Programmed or timed intercourse is a simple technique in assisted reproductive technology which is based on the control of ovulation to determine the moment in which to have sexual intercourse when trying for pregnancy.
This method can be carried out taking into account the woman's natural cycle or even ovulation can be induced. Another way to perform timed intercourse is through ovarian stimulation.
Like other fertility treatments, timed intercourse has a number of benefits and drawbacks.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 4.7.
- 5.
- 6.
- 7.
- 8.
What is timed intercourse?
In order for pregnancy to take place, it is necessary for the egg and sperm to fuse and create the embryo which must implant in the mother's uterus to continue its development until birth.
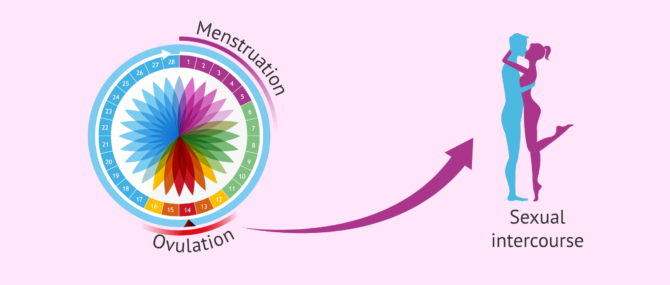
The egg is found inside the ovary and, when it reaches its final stage of maturation, it is expelled into the fallopian tubes. This is what we know as ovulation and occurs approximately in the middle of the cycle.
Outside the ovary, the egg is only able to survive about 24 hours, so the sperm only have this time to reach it and fertilize it.
Timed sexual intercourse consists of synchronizing the moment when the woman releases the egg into the fallopian tubes with the man's ejaculation, that is, with the entrance of the sperm into the female reproductive system. It is therefore a matter of synchronizing ovulation with the couple's sexual relationships.
In this way, we increase the probability for the egg and sperm to meet and for fertilization to occur.
How does timed intercourse work?
In order to be able to indicate to the couple the ideal moment to have sexual intercourse that increases the pregnancy success rates, the woman's menstrual cycle is monitored by means of blood tests and ultrasound scans.
This is the basis when it comes to scheduling intercourse. After about two weeks, a pregnancy test is performed in order to determine if the technique was successful, that means, whether or not pregnancy has taken place.
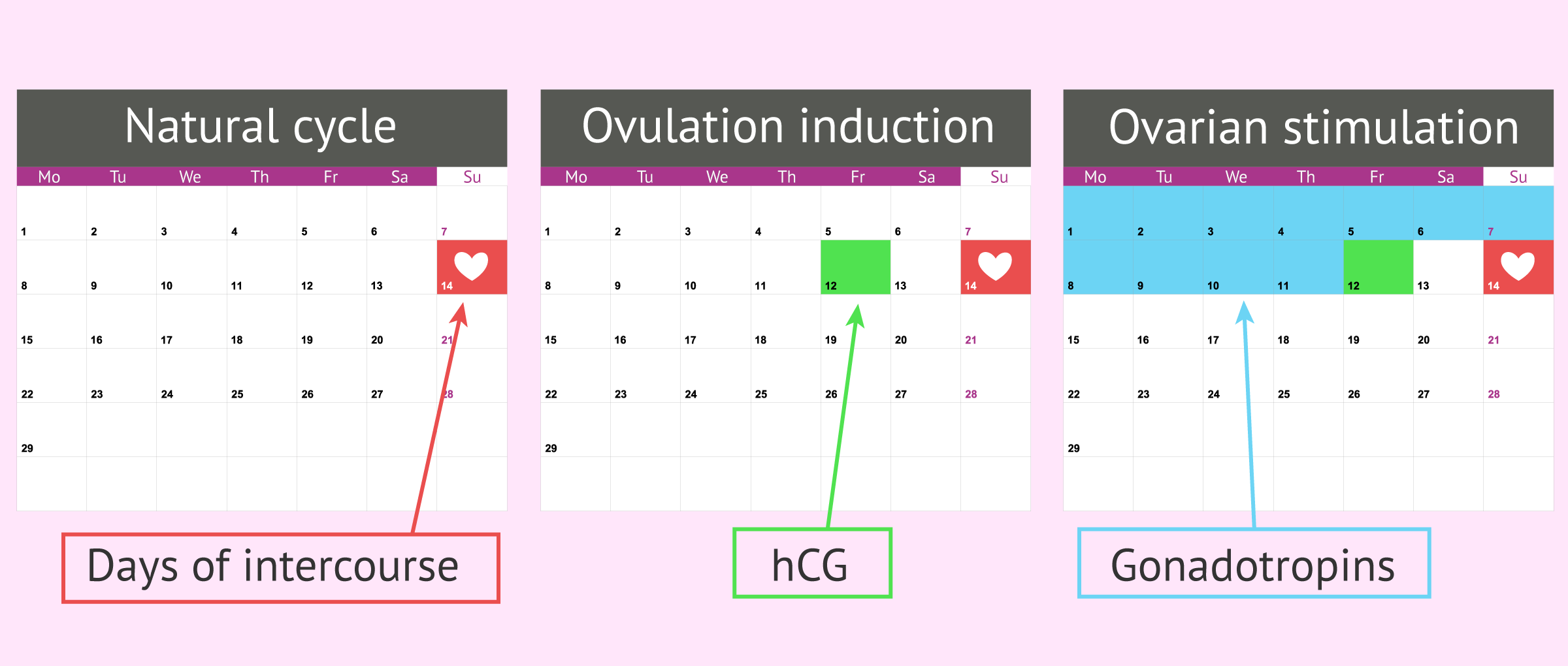
As we see in the following image, scheduling intercourse can be done during a natural cycle (without medication) or by giving the woman hormonal medication to better control follicular development and ovulation.
The following details the process for the different options of programmed intercourse.
Timed intercourse in natural cycle
The patient is not given hormonal medication but the ovarian cycle is allowed to take its natural course. Only the follicular growth is monitored by ultrasound and the LH (luteinizing hormone) level by blood tests.
The amount of LH is measured meticulously from the ninth day of menstruation and, once the LH level increases, the gynecologist schedules the perfect day for conception. This increases the chances of getting pregnant.
Natural cycle with ovulation induction
This is an intermediate process between the natural cycle and ovarian stimulation. The natural cycle with ovulation induction consists of controlling the natural growth of the egg and, when it is observed by ultrasound that the egg is already mature - that is, when the follicle is about 14 mm - the patient is given an injection of the hCG hormone.
This hormone triggers ovulation about 36 hours after subcutaneous administration, i.e. it mimics the endogenous LH peak. It is also possible to trigger ovulation by giving LH hormone.
Considering undergoing a fertility treatment? By getting your individual Fertility Report your will see different clinics especially selected for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
Thus, sexual intercourse is scheduled about 2 days after the hCG injection to facilitate the meeting of sperm and egg.
Ovarian stimulation
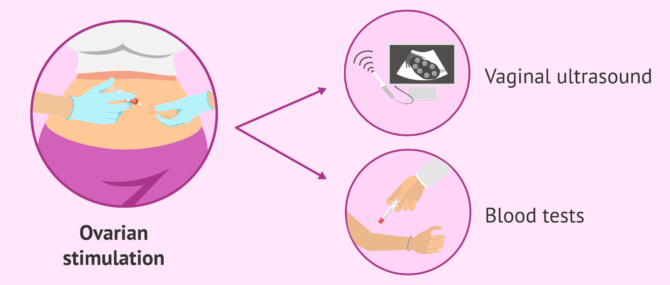
In this case, the woman receives a daily injection of gonadotropins (FSH, LH or HMG), hormones that act on the ovary. This treatment is given to stimulate the ovaries and promote the growth and maturation of eggs. This growth is monitored by ultrasound and blood tests.
Once the controls indicate that the egg is mature, the woman receives an hCG injection, which will trigger ovulation about 2 days after administration. Thus, the couple will be advised to maintain sexual intercourse 36 to 48 hours after administering hCG. As before, it is also possible to give LH.
The hormonal medication is given subcutaneously from the first day of the cycle, that is, the day when menstruation stops, and lasts between 8 and 14 days, depending on the response of each woman.
Oral clomiphene citrate and anti prolactin medications are also sometimes given to treat ovulatory problems in women and to optimize the ovarian cycle.
Since fertilization occurs naturally, careful monitoring of ovarian development is essential to prevent multiple pregnancy.
Advantages and disadvantages
Timed intercourse is the simplest assisted reproduction technique, and has numerous advantages:
- It is the least invasive reproductive technique and the closest to the physiological or natural process of fertilization.
- It has a lower cost. In fact, it is the most economical of the various infertility treatment options.
- It provides good results in young couples without specific fertility problems, as well as for couples in which the women have dysovulation (poor or irregular ovulation).
- This method is an alternative to sexual intercourse for couples who for religious or moral reasons do not want to resort to artificial insemination or in vitro fertilization.
On the flip side, we find the disadvantages why timed intercourse is not one of the most widely used techniques:
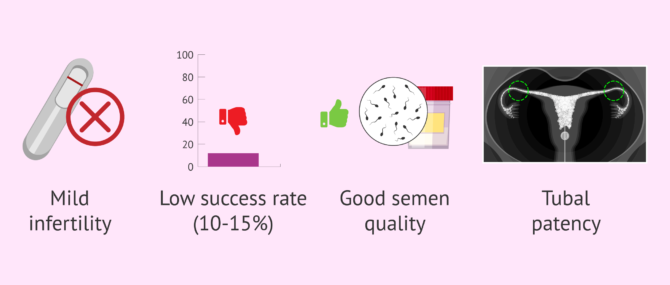
- The cases in which it is indicated are rare since it is used in mild or unexplained infertility.
- The pregnancy rate is low, no more than 10-15%. In fact, it has much lower pregnancy rates than artificial insemination or IVF.
- It is necessary that the semen is of good quality, that is to say, that it does not present serious alterations.
- As for the woman, she must have permeable tubes and good ovarian quality.
Timed intercourse reduces the stress of waiting for treatment and dramatically improves pregnancy rates in young couples with subfertility.
Subfertility is attributed to those couples who find it more difficult to achieve natural pregnancy due to different disorders, but not impossible. The latter would be defined as sterility or infertility.
However, the success rate is very low, forcing, in many cases, to resort to more complex techniques after 3-4 months of unsuccessful scheduled intercourse.
FAQs from users
When is timed intercourse indicated?
Timed intercourse is the simplest reproductive technique. It is used for simple cases, usually in young women with a short time of infertility. It is an easy and cheap technique that tries to optimise natural conditions.
It involves gently stimulating ovulation and monitoring the woman until she is close to ovulation. We help the ovulation process with an ovulation inducing drug and indicate the best time for the couple to have intercourse.
Timed intercourse is very often used in women with chronic anovulation, usually due to polycystic ovary syndrome, who need ovulation induction treatment in order to have regular cycles.
Is ovulation induction and time intercourse the same?
No, ovulation induction is the process by which the growth of 1 or several follicles of the ovary is produced thanks to the administration of drugs called Gonadotropins. After this, ovulation is usually triggered in a controlled manner.
Once this ovulation induction has been performed, intercourse can be programmed, that is to say, the couple can be told when ovulation will occur approximately and when they should have sexual intercourse to increase the chances of pregnancy.
Are better results obtained with programmed coitus in a natural cycle or with artificial insemination?
Better results are obtained with artificial insemination than with timed intercourse, both in natural and stimulated cycles.
What is the cost of timed intercourse?
Directed coitus is the most economical reproductive technique, since it only requires the payment of ultrasound and analytical controls and, in case of not doing it in a natural cycle, the cost of the medication administered.
The exact price will vary from one clinic to another depending on the cost that each center sets for the visits and controls. In relation to the medication, there is also variation depending on the indicated dose.
How does timed intercourse work?
Timed intercourse consists of performing sexual intercourse based on the timing of ovulation. This means that intercourse is timed to take into account the timing of ovulation and ejaculation.
Timed intercourse can be performed using the woman's natural cycle, natural cycle with ovulation induction and stimulated cycle with ovulation induction. The choice of one or another form of timed intercourse will depend on the characteristics of each couple.
How many days of abstinence are recommended before scheduled intercourse?
Generally, for any assisted reproduction technique, a sexual abstinence of between 3 and 5 days is recommended. However, each case is different and, therefore, it is advisable to consult with the specialist who will monitor the coitus.
What is the probability of having twins with directed intercourse?
If programmed intercourse is performed in a natural cycle or with ovulation induction, the probability of multiple pregnancy is very low and equal to the probability with sexual intercourse.
In the case of ovarian stimulation prior to intercourse, this probability increases. It is therefore essential to closely monitor ovarian growth caused by hormone medication.
Suggested for you
Due to the low effectiveness of timed intercourse in many situations, many couples wonder whether it is worth trying it or whether it is better to resort directly to artificial insemination. If you want to know the differences between the two techniques, I recommend you read this article: Programmed intercourse or artificial insemination?
There is the option of scheduled intercourse without medical supervision. To do this, it is useful to know what ovulation is and when it occurs. Get more information here: What is ovulation?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Abu Hashim H, Ombar O, Abd Elaal I. Intrauterine insemination versus timed intercourse with clomiphene citrate in polycystic ovary syndrome: a randomized controlled trial.Acta Obstet Gynecol Scand
. 2021 Jun 23. doi: 10.1111/aogs.14193 (View)
So Hyun Ahn, Inha Lee, SiHyun Cho, Hye In Kim, Hye Won Baek, Jae Hoon Lee, Yun Jeong Park, Heeyon Kim, Bo Hyon Yun, Seok Kyo Seo, Joo Hyun Park, Young Sik Choi, Byung Seok Lee. Predictive Factors of Conception and the Cumulative Pregnancy Rate in Subfertile Couples Undergoing Timed Intercourse With Ultrasound. Front Endocrinol (Lausanne). 2021 Apr 15;12:650883. doi: 10.3389/fendo.2021.650883 (View)
S van Wessel, T Hamerlynck, V Schutyser, C Tomassetti, C Wyns, M Nisolle, J Verguts, R Colman, S Weyers, J Bosteels. Anti-adhesion Gel versus No gel following Operative Hysteroscopy prior to Subsequent fertility Treatment or timed InterCourse (AGNOHSTIC), a randomised controlled trial: protocol. Hum Reprod Open. 2021 Feb 16;2021(1):hoab001. doi: 10.1093/hropen/hoab001 (View)
FAQs from users: 'When is timed intercourse indicated?', 'Is ovulation induction and time intercourse the same?', 'Are better results obtained with programmed coitus in a natural cycle or with artificial insemination?', 'What is the cost of timed intercourse?', 'How does timed intercourse work?', 'How many days of abstinence are recommended before scheduled intercourse?' and 'What is the probability of having twins with directed intercourse?'.
Authors and contributors