Male fertility is defined as the ability of men to impregnante a women and subsequently have a baby. As such, for a man to be able to conceive, his reproductive system needs to work properly.
In short, to consider a male as fertile, he needs to meet the following requirements:
- The testes have to produce enough sperm in terms of quantity and quality in order to be able to fertilize the female's egg cell.
- Sperm ejaculation has to occur inside the vagina of the woman. This can only be achieved by having full sexual intercourse.
This system is connected and regulated by the sex hormones of males, which start working during puberty.
Provided below is an index with the 9 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 2.
- 3.
- 4.
- 5.
- 5.1.
- 5.2.
- 5.3.
- 5.4.
- 5.5.
- 5.6.
- 5.7.
- 6.
- 7.
- 8.
- 9.
Structure of the male reproductive system
The male reproductive system consists of a set of internal and external organs depending on their location. To follow is a detailed description classification of both:
External organs
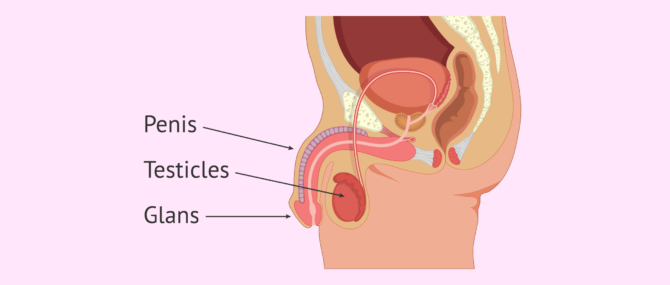
The most important external genitalia of men are the penis and the testes or testicles. These are considered to be external sexual organs because they can be found outside the abdominal cavity.
- Testes or testicles
- These egg-shaped organs are located inside a sack of skin called the scrotum. Their main function is the production of sperm (spermatogenesis) inside the seminiferous tubules, as well as the production of testosterone.
- Penis
- This is the primary male sex organ used during copulation. Its main function is to place the semen inside the vagina of the female during intercourse. The penis is made of the corpus cavernosum, which fills with blood in an erection, and the corpus spongiosum, which forms the glans at the end of the penis.
The testes are located externally because they have to be kept at a lower temperature than that of the body for sperm production. Alterations in the anatomy of the male reproductive system can lead to male infertility, as in the case of cryptorchidism.
Internal organs
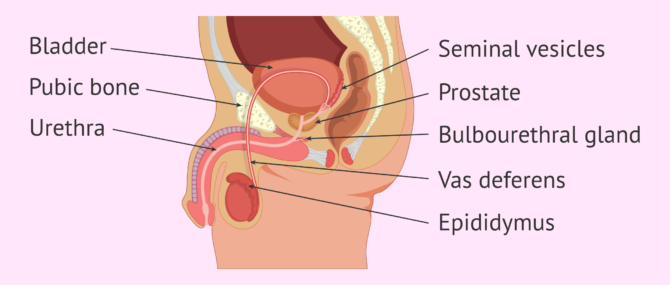
The genitalia of the internal male reproductive organs can be found mainly within the pelvis. Their function is the release and transport of the components used to produce the spermatozoa and semen.
- Epididymis
- Refers to the whole set of seminiferous tubules, and is found behind each testis. It stores the spermatozoa and provides the correct atmosphere for their development.
- Vas deferends or ductus deferens
- A tube that transports sperm from the epididymis to the ejaculatory ducts.
- Seminal vesicles
- These glands are responsible for producing almost all the substances contained in the ejaculate. Moreover, they nourish and provide energy to the sperm that travel in it.
- Prostate
- A glandular organ that also secretes seminal fluid to protect the sperm. Beneath it there are the bulbourethral glands, or Cowper's glands, which secrete a lubricating fluid.
- Urethra
- Males use this conduct for both ejaculation and urination. It opens at the end of the penis.
Contrary to what happens in females, the urethra of males is part of both the excretory and the reproductive systems, as it is used for ejaculating and urinating interchangeably.
If you need to undergo IVF to become a mother, we recommend that you generate your Fertility Report now. In 3 simple steps, it will show you a list of clinics that fit your preferences and meet our strict quality criteria. Moreover, you will receive a report via email with useful tips to visit a fertility clinic for the first time.
When do males start producing sperm?
Since birth, boys have a different reproductive system from that of girls. Their reproductive organs, however, are not functional until they reach puberty.
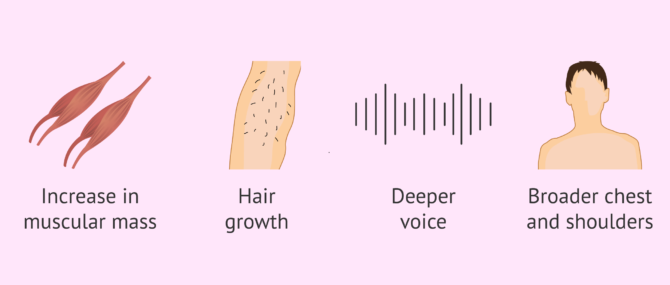
When males turn 11-12 years of age, their endocrine system starts releasing male sex hormones (androgens). They begin their journey towards sexual maturity. At this point, known as puberty, is when they start producing sperm in the testes and developing the common male sexual characteristics:
- Increase in height and muscle mass
- Hair becomes larger and thicker
- Appearance of facial hair
- Deepening of the voice
- Increase in body fat
- Shoulders and chest become broader
- First conscious ejaculations occur
From this moment the male is fertile: he is now a teenager and has the capacity to procreate and have children.
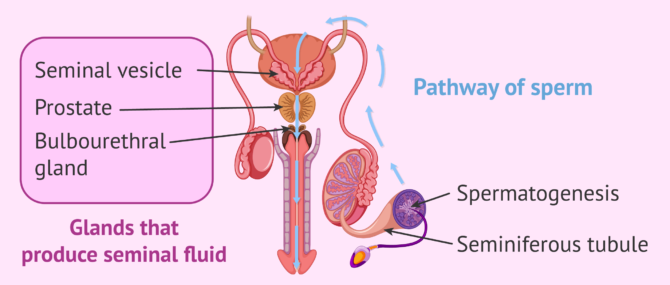
The pathway of sperm
An essential aspect of male fertility is spermatogenesis, a process that takes place within the seminiferous tubules found inside the testes.
Sperm production is a complicated process. It is estimated to take between 64 and 72 days. The male germ cells (spermatogonia) divide sucessively until they have a head and a short tail.
Once made, these sperm are stored in the epididymis, where they mature and acquire the appropriate motility. They then travel to the vas deferens, where they mix with the seminal fluid released by the accessory glands (seminal vesicles, prostate, and bulbourethral glands). Finally, the sperm produced reach the urethra and leave the man's body in ejaculation.
After intercourse and ejaculation, semen enters the vagina, and start their journey of the female reproductive tract thanks to their ability to swim and move forward. Only those able to meet the egg in the Fallopian tube have the chance to fertilize it and create an embryo.
Advice for improving male fertlity
The advice improving fertility in women are quite well known, but the same is not true for men. However, there are some recommendations that can help increase fertility in men.
Having a healthy lifestyle and following a balanced Mediterranean diet minimizes the risk of reproductive alterations in men. In addition, moderate physical exercise also has benefits on semen quality and, therefore, on male fertility.
Stressful situations are undesirable, as they can damage the spermatozoa. Furthermore, it is not advisable to maintain long periods of sexual abstinence. If too much time passes between ejaculations, sperm quality may also be reduced.
FAQs from users
What are spermatic or ejaculatory ducts?
The sperm ducts are made up of the epididymis, the vas deferens, the ejaculatory ducts and the man's urethra. They constitute a set of ducts whose function is to liberate the spermatozoa to the outside by means of ejaculation.
How long does it take from sperm production to ejaculation?
Spermatogenesis is the process whereby male reproductive cells are formed, from the immature ones, spermatogonia, until the mature ones, spermatozoa. This complicated process occurs within the seminiferous tubule in the testis and takes about 64-72 days.
Once spermatozoa (sperm cells) have been produced, they leave the testis and travel to the epididymis, where they will acquire the necessary motility in a process that lasts 10 days approximately. Spermatozoa will be stored in the epididymis until they are expelled with ejaculation. When ejaculation starts, sperm travel through the vas deferends and mixes with the seminal fluid that originates in the secretory glands, creating what we all know as semen. Finally, it is expelled through the urethra.
What diseases are related to the male reproductive system?
All those that affect sperm production or the ability to expel sperm during ejaculation. In this sense, we find disorders at 3 different levels:
- Pretesticular: hormonal alterations due to medication intake, lifestyle habits, diabetes, etc.
- Testicular: varicocele, hydrocele, cryptorchidism, orchitis, etc.
- Post-testicular: obstruction of the seminal ducts due to inflammation, retrograde ejaculation, etc..
It is also possible that there is a genetic disease that causes infertility, such as Klinefelter's syndrome, microdeletions of the Y chromosome, etc.
How can chemotherapy affect fertility in males?
Since chemotherapy works by killing cells that are dividing quickly, and sperm cells are included within this group, chemotherapy affects them greatly. Permanent infertility can occur if all the spermatogonial sperm cells are damaged to the point that they can no longer produce sperm. This risk is dependent on the patient's age, the type of drug used, and the dose given.
How can we evaluate a man's fertility?
To know if a man has the capacity to be able to impregnate a woman naturally, it is first necessary to do a spermogram to check the seminal parameters. Then, depending on the results, a hormonal analysis and a physical examination by the urologist can be done to obtain more information.
How is fertility in men after 45 years of age?
Male fertility decreases with ages, above all after 40 years old. However, this decrease is not as pronounced as it is in women. It is characterized by a progressive reduction in seminal volume, sperm concentration etc. It is also possible to see genetic alterations in the DNA of the sperm. In spite of this, there are men who continue to be fertile and have had children after the age of 50 or 60.
You can read more about this in the following article: The andropause - male menopause.
What is male fertility?
Male fertility is the male's ability to achieve pregnancy and have a baby. Therefore, his reproductive system must function properly and produce sperm. In addition, it is important that the quality of his semen is good in order to fulfill his dream of becoming a father.
If the male has any alteration in his reproductive system and his sperm quality is low, it will be more difficult to get a woman pregnant.
Recommended reading
If you want to know more in detail how the sperm production process is, you can continue reading in the following article: Spermatogenesis.
Male hormones are very important for the proper functioning of the reproductive system. If you are interested in knowing more about the role of each sex hormone, click the following link:Male hormones and fertility.
If you need more information about the possible causes that prevent the correct functioning of the reproductive system in men, you can continue reading in the following post: Possible causes of male sterility.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Craig Niederberger. Introduction: Male Fertility Testing: The Past, Present, and Future. J Urol. 2019 Nov;202(5):852-853. doi: 10.1097/JU.0000000000000468.
Cristina de Angelis, Mariano Galdiero, Claudia Pivonello, Francesco Garifalos, Davide Menafra, Federica Cariati, Ciro Salzano, Giacomo Galdiero, Mariangela Piscopo, Alfonso Vece, Annamaria Colao, Rosario Pivonello. The role of vitamin D in male fertility: A focus on the testis. Rev Endocr Metab Disord. 2017 Sep;18(3):285-305. doi: 10.1007/s11154-017-9425-0.
Md Saidur Rahman, Woo-Sung Kwon, Myung-Geol Pang. Prediction of male fertility using capacitation-associated proteins in spermatozoa. Mol Reprod Dev. 2017 Sep;84(9):749-759. doi: 10.1002/mrd.22810. Epub 2017 Jun 8. (view)
Montserrat Gomendio, Aurelio F Malo, Julian Garde, Eduardo R S Roldan. Sperm traits and male fertility in natural populations. Reproduction. 2007 Jul;134(1):19-29. doi: 10.1530/REP-07-0143 (view)
Trevor G Cooper. The epididymis, cytoplasmic droplets and male fertility. Asian J Androl. 2011 Jan;13(1):130-8. doi: 10.1038/aja.2010.97. Epub 2010 Nov 15 (view)
FAQs from users: 'What are spermatic or ejaculatory ducts?', 'How long does it take from sperm production to ejaculation?', 'What diseases are related to the male reproductive system?', 'What affects fertility in males?', 'What increases fertility in males?', 'How can chemotherapy affect fertility in males?', 'How can we evaluate a man's fertility?', 'What is the male reproductive organ that makes testosterone?', 'How is fertility in men after 45 years of age?', 'Does diabetes affect fertility in males?' and 'What is male fertility?'.
Authors and contributors

More information about Michelle Lorraine Embleton




Hello Sandra,
I want to know if there is any way that could help us check if husband is infertile at home. We’ve been told recently that he’s got a blockage in his reproductive tract, and it’s why we’ve been unable to conceive despite having been ttc for 3 yrs and a half.
Any advice pls?
Dear majorHUM,
Obstructive azoospermia is the least severe type of azoospermia, as sperm production still takes place. The problem is that, in spite of being produced, they cannot come out of the man’s body due to the blockage present in the ejaculatory ducts, which can be caused by infections, inflammations, retrograde ejaculation, etc. The most appropriate treatment in this case involves surgery for the removal of the blockage. Also, a testicular biopsy could help you retrieve sperm from the testes and fertilize them with your egg cells in the laboratory by means of in vitro fertilization (IVF).
See also: What is obstructive azoospermia?
I hope this helps,
Best wishes