In recent years, we can observe a decline in semen quality, due to certain factors related to the current lifestyle.
In this way, knowing the factors that affect sperm quality can allow the male to acquire certain healthy habits that will help him to improve his spermatozoa quality.
However, it should be noted that male infertility may also be due to factors that cannot be modified.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 2.4.
- 2.5.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 4.7.
- 4.8.
- 5.
- 6.
- 7.
- 8.
How is semen quality evaluated?
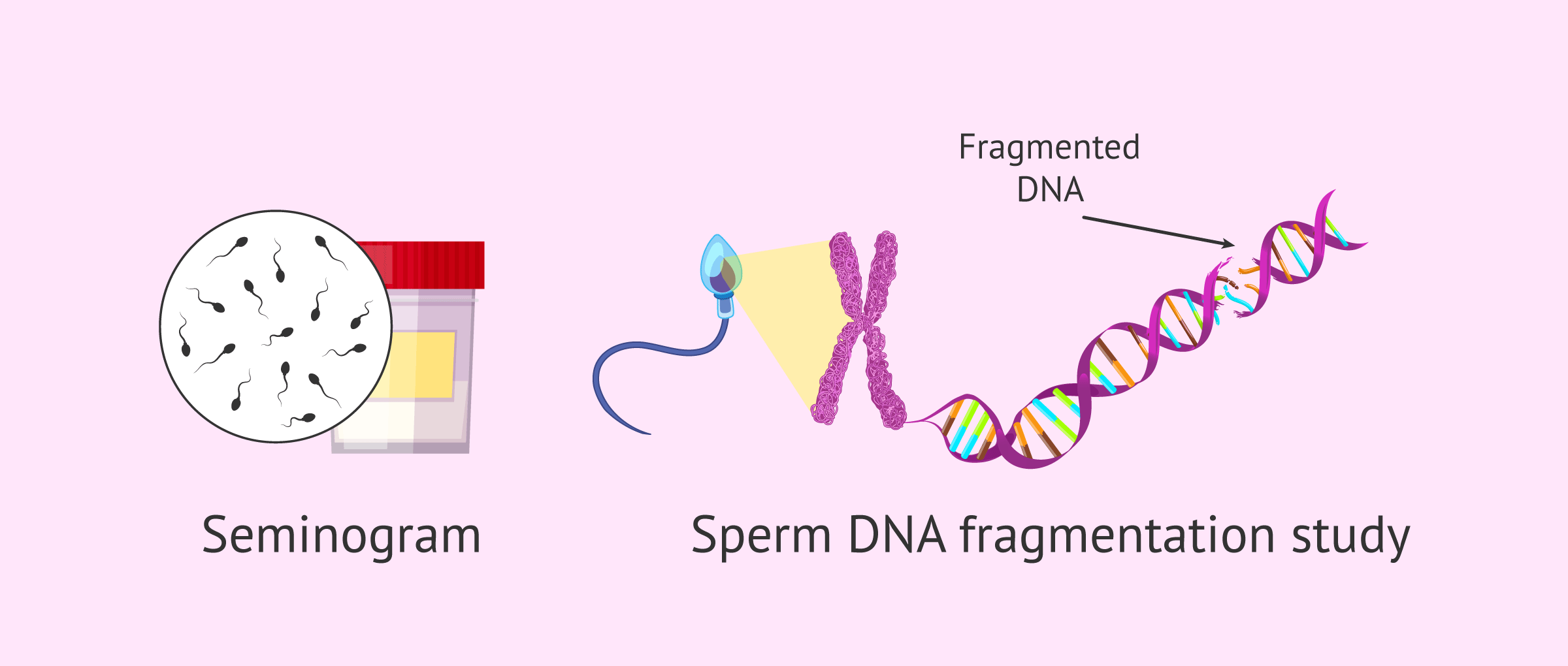
The test usually performed to evaluate semen quality is the seminogram. This test provides results about sperm concentration, motility, and morphology.
However, there are other important aspects in determining the quality of a semen sample, such as the integrity of the sperm DNA. Additional tests such as the sperm DNA fragmentation study should be performed to analyze this parameter.
Alterations in these seminal parameters can hinder or even prevent the fertilization of the egg and, thus, pregnancy. A man with poor semen quality is less likely to get his partner pregnant, although this will also depend on whether there is an associated female fertility problem or not.
Fertility treatments, like any other medical treatment, require that you trust the fertility specialists that will be by your side during your journey. Logically, each clinic has a different work methodology. Our Fertility Report will offer you a selection of recommended clinics, that is, fertility centers that have passed our rigorous selection process. Moreover, our system is capable of comparing the costs and conditions of each one so that you can make a well-informed decision.
Factors that influence semen quality
As mentioned above, there are some factors related to the male's lifestyle and, therefore, modifiable, that could be affecting his seminal quality.
Some of them are detailed below.
Nutrition
A diet rich in fruits, vegetables, legumes, fish, nuts, poultry, and low-fat dairy products may be associated with good sperm quality.
In addition, increasing selenium, zinc, omega-3 fatty acids, coenzyme Q10, and carnitine intake, possible through dietary supplements, could improve semen quality. However, it´s not recommended to administer food supplements without a medical recommendation.
If you wish to read more information about this topic, we recommend you to visit the following link: What are the foods that can improve male fertility?
Tobacco, alcohol and drugs
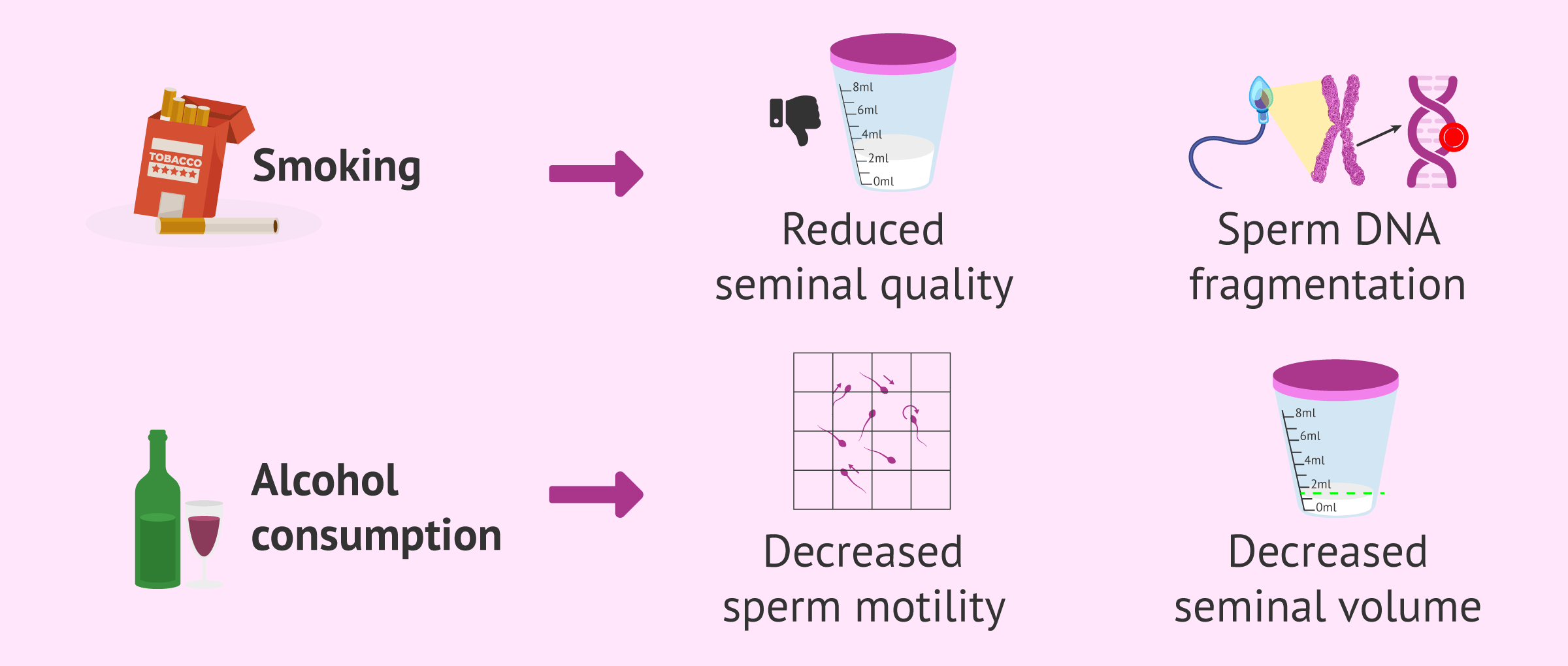
In general, several studies have found that seminal parameters are worse in male smokers, although the effect may depend on the dose of cigarettes. In addition, sperm DNA fragmentation may also be increased in smokers.
As for daily alcohol consumption, it could affect the seminal volume and sperm morphology. This is because of a possible effect on testosterone metabolism and spermatogenesis, such as sperm production. However, occasional moderate consumption may not affect sperm parameters.
Regular consumption of marijuana, one of the most widespread drugs, is also associated with altered semen quality.
Obesity
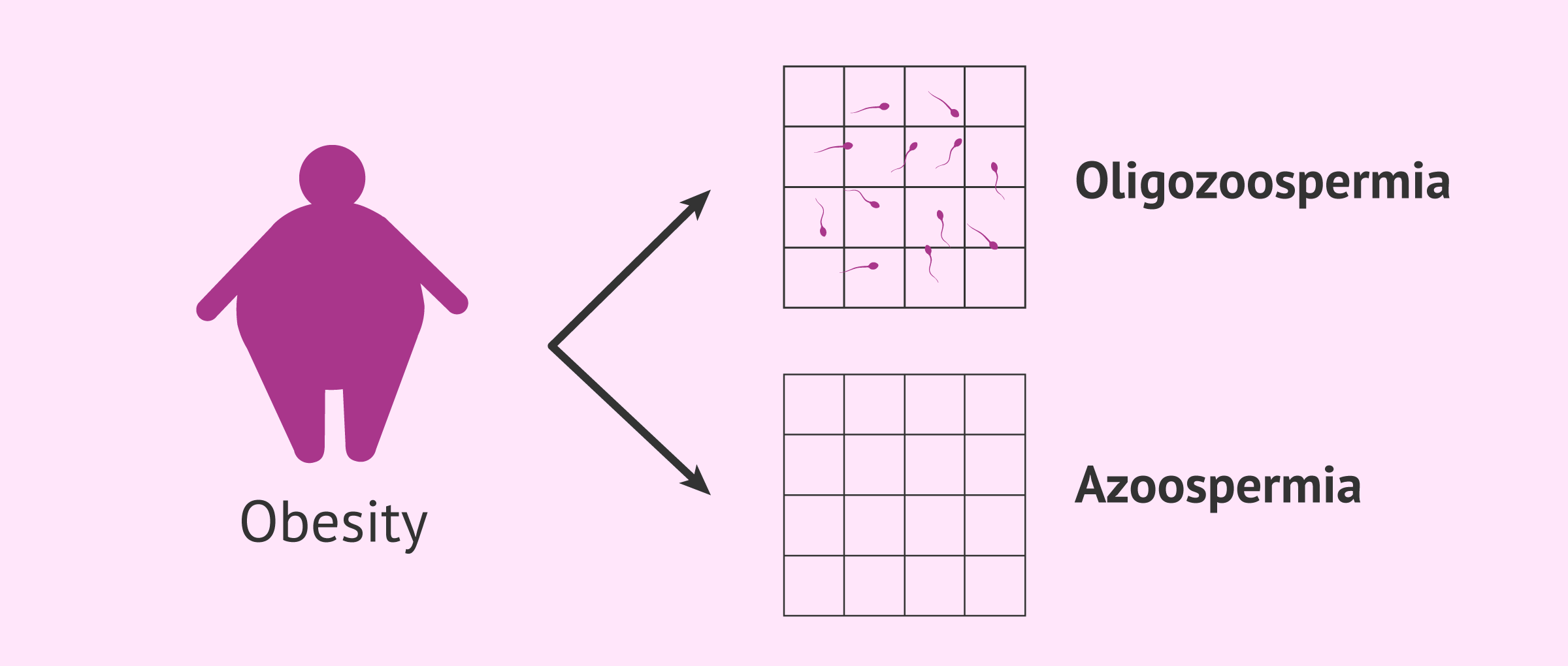
Couples with obese males may be more likely to have infertility problems.
When there is overweight or obesity, the male is more likely to have oligozoospermia or azoospermia. These alterations in the number of spermatozoa can seriously affect male fertility and, therefore, cause infertility problems.
In addition, the relationship of obesity with metabolic syndrome and systemic proinflammatory state could increase oxidative stress. The main consequence of this oxidative stress would be an increase in sperm DNA fragmentation.
Nevertheless, paternal obesity could also affect the results of assisted reproduction techniques results in terms of live birth rate.
Cell phone
Exposure to radiation from cell phones has been associated with lower semen quality, the effect of which may depend on the duration of exposure. In addition, several studies have observed a negative effect of cell phones on sperm motility.
This exposure could cause increased oxidative stress in the testes, which increases sperm DNA damage.
However, the results of the studies are not conclusive. This is why the possible effects of cell phone use on semen quality are not entirely clear.
Scrotal temperature
Testicular temperature is 2-4 degrees lower than body temperature for optimal spermatogenesis.
The use of excessively tight clothing can cause an increase in temperature in the testicular area, which can therefore affect spermatogenesis.
Similarly, resting a laptop computer on the legs can cause an increase in testicular temperature, as can the use of saunas, the position in which one sleeps or spending long periods of time driving.
Recommendations to improve sperm quality
Taking into account the aforementioned factors, there are a series of recommendations that the male can take into account to improve his seminal quality.
- Controled diet and moderate physical activity to maintain an adequate weight.
- Follow a Mediterranean diet, with a high content of fruits, vegetables, legumes...
- Consult a specialist about taking a nutritional supplement.
- Tobacco, alcohol and drugs.
- Do not carry your cell phone in your trouser pockets, especially in the front pockets.
- Avoid tight clothing.
- Do not rest the laptop on the legs and take care of other actions that could raise the testicular temperature.
It is possible that taking care of all these factors, in a sustained manner over time, may help to improve semen quality.
FAQs from users
How can semen quality be improved?
There are different ways to achieve the goal of increasing sperm quality:
- Healthy habits
- regular intake of antioxidants (tomato, nuts), not excessive exercise, ensuring proper regulation of testicular temperature (not tight underwear), avoiding hormonal disruptors (plastics, fuels...) are useful to naturally improve sperm quality.
- Medications
- They are usually medications that provide trace elements, vitamins and antioxidants externally, and their use is a good option before or during assisted reproduction treatments.
- Nonsteroidal anti-inflammatory drugs
- always under medical prescription. These drugs reduce sperm DNA fragmentation.
- Others
- the use of hormones such as gonadotropins or testosterone may be necessary to improve sperm quality. These medications should always be used after a doctor's prescription.

What are the 5 recommended foods to improve semen?
Leading a healthy lifestyle and a balanced diet helps improve semen quality.
Foods high in vitamin C and antioxidants, such as oranges, blueberries and strawberries, help improve sperm motility. Foods rich in vitamin B12 (meats, dairy products and derivatives), rich in Zinc (cashews, oysters, cocoa, etc.) or with a high amount of vitamin E (olive oil, walnuts, almonds...) are also beneficial to improve semen quality.
Can you increase sperm count?
Yes, as long as the male testicles are functional and there is sperm production. There are nutritional supplements that can help improve sperm production, such as vitamin complexes and antioxidants that reduce the damage caused by free radicals to spermatozoa.
Read more
Can acupuncture help with teratozoospermia?
Yes, according to some studies. Broadly speaking, acupuncture increases pregnancy rates in cases of idiopathic or unexplained infertility. Also, there is proof that is can improve sperm quality in cases of oligospermia, asthenospermia, and teratozoospermia.
Can eating more berries improve sperm quality?
Yes. Many berries contain antioxidant pigments and have a high capacity to absorb oxygen free radicals. For this reason, berries are perfect for protecting sperm from oxidative stress.
In addition, blueberries, blackberries, currants, and strawberries are rich in vitamin C and other nutrients. Due to their high vitamin C content, these foods help protect cells from damage
How can I improve amorphous sperm in semen?
In the first place and as long as the cause of teratozoospermia is not a specific pathology, the male should follow some guidelines to modify his lifestyle, which may be interfering negatively in his reproductive state. Some men who give up habits such as tobacco or alcohol and follow a healthy diet see an improvement in their seminal quality after about 3 months.
Can olive oil help with poor sperm quality?
Olive oil is a monounsaturated fat that is rich in oleic acid. If taken in great amounts, it helps destroy and eliminate the presence of "bad" cholesterol (LDL) in blood flow, which can help reduce the risk of having a cardiovascular and/or brain disease.
In relation to reproductive health, regular use of olive oil (especially virgin olive oil) along with the elimination of LDL cholesterol boost the arrival of oxygen to the testes. In other words, spermatogenesis will occur in optimum conditions.
Do walnuts help improve semen quality?
Walnuts are one of the foods that contribute to improve sperm quality in the male. This food could help to improve the quantity of sperm, but also the mobility and shapes of sperm due to its antioxidant capacity.
Recommended readings
In this article, we further explain sperm DNA fragmentation. If you want to learn more about this topic, you can visit the following link: Sperm DNA Fragmentation - Causes & Effect on Fertility.
If, however, you are interested in knowing more about obesity and low sperm quality, we recommend you to read this article: Male infertility and low semen quality due to obesity
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Adams JA, Galloway TS, Mondal D, Esteves SC, Mathews F. Effect of mobile telephones on sperm quality: a systematic review and meta-analysis. Environ Int. 2014 Sep;70:106-12 (View)
Agarwal A, Deepinder F, Sharma RK, Ranga G, Li J. Effect of cell phone usage on semen analysis in men attending infertility clinic: an observational study. Fertil Steril. 2008 Jan;89(1):124-8 (View)
Agarwal A, Durairajanayagam D. Are men talking their reproductive health away? Asian J Androl. 2015 May-Jun;17(3):433-4 (View)
Asare-Anane H, Bannison SB, Ofori EK, Ateko RO, Bawah AT, Amanquah SD, Oppong SY, Gandau BB, Ziem JB. Tobacco smoking is associated with decreased semen quality. Reprod Health. 2016 Aug 5;13(1):90 (View)
Balawender K, Orkisz S. The impact of selected modifiable lifestyle factors on male fertility in the modern world. Cent European J Urol. 2020;73(4):563-568 (View)
Bandel I, Bungum M, Richtoff J, Malm J, Axelsson J, Pedersen HS, Ludwicki JK, Czaja K, Hernik A, Toft G, Bonde JP, Spanò M, Malm G, Haugen TB, Giwercman A. No association between body mass index and sperm DNA integrity. Hum Reprod. 2015 Jul;30(7):1704-13 (View)
Bendayan M, Alter L, Swierkowski-Blanchard N, Caceres-Sanchez L, Selva J, Robin G, Boitrelle F. Toxiques, mode de vie, environnement : quels impacts sur la fertilité masculine ? [Environment and lifestyle: Impacts on male fertility?]. Gynecol Obstet Fertil Senol. 2018 Jan;46(1):47-56. French (View)
Campbell JM, Lane M, Owens JA, Bakos HW. Paternal obesity negatively affects male fertility and assisted reproduction outcomes: a systematic review and meta-analysis. Reprod Biomed Online. 2015 Nov;31(5):593-604 (View)
Esteves SC, Agarwal A, Sharma R, Harlev A. Reply to Eugenio Ventimiglia, Montorsi Francesco, and Andrea Salonia's Letter to the Editor re: Reecha Sharma, Avi Harlev, Ashok Agarwal, Sandro C. Esteves. Cigarette Smoking and Semen Quality: A New Meta-analysis Examining the Effect of the 2010 World Health Organization Laboratory Methods for the Examination of Human Semen. Eur Urol 2016;70:635-45. Eur Urol. 2017 Jan;71(1):e21-e22 (View)
Hatch EE, Willis SK, Wesselink AK, Mikkelsen EM, Eisenberg ML, Sommer GJ, Sorensen HT, Rothman KJ, Wise LA. Male cellular telephone exposure, fecundability, and semen quality: results from two preconception cohort studies. Hum Reprod. 2021 Apr 20;36(5):1395-1404 (View)
Karayiannis D, Kontogianni MD, Mendorou C, Douka L, Mastrominas M, Yiannakouris N. Association between adherence to the Mediterranean diet and semen quality parameters in male partners of couples attempting fertility. Hum Reprod. 2017 Jan;32(1):215-222 (View)
Kozopas NM, Chornenka OI, Vorobets MZ, Lapovets LY, Maksymyuk HV. Body Mass Index and Sperm Quality: Is there a Relationship? J Hum Reprod Sci. 2020 Apr-Jun;13(2):110-113 (View)
Liu K, Li Y, Zhang G, Liu J, Cao J, Ao L, Zhang S. Association between mobile phone use and semen quality: a systemic review and meta-analysis. Andrology. 2014 Jul;2(4):491-501 (View)
López Teijón M, Garcia F, Serra O, Moragas M, Rabanal A, Olivares R, Alvarez JG. Semen quality in a population of volunteers from the province of Barcelona. Reprod Biomed Online. 2007 Oct;15(4):434-44 (View)
MacDonald AA, Herbison GP, Showell M, Farquhar CM. The impact of body mass index on semen parameters and reproductive hormones in human males: a systematic review with meta-analysis. Hum Reprod Update. 2010 May-Jun;16(3):293-311 (View)
Mir J, Franken D, Andrabi SW, Ashraf M, Rao K. Impact of weight loss on sperm DNA integrity in obese men. Andrologia. 2018 Feb 1 (View)
Mostafa RM, Nasrallah YS, Hassan MM, Farrag AF, Majzoub A, Agarwal A. The effect of cigarette smoking on human seminal parameters, sperm chromatin structure and condensation. Andrologia. 2018 Apr;50(3) (View)
Okechukwu CE. Does the Use of Mobile Phone Affect Male Fertility? A Mini-Review. J Hum Reprod Sci. 2020 Jul-Sep;13(3):174-183 (View)
Ricci E, Al Beitawi S, Cipriani S, Candiani M, Chiaffarino F, Viganò P, Noli S, Parazzini F. Semen quality and alcohol intake: a systematic review and meta-analysis. Reprod Biomed Online. 2017 Jan;34(1):38-47 (View)
Salas-Huetos A, James ER, Aston KI, Jenkins TG, Carrell DT. Diet and sperm quality: Nutrients, foods and dietary patterns. Reprod Biol. 2019 Sep;19(3):219-224. (View)
Sansone A, Di Dato C, de Angelis C, Menafra D, Pozza C, Pivonello R, Isidori A, Gianfrilli D. Smoke, alcohol and drug addiction and male fertility. Reprod Biol Endocrinol. 2018 Jan 15;16(1):3 (View)
Sepaniak S, Forges T, Gerard H, Foliguet B, Bene MC, Monnier-Barbarino P. The influence of cigarette smoking on human sperm quality and DNA fragmentation. Toxicology. 2006 Jun 1;223(1-2):54-60 (View)
Sermondade N, Faure C, Fezeu L, Shayeb AG, Bonde JP, Jensen TK, Van Wely M, Cao J, Martini AC, Eskandar M, Chavarro JE, Koloszar S, Twigt JM, Ramlau-Hansen CH, Borges E Jr, Lotti F, Steegers-Theunissen RP, Zorn B, Polotsky AJ, La Vignera S, Eskenazi B, Tremellen K, Magnusdottir EV, Fejes I, Hercberg S, Lévy R, Czernichow S. BMI in relation to sperm count: an updated systematic review and collaborative meta-analysis. Hum Reprod Update. 2013 May-Jun;19(3):221-31 (View)
Sharma R, Harlev A, Agarwal A, Esteves SC. Cigarette Smoking and Semen Quality: A New Meta-analysis Examining the Effect of the 2010 World Health Organization Laboratory Methods for the Examination of Human Semen. Eur Urol. 2016 Oct;70(4):635-645 (View)
Vanderhout SM, Rastegar Panah M, Garcia-Bailo B, Grace-Farfaglia P, Samsel K, Dockray J, Jarvi K, El-Sohemy A. Nutrition, genetic variation and male fertility. Transl Androl Urol. 2021 Mar;10(3):1410-1431 (View)
FAQs from users: 'How can semen quality be improved?', 'What are the 5 recommended foods to improve semen?', 'Can you increase sperm count?', 'Can acupuncture help with teratozoospermia?', 'Can eating more berries improve sperm quality?', 'How can I improve amorphous sperm in semen?', 'Can olive oil help with poor sperm quality?' and 'Do walnuts help improve semen quality?'.
Authors and contributors
More information about Cristina Algarra Goosman








I have been trying to get pregnant for quite some time now and I can’t seem to get pregnant. My husband is a little overweight and does some of the things you post here wrong. could that be the cause?
Hello Karen,
It may be possible that the quality of your husband´s sperm has been compromised by his health habits, this could be the cause of your difficulty to get pregnant. Nevertheless, many factors can influence this journey. I recommend you to go see a specialist so they can evaluate both your egg quality and his sperm quality.
However, I encourage him to make changes in his habits and try to eliminate as many toxic habits as possible, that will undeniably improve his sperm quality.
I hope I could help out.