Embryo implantation is the process by which the embryo, which is about 7 days old since fertilization, attaches to the endometrium and begins gestation. After this, the embryo will begin its development and that of the structures that allow its nutrition, such as the vitelline vesicle and the placenta.
In addition, the synthesis of the beta-hCG hormone will also begin and the woman will feel the first symptoms of pregnancy.
On the other hand, so that the embryo can implant in the endometrium and give rise to an evolving pregnancy, it is essential that this uterine layer acquires certain characteristics of thickness and appearance.
Provided below is an index with the 9 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 4.
- 5.
- 5.1.
- 5.2.
- 5.3.
- 5.4.
- 5.5.
- 5.6.
- 5.7.
- 5.8.
- 5.9.
- 5.10.
- 5.11.
- 6.
- 7.
- 8.
- 9.
Conditions for implantation
Embryo implantation is not achieved in all menstrual cycles even if you have unprotected sex during fertile days. The proper uterine environment needs to be created, where the endometrium and embryo can interact.
Thus, implantation is also not 100% safe in assisted reproduction cycles, even though fertilization has taken place in the laboratory and good-quality embryos are transferred.
In the following section, we are going to discuss the most important factors for the implantation of an embryo to take place and thereby achieve pregnancy.
Factors related to the embryo
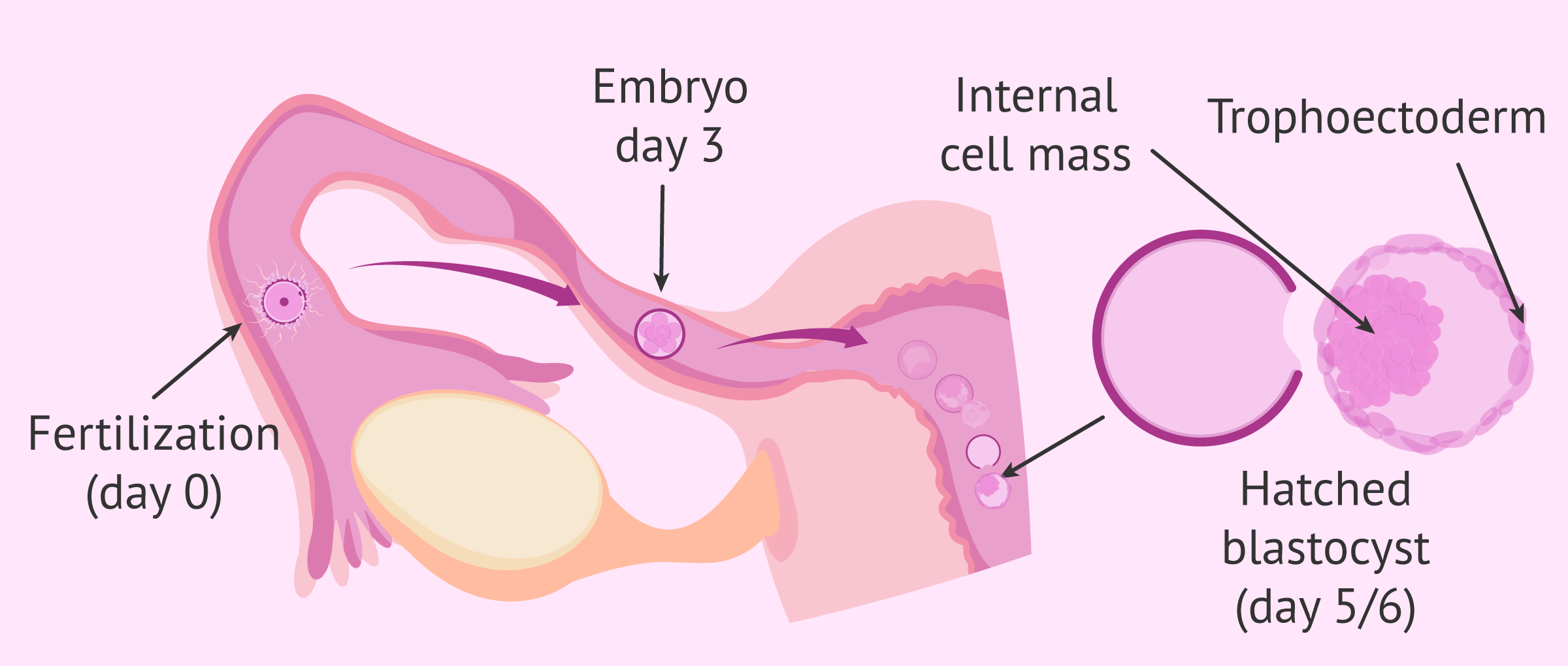
For an embryo to be able to join the endometrium, it must be in the blastocyst stage. At this point in its development, it has about 200-400 cells and is made up of two well-differentiated parts:
- Internal cell mass
- cells that will give rise to the embryo itself.
- Trophoectoderm
- are the outermost cells that will form the placenta and other embryonic attachments.
Additionally, prior to implantation, the blastocyst must also have detached from its zona pellucida, the outer layer that surrounds it, and have reached its maximum degree of expansion: the hatched blastocyst.
Another crucial factor that will determine whether implantation occurs is embryo quality, which can only be evaluated in patients undergoing in vitro fertilization (IVF) treatment.
On the other hand, in cycles where fertilization occurs naturally in the fallopian tubes, the correct transport of the embryo from the tube to the uterus must also occur.
Factors related to the endometrium
The endometrium is the innermost layer of the uterus, which is renewed in each menstrual cycle in order to accommodate the embryo during pregnancy. For this reason, if implantation does not take place, the endometrium is shed and eliminated each month in the form of menstruation.
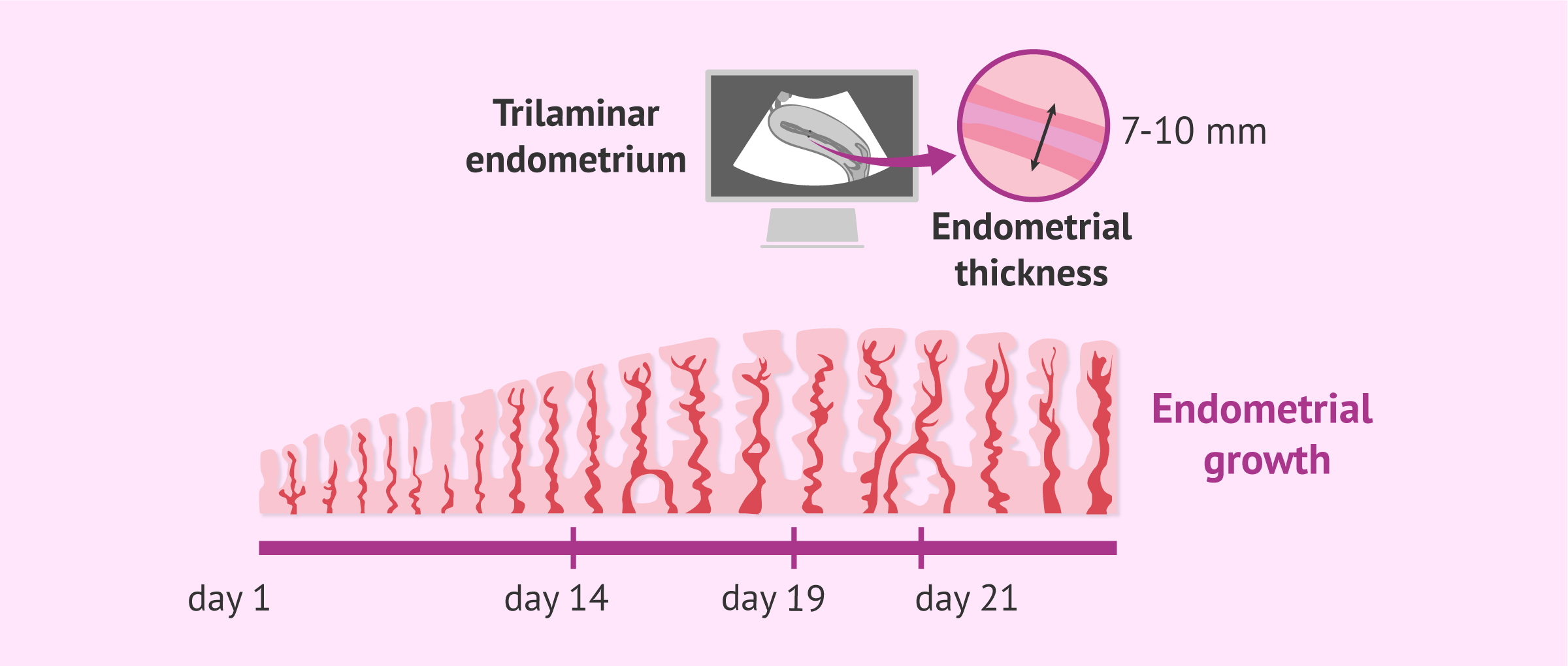
Throughout the menstrual cycle, the endometrium thickens little by little and undergoes changes thanks to the action of the female sex hormones: estrogens and progesterone.
For embryo implantation to occur, the endometrium must be receptive. This is achieved when its endometrial thickness is between 7-10 mm and its appearance is trilaminar.
In addition to this, it is also necessary to express certain molecules in the uterus, such as cytokines, integrins, adhesion molecules, and growth factors, which are responsible for mediating a close dialogue with the embryo.
When does implantation occur?
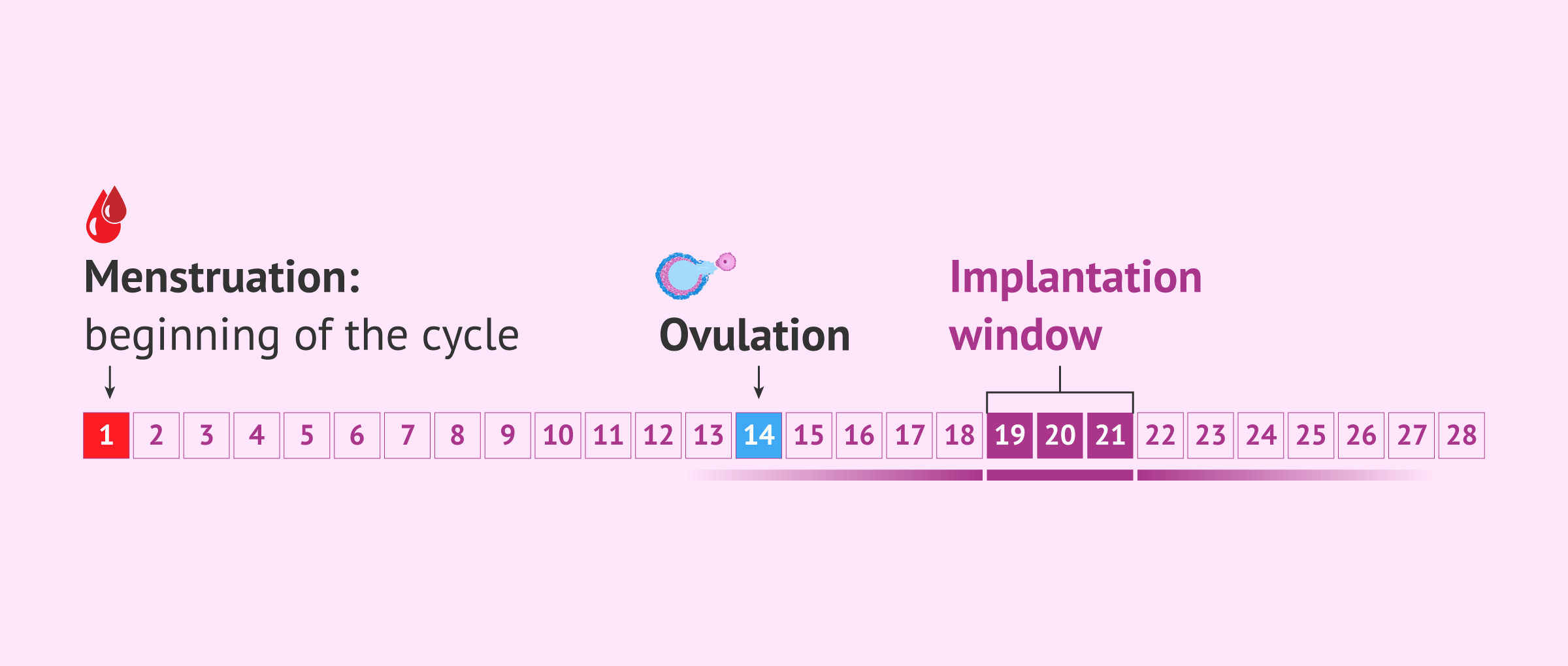
As we have already said, the nesting of the embryo will only take place when the endometrium is receptive. This time of the menstrual cycle is known as the implantation window and has an approximate duration of 4 days.
In most women, the implantation window runs from day 19 to day 21 of the menstrual cycle. At this time, if there has been fertilization, the blastocyst will be about 6 or 7 days old and ready to implant.
However, there are women with the implantation window displaced, which can lead to implantation failure and sterility.
In short, implantation occurs at a specific time in the menstrual cycle, when the endometrium changes from a nonreceptive to a receptive state under the hormonal influence and there is a synchrony between embryo and endometrium.
Phases of implantation
Once the dialogue between the embryo and the maternal endometrium has been established, the embryo implantation or nesting, which usually takes place in the middle third of the posterior face of the uterus, begins.
In the section below, we are going to describe each of the phases into which this implementation period is divided.
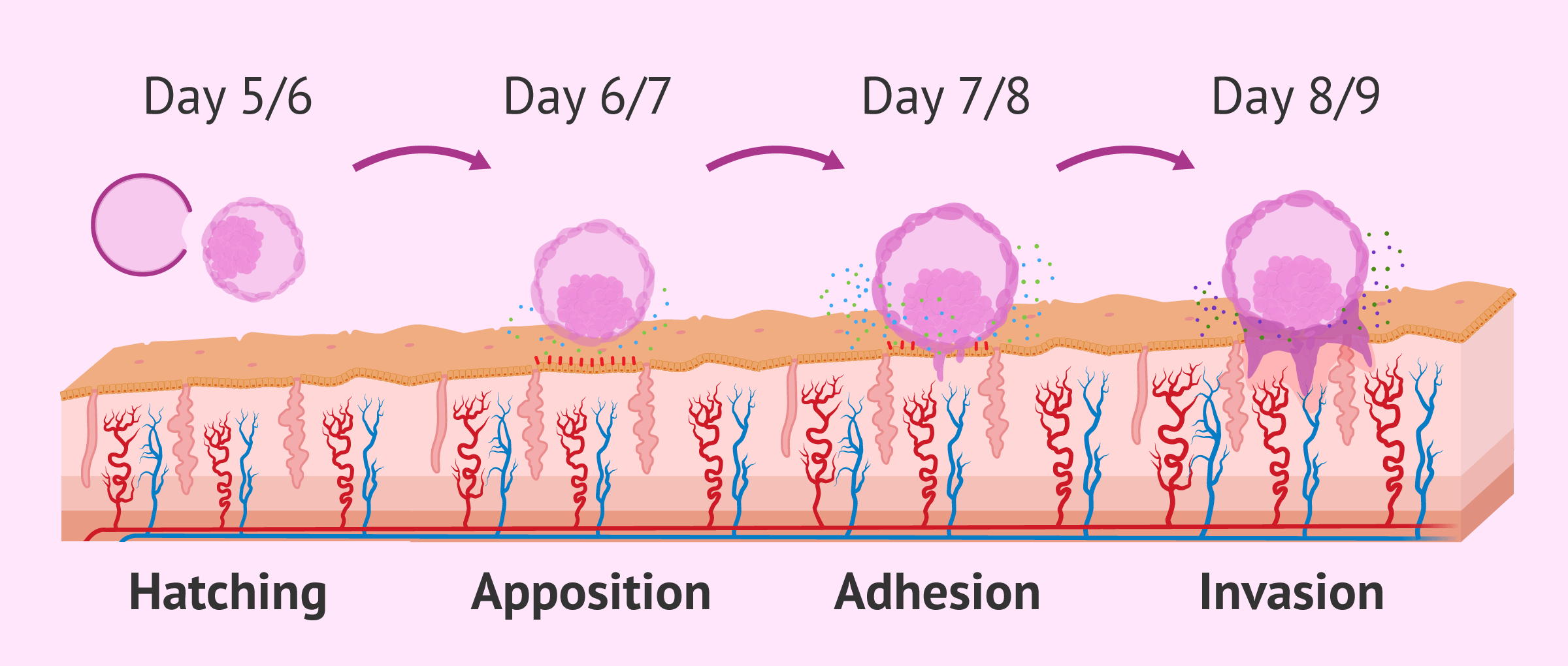
Hatching and pre-contact
On days 5 and 6 of development, the embryo begins to hatch until it detaches from its zona pellucida, the external protein membrane that protects it in its first days after fertilization.
As the embryo increases in size, the zona pellucida becomes thinner until it finally breaks down. Finally, the embryo manages to leave it through a series of contractions and begins to interact with the endometrium.
In patients undergoing IVF treatment, blastocysts that have already hatched can be transferred to the uterus, either because hatching has occurred in culture or because assisted hatching has been performed. Assisted hatching may favor embryo implantation.
If you are interested in reading about this, you can access the next post: assisted hatching prior to embryo transfer.
Apposition
During this phase, the embryo seeks its position on the endometrial tissue and remains immobile while it is oriented so that its internal cell mass points towards the endometrium to allow the proper formation of the placenta later on.
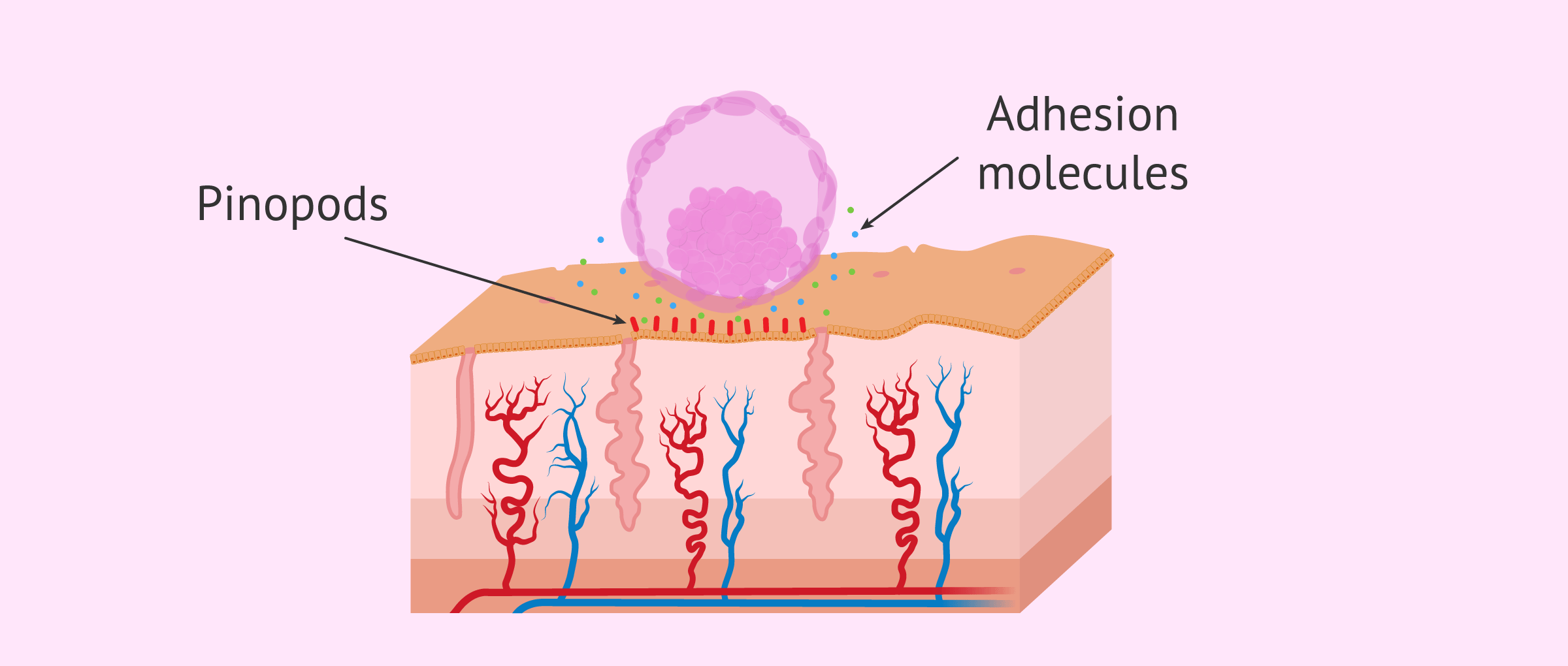
Here, the purported pinopods play an important role: These are the cytoplasmic projections of endometrial epithelial cells that help the blastocyst come into contact.
It is proven that these pinopods are clear morphological markers of endometrial receptivity and only appear during the implantation window, disappearing around the 24th day of the cycle.
Adhesion
The blastocyst trophoectoderm adheres to the endometrial epithelium and is united by the action of the adhesion molecules: integrins β1, β3, and β4, L-selectins, proteoglucans, fibronectins, etc.
This happens about 7 days after fertilization, when the blastocyst already has a diameter of 300-400 µm.
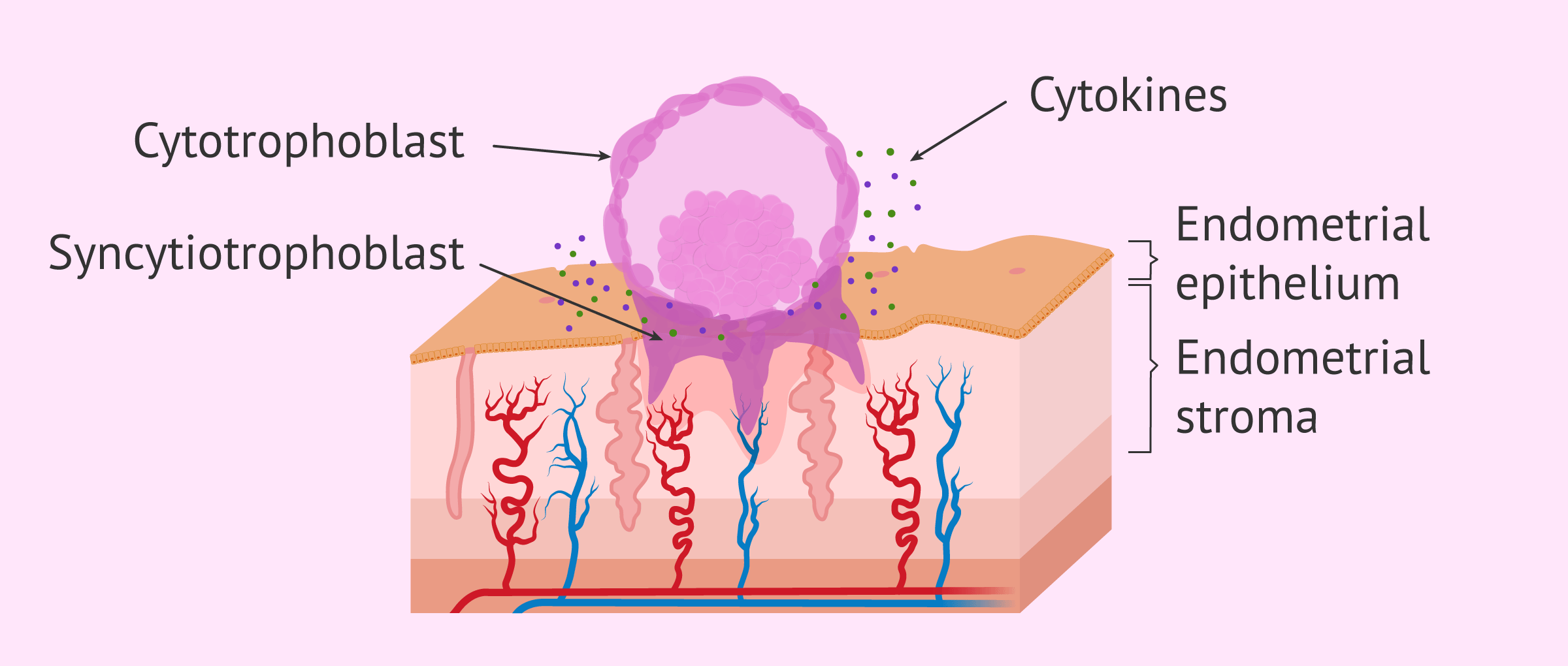
Invasion
The blastocyst, more specifically the trophoblast or embryonic trophectoderm, proliferates towards the endometrium, displaces the epithelial cells, and finally invades the endometrial stroma, making contact with the maternal blood.
This entire invasion mechanism is controlled by cytokines, molecules that act as mediators of implantation and allow dialogue between the embryo and the endometrium.
In response to this dialogue, the blastocyst is activated and initiates differentiation of the trophoblast into cytotrophoblast and syncytiotrophoblast.
Specifically, the syncytiotrophoblast is the one that acquires the invasive capacity. It synthesizes proteolytic enzymes such as serinproteases, metalloproteinases, and collagenases that break the basement membrane of the endometrial epithelium and allow the complete entry of the blastocyst.
This destruction of the endometrium during the penetration of the syncytiotrophoblast is the cause of the slight vaginal bleeding that some women suffer and that can be confused with abnormal menstruation. It's the known implantation bleeding.
Although at first glance it may seem simple for a blastocyst to be implanted in the maternal endometrium, this process is highly complex and not yet fully known.
Symptoms of embryo implantation
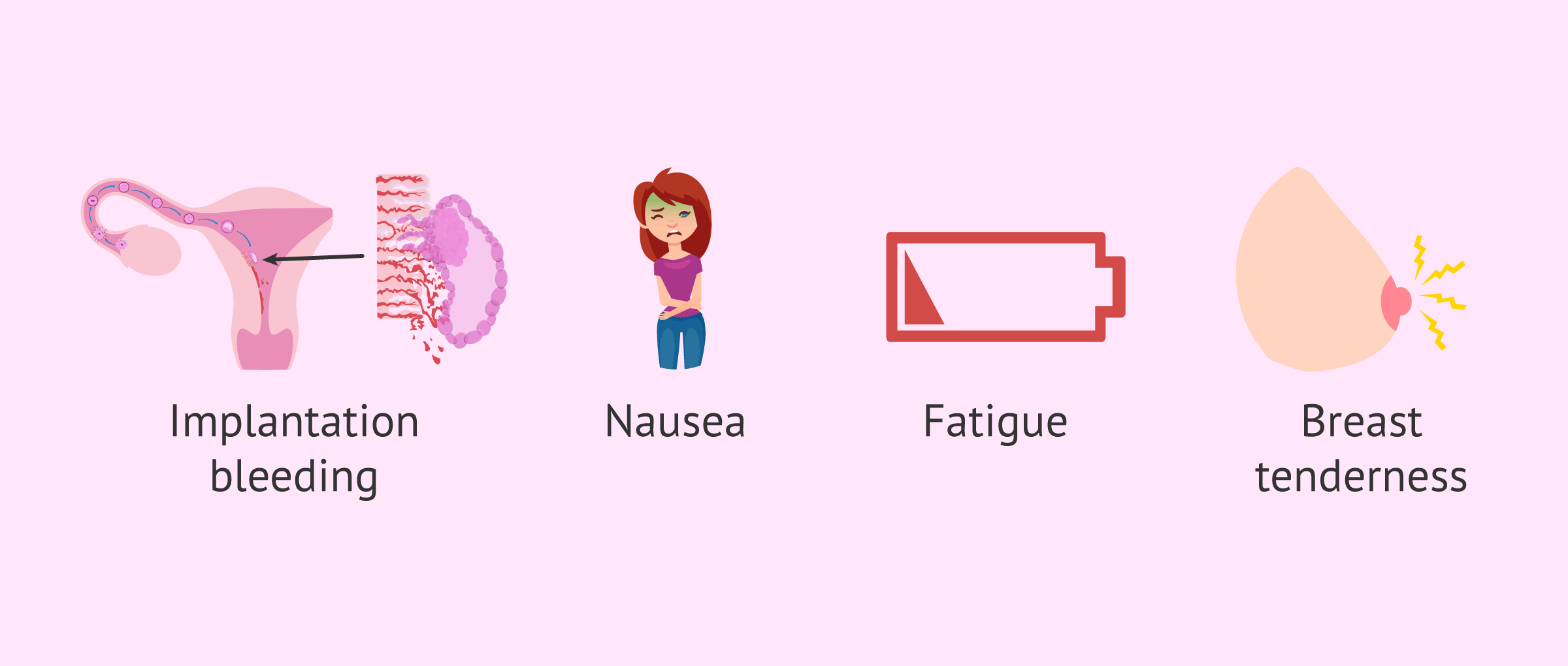
As we have already mentioned, once the embryo invades the endometrium and penetrates it, a small amount of bleeding known as implantation bleeding occurs. This spotting is lighter than that of menstruation and, in addition, its duration is shorter. However, many women confuse implantation bleeding with menstrual bleeding.
Another change that also occurs after embryo implantation is the increase in the levels of human chorionic gonadotropin hormone or hCG, as well as estrogen and progesterone levels. Therefore, women may experience nausea, fatigue, breast tenderness, etc. as a result of embryo implantation and hormonal changes.
However, the absence of symptoms after embryo implantation does not mean anything wrong. Each woman is different and not having discomfort does not mean that implantation has not occurred.
We recommend you read the following article for more information: What is implantation bleeding? Characteristics, signs and symptoms.
FAQs from users
Does stress affect embryo implantation?
Embryo implantation is a complex process in which several factors are involved. It is a dialogue that takes place between the transferred embryo and the properly prepared endometrium at that time. Most of the research on the interaction between emotional stress and infertility over the last 30 years has shown that, although infertility causes stress, stress does not necessarily cause infertility. However, acute and chronic stress can reduce the success rate of fertility treatments.
Stress acts by different mechanisms and its correct assessment requires a collaboration between gynecology, biology and psychology. The available evidence determines that the fertility treatment protocol should include stress management and stress reduction as factors of major importance.
For this purpose, there are various psychological methods such as cognitive behavioral therapy or adequate training in relaxation techniques that help to reduce stress levels. Therefore, it is important to have an initial psychological assessment to evaluate stressors that may interfere with the reproductive health of both members of the couple, whether to initiate assisted reproduction treatment, or in any couple with infertility, whatever its origin.
How important are cytokines in the embryo implantation process?
Cytokines are proteins that regulate interactions between different cells in the body and therefore contribute to the "dialogue" between them. It is logical to think that this interaction or dialogue between the endometrium and the embryo is modulated, among others, by this set of proteins called cytokines. Their function is key, and each day it is understood a little better what is the role they play and what is their true relevance.
Can stress influence the embryo implantation process?
Yes, stress can influence the embryo implantation process, although its exact impact remains under study. From a biological and clinical perspective, physical or psychological stress can alter several mechanisms involved in implantation.
Read more
Can transvaginal ultrasound affect embryo implantation?
Antonio Forgiarini, gynaecologist at the Next Fertility clinic in Valencia answers us in this video:
No, there is no reason to think that it could happen. We use transvaginal ultrasound normally with a recent pregnancy or during the controls, in the first ecography after the the embryo transfer or sometimes while we do the transfer. It's a a very hard moment but, if we cannot see the uterus with transabdominal ecography, we can use the transvaginal one and we have absolutely good results as pregnancies.
What is the difference between fertilization and implantation?
Fertilization is the union between the egg and the sperm to create a new being: the embryo, which will develop during pregnancy. Implantation, on the other hand, is the process by which the embryo enters the endometrium (the layer that lines the uterus internally) in order to form the placenta and thus be able to nourish and grow during pregnancy.
Does the egg, the zygote, embryo or fetus implant?
The embryo is the one that penetrates the endometrium during implantation. Once fertilization occurs, we are no longer talking about egg, but zygote. Once the zygote is formed, it is divided to give rise to what we call embryo. From the 8th week of pregnancy, the embryo is called fetus.
For more information about the differences, refer to the following article: What is the difference between zygote, embryo and fetus?
Does embryo implantation slightly hurt?
A slight discomfort may be noticed as in menstruation, but there is no significant pain. Normally, the woman does not notice anything and does not realize that implantation has taken place until the pregnancy test is done and she tests positive.
Is an anormal implanation of the embryo possible?
Yes, it can implant in the wrong place outside the uterus. This is called ectopic pregnancy and can occur, for example, in the fallopian tubes.
It is also possible for the embryo to implant correctly in the endometrium but not be able to continue its development, i.e. give rise to a non-evolutionary gestation. This can occur because there is some alteration in the embryo, either in its development or in its genes.
An example of non-evolutionary gestation is the biochemical pregnancy, in which the gestational sac is formed, but there is no fetus inside. In this type of pregnancy a spontaneous abortion occurs, usually very early.
How do I know if the embryo has implanted? Are there symptoms?
To know if there has been implantation, a pregnancy test must be done. It is necessary to wait either 15 days after ovulation, or until the period is delayed, for the result of this test to be reliable.
The woman may also have symptoms of pregnancy such as implantation bleeding.
You may consult this article to find out more about the symptoms that may appear after embryo implantation: First signs of embryo implantation.
Can you favor embryo implantation?
There are a number of tricks that can help improve the chances of implantation. Having a positive mood, reducing stress, maintaining a balanced diet, exercising moderately and avoiding harmful substances such as alcohol, tobacco and caffeine can help implantation to some extent.
How many days does it take for the fertilized egg to implant?
Implantation of the embryo takes approximately 4-5 days, from the time the blastocyst hatches until the trofoectoderm completely invades the endometrium.
This occurs between days 5 and 8 of embryonic development, i.e., this is the time it takes for the embryo to implant after fertilization between the egg and sperm.
Recommended readings
In the course of gestation, embryo implantation occurs in the fourth week of pregnancy, before the beginning of the second month. If you want to know all the details that happen in this week, you can read more here: 4 weeks pregnant: embryo implantation in the uterus.
For women seeking pregnancy through assisted reproduction, proper endometrial preparation is essential for embryo implantation to take place. You can read more about this in the following article: How will the endometrium for the embryo transfer be prepared?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Borini A, Lagalla C, Cattoli M, Sereni E, Sciajno R, Flamigni C, Coticchio G: Predictive factors for embryo implantation potential. Reprod Biomed Online 2005, 10:653–668 (View)
Joanne Muter, Vincent J Lynch, Rajiv C McCoy, Jan J Brosens. Human embryo implantation. Development. 2023 May 15;150(10):dev201507. doi: 10.1242/dev.201507 (View)
Mardon H, Grewal S, Mills K. Experimental models for investigating implantation of the human embryo. Semin Reprod Med 2007; 25:410 – 417 (View)
Norberto López Serna. Biología del desarrollo. Cuaderno de trabajo. Capítulo 9: Implantación. McGraw-Hill 2012; ISBN: 978-607-15-0657-3
Shuang Zhang, Haiyan Lin, Shuangbo Kong, Shumin Wang, Hongmei Wang, Haibin Wang, D Randall Armant. Physiological and molecular determinants of embryo implantation. Mol Aspects Med. 2013 Oct;34(5):939-80. doi: 10.1016/j.mam.2012.12.011 (View)
Wan-Tinn Teh, John McBain, Peter Rogers. What is the contribution of embryo-endometrial asynchrony to implantation failure? J Assist Reprod Genet. 2016 Nov;33(11):1419-1430. doi: 10.1007/s10815-016-0773-6 (View)
FAQs from users: 'Does stress affect embryo implantation?', 'How important are cytokines in the embryo implantation process?', 'Can stress influence the embryo implantation process?', 'Can transvaginal ultrasound affect embryo implantation?', 'What is the difference between fertilization and implantation?', 'Does the egg, the zygote, embryo or fetus implant?', 'Does embryo implantation slightly hurt?', 'Is an anormal implanation of the embryo possible?', 'How do I know if the embryo has implanted? Are there symptoms?', 'Can you favor embryo implantation?' and 'How many days does it take for the fertilized egg to implant?'.
Authors and contributors

More information about Cristina Algarra Goosman









I have the same pain in my lower side of stomach after an ICSI treatment, it is normal or what? Please, I am worried about it.
Yes, this is a common post embryo transfer symptom. Don’t worry 😉