Folliculogenesis refers to the development of ovarian follicles from primordial follicles to their final stage: the follicle of Graaf. This process involves an increase in follicular size, as well as in its maturational state, as its development progresses.
However, not all ovarian follicles that begin their maturation will complete it. Many of these follicles will degenerate and be lost midway in a process known as atresia.
However, ovarian follicles that are able to complete their development will give rise to a Graafian follicle. This fully mature follicle will be the one that will expel the oocyte inside it through ovulation.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 1.3.
- 1.4.
- 1.5.
- 1.6.
- 2.
- 3.
- 4.
- 4.1.
- 4.2.
- 5.
- 6.
- 7.
- 8.
What are the stages of folliculogenesis?
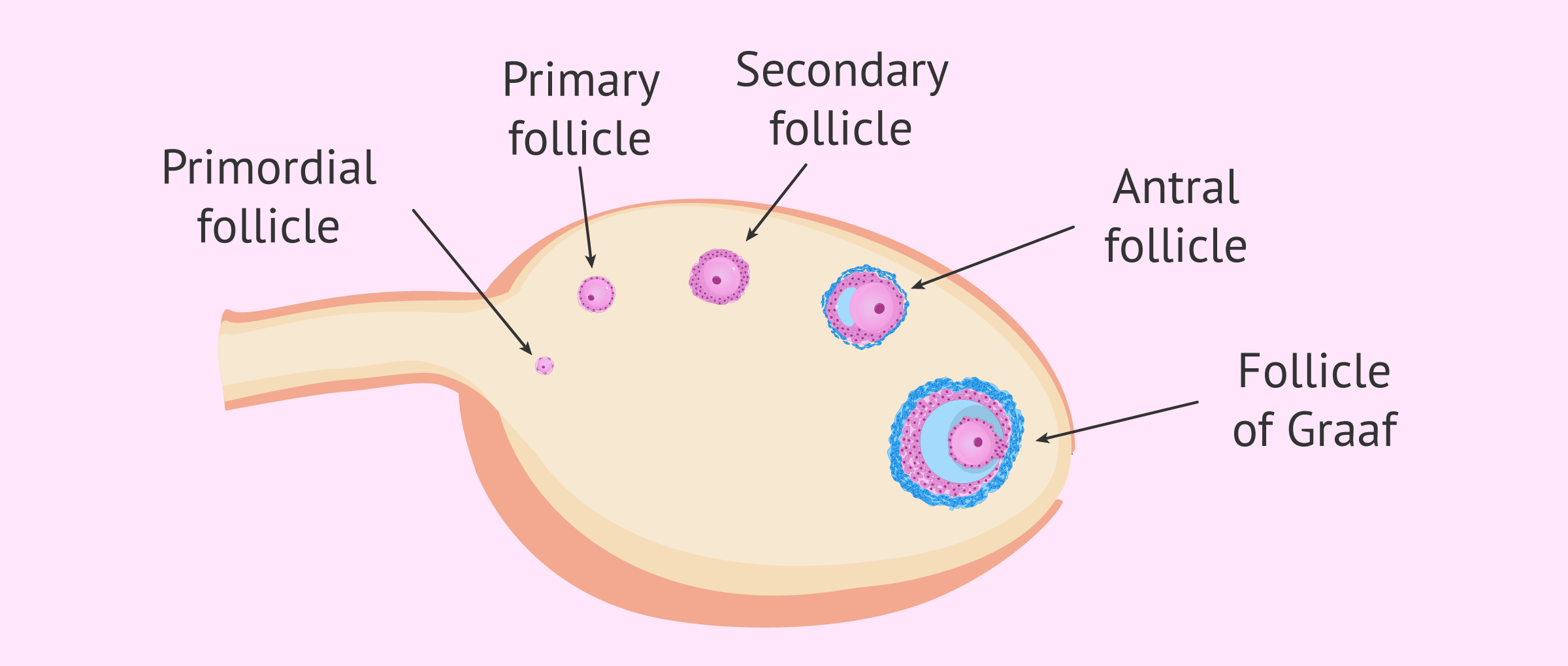
The follicles are located in the ovarian cortex, that is, peripherally in the ovary, and are the structures that contain the oocytes. As the follicular development process progresses, the follicles are named differently, which determines the different phases of folliculogenesis.
It is especially important to mention that folliculogenesis is a highly regulated and controlled process. In addition, interactions occur between the cells surrounding the oocyte (and forming part of the follicle) and between these cells and the oocyte itself.
Primordial follicle
The primordial follicle constitutes the first stage of follicular development. It is a follicle formed by an oocyte that is surrounded by a single layer of flattened pre-granulosa cells.
These primordial follicles are formed in the fetal period of the female, beginning to form in approximately the third month of gestation. Although about 5 million primordial follicles are formed, after the fifth month of gestation many of them die due to atresia. Thus, a woman is born with a certain and finite number of oocytes, which are found in these primordial follicles.
The approximate number of primordial follicles contained in a woman's ovaries at birth is 1-2 million, being only about 500,000 at the time of puberty. The loss of primordial follicles is constant until they are exhausted when a woman reaches menopause.
Primordial follicle
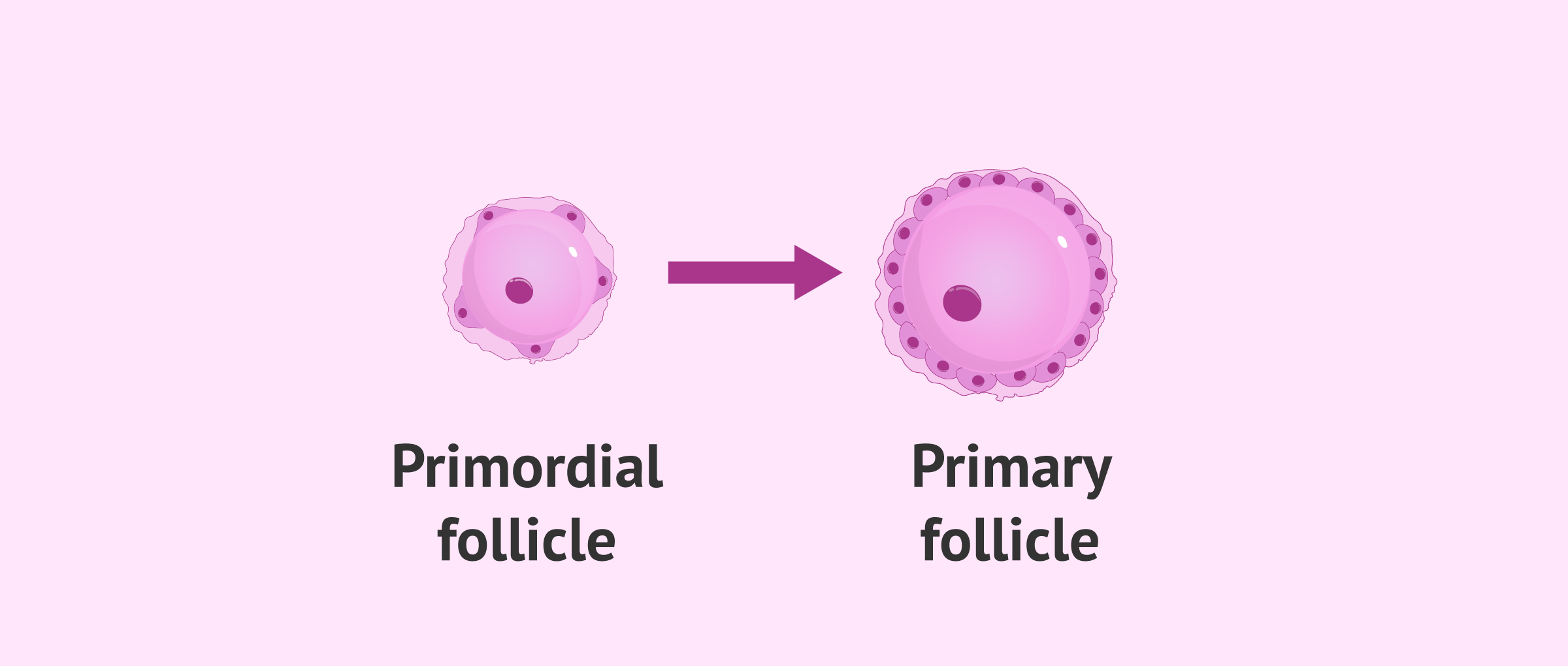
The primordial follicles constitute the "reserve" from which some of them will be stimulated to advance in their development to primary follicles.
In the primary follicle stage, the flat cells that surrounded the oocyte in the primordial follicle now become cubic (die-shaped) granulosacells. In addition, the oocyte itself increases in size.
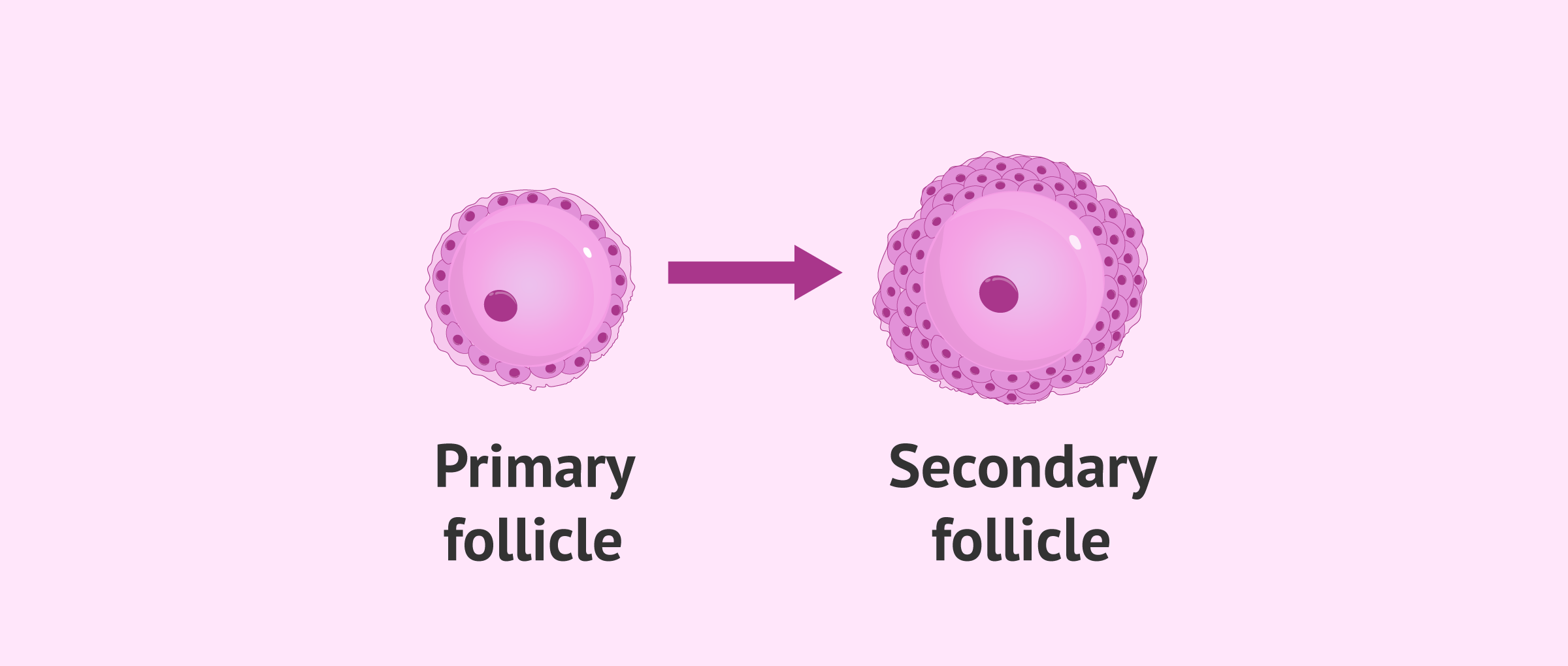
Secondary follicle
In the secondary follicle stage, the granulosa cell layers surrounding the oocyte are several, between 6 and 7.
On the other hand, the zona pellucida that will surround the oocyte, which is composed of glycoproteins, also begins to form in the secondary follicle.
Preantral follicle
At this pre-antral follicle stage, the granulosa cells continue to increase. In addition, the oocyte will also be surrounded by the cells of the theca, which will constitute the inner theca and the outer theca.
However, the most characteristic feature of this preantral stage is that the granulosa cells will acquire receptors for FSH (follicle-stimulating hormone). Thus, follicular development from the early antral stage onwards becomes gonadotropin-dependent.
Antral follicle
The antral (or tertiary) follicle is characterized by the presence of a cavity filled with follicular fluid, known as the antrum antrum.
As mentioned, the development of these follicles is now dependent on gonadotropins (FSH and LH). With the onset of puberty, menstrual cycles begin. This means that in the follicular phase of each menstrual cycle, due to the increase of FSH, there will be a recruitment of several of these follicles that will continue their development. However, many of them will not be able to continue their maturation because of the subsequent drop in FSH levels.
In this way, a process of follicular selection and dominance is established. This means that many follicles will enter atresia and only one of them, the most capable, will be able to complete its development in each menstrual cycle. This follicle is called the dominant follicle.
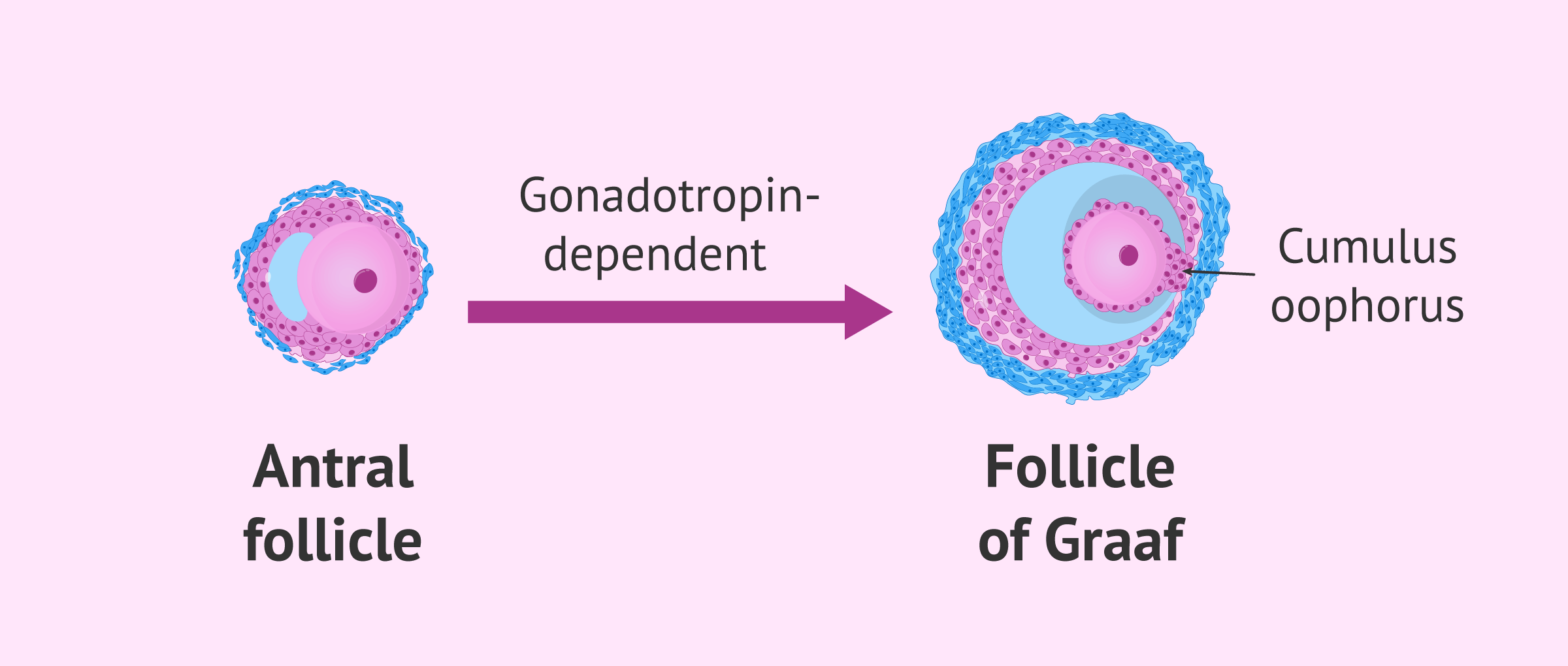
Graaf follicle
The Graafian or pre-ovulatory follicle is the fully developed follicle, which will lead to ovulation of the oocyte it contains. Due to the growth of the antrum, the oocyte is located in one of the sides of the follicle. The oocyte, however, remains surrounded by granulosa cells, forming the cumulus oophorus or cumulus.
When the gonadotropin peak occurs in the middle of the menstrual cycle, the cells of the Graafian follicle cumulus will produce hyaluronic acid. As a consequence, the cumulus will increase in size and acquire a "mucus" consistency. This process is known as mucification of the cumulus and is essential for ovulation to occur.
On the other hand, once ovulation has taken place, the remaining follicular cells left in the ovary will give rise to the corpus luteum. This structure will produce estrogens and, in greater quantity, progesterone that will prepare the endometrium for possible embryo implantation. If pregnancy occurs, the corpus luteum will remain until approximately the fourth month of pregnancy. Conversely, if there is no gestation in that menstrual cycle, the corpus luteum degenerates.
Hormonal control
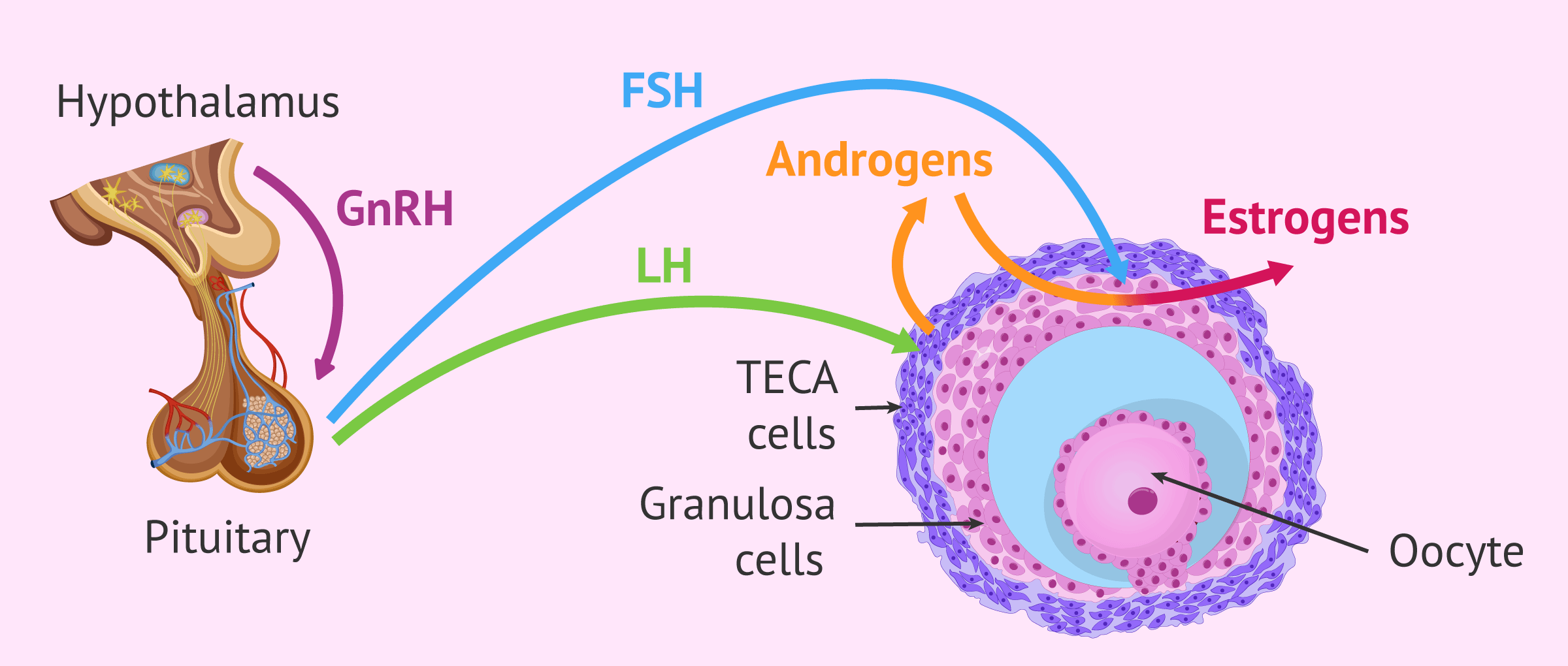
As we have seen, follicular development from the early antral follicle will depend on gonadotropin hormones, especially FSH. However, we cannot forget that the release of these hormones by the pituitary gland depends on the gonadotropin-releasing hormone (GnRH) produced by the hypothalamus.
In turn, LH will promote androgen production in the follicular theca cells. These androgens may be converted to estrogens in the granulosa cells by the action of FSH. Thus, the estrogen surge produced by the dominant follicle is very important in controlling the cycle, as this is what will induce the LH surge necessary for ovulation.
If you wish to learn more about this topic, we recommend you to read this article: The menstrual cycle: what happens in each of its phases?
Folliculogenesis - Ovogenesis
The mature follicle must also expel a mature egg at ovulation. This is why the development and maturation of the oocyte, i.e., ovogenesis, must occur in parallel with folliculogenesis.
The primordial follicles will contain primary oocytes arrested in the prophase of the first division of meiosis. Once puberty arrives, these primary oocytes will be able to continue their maturation. However, for this to occur, it is necessary that the follicle that contains them also advances in its development.
Meiosis is a special type of cell division to create gametes (eggs and sperm), since it is necessary that the number of chromosomes of the cell of origin is reduced by half.
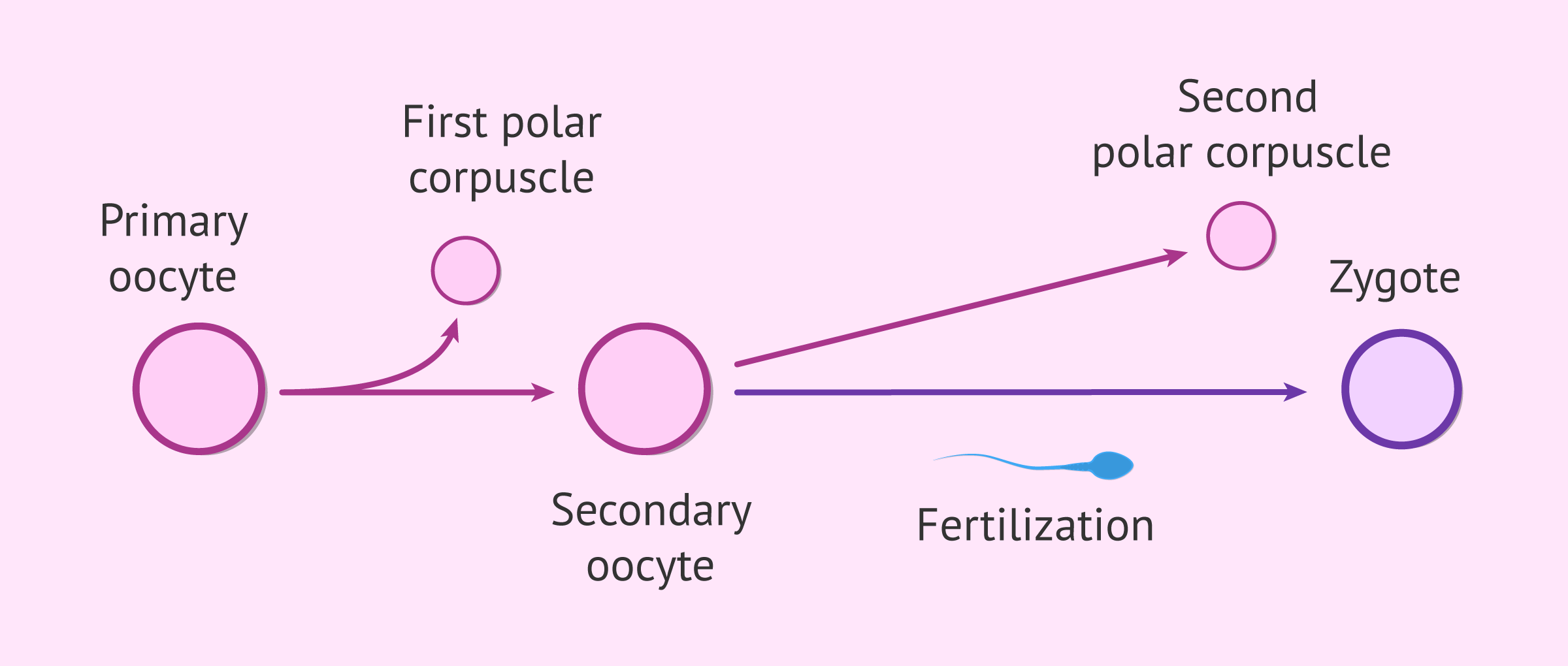
In Graafian follicles, just before ovulation, the peak of luteinizing hormone (LH) triggers the oocyte to resume meiosis. In this way, the primary oocyte will give rise to a secondary oocyte and the first polar corpuscle. This process could be related to the mucification of the cumulus explained above, since this expansion of the cumulus would diminish the inhibitory effect of meiosis that the surrounding cells would be exerting on the oocyte.
The secondary oocyte generated will be arrested in the metaphase of meiosis II and will be ovulated at this stage, considered mature, to the fallopian tubes. Finally, the secondary oocyte will be able to complete meiosis if fertilization by a sperm occurs. If this occurs, the secondary oocyte will produce a fertilized egg (zygote) and the second polar corpuscle.
Otherwise, if not fertilized, the secondary oocyte will degenerate.
You have much more information about the process of meiosis in this article: What is the relationship between meiosis and fertility.
FAQs from users
What is the duration of folliculogenesis?
A primordial follicle can spend years in "quiescence" until it initiates its development. Subsequently, once initiated, it takes approximately 150 days for a primordial follicle to become a Graafian follicle. This means that the follicle that will ovulate in a given menstrual cycle began to develop about 5 menstrual cycles earlier, along with many other follicles that have been lost during their development due to atresia.
What is the relationship between ovarian stimulation in assisted reproduction treatments and folliculogenesis?
Ovarian stimulation in assisted reproduction treatments is aimed at the development and maturation of several follicles, unlike what occurs in a normal menstrual cycle in which a dominance is established that leads to the development of a single follicle.
This "multiple" follicular development of ovarian stimulation is achieved by the administration of gonadotropins, since folliculogenesis from the pre-antral follicle is dependent on these hormones. In this way, it prevents the loss of follicles that would go into atresia in a natural menstrual cycle in favor of the dominant follicle, so that several of these follicles will be able to continue their development.
Recommended readings
Throughout the article, we have constantly mentioned ovulation. If you are interested in learning more about this topic, we recommend you to visit this link: When does ovulation occur and what are the symptoms?
On the contrary, if you are interested in learning more about gonadotropins, you can read the article: Gonadotropins: What are they and what are their functions?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Baerwald AR, Adams GP, Pierson RA. Ovarian antral folliculogenesis during the human menstrual cycle: a review. Hum Reprod Update. 2012 Jan-Feb;18(1):73-91.
Gershon E, Dekel N. Newly Identified Regulators of Ovarian Folliculogenesis and Ovulation. Int J Mol Sci. 2020 Jun 26;21(12):4565.
Hsueh AJ, Kawamura K, Cheng Y, Fauser BC. Intraovarian control of early folliculogenesis. Endocr Rev. 2015 Feb;36(1):1-24.
Rimon-Dahari N, Yerushalmi-Heinemann L, Alyagor L, Dekel N. Ovarian Folliculogenesis. Results Probl Cell Differ. 2016;58:167-90.
FAQs from users: 'What is the duration of folliculogenesis?' and 'What is the relationship between ovarian stimulation in assisted reproduction treatments and folliculogenesis?'.
Author
More information about Cristina Algarra Goosman



Hi, I am 39 years old and I am going to start IVF treatment. There is one thing that is not clear to me if I already have a low ovarian reserve if I do a stimulation I will not be losing more follicles than I would normally lose? I don’t want to lose opportunities
Hello Spencer,
The ovarian stimulation that is performed in the first steps of IVF treatment aims to allow the development of all the follicles that would not get to develop and therefore the body would eliminate (atresia).
Therefore, you would not be discarding more follicles than your body would naturally do, but you would be taking advantage of the ones your body discards.
I hope I have helped you.
Best regards
Hi, I have a problem, when I have anovulatory cycles what does it mean? I can’t get pregnant and I’ve been told it’s a problem with the follicles.
Hello Aleeah,
Anovulatory cycles are characteristic of ovulation failure, i.e. the ovary does not release an egg monthly, therefore, there is no chance of achieving pregnancy.
I recommend that you read this article: What is anovulation? In it, we explain the different causes and treatments for this situation.
I hope I have helped you.
Best regards.