A recent scientific study has investigated how the bacteria present in the uterus directly affect assisted reproduction treatments.
This extensive research was carried out by the authors F. Giangrazi, J.A. Sugrue, V.M. Sularea, A.A.I. Brugman, M. Horan, M. Wingfield, D.A. Crosby, L.E. Glover, and C. O'Farrelly. To achieve this, multiple prestigious centers and institutions have collaborated, including Trinity College Dublin, the Institut Pasteur in Paris, the National Maternity Hospital in Dublin, the Merrion Fertility Clinic, and University College Dublin.
The results demonstrate that the cellular and bacterial balance of the endometrium is a fundamental factor in achieving pregnancy.
Provided below is an index with the 6 points we are going to expand on in this article.
Microbiome and fertility
Traditionally, it was thought that the inside of the uterus was a sterile environment, but today it is known that it hosts a community of microorganisms. This uterine bacterial flora plays a vital role in reproductive processes:
- Women who fail to get pregnant after fertility treatment often have a more diverse endometrial microbiome than normal.
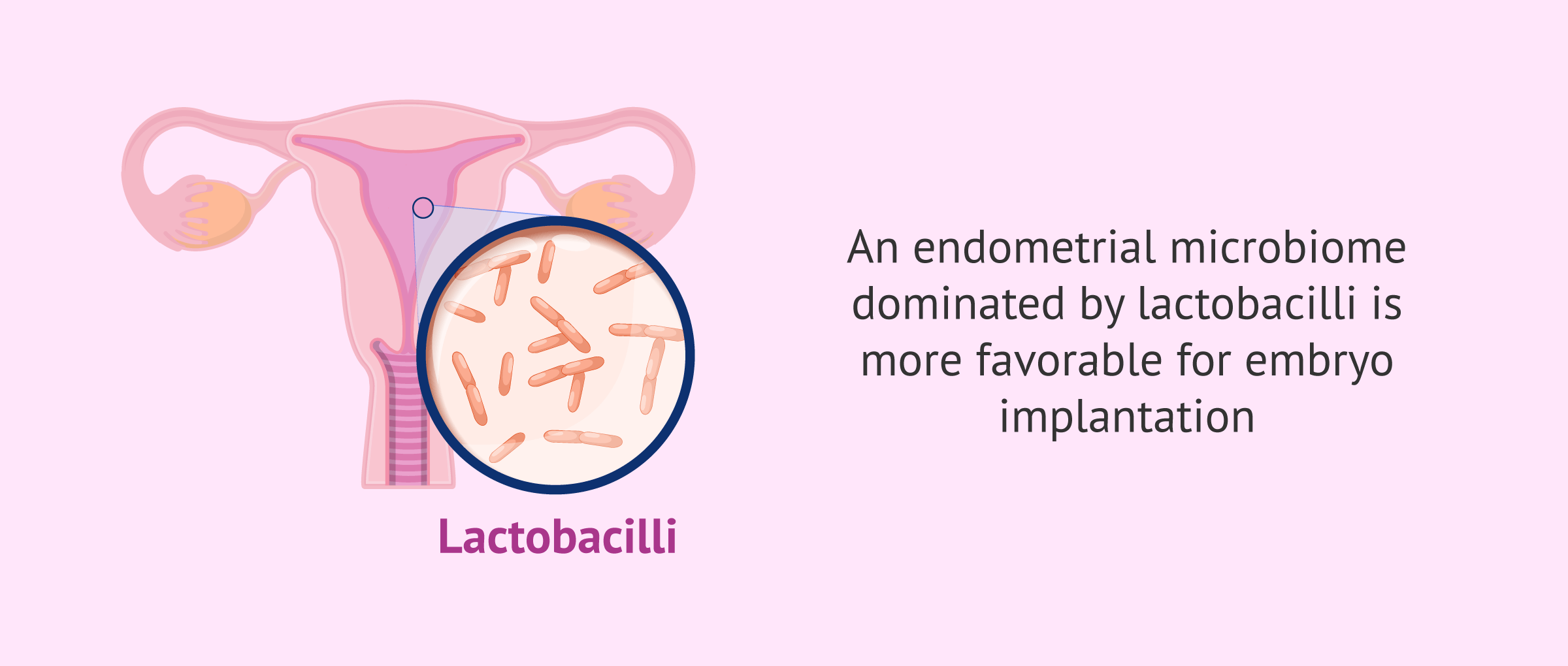
- A healthy endometrium that is conducive to pregnancy is primarily dominated by bacteria of the Lactobacillus genus.
- The decrease in lactobacilli has a negative impact on reproductive success.
When the protective flora decreases, other bacteria can colonize the uterus and alter the ideal conditions that the embryo needs for correct implantation.
Bacteria that hinder pregnancy
Thanks to advanced analysis of bacterial DNA, specialists have managed to identify which microorganisms could be associated with failing to achieve pregnancy and with implantation failures:
- A significantly higher presence of pathogenic bacteria, such as Prevotella and Corynebacterium, has been detected in women who failed to conceive after assisted reproduction treatment.
- Prevotella spp. is among the bacteria that produce butyrate, a specific metabolic substance.
The increase in butyrate in the uterine cavity has direct consequences: it decreases the function of the endometrial epithelial barrier and increases the expression of inflammatory markers, which can make it difficult for the embryo to find a suitable place to implant.
The role of uterine inflammation
The accumulation of harmful bacterial compounds such as butyrate generates a strong "defensive" reaction in the woman's body:
- The endometrial tissue experiences an increase in its local inflammation levels.
- Butyrate alters the expression of genes related to uterine receptivity.
- This would cause false cellular signaling that alters the exact moment when the uterus is ready to receive the embryo.
By understanding how these bacteria alter the uterine barrier and generate inflammation, we are undoubtedly closer to developing new strategies to correct this microbial flora before transferring the embryo, thus increasing the chances of reproductive success.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Giangrazi F, Sugrue JA, Sularea VM, Brugman AAI, Horan M, Wingfield M, Crosby DA, Glover LE, O'Farrelly C. Contribution of endometrial microbiome to inflammation-mediated infertility in women undergoing ART. Hum Reprod. 2026 Feb 3:deaf252. doi: 10.1093/humrep/deaf252. Epub ahead of print. PMID: 41633818. (View)