A woman may notice certain changes in her vaginal discharge throughout the menstrual cycle and even take notes to identify the pattern of these changes. These variations are completely normal, due to the different hormone levels in the different phases of the menstrual cycle.
However, unusual changes in the quantity, color, consistency and odor of vaginal discharge are a reason for consulting a specialist.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 5.
- 6.
- 7.
- 8.
Normal vaginal discharge
A woman's vaginal discharge may undergo certain changes without indicating a problem. These normal changes occur throughout the menstrual cycle, as variations in hormone levels lead to different characteristics of cervical mucus.
Cervical mucus is a secretion of the cells of the cervix, so it is part of the fluid that the woman expels through the vagina. However, this discharge may vary in appearance and quantity depending on the time of the woman's cycle:
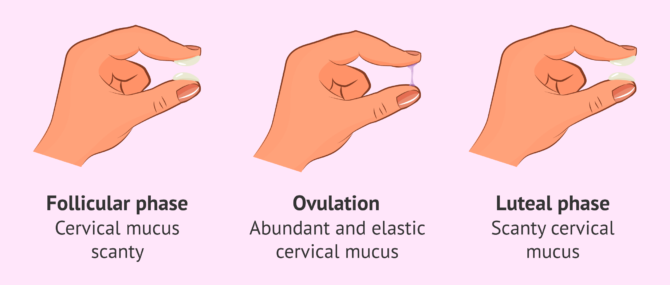
- Follicular Phase Once menstruation is over, cervical mucus is very thin. However, as the estrogen level increases, the mucus will increase in quantity and become viscous and sticky.
- Ovulation. The amount of cervical mucus will be maximal and will have an appearance similar to raw egg white, i.e., more transparent, watery and elastic.
- Luteal phase Cervical mucus again becomes thinner and thicker.
These secretions may turn a whitish or yellowish color when exposed to air and dried, but these are normal variations.
Thus, the vaginal fluid undergoes variations when a woman is of reproductive age (if a hormonal contraceptive method is not used, which would alter this pattern). However, due to the hormonal changes that occur at menopause, it is common for fluid to be thinner and vaginal dryness to occur.
In addition, it is also completely normal to notice a different and more abundant vaginal discharge with sexual arousal, as this is produced for natural lubrication.
Changes in vaginal discharge
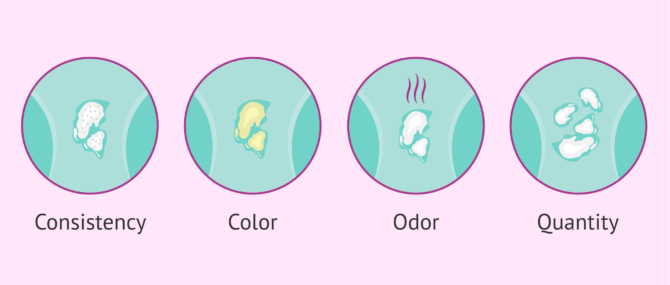
It is important for the woman to know how to detect when there is a change in vaginal discharge that deviates from the normal variations mentioned above. These changes may be seen in any of these vaginal discharge characteristics:
- Consistency
- the vaginal discharge becomes more lumpy or pasty in consistency or may even be slightly foamy.
- Color.
- vaginal discharge may become more yellowish, whitish, grayish or even greenish. It may also have a brownish color in the days around menstruation, which would be completely normal.
- Odor
- vaginal discharge is usually odorless or mild-smelling, so a foul-smelling or strong-smelling discharge may be one of the most striking changes.
- Quantity
- the woman may notice an increased amount of vaginal fluid.
Thus, for any variation of this type that occurs more or less suddenly in the vaginal discharge, it is advisable to consult a specialist. In addition, the woman should indicate if this change occurs along with other symptoms such as vaginal itching or burning, or even fever or abdominal pain.
Normal vaginal discharge
When a woman notices an increase in vaginal fluid, a strong odor, or a different consistency and color, it may indicate an infection.
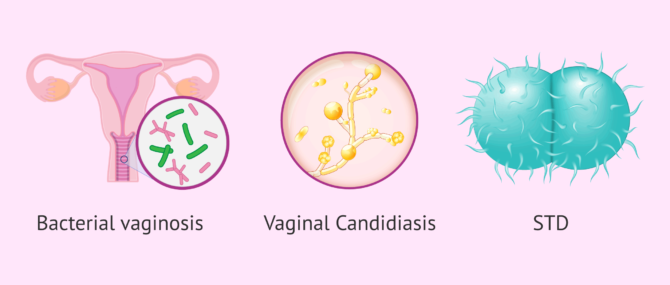
- Bacterial vaginosis
- is due to the proliferation of certain bacteria that normally inhabit the vagina. This causes a whitish to grayish or even yellowish-greenish discharge with a strong fishy odor.
- Vaginal candidiasis
- infection caused by fungi found in the vagina, when there is an imbalance and they increase their population. One of its symptoms is a change in vaginal discharge, which varies from a whitish, slightly watery discharge to a thick, abundant white discharge similar to cottage cheese.
- Chlamydia
- is a sexually transmitted disease (STD) of bacterial origin (caused by Chlamydia trachomatis). Only some women present symptoms, such as a whitish-yellowish, lumpy discharge with a strong odor.
- Gonorrhea
- STD caused by Neisseria gonorrhoeae that can cause abnormalities in the discharge such as a more yellowish color, although it often produces no symptoms.
- Trichomoniasis
- this STD is caused by the parasite Trichomonas vaginalis. It produces a yellowish, grayish or greenish vaginal discharge, which may be frothy and foul smelling.
Finally, a brown or pinkish discharge from bleeding that is not related to menstruation is a reason to consult a gynecologist to rule out cervical cancer.
Therefore, in the presence of abnormal vaginal discharge, a specialist should be consulted. In this way, depending on the causes, you will be able to indicate the most appropriate treatment.
FAQs from users
Are there any home remedies for foul-smelling discharge?
First of all, in the presence of a discharge with a strong or unpleasant odor (which some women describe as fishy), a specialist should be consulted, as it may be a symptom that the woman is suffering from an infection. Thus, depending on the cause, the specialist will provide the most appropriate treatment.
However, we can perform certain preventive remedies, such as:
- Avoiding STDs with barrier contraceptive methods such as condoms.
- Use cotton underwear, which is more breathable than synthetic, and do not wear tight-fitting garments.
- Take yogurt, for example, as probiotics may contribute to a healthy vaginal flora.
- Do not use douches or perfumed products.
- Do not forget tampons inside the vagina.
De este modo, se evitan algunas de las situaciones que podrían llevar a tener un flujo vaginal con mal olor.
Can there be changes in flow due to a urinary tract infection?
When a woman notices changes in vaginal discharge, she should see a specialist. It is possible that the symptoms she notices, such as vaginal pain or itching, are caused by another type of infection and are not due to a urinary tract infection or cystitis.
What does a yeast-smelling discharge mean?
Un flujo que tiene olor a levadura puede indicar una infección vaginal por hongos. Yeast infections are usually caused by Candida albicans and produce a thick, whitish discharge that is usually odorless, but may smell faintly of yeast.
Recommended reading
If you want to learn more about cervical mucus and its variations during the menstrual cycle, you can read the following article: How is cervical mucus during ovulation and fertile days?
On the other hand, if you want to know more about sexually transmitted diseases (STDs), we recommend you to visit this link: Sexually Transmitted Diseases (STDs) in men and women.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Chatzivasileiou P, Vyzantiadis TA. Vaginal yeast colonisation: From a potential harmless condition to clinical implications and management approaches-A literature review. Mycoses. 2019 Aug;62(8):638-650. (See)
Chen X, Lu Y, Chen T, Li R. The Female Vaginal Microbiome in Health and Bacterial Vaginosis. Front Cell Infect Microbiol. 2021 Apr 7;11:631972. (See)
Cooke G, Watson C, Deckx L, Pirotta M, Smith J, van Driel ML. Treatment for recurrent vulvovaginal candidiasis (thrush). Cochrane Database Syst Rev. 2022 Jan 10;1(1):CD009151. (See)
De Seta F, Lonnee-Hoffmann R, Campisciano G, Comar M, Verstraelen H, Vieira-Baptista P, Ventolini G, Lev-Sagie A. The Vaginal Microbiome: III. The Vaginal Microbiome in Various Urogenital Disorders. J Low Genit Tract Dis. 2022 Jan 1;26(1):85-92. (See)
Deka N, Hassan S, Seghal Kiran G, Selvin J. Insights into the role of vaginal microbiome in women's health. J Basic Microbiol. 2021 Dec;61(12):1071-1084. (See)
Hlatshwayo M, Reno HEL, Yarbrough ML. STI update: Testing, treatment, and emerging threats. Cleve Clin J Med. 2019 Nov;86(11):733-740. (See)
Kalia N, Singh J, Kaur M. Microbiota in vaginal health and pathogenesis of recurrent vulvovaginal infections: a critical review. Ann Clin Microbiol Antimicrob. 2020 Jan 28;19(1):5. (See)
Lev-Sagie A, De Seta F, Verstraelen H, Ventolini G, Lonnee-Hoffmann R, Vieira-Baptista P. The Vaginal Microbiome: II. Vaginal Dysbiotic Conditions. J Low Genit Tract Dis. 2022 Jan 1;26(1):79-84. (See)
Mendling W. Vaginal Microbiota. Adv Exp Med Biol. 2016;902:83-93. (See)
Rodríguez-Cerdeira C, Gregorio MC, Molares-Vila A, López-Barcenas A, Fabbrocini G, Bardhi B, Sinani A, Sánchez-Blanco E, Arenas-Guzmán R, Hernandez-Castro R. Biofilms and vulvovaginal candidiasis. Colloids Surf B Biointerfaces. 2019 Feb 1;174:110-125. (See)
Saraf VS, Sheikh SA, Ahmad A, Gillevet PM, Bokhari H, Javed S. Vaginal microbiome: normalcy vs dysbiosis. Arch Microbiol. 2021 Sep;203(7):3793-3802. (See)
Tuddenham S, Hamill MM, Ghanem KG. Diagnosis and Treatment of Sexually Transmitted Infections: A Review. JAMA. 2022 Jan 11;327(2):161-172. (See)
FAQs from users: 'Are there any home remedies for foul-smelling discharge?', 'Can there be changes in flow due to a urinary tract infection?' and 'What does a yeast-smelling discharge mean?'.
Authors and contributors