Spermatogenesis is a process whose main function is the production of spermatozoa.
Sperm formation consists of different phases (proliferative, meiotic and spermiogenesis) and takes place inside the testicles, in rounded structures called seminiferous tubules.
Once formed, the sperm are expelled into the center of the tubule and transported to the epididymis (upper part of the testicle), where the final maturation of the sperm takes place. Mature sperm are expelled in the ejaculate and, after capacitation, are capable of fertilizing the egg.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 5.
- 6.
- 7.
- 8.
What is spermatogenesis?
Spermatogenesis is the process by which spermatozoa are formed. It occurs continuously in adult males and, for a complete cycle of spermatogenesis to take place, approximately 75-90 days are necessary for the human species.
Spermatozoa are the male gametes, i.e., the sex cells of the male. Therefore, they are haploid (contain half of the genetic information) and during spermatogenesis, they must change from somatic cells with 46 chromosomes (diploid) to sex cells with 23 chromosomes (haploid). This is achieved by meiosis.
The biological function of this reduction in the number of chromosomes in the gametes is that once the fusion of the two gametes, fertilization, occurs, the resulting zygote will have the correct number of chromosomes: 46.
For this process to be possible, specific hormonal control of the hypothalamic-pituitary-testicular axis that favors the production of spermatozoa is necessary. This first occurs with the onset of puberty in the male. From that moment on, the testicles will produce sperm continuously thanks to the start of the hormonal cascade.
If you wish to learn more about the process of gamete formation (gametogenesis) and meiosis, we recommend that you read the following article: What is the relationship between meiosis and fertility?
Phases of spermatogenesis
There are three basic stages during sperm formation: proliferative phase, meiotic phase and spermiogenesis. Each of these stages is described in detail below:
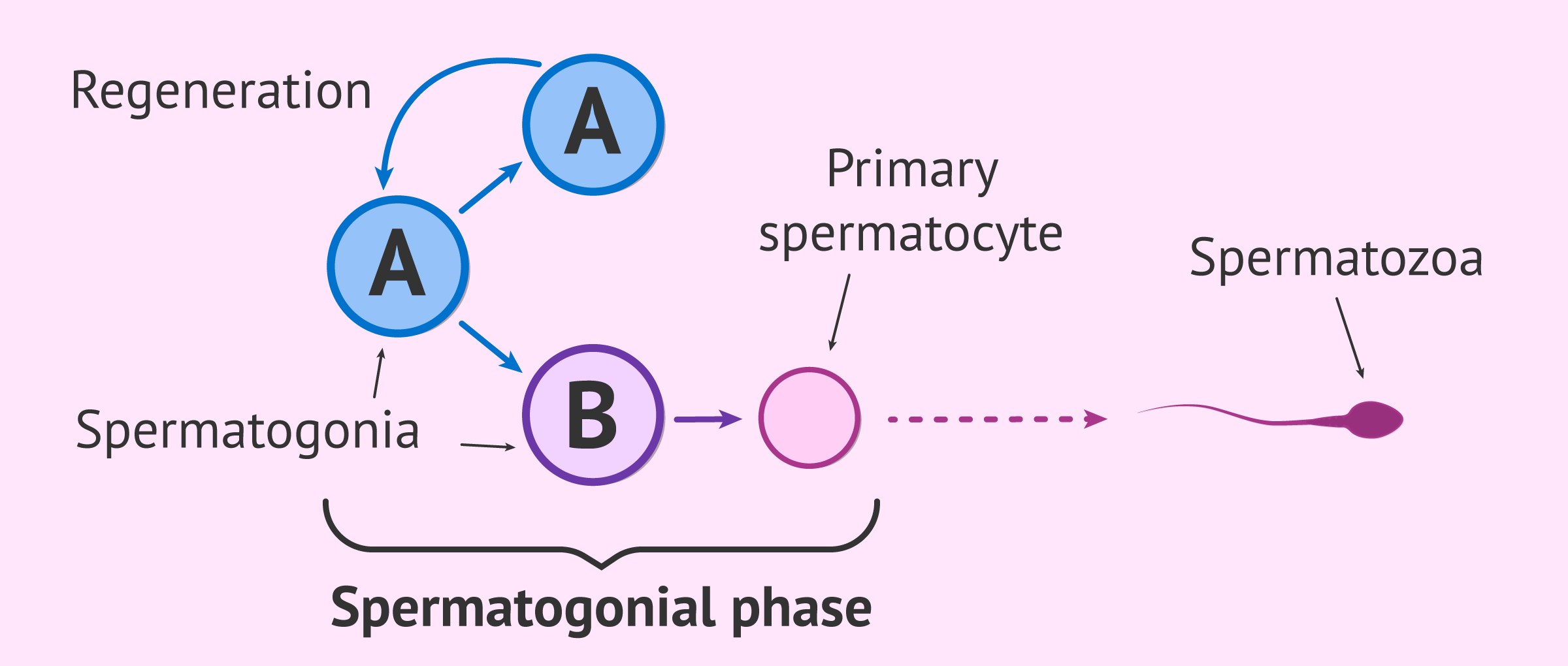
Proliferative phase
The proliferative phase of spermatogenesis is also called spermatogonial phase. From a germ stem cell, type A spermatogonia are formed. These, by mitosis (cell division), will give rise to type A and B spermatogonia:
- Type A: will continue to replicate and can give rise to type A and B spermatogonia.
- Type B: will give rise to one primary spermatocyte which, in turn, will give rise to four mature spermatozoa once spermatogenesis is complete.
Once a male reaches reproductive age (puberty or adolescence), these cells will divide multiple times to form a cell type called the primary spermatocyte. Throughout these divisions, some cellular changes take place.
It is known as proliferative phase by the multitude of mitoses that occur. The main objective is to form many sperm precursor cells, i.e., many spermatocytes.
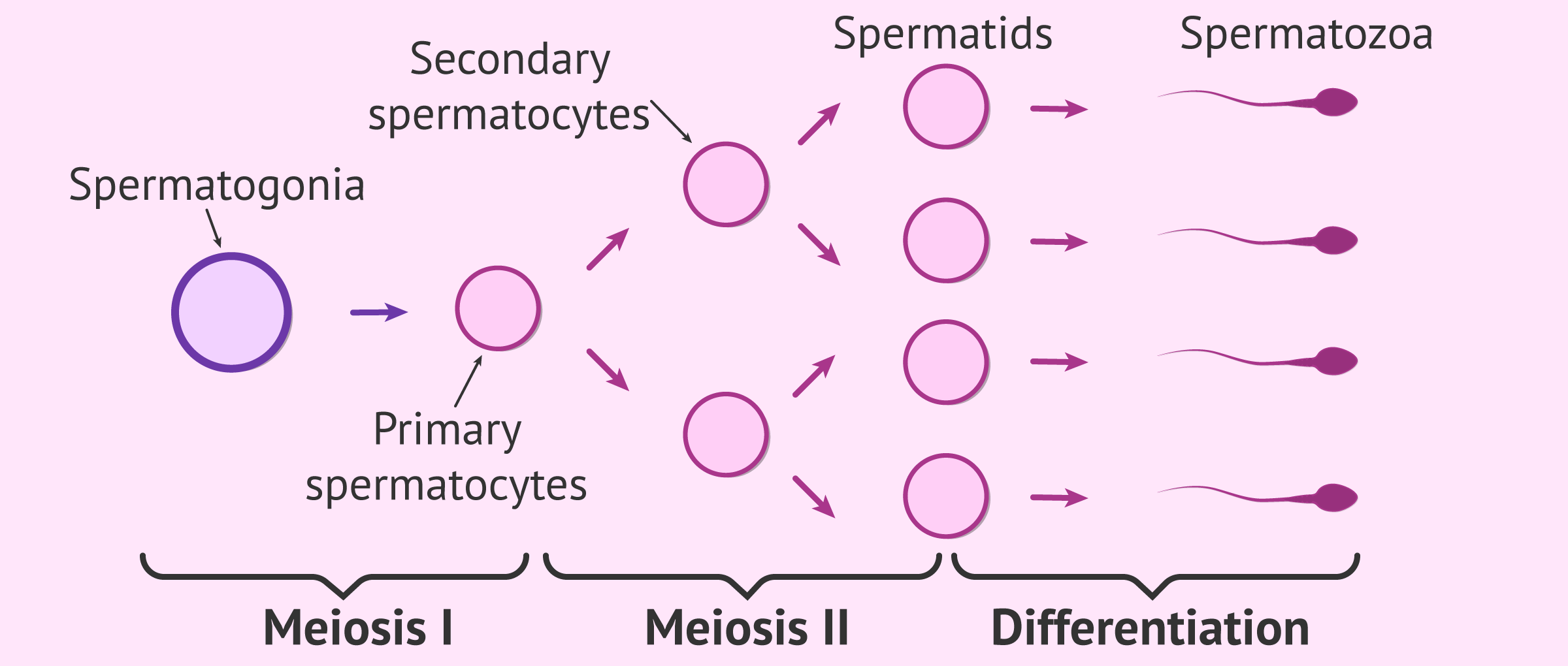
Meiotic phase
Also known as spermatocytogenesis, this is the stage at which a new type of cell division, meiosis, begins, which reduces genetic information by half. Thanks to it, haploid cells are produced, which are called spermatids.
We can divide meiosis into two substages:
- Meioisis I
- each primary spermatocyte gives rise to two haploid secondary spermatocytes.
- Meioisis II
- two spermatids are produced from each secondary spermatocyte, so that, in total, from each primary spermatocyte (diploid), we obtain four spermatids (haploid).
These cells are already very similar to spermatozoa: we can already appreciate in them the formation of a small flagellum.
Spermiogenesis
In the last stage of sperm formation, the final maturation of the spermatids occurs to give rise to mature spermatozoa.
Its tail increases in size and gives rise to the flagellum, which will allow its development. The head of the spermatozoon decreases and acquires the characteristic pointed shape due to the reduction of the cytoplasm, the elongation of the nucleus, and the formation of the acrosome.
Finally, mature sperm is released into the center of the seminiferous tubule. Although at this point the sperm is ready to be ejaculated, it will need to go through the capacitation process to be able to fertilize the egg. Naturally, capacitation occurs as the sperm travels through the female reproductive tract until it reaches the egg.
However, it is also possible to carry it out in the laboratory if in vitro fertilization(IVF) is necessary. For this purpose, the density gradient procedure is most commonly used, although sperm capacitation can also be carried out using the Swim-up method.
Hormonal regulation of spermatogenesis
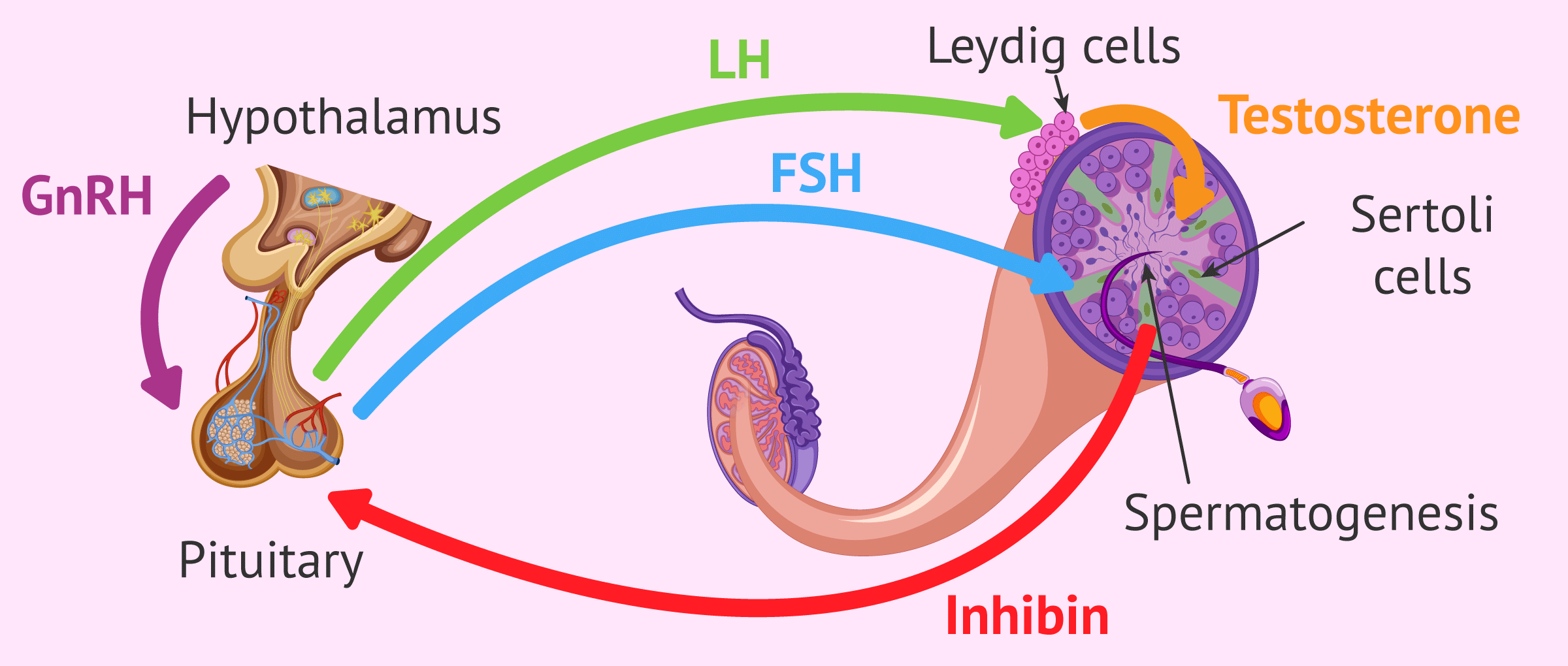
Spermatogenesis is hormonally regulated by negative feedback involving the hypothalamus, pituitary, and testes. The hormones involved in the control of the sperm formation process are:
- Testosterone
- is secreted by cells located in the testis called Leydig or interstitial cells. Among many other functions in the body, testosterone is responsible for activating genes that promote spermatogonial differentiation.
- FSH (follicle-stimulating hormone)
- is secreted by the pituitary gland and acts on the testicle. Specifically, it exerts its function on the testicular cells known as Sertoli or nurse cells, which are responsible for nourishing the spermatozoa and promoting their development and maturation.
- LH (luteinizing hormone)
- is also secreted by the pituitary gland. Its main function is to activate the release of testosterone by Leydig cells.
- Inhibin
- is released by Sertoli cells? It exerts its function on the pituitary gland, inhibiting FSH release and thus halting spermatogenesis.
If you would like to know more on a hormonal level, you may find it interesting to read the following article: Male hormone analysis: what should the normal hormone levels be?
FAQs from users
How long does it take from sperm production to ejaculation?
Spermatogenesis is the process whereby male reproductive cells are formed, from the immature ones, spermatogonia, until the mature ones, spermatozoa. This complicated process occurs within the seminiferous tubule in the testis and takes about 64-72 days.
Once spermatozoa (sperm cells) have been produced, they leave the testis and travel to the epididymis, where they will acquire the necessary motility in a process that lasts 10 days approximately. Spermatozoa will be stored in the epididymis until they are expelled with ejaculation. When ejaculation starts, sperm travel through the vas deferends and mixes with the seminal fluid that originates in the secretory glands, creating what we all know as semen. Finally, it is expelled through the urethra.
Is sperm production daily?
Yes, sperm cells are continuously formed in the seminiferous tubules.
How many spermatozoa do each spermatogonia form?
Each type A spermatogonia can give rise to:
- Type A spermatogonia, which will continue to replicate.
- Type B spermatogonia, from which a primary spermatocyte will be formed, which will continue its development until it becomes a spermatozoon.
Therefore, from a type A spermatogonia, infinite spermatozoa can be formed.
In contrast, of each type B, only four sperm will be formed at the end of the spermatogenesis process.
How many sperm are generated from a primary spermatocyte?
A partir de un espermatocito primario se obtienen cuatro espermatozoides.
How many spermatozoa result from a secondary spermatocyte?
Two spermatozoa are formed from each secondary spermatocyte.
Recommended readings
As we have seen, spermatogenesis is tightly regulated by a hormonal cascade. If you want to know more about the role of these hormones in male fertility, we recommend that you read the following article: Which male hormones are involved in reproductive function?
On the other hand, if you want to know the stages that the sperm has to go through before reaching the egg, you will find more information here: Path of the sperm to the egg.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Adetunji P Fayomi, Kyle E Orwig. Spermatogonial stem cells and spermatogenesis in mice, monkeys and men. Stem Cell Res. 2018 May:29:207-214. doi: 10.1016/j.scr.2018.04.009. Epub 2018 Apr 21 (View)
Filipe Tenorio Lira Neto, Phil Vu Bach, Bobby B Najari, Philip S Li, Marc Goldstein. Spermatogenesis in humans and its affecting factors. Semin Cell Dev Biol. 2016 Nov:59:10-26. doi: 10.1016/j.semcdb.2016.04.009 (View)
Rossella Cannarella, Rosita A Condorelli, Laura M Mongioì, Sandro La Vignera, Aldo E Calogero. Molecular Biology of Spermatogenesis: Novel Targets of Apparently Idiopathic Male Infertility. Int J Mol Sci. 2020 Mar 3;21(5):1728. doi: 10.3390/ijms21051728 (View)
Yi Xiong, Chao Yu, Qianting Zhang. Ubiquitin-Proteasome System-Regulated Protein Degradation in Spermatogenesis. Cells. 2022 Mar 21;11(6):1058. doi: 10.3390/cells11061058 (View)
FAQs from users: 'How long does it take from sperm production to ejaculation?', 'Is sperm production daily?', 'How many spermatozoa do each spermatogonia form?', 'How many sperm are generated from a primary spermatocyte?' and 'How many spermatozoa result from a secondary spermatocyte?'.
Authors and contributors
More information about Cristina Algarra Goosman






Is there a pattern to the creation of spermatozoa or is it done in waves?
Hi Luke,
Spermatozoa are continuously growing so if we were to do a biopsy we would get mature spermatozoa, spermatogonia, primary spermatocytes, secondary spermatocytes… That is to say, gametes in all stages of development since this is produced continuously.
I hope I have helped you,
Best regards
I can’t believe that tiny thing requires such a long process to be produced. I’ve always thought sperm grow faster, but 3 months is too much… wow!!