Embryo implantation is the process by which an embryo attaches to the endometrium of the woman's uterus. This occurs about 7 days after fertilization and is an essential event for gestation to begin, whether it is sought naturally or by assisted reproduction techniques.
Although it may seem simple, the truth is that implantation requires that the embryo and the endometrium are in the right conditions and that there is perfect synchrony between the two. For this reason, both embryonic and endometrial factors could affect implantation.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 1.3.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 5.
- 6.
- 7.
- 8.
Embryonic factor
It is logical to think that the embryo has a lot to say at the moment of implantation. In addition, the embryo transfer technique itself must be very careful, so that it is as atraumatic as possible for the embryo and the uterus.
Embryo quality
The quality of the embryo that is transferred is related to its chances of implantation. Thus, A-quality embryos (optimal quality) are more likely to implant than C-quality embryos (intermediate quality).
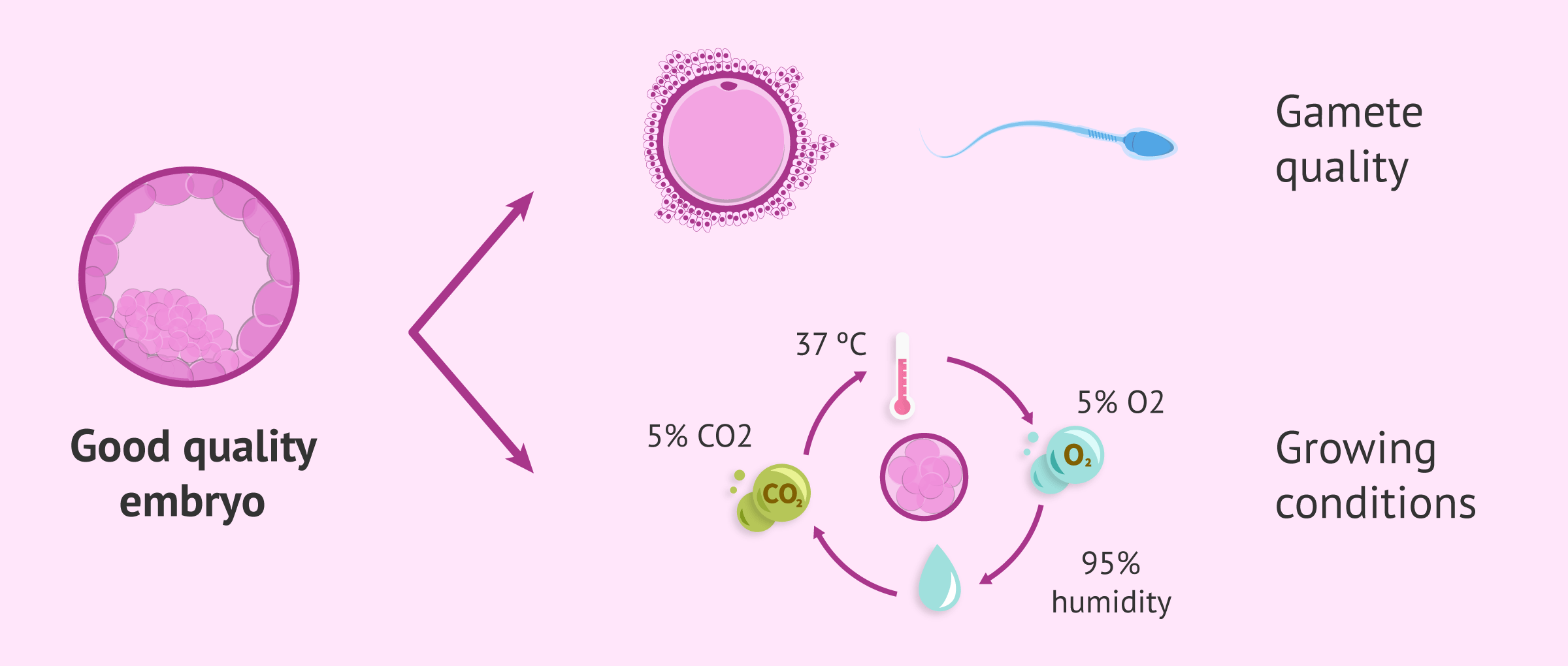
Although embryo quality is largely determined by the quality of the gametes (egg and sperm), achieving good quality embryos will also depend on the laboratory. It is essential to have the required technical and human resources, as well as an exhaustive control of the culture conditions, since these must always be optimal to favor embryonic development.
In addition, if the embryo remains in culture in a time-lapse incubator, the selection of the best embryo can be made based on morphokinetic parameters. This means that not only morphological parameters (the appearance of the embryo) are taken into account, but also the kinetics, that is, the times at which certain stages of embryonic development have occurred.
If you want to know more about embryo quality, you can continue reading in this link: How are embryos classified according to their day of development?
Blastocyst transfer
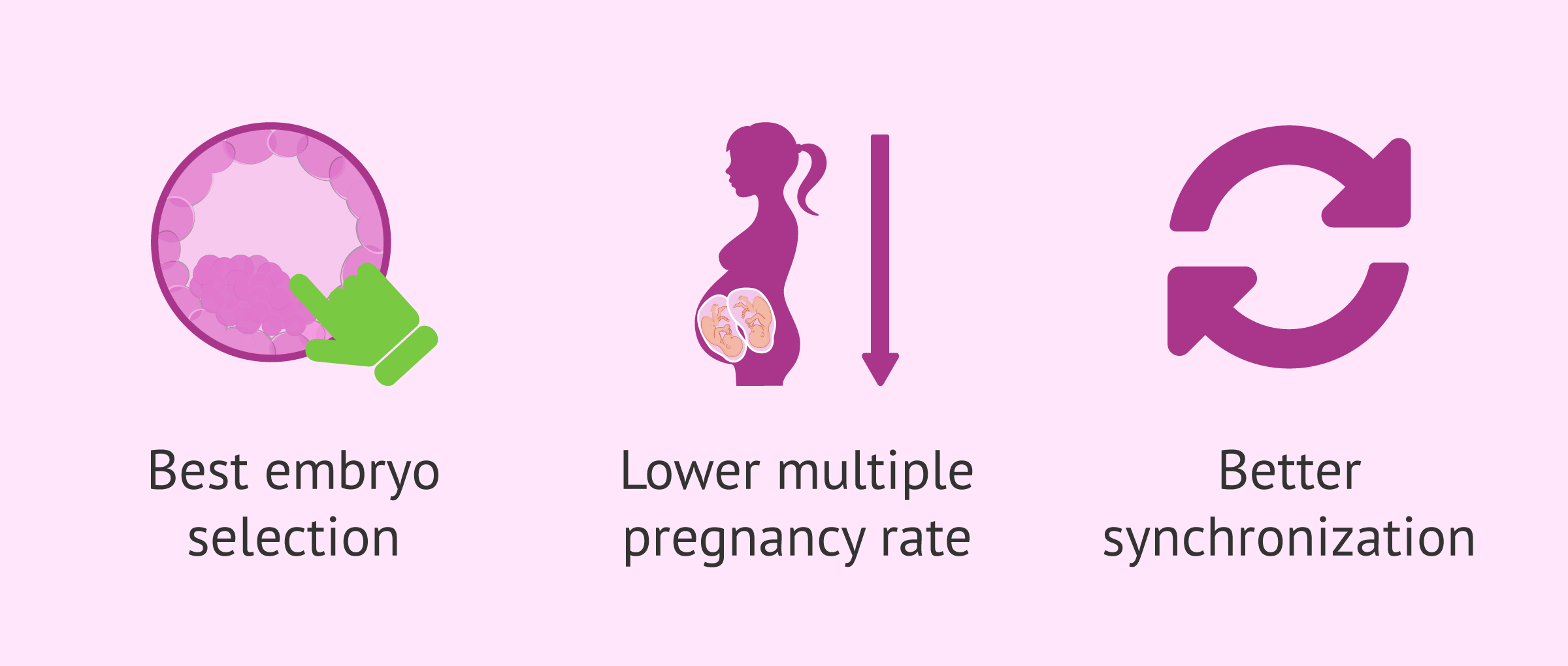
A prolonged culture until blastocyst (day 5 of embryo development) allows a better selection of the embryo to be transferred. With respect to transfer on day 3 of development, prolonged culture allows more information to be obtained from the embryos.
All this translates into a tendency to transfer a single embryo in each transfer, the one with the highest implantation potential. This leads to reduced rates of multiple pregnancy, which has more risks for the mother and the babies.
On the other hand, in a natural conception, the embryo arrives in the woman's uterus around day 4-5 of embryonic development. Therefore, transfer at the blastocyst stage involves better synchronization with the endometrium.
You can read more details about the differences between day 3 and blastocyst-stage embryo transfer in the following article: When to transfer embryos on day 3 or day 5?
Pre-implantation genetic testing (PGT)
Despite all of the above, an embryo that is apparently of good quality may have genetic alterations. Thus, an embryo with an abnormal chromosomal content can result in implantation failure, miscarriage, or the birth of a baby, for example, with Down syndrome.
However, it is now possible to perform a preimplantation genetic test(PGT, formerly known as PGD) on embryos. This test is especially useful in cases of advanced maternal age, repeated miscarriages or repeated implantation failures, and severe malefactors.
PGT consists of extracting a small number of cells from the embryo by embryo biopsy, which will be sent for genetic analysis. The embryos will remain frozen (vitrified) until the results are obtained, which will allow the transfer of only those that have obtained a favorable result.
If you are interested in reading more about this genetic study, you can read the following article: What is preimplantation genetic diagnosis or PGD?
Endometrial factor
As we have already mentioned, the endometrium must be in optimal conditions to receive the embryo. If this does not occur, implantation will be difficult despite the transfer of viable embryos of good quality.
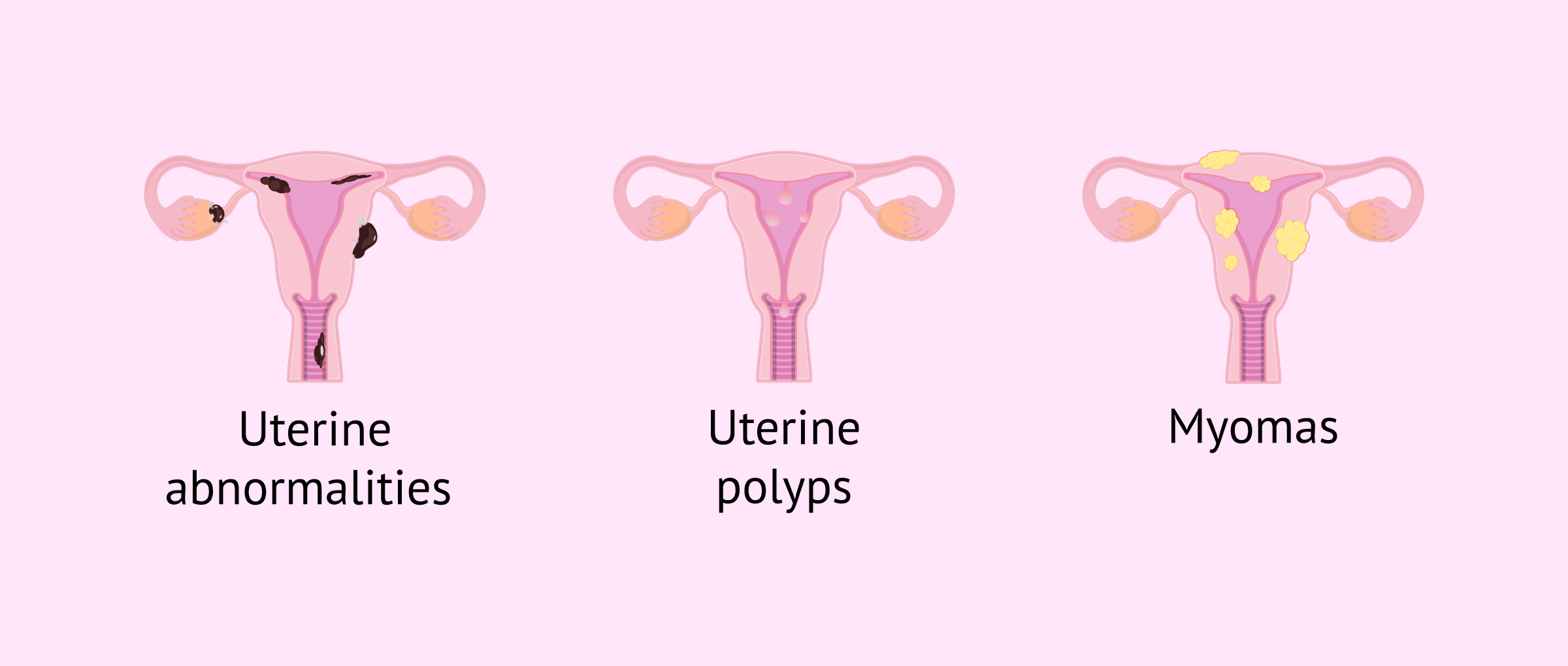
Initially, it is important to know if there is any uterine alteration, or any polyp or myoma that could be affecting implantation. However, there are other aspects of the endometrium that can be analyzed.
Implementation window
In assisted reproduction techniques, the endometrium is usually controlled and prepared with hormonal medication to receive the embryo in optimal conditions. Ultrasonographically, an endometrium is ready for embryo transfer when it has a trilamellar appearance and a thickness of about 7-10 mm.
This type of endometrial preparation becomes especially important when a vitrified embryo transfer is to be performed, or when the embryos come from ovodonation.
However, the window of implantation is sometimes displaced, which can cause implantation failure even when good-quality embryos are transferred.
The window of implantation is the period of time in which the endometrium is receptive to embryo implantation.
However, there are now tests that can analyze endometrial receptivity. Thus, based on an endometrial biopsy, these tests make it possible to know when the best time for embryo transfer is.
If you want to read more information about this type of test, you can access the following link: What is the ERA endometrial receptivity test, and what is it for?
Endometrial microbiome
The endometrial microbiome is an aspect that is being given increasing importance. These are the microorganisms that are present in the uterus, which may be modifying the chances of implantation.
However, today it is possible to study whether there are any bacteria causing endometritis, as well as whether the endometrial microbiome as a whole is the most favorable for implantation.
In addition, this type of test makes a recommendation on the most appropriate treatment based on the results.
You can obtain more information about these tests by accessing the following article: What is the EndomeTRIO test - Indications, and price.
Other aspects
A thrombophilia or immune problem could also be affecting implantation. For gestation to occur, maternal-fetal tolerance is necessary to allow foreign tissue (such as the embryo in the mother's body) to implant in order to continue embryonic development.
Therefore, in certain cases, a study will be necessary to assess these causes. In this way, the specialist will evaluate if the woman needs a treatment that can help the implantation to occur correctly.
At this point, it is important to mention vitamin D. This vitamin seems to be related to embryo implantation due to its anti-inflammatory and immunomodulatory effects.
For this reason, it may be advisable to determine vitamin D levels and whether supplementation is necessary. However, this should always be supervised by the specialist, who will adjust the required dose.
Recommendations
Generally speaking, there are certain tips that could improve embryo implantation:
- Avoid stress. The best thing to do after the embryo transfer is to lead a normal life, as long as the specialist has not indicated otherwise.
- No physical effort Despite being able to perform the daily routine, it is important to avoid activities that require great effort, such as weight-bearing or intense sports. For this reason, depending on the woman's job, sick leave may be appropriate in certain cases.
On the other hand, having good habits is always beneficial, both before and after the transfer. It´s important quitting tobacco and alcohol, as well as control caffeine consumption.
FAQs from users
Can the implantation rate be improved?
Yes, it is possible. For this, it will be necessary to determine the exact moment for the embryo transfer, taking into account the affinity of the endometrium and the maturation of the blastocyst.
Read more
In which cases is assisted hatching recommended?
Assisted hatching is usually used as a complementary technique since in some cases it can help the implantation of the embryo. It involves making a small hole in the pellucid layer that covers the embryo (the area that protects the embryo) to promote hatching (the embryo leaving its membrane) for subsequent implantation.
It is usually recommended for patients who have obtained poor quality embryos in previous treatments, in elderly patients (whose oocytes have a thicker or more hardened membrane) and in implantation failures. It is of great help to use it in the transfer of embryos that have already been cryopreserved.
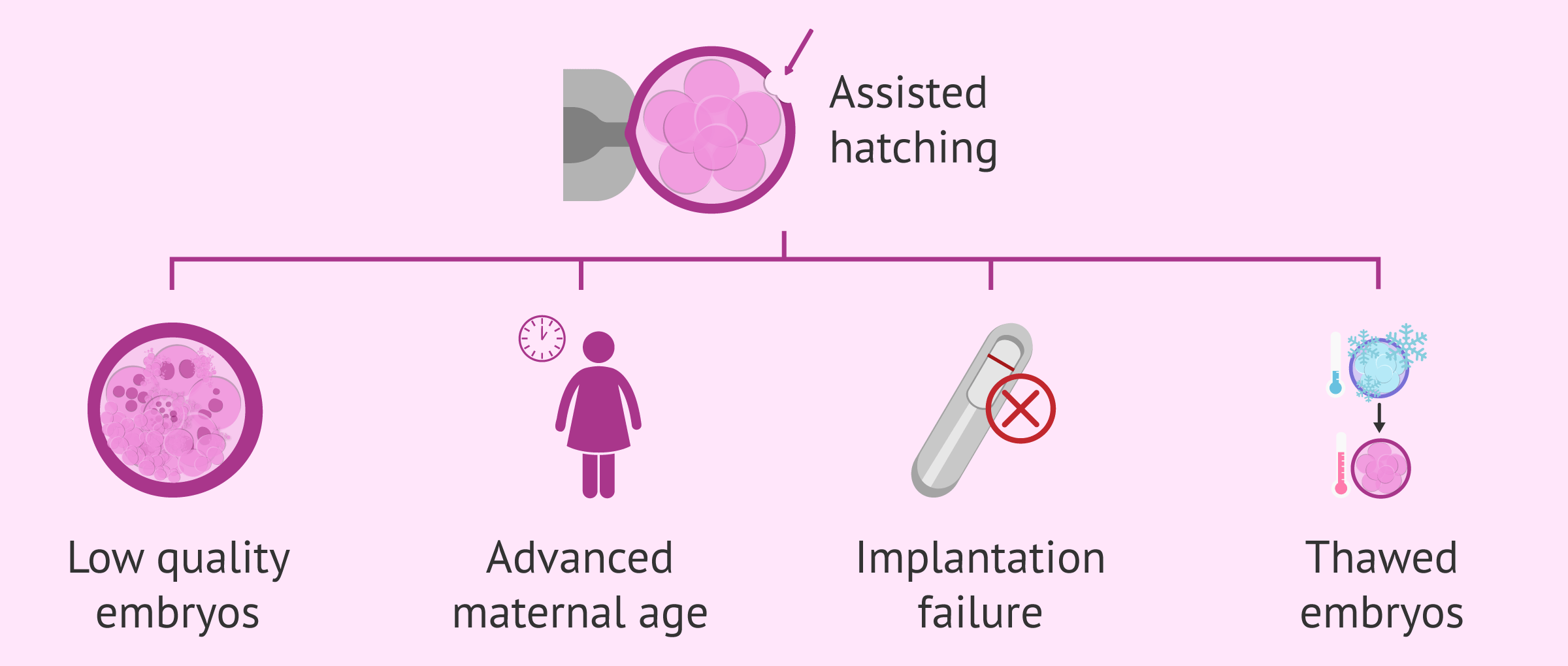
It should only be used in the cases described above, in the rest of the clinical situations it is not advisable because it does not imply any confirmed benefit.
Can endometrial scratching be performed on any woman to increase the chances of pregnancy with IVF?
Normally, endometrial scratching is performed in women who have undergone an unsuccessful embryo transfer and there is a suspicion of a problem at the uterine level. However, the use of this technique is only recommended if established by the medical staff.
Read more
How can egg implantation be improved?
Actually, what implants in the endometrium is not an ovum as such, but a fertilized ovum, which has initiated embryonic development and has given rise to an embryo at the blastocyst stage.
Thus, the way to improve the implantation of the embryo in the endometrium will be to ensure that the conditions of both are optimal (good embryo quality, correct genetic content of the embryo, favorable endometrial microbiome) and that both are synchronized (transfer on day 5, endometrial receptivity test with a receptive result).
Recommended readings
If you are interested in reading more about the embryo implantation process, we recommend you to visit this article: What is embryo implantation and when does it occur?
On the other hand, if you are in the beta wait of your IVF treatment and you want to read some recommendations, you can click on the following link: What is the two-week wait - Symptoms and advice after treatment.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Bashiri A, Halper KI, Orvieto R. Recurrent Implantation Failure-update overview on etiology, diagnosis, treatment and future directions. Reprod Biol Endocrinol. 2018 Dec 5;16(1):121. (See)
Bellver J, Simón C. Implantation failure of endometrial origin: what is new? Curr Opin Obstet Gynecol. 2018 Aug;30(4):229-236. (See)
Coughlan C. What to do when good-quality embryos repeatedly fail to implant. Best Pract Res Clin Obstet Gynaecol. 2018 Nov;53:48-59. (See)
Glujovsky D, Farquhar C, Quinteiro Retamar AM, Alvarez Sedo CR, Blake D. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology. Cochrane Database Syst Rev. 2016 Jun 30;(6):CD002118. (See)
Greco E, Litwicka K, Minasi MG, Cursio E, Greco PF, Barillari P. Preimplantation Genetic Testing: Where We Are Today. Int J Mol Sci. 2020 Jun 19;21(12):4381. (See)
Günther V, Otte SV, Freytag D, Maass N, Alkatout I. Recurrent implantation failure - an overview of current research. Gynecol Endocrinol. 2021 Jul;37(7):584-590. (See)
Pirtea P, Scott RT Jr, de Ziegler D, Ayoubi JM. Recurrent implantation failure: how common is it? Curr Opin Obstet Gynecol. 2021 Jun 1;33(3):207-212. (See)
Simcox LE, Ormesher L, Tower C, Greer IA. Thrombophilia and Pregnancy Complications. Int J Mol Sci. 2015 Nov 30;16(12):28418-28. (See)
Teh WT, McBain J, Rogers P. What is the contribution of embryo-endometrial asynchrony to implantation failure? J Assist Reprod Genet. 2016 Nov;33(11):1419-1430. (See)
Zohni KM, Gat I, Librach C. Recurrent implantation failure: a comprehensive review. Minerva Ginecol. 2016 Dec;68(6):653-67. (See)
FAQs from users: 'Can the implantation rate be improved?', 'In which cases is assisted hatching recommended?', 'Can endometrial scratching be performed on any woman to increase the chances of pregnancy with IVF?' and 'How can egg implantation be improved?'.
Authors and contributors



More information about Cristina Algarra Goosman






Hi, I am a person who goes to the gym almost every day, it’s my medicine. I had my transfer this morning and I am a little worried that my normal gym routine may hurt the chances of implantation.
Hi ShayMitch,
After an embryo transfer, you do not have to take complete rest but you should avoid exertion. If you exercise regularly, I recommend that you continue to go to the gym and try to adapt and modify the most intense exercises to increase the chances of implantation.
Best of luck!