When talking about fertility studies related to men, the analysis of semen quality is a fundamental test for the diagnosis of semen.
To assess sperm quality, a seminogram is performed, which is an analytical test in which various parameters of the sperm are studied, such as their mobility, morphology, and concentration.
These sperm quality parameters must reach the minimum values established by the WHO (World Health Organization). A sample with values below the reference standards can affect the search for pregnancy since it is necessary for the sperm to have a certain quality to fertilize the egg and allow gestation.
However, contrary to what you may think, sperm values can be improved. And although in some cases men's reproductive problems have a physiological cause, in many other cases external factors affecting the sperm and ejaculate are involved. Therefore, it is essential to study male fertility by means of seminogram, and to detect those factors that are intervening in it. In this way, it will be possible to introduce the necessary changes in the male's lifestyle that will help to improve sperm quality.
Provided below is an index with the 10 points we are going to expand on in this article.
- 1.
- 2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 3.5.
- 3.6.
- 3.7.
- 3.8.
- 4.
- 5.
- 6.
- 6.1.
- 6.2.
- 6.3.
- 6.4.
- 6.5.
- 6.6.
- 6.7.
- 7.
- 8.
- 9.
- 10.
How does healthy sperm look like?
The semen study allows us, among other things, to evaluate the main characteristics of the spermatozoa.
Although many values have been studied, the three most representative parameters to define semen quality are concentration, motility, and morphology. These three parameters give us an idea of what a healthy spermatozoon capable of producing a pregnancy should be like. The seminogram analyzes the number of sperm in the ejaculate that meets these standards:
- Concentration
- refers to the amount of sperm that should be in the ejaculate. Below 15 million/mL, you may have trouble getting pregnant. As the number of sperm in the ejaculate increases, the chances of reaching the egg and fertilizing it are higher.
- Motility
- about 40% of the sperm must have good motility. They must swim through the female reproductive tract in order to fertilize the egg.
- Morphology
- the shape of spermatozoa in the male ejaculate is very diverse. However, a minimum of spermatozoa are required to have oval heads with robust necks and mobile tails.
Next, Dr. Sergio Rogel shows us which are the aspects that are studied in a basic semen analysis, and also tells us about what has been called an advanced semen analysis:
Nowadays there are other aspects that can be analyzed in a semen sample, which have come to be called advanced semen analysis, such as the study of apoptosis, DNA fragmentation, and sperm DNA protamination.
If you want to know about other parameters studied in the semen analysis, you can consult the article What Is a Semen Analysis Report? - Purpose, Preparation & Cost.
Abnormal sperm quality values
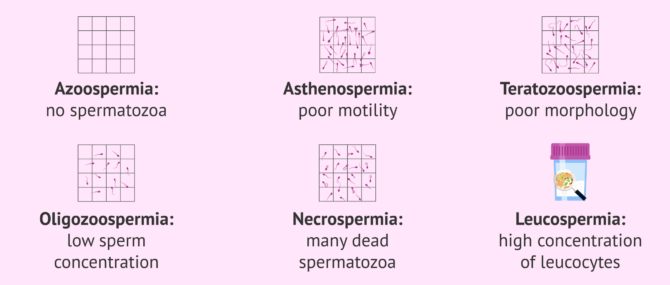
As we have already mentioned, the WHO establishes certain values to establish normozoospermia or normal semen quality. If one or more parameters show a value below the reference value, the sample will be classified as:
- Azoospermia: when the sample has zero sperm in it
- Oligozoospermia: when the sample has less than 15 million sperm/ml
- Asthenozoospermia: when less than 32% of sperm have progressive motility
- Teratozoospermia: if more than 96% of sperm have an abnormal shape
- Hypospermia: low seminal volume in ejaculation
- Leucospermia: when there is a high amount of white cells or leukocytes in the semen
- Necrospermia: when more than 42% of the sperm in the ejaculate are dead
It may occur that there are alterations in more than one parameter, such as cases of oligoasthenoteratozoospermia. These samples with a combination of sperm alterations mark a poorer sperm quality, which will lead to greater difficulty in achieving pregnancy and therefore greater need to resort to assisted reproductive technologies.
However, sperm quality and sperm parameters are not static. This means that for the same man the study values will be similar in all his semen analysis, but they will not always be identical. There are many factors that may be influencing semen quality and can decrease or increase semen quality.
That is why before diagnosing a man with a fertility problem in his semen analysis, this test should be repeated at least 2 times. In this way, it will be possible to corroborate the patient's diagnosis and propose a treatment.
There are several factors that can influence semen quality. Here are some of the most representative ones.
Factors affecting semen quality
There are many factors that affect the concentration, motility, and morphology of spermatozoa. Some of these are unavoidable, but many others are external factors that affect semen quality and can be changed or improved. Here are some of the most representative ones.
Age
Unlike women, men can continue to procreate throughout their lives. But contrary to popular belief, this ability does not remain unchanged over time. Numerous studies indicate that sperm quality can decrease, especially in concentration, motility, and morphology in terms of parameters. This causes a decrease in fertility.
The decrease in the ability to procreate is due to the fact that aging in men is accompanied by a decrease in testosterone levels. This hormone is responsible for regulating sperm production.
Hormonal disorders
Those people who have some kind of alteration in the pathway that controls sex hormones can see their fertility affected by abnormal levels of testosterone.
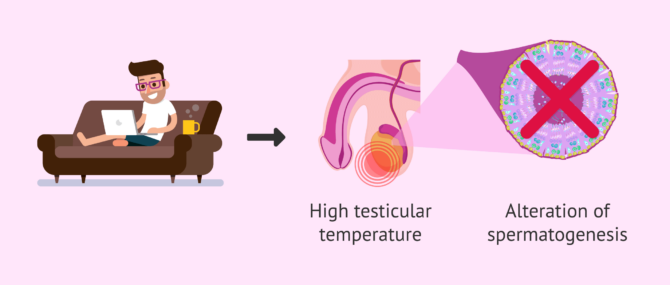
High temperatures
Sperm formation takes place in the testicle at 2 degrees below the temperature of the rest of the body. Any exposure to heat can lead to a decrease in spermatogenesis performance.
Having a testicle inside the abdomen instead of in the scrotal sac, varicocele (varicose veins in the testicle) that increase the blood supply to the testicle, or wearing tight pants and underwear may have an effect on the increased temperature of the testicle.
Fevers can produce this effect on the testicle, and worsen the individual's sperm quality for a short period of time. In addition, the use of electrical devices that give off heat and are often placed on the lap (laptops, for example) can have a harmful effect by altering the temperature of the scrotum.
In the article What Are The Causes of Testicular Hyperthermia? we talk about the consequences of exposure of the testicles to high temperatures.
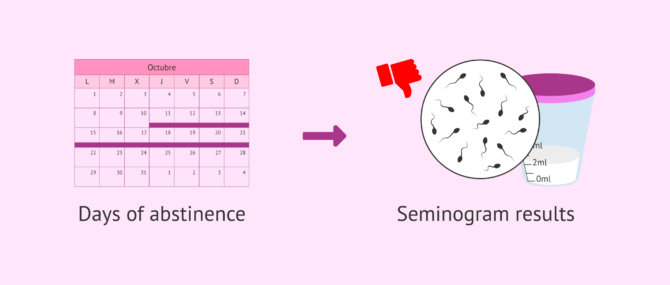
Sexual Abstinence
A very active sexual life can result in a low sperm concentration in the semen analysis. However, this is not indicative of any problem, simply that ejaculations are so frequent that sperm production is not sufficient to meet the demand.
However, prolonged sexual abstinence can have an impact on semen quality. The sperm is not ejaculated and harmful substances accumulate and increase the oxidative stress of the semen. In addition, if this time without producing ejaculates is prolonged, it can have repercussions on the production of spermatozoa, as the testicles slow down their production as they are not used as often as they should be.
You can continue reading about the importance of the abstinence period in the article How does sexual abstinence affect sperm quality?
Alcohol and drugs
Alcohol and drugs can influence hormone levels and, as a consequence, seminal parameters.
In addition, it has been observed that men who drank alcohol in excess had worse sperm parameters and these decreased as the amount of alcohol consumed increased.
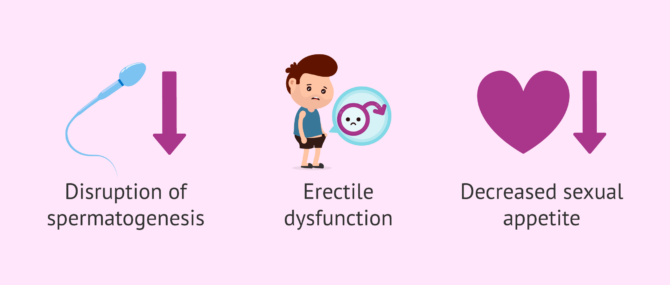
Stress
Although the mechanisms by which stress affects fertility have not yet been discovered, many studies suggest that anxiety can cause lower sperm concentration, motility, and morphology.
The key seems to lie in the high blood glucocorticoid levels detected in chronically stressed men. This substance can affect male sex hormones and, therefore, the creation of sperm.
Stress can also create problems such as erectile dysfunction and sexual dysfunction, which leads men to reduce the frequency of sexual acts and the chances of pregnancy.
If you want to go deeper into the subject you can continue reading in Is Stress Linked To Male Infertility?
Chemicals and toxics
Many studies have shown that toxic substances such as pesticides, lead or mercury can have an impact on sperm quality.
One example is bisphenol A, a substance found in some plastics that has been shown to influence fertility.
Medication
Certain medications can affect sperm production. Many of them have reversible effects when stopped. However, many other drugs can have irreversible effects. For this reason, it is necessary that the medication is prescribed by a doctor and that you consult with them beforehand if try to get pregnant.
Anabolic steroids are a good example of this, as many athletes use them without a prescription. This substance alters hormone levels in men to produce an increase in muscle mass but has an impact on semen quality.
What to do to improve sperm quality?
As we have seen, the quality of semen can vary from one semen analysis to another due to the influence of numerous factors.
After obtaining a bad seminogram result, it is therefore often recommended to repeat the sperm test after 3 to 6 months. During this time, the patient will be given indications on healthy habits and general recommendations related to aspects that may be related to sperm.
If you want to improve sperm quality, these are some of the recommendations you should follow:
- Healthy diet
- a diet rich in vegetables and fruit can help maintain healthy sperm parameters. The vitamins and antioxidants in these foods can help keep oxidative stress that damages sperm cells at bay.
- Exercise
- physical activity keeps oxidative stress at low levels. In addition, it prevents obesity and therefore protects against diseases of the endocrine system. Paradoxically, intense physical exercise can produce the opposite effect: a decrease in semen quality and an altered hormonal profile.
- Supplements
- there are pills to improve sperm quality. These are food complexes based on vitamins and antioxidants that can help to eliminate those residues that produce oxidative stress and that can damage the quality of the semen.
In any case, in this link you can read more general recommendations to improve semen quality: Is it possible to improve sperm quality? - Recommendations.
Decline in semen quality over the last decades
It has long been hypothesized that sperm quality in men has been declining in recent decades. Many put tobacco, stress, and environmental toxins in the limelight as the cause of this damage.
For years, several studies have tried to prove what many voices were clamoring for: that the decline in male fertility was a fact.
Most of the data studied were extracted from fertility centers. Among them, studies showed that during several periods analyzed between 2002 and 2017, sperm motility had been decreasing in men with normal semen. However, these papers were not representative of the population, as the group of men in the study was subjects with fertility problems who came for assisted reproductive treatment, therefore, these men were not representative of the male population.
Another study carried out in the United States analyzed semen donor semen parameters for 10 years. The results indicated a decrease in semen analysis values and raised the following issue: If the sperm parameters of sperm donors are exceptionally high and their decline is undeniable, the same trend (or greater impact) will be repeated in the rest of the population.
However, it wasn't until 2017 that a study proved the worst omens. It was confirmed that the quality of men's semen has been declining. It was shown that from the 1970s to the present day the concentration and number of motile sperm in men is worse. These results were tested in a study that collected data from several decades and from men from all continents and social classes.
FAQs from users
How does vitamin supplements improve semen quality?
Several studies have suggested that semen quality and fertility in men have declined during the last decades. Deterioration in semen samples has been related to environmental pollution, occupational habits, lifestyle changes, exposure to toxins (tobacco, etc.), and dietary habits.
Oxidative stress is considered the main cause of sperm DNA damage. Reduced individual and total antioxidant capacity and high concentrations of seminal ROS (reactive oxygen species) have been detected in men with elevated DNA damage in numerous studies. As for dietary factors, a lower intake of some antioxidant nutrients, such as vitamins A, C and E, carnitine, folate, zinc or selenium, has been associated with male infertility.
Antioxidant therapy of vitamin administration has been tested in numerous trials. The general view is that antioxidant treatment may play a relevant role, although some results have been inconsistent. Among the most recommended preparations are vitamin E and C, zinc, selenium, coenzyme Q10 or L-carnitine.
Can cellphones affect sperm quality?
Yes, electromagnetic radiation of cellphones can in fact affect several parts of the body, including the testes. In this case, the effects are more noticeable amongst males who are used to put their phone in their pocket.
Other factors to keep in mind are:
- Model or type of device
- Usage of Internet, if any
- Internet connection speed (3G or 4G)
- For how long the phone is kept in the pocket of the trousers
- Other places where the phone is kept
According to various studies, radiation of mobile phones affects the viability and motility of sperm. Sperm concentration is affected as well, though to a lesser extent.
I have heard Scottish kilts improve male fertility, is it true?
Yes, recent studies have shown that the use of the kilt, the traditional tartan-patterned Scottish dress that boys and men from this land wear with proud, seems to improve the quality of their semen.
The traditional, healthier and even manlier way of wearing this dress is without underpants, and it is that very looseness what increases sperm production, leading to a subsequent increase un sperm concentration.
The scrotum, being some degrees below the temperature of the rest of the body, optimizes spermatogenesis, that is why Scottish men that choose that attire see their semen quality improved.
This study was carried out by a group of Scottish researchers and their results were published in the Scottish Medical Journal. According the their research, men who has been using the kilt for years have better sperm concentration levels. Moreover, a boost in the fertility of these men was confirmed.
Can the use of a laptop cause male infertility?
The use of the laptop on the male's legs can affect the formation of sperm due to the heat produced by the computer's battery, which increases the temperature of the testicles.
An increase in scrotal temperature of more than 1ºC from the initial value may inhibit spermatogenesis. This happens when the laptop is used for long periods of time and very often. It is therefore best to use a table or other support for the laptop and not to place it directly on the body.
Can eating habits affect a man's sperm count?
Absolutely yes. Diet and eating habits are key factors when it comes to determining sperm quality in males.
A number of studies have demonstrated that what you eat on a daily basis, especially if it contains high amounts of carbohydrates and saturated fats, can diminish the sperm count, causing oligozoospermia.
Can drinking too much coffee cause oligospermia?
Consuming excessive amounts of caffeine might indeed be linked to a reduction in sperm concentration. However, it might just be one additional element within a combination of poor habits, such as neglecting nutrition or overusing tobacco, alcohol, or other substances.
Read more
Does bike riding lead to low sperm count?
Some studies affirm that men who spend a lot of time on the bicycle may see their semen quality affected due both to tight clothing that increases the temperature of the testicles, and to the knocking of the genitals with the saddle.
The great effort that occurs in this type of endurance sports also contributes to the formation of reactive oxygen substances that affect male fertility.
Finally, high pressure on the nerves and blood vessels in the scrotal area can also contribute to impotence and erectile dysfunction in cyclists, so it is recommended to use alternative saddles that exercise less pressure on the groin and increase blood flow to the penis.
Suggested for you
As we have seen, the parameters studied in spermograms are susceptible to being altered by bad lifestyle habits or by being in contact with components that are harmful to reproductive health. Our fertility experts have written an extensive article explaining how to improve sperm quality. If you are interested and want to know what actions you can take to improve your sperm, we recommend you: Is it possible to improve sperm quality? - Recommendations.
If you want to know what the seminogram consists of and which parameters are most important to be able to interpret it, you can visit our article What is a basic semen analysis and how is it done step by step?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Kvist U, Björndahl L. ESHRE Monographs: Manual on Basic Semen Analysis. Oxford: Oxford University Press, 2002 (View)
Andrade-Rocha FT (2003).Semen analysis in laboratory practice: an overview of routine test. J Clin Lab Anal 2003; 17: 247-258 (View)
Sigman M, Zini A. (2009). Semen analysis and sperm function assays: what do they mean? Semin Reprod Med; 27: 115-123 (View)
Álvarez C, Castilla JA, Ramírez JP, Vergara F, Yoldi A, Fernández A, Gaforio JJ. External quality control program for semen analysis: Spanish experience. J Assist Reprod Genet 2005;22:379-87 (View)
Cooper TG, Björndahl L, Vreeburg J, Nieschlag, E. Semen analysis and external quality control schemes for semen analysis need global standardization. Int J Androl 2002;25:306-311 (View)
Male infertility best practice policy committee of the American Urological Association (AUA) (2010). The optimal evaluation of the infertile male. AUA Best Practice Statement.
Sociedad Española de Fertilidad (SEF) (2011). Manual de Andrología. Coordinador: Mario Brassesco. EdikaMed, S.L. ISBN: 978-84-7877.
Sakkas D, Álvarez JG. Sperm DNA fragmentation: mechanisms of origin, impact on reproductive outcome, and analysis. Fertil Steril. 2010;93:1027-36 (View)
World Health Organization (WHO) (2000). WHO Manual for the Standardized Investigation, Diagnosis and management of the infertile male. Cambridge: Cambridge University Press.
Guzick DS, Overstreet JW, Factor-Litvak P, Brazil CK, Nakajima ST, Coutifaris C, et al. (2001). Sperm morphology, motility, and concentration in fertile and infertile men. N Engl J Med 2001; 345: 1388-1393 (View)
FAQs from users: 'How does vitamin supplements improve semen quality?', 'Can cellphones affect sperm quality?', 'I have heard Scottish kilts improve male fertility, is it true?', 'Can the use of a laptop cause male infertility?', 'Can eating habits affect a man's sperm count?', 'Can drinking too much coffee cause oligospermia?' and 'Does bike riding lead to low sperm count?'.
Authors and contributors
More information about Cristina Algarra Goosman