review, 2009;3(2):93-96.
Male infertility best practice policy committee of the American Urological Association (AUA). The optimal evaluation of the infertile male. AUA Best Practice Statement. Revised, 2010.
Matsumiya K, Namiki M, Takahara S, et al. Clinical study of azoospermia. Int J Androl 1994;17:140-2.
Tharakan T, Luo R, Jayasena CN, Minhas S. Non-obstructive azoospermia: current and future perspectives. Fac Rev. 2021 Jan 26;10:7. doi: 10.12703/r/10-7. eCollection 2021. (View)
WHO Manual for standardized investigation and diagnosis and management of the infertile male. Cambridge: Cambridge University Press, 2000.
FAQs from users: 'Is there any preventive treatment for azoospermia?', 'Is it possible to be a father with secretory azoospermia?', 'What are the symptoms of azoospermia?', 'Which type of azoospermia is more serious in relation to infertility?', 'Can natural pregnancy be achieved with secretory azoospermia?', 'Is azoospermia the same as aspermia?', 'Is pregnancy possible with IUI in cases of azoospermia?', 'Can a man with zero sperm count get a woman pregnant?' and 'If my sperm count is zero but I have obtained few sperms with a testicular biopsy, what are my chances of success with ICSI?'.
Authors and contributors

More information about Cristina Algarra Goosman










Dear Doctor,
I am 30 years old man, got married two years before, since then we were trying to have a baby, but later on my Semen report it was said “Azoospermia”.
My Question is, how can I identify if my azoospermia is a Secretory or Obstructive one.
Which test should I perform to know the type of Azoospermia?
Please suggest.
Regards
Balasurbamanian T
Dear Balasurbamanian T,
First, with a testicular palpation, the doctor can detect if there is sperm production in the testicles. Then, an analysis of hormone values can help to determine if there’s a problem affecting sperm production.
Finally, if these 2 tests reveal that you can produce sperm, you can undergo a testicular biopsy or sperm aspiration to look for sperm and then, use it in an assisted reproduction technique to have a baby.
For more information about how to diagnose azoospermia, you can read this post: How Is Azoospermia Diagnosed?
I hope I could help you,
Regards
I am 48 years old. I have been married since 2002. Till now I have no baby. I made more test for sperm, fertility, stimulations , fsh and other hormones. In all these tests I found no sperm. Volume 3ml, greywish; this classified me as “azoospermia”. They also took samples from my testicles but no sperm seen. And in all time the FSH is high (27). Now the semen is like watery. Before I married it was thick; more, my ejaculate comes soon within only 2-5 minutes in a little vol. My testicles are atrophic now; not like before. In the past, after the adult age I brought out my semen by hand 2-3 time per week as optimum. I think this is a main cause for my case. Please how can I deal with this disease?
On the other hand my wife is also ill: her tubes are closed. Monthly cycle is not regular (18 – 23 days only); there is some more other problems, her age is 38 years old. Please reply me as soon as possible I need your help.
Thanks
Thanks for your information.