Cholesterol is a necessary lipid in our body, although it is often considered harmful. This molecule is present in cell membranes and is also important for the production of bile acids (which digest fats) and other molecules such as certain hormones.
Thus, cholesterol plays an important role in fertility and pregnancy, as it is the precursor of steroid hormones including estrogens, androgens, and progestogens.
Provided below is an index with the 9 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 3.
- 4.
- 5.
- 5.1.
- 5.2.
- 5.3.
- 5.4.
- 6.
- 7.
- 8.
- 9.
Normal cholesterol levels
Although cholesterol is synthesized in the liver, the cholesterol we ingest through our diet also contributes to the total values.
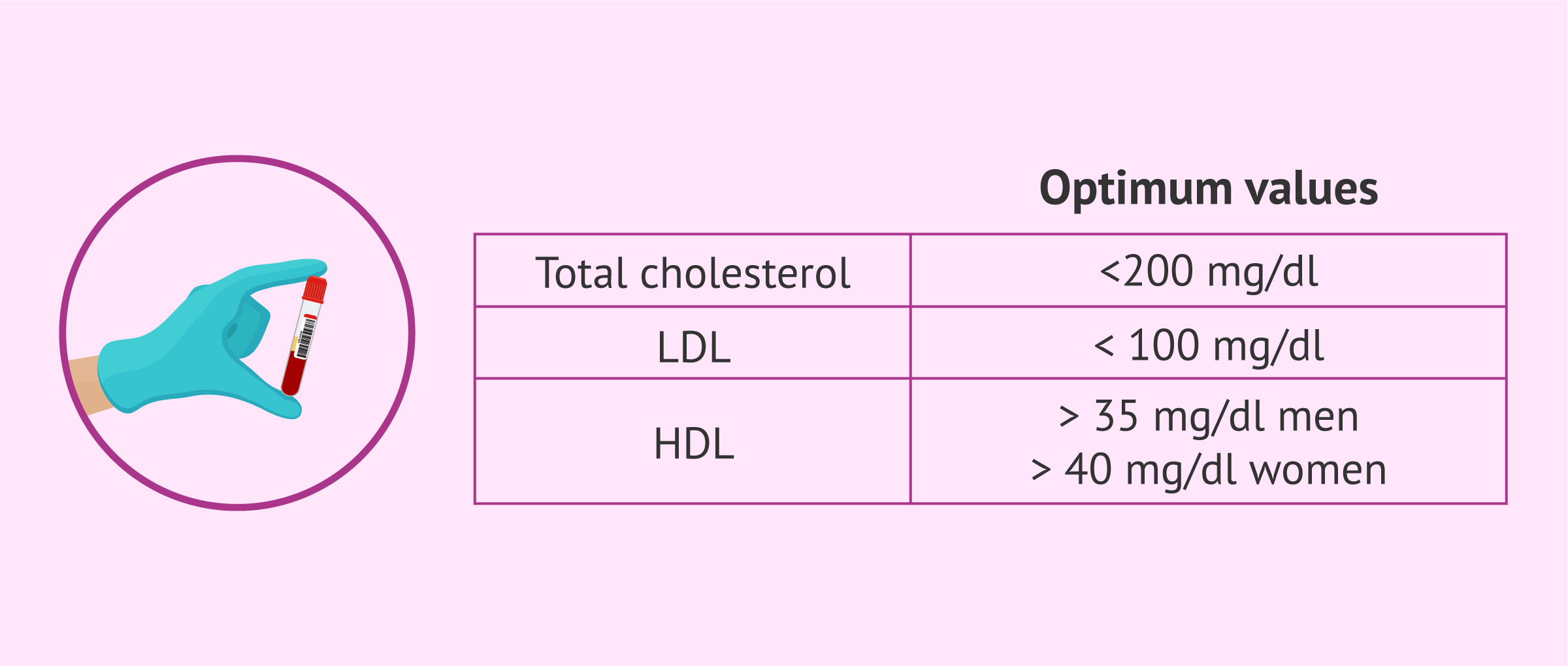
Therefore, to know the cholesterol levels, they can be evaluated by a blood test. Normally, three parameters will appear in the results of this test:
- Total cholesterol. It must be less than 200 mg/dl.
- LDL. It refers to low-density lipoproteins, the "bad cholesterol", and should be below 100 mg/dl.
- HDL. These are high-density lipoproteins or "good cholesterol" and ideally should be greater than 35 mg/dl in men and 40 mg/dl in women.
These lipoproteins are responsible for transporting cholesterol in the blood. LDL transports cholesterol from the liver to the tissues, while HDL takes the reverse route.
Cholesterol in pregnancy
When a woman is pregnant, cholesterol levels rise above the values considered normal for a non-pregnant adult woman.
This increase is more noticeable once the first trimester of pregnancy has passed, due to the hormonal and metabolic changes that women experience during gestation. However, high cholesterol during pregnancy should naturally decrease shortly after delivery.
However, it is common that cholesterol levels are not strictly controlled in pregnant women and, therefore, there is no range that establishes normal cholesterol values during pregnancy.
High cholesterol before pregnancy
In spite of what we have just mentioned, a greater follow-up is performed if the pregnant woman had a high cholesterol problem (hypercholesterolemia) prior to becoming pregnant.
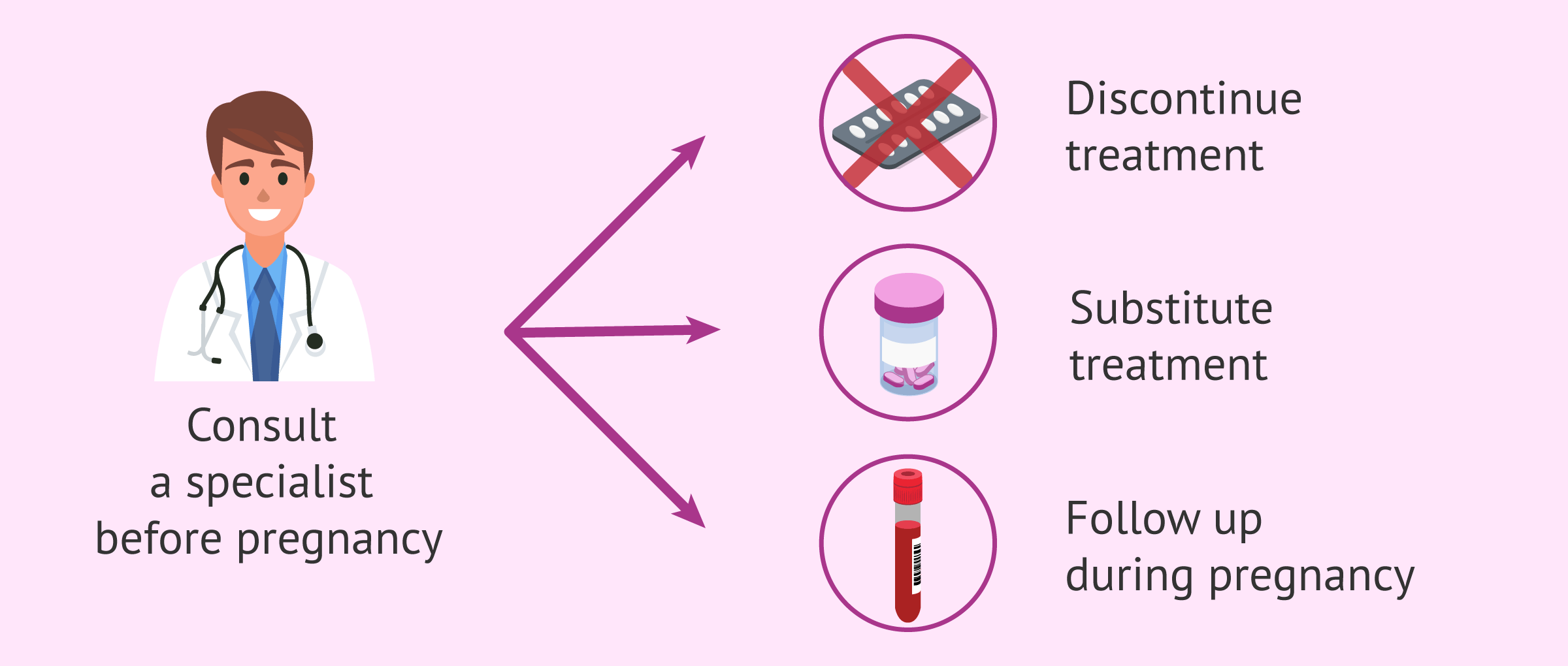
Therefore, it is necessary for a woman who already knows she has a high cholesterol problem to consult with her physician at the time she wants to seek gestation. Thus, the specialist will be able to control your cholesterol levels, assess whether it is necessary to replace your treatment with another medication during pregnancy and carry out an appropriate follow-up.
One of the main reasons is that statins, a very common type of cholesterol-lowering drug, are not considered appropriate during pregnancy and lactation. Because of this, the woman should stop this treatment even about two months before becoming pregnant or, failing that, when she becomes aware of the pregnancy.
Risks of high cholesterol in pregnancy
As we have mentioned, it is completely normal for cholesterol levels to increase during pregnancy, especially from the first trimester onwards.
However, if cholesterol is excessively elevated, it may be related to an increased risk of certain pregnancy complications. Among them, we can mention the following:
- Preterm delivery.
- Preeclampsia.
- Gestational diabetes
In addition, high cholesterol during pregnancy may be associated with certain complications for the offspring, such as elevated LDL cholesterol levels or increased severity of myocardial infarction.
Therefore, it is important to monitor cholesterol levels during pregnancy and adopt habits that help to keep them under control.
Recommendations
To prevent cholesterol levels from increasing to undesirable levels during pregnancy, pregnant women should keep the following recommendations in mind:
- Follow a balanced, varied diet, rich in fiber and low in saturated fats. Fat intake should come from healthy sources, such as fish, nuts and olive oil.
- Exercise adapted to pregnancy.
However, it is important to mention that it is also not ideal to have low cholesterol levels during pregnancy, as it is a molecule necessary for growth and for the development of fetal organs.
FAQs from users
Is it dangerous to have cholesterol above 300 in pregnancy?
It has been proposed that elevated cholesterol levels may cause damage to the fetal blood vessels, leading to a predisposition to develop cholesterol problems, arteriosclerosis, and cardiovascular pathologies in the future.
Read more
How should cholesterol levels be in the third trimester of pregnancy?
Normally, in the second trimester of pregnancy, cholesterol levels begin to increase above levels considered normal for a woman who is not pregnant. Therefore, in the third trimester of pregnancy, cholesterol values will be increased.
This rise in cholesterol levels is considered physiological during pregnancy. However, if cholesterol values increase excessively, pregnancy complications such as preeclampsia, preterm delivery and gestational diabetes may be associated with it.
Do I have to lower my cholesterol levels to get pregnant?
It is advisable for cholesterol levels to be at adequate levels, both for seeking a pregnancy (either naturally or through assisted reproduction techniques) and for other important aspects such as having a good cardiovascular health.
In addition, if cholesterol levels are elevated in women, the time to achieve a pregnancy may be longer than if the levels are adequate.
Therefore, the best thing to do is to try to reduce cholesterol levels with a healthy and varied diet, avoiding bad habits such as smoking and exercising frequently.
Is treatment for high cholesterol necessary during pregnancy?
It will depend on the situation. Patients with high cholesterol prior to becoming pregnant should discontinue treatment if they are taking statins, since their use is not recommended during pregnancy.
However, since cholesterol levels increase during pregnancy, it will be convenient to control their values, either by means of a healthy diet low in saturated fats or, if the specialist considers it appropriate, with the help of a recommended drug.
Recommended readings
If you are pregnant, you may want to get information about vitamins to take during pregnancy. To do so, you can visit the following link: What vitamins to take during pregnancy?
On the other hand, you may also be interested in the food you should eat while breastfeeding. In this case, we recommend that you read the following article: Feeding and nutrition of the mother during lactation
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Bartels Ä, Egan N, Broadhurst DI, Khashan AS, Joyce C, Stapleton M, O'Mullane J, O'Donoghue K. Maternal serum cholesterol levels are elevated from the 1st trimester of pregnancy: a cross-sectional study. J Obstet Gynaecol. 2012 Nov;32(8):747-52. (Ver)
Cacciatore F, Bruzzese G, Abete P, Russo G, Palinski W, Napoli C. Maternal hypercholesterolaemia during pregnancy affects severity of myocardial infarction in young adults. Eur J Prev Cardiol. 2021 Oct 18:zwab152. (Ver)
Cai X, Liang N, Wang H, Gao A, Xiao R, Yu H. Lipidomic profiles of maternal blood at the earlier stage of gestation and umbilical venous blood in response to supraphysiological hypercholesterolemia versus physiological hypercholesterolemia: An evidence of potential biomarkers and early intervention. Biochim Biophys Acta Mol Cell Biol Lipids. 2020 Mar;1865(3):158587. (Ver)
Cantin C, Arenas G, San Martin S, Leiva A. Effects of lipoproteins on endothelial cells and macrophages function and its possible implications on fetal adverse outcomes associated to maternal hypercholesterolemia during pregnancy. Placenta. 2021 Mar;106:79-87. (Ver)
Cantin C, Fuenzalida B, Leiva A. Maternal hypercholesterolemia during pregnancy: Potential modulation of cholesterol transport through the human placenta and lipoprotein profile in maternal and neonatal circulation. Placenta. 2020 May;94:26-33. (Ver)
Chen Q, Chen H, Xi F, Sagnelli M, Zhao B, Chen Y, Yang M, Xu D, Jiang Y, Chen G, Luo Q. Association between maternal blood lipids levels during pregnancy and risk of small-for-gestational-age infants. Sci Rep. 2020 Nov 16;10(1):19865. (Ver)
Ferriols E, Rueda C, Gamero R, Vidal M, Payá A, Carreras R, Flores-le Roux JA, Pedro-Botet J. Comportamiento de los lípidos durante la gestación y su relación con acontecimientos obstétricos desfavorables [Relationship between lipid alterations during pregnancy and adverse pregnancy outcomes]. Clin Investig Arterioscler. 2016 Sep-Oct;28(5):232-244. Spanish. (Ver)
Fuenzalida B, Cantin C, Kallol S, Carvajal L, Pastén V, Contreras-Duarte S, Albrecht C, Gutierrez J, Leiva A. Cholesterol uptake and efflux are impaired in human trophoblast cells from pregnancies with maternal supraphysiological hypercholesterolemia. Sci Rep. 2020 Mar 24;10(1):5264. (Ver)
Jin WY, Lin SL, Hou RL, Chen XY, Han T, Jin Y, Tang L, Zhu ZW, Zhao ZY. Associations between maternal lipid profile and pregnancy complications and perinatal outcomes: a population-based study from China. BMC Pregnancy Childbirth. 2016 Mar 21;16:60. (Ver)
Kallol S, Albrecht C. Materno-fetal cholesterol transport during pregnancy. Biochem Soc Trans. 2020 Jun 30;48(3):775-786. (Ver)
Wu Y, Sun G, Zhou X, Zhong C, Chen R, Xiong T, Li Q, Yi N, Xiong G, Hao L, Yang N, Yang X. Pregnancy dietary cholesterol intake, major dietary cholesterol sources, and the risk of gestational diabetes mellitus: A prospective cohort study. Clin Nutr. 2020 May;39(5):1525-1534. (Ver)
FAQs from users: 'Is it dangerous to have cholesterol above 300 in pregnancy?', 'How should cholesterol levels be in the third trimester of pregnancy?', 'Do I have to lower my cholesterol levels to get pregnant?' and 'Is treatment for high cholesterol necessary during pregnancy?'.
Authors and contributors
More information about Cristina Algarra Goosman





Hello, I have always had cholesterol problems, I have been medicated but now I’m afraid that it will get out of control, is there anything special I can do?
Hello Kaylin,
It is important that you consult with your doctor if the treatment you were previously taking is compatible with pregnancy, and if not find a medication that replaces the effect of the one you were taking before and is compatible with pregnancy.
It is advisable to lead a healthy life and try to keep cholesterol levels as low as possible because they naturally increase during pregnancy and if not controlled can be harmful to the health of the mother and fetus.
I hope I have helped you.
Best regards.
Hi, I have a rather sedentary lifestyle and I don’t take care of my food, does that mean I have high cholesterol? How can I measure it?
Hello Ariana1992,
Lifestyle, nutrition, and physical activity can condition a person’s cholesterol levels. It is important to perform tests, usually blood tests, for the doctor to determine cholesterol levels.
This way you will be able to know if they are elevated or considered normal. People with elevated cholesterol levels on average take longer to get pregnant, so a lifestyle change is recommended in these cases.
I hope I have helped you.
Best regards.