Genital herpes is a sexually transmitted infection(STI) that can be transmitted through vaginal, anal or oral sex. However, mother-to-child transmission during birth(neonatal herpes) is also possible.
The most characteristic symptom of genital herpes infection (although symptoms may be absent) is the presence of blisters in the genital or anal area, which may rupture resulting in painful sores that will heal into scabs. In addition, after infection, the virus remains latent in the body and may cause new outbreaks or recurrences.
On the other hand, it is important to know that genital herpes can be transmitted even when no symptoms are present.
Provided below is an index with the 11 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 3.
- 4.
- 5.
- 6.
- 7.
- 7.1.
- 7.2.
- 8.
- 9.
- 10.
- 11.
What is genital herpes and how is it transmitted?
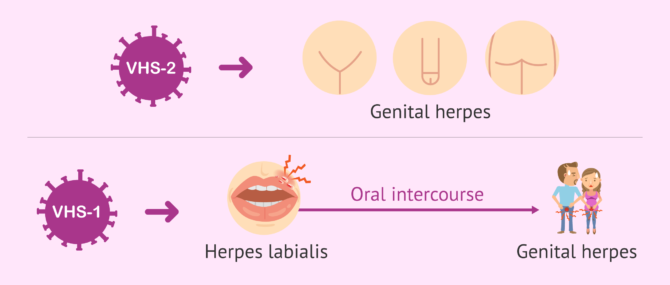
Genital herpes is a sexually transmitted infection (STI) that can be caused by herpes simplex virus type 1(HSV-1) or herpes simplex virus type 2(HSV-2).
While HSV-2 is the most common virus causing genital herpes, HSV-1 is more commonly associated with oral or labial herpes. However, HSV-1 can be transmitted to the genital area during oral sex, and HSV-1 can cause herpetic lesions on the genitals.
Thus, genital herpes can be transmitted during vaginal, anal or oral sex. The virus enters the body through the mucous membranes (such as those covering the genitals or mouth), but can also enter the body through the skin if it has small wounds or scratches.
It is important to mention that the virus can be transmitted to another person even if, at the time of sexual intercourse, the person with herpes has no symptoms.
In addition, the virus can also be transmitted at the time of delivery from a mother with the infection to her newborn (before birth is less common), which can cause serious problems for the baby.
On the other hand, transmission of genital herpes by objects (such as toilets) that a person with the infection has used is quite unlikely, since the virus does not survive for long outside the body.
Symptoms
Symptoms may be absent or very mild following HSV infection, leading to symptoms going unnoticed or being attributed to other causes. Therefore, it is quite common for a person with genital herpes to have this STI without knowing it.
In the case of presenting symptoms, these may be:
- Genital pain, itching, burning.
- Small, light-colored blisters in the genital or anal area (they may also appear on the buttocks and inner thighs) that give rise to painful sores or ulcers when they break and, later, to scabs in the healing process.
- Swollen groin nodes, headache, muscle pain, malaise and fever, these symptoms being more common in the initial outbreak.
Symptoms usually appear 2-12 days after infection. However, the virus can be dormant for years without symptoms, making it difficult to determine when infection occurred.
Recurrences or outbreaks
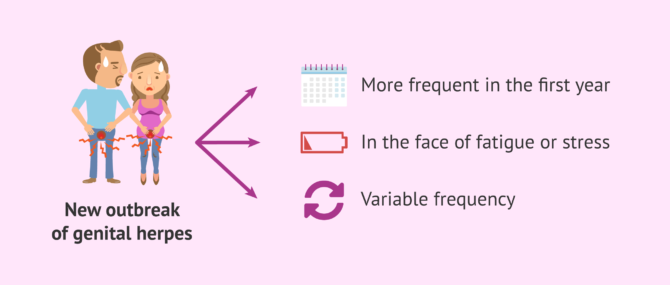
Once a person is infected with the herpes simplex virus, despite having outgrown the symptoms, the virus remains inactive (dormant) within the body and may reactivate from time to time (especially in the first year after infection).
At this point, it is important to mention that these recurrences are more common when genital herpes is caused by HSV-2.
The person may notice some itching and pain before the sores appear. Some of the factors that have been related to the appearance of a new outbreak would be menstruation, fatigue or tiredness and stress.
These new outbreaks may be infrequent or very frequent (even several per year), but are usually less intense and shorter than the initial outbreak. In addition, these recurrences may become less and less frequent over the years.
What to do to alleviate symptoms?
In order to try to alleviate the pain caused by genital herpes sores and have them heal as soon as possible, it will be important:
- Wash the sores carefully with soap and water.
- Dry the sores well by gently patting them dry.
- Wear loose-fitting clothing and, preferably, avoid synthetic fabrics and opt for cotton underwear.
- Put cold on the area of the sores.
- Take antiviral treatment as prescribed by the specialist and consult if analgesics can be taken to try to relieve the pain.
On the other hand, it is very important to wash hands thoroughly after touching the sores, otherwise the virus could spread to other areas of the body or to other people.
Diagnosis
Sometimes, the specialist can make a diagnosis of genital herpes based on symptoms and examination of the genital area, but it is common for a sample of the sores to be taken for laboratory confirmation of the diagnosis.
However, if no sores are present at that time (asymptomatic persons or between outbreaks), a blood test may be performed. This blood sample is used to determine if HSV antibodies are present, which would confirm the infection.
Treatment
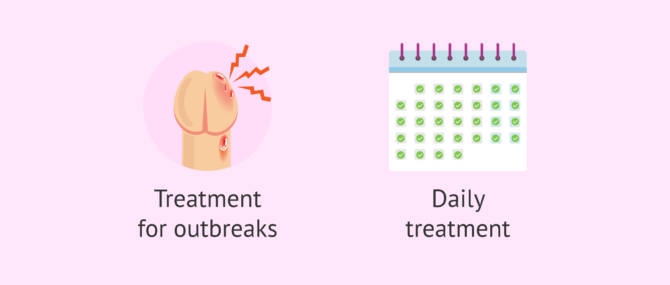
Currently, there is no cure for genital herpes. However, taking antiviral drugs (such as acyclovir, valacyclovir or famciclovir) when there is an outbreak of genital herpes may decrease symptoms and make symptoms last fewer days. In the event of a new outbreak, after identifying the first symptoms, antiviral treatment should ideally be started as soon as possible.
If outbreaks occur on a frequent basis, antivirals can be taken daily to try to prevent it and thus reduce the occurrence of new outbreaks. In addition, daily antivirals may reduce the risk of transmission to sexual partners.
Therefore, a specialist should be consulted, who will prescribe the most appropriate way to take the antivirals according to the particular situation.
Prevention
To prevent genital herpes, being an STI, the most effective measure would be sexual abstinence. However, a sexually active person should always use a condom correctly during sexual intercourse (or latex dental dams for oral sex).
This is to prevent contracting (or transmitting) genital herpes, as many people have the infection without knowing it and genital herpes can be transmitted even in the absence of symptoms. If you know you have genital herpes, you should tell your sexual partner.
However, condoms reduce the risk, but if the virus is present in areas that condoms do not protect, infection or transmission is possible.
In any case and even when using a condom, sexual intercourse should be avoided from the onset of symptoms and when there are active lesions or sores, until symptoms are no longer present.
Genital herpes and pregnancy
A pregnant woman should report any suspected or diagnosed genital herpes to her physician, as it could lead to miscarriage or premature delivery.
In addition, it is important to avoid getting genital herpes during pregnancy, especially when the pregnancy is coming to an end, as this would increase the chances of transmitting it to the baby during delivery.
On the other hand, if the woman has an outbreak of genital herpes at the time of delivery, the specialist will recommend a cesarean section.
The goal is to try to prevent the baby from getting neonatal herpes, which could cause serious complications and even death.
FAQs from users
Is there an increased risk of HIV infection if you have genital herpes?
Yes, genital herpes sores can be a route of entry for the human immunodeficiency virus (HIV), increasing the risk of HIV infection.
On the other hand, if the person with genital herpes is HIV-positive, the risk of transmitting HIV to a sexual partner is also increased.
Can oral herpes lead to genital herpes?
Yes, a person with cold sores or oral herpes can transmit the virus to their sexual partner's genital area if they have oral sex, potentially causing genital herpes.
It is more common for herpes simplex virus type 1 (HSV-1) to cause cold sores and herpes simplex virus type 2 (HSV-2) to cause genital herpes, but through oral sex, HSV-1 can cause genital herpes
Suggested for you
If you want to know more about seminal quality, we recommend you to read this article: Sexually transmitted diseases (STDs) in men and women.
On the other hand, if you want to know more about condoms, you can click on the following link: Contraceptive methods: types, effectiveness, risks and prices.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Bennett C, Rebafka A, Carrier J, Cook S, Edwards D. Impact of primary and recurrent genital herpes on the quality of life of young people and adults: a mixed methods systematic review. JBI Evid Synth. 2022 Jun 1;20(6):1406-1473. doi: 10.11124/JBIES-21-00057. PMID: 35199654. (View)
Devine A, Xiong X, Gottlieb SL, de Mello MB, Fairley CK, Ong JJ. Health-related quality of life in individuals with genital herpes: a systematic review. Health Qual Life Outcomes. 2022 Feb 16;20(1):25. doi: 10.1186/s12955-022-01934-w. PMID: 35172828; PMCID: PMC8848826. (View)
Fuente del contenido: Herpes genital. Autor original Dr. Ignacio Antépara Ercoreca y revisado por Dra. Yolanda Patricia Gómez González. Sitio Web tuotromedico. [View]
Majewska A, Mlynarczyk-Bonikowska B. 40 Years after the Registration of Acyclovir: Do We Need New Anti-Herpetic Drugs? Int J Mol Sci. 2022 Mar 22;23(7):3431. doi: 10.3390/ijms23073431. PMID: 35408788; PMCID: PMC8998721. (View)
Ngalame AN, Mubiana-Mbewe M, Dionne JA. Genital Tract Infections in Women, Pregnancy and Neonates. Obstet Gynecol Clin North Am. 2022 Dec;49(4):751-769. doi: 10.1016/j.ogc.2022.07.004. PMID: 36328678. (View)
Omarova S, Cannon A, Weiss W, Bruccoleri A, Puccio J. Genital Herpes Simplex Virus-An Updated Review. Adv Pediatr. 2022 Aug;69(1):149-162. doi: 10.1016/j.yapd.2022.03.010. Epub 2022 Jun 21. PMID: 35985707. (View)
Rathbun MM, Szpara ML. A holistic perspective on herpes simplex virus (HSV) ecology and evolution. Adv Virus Res. 2021;110:27-57. doi: 10.1016/bs.aivir.2021.05.001. Epub 2021 Jun 26. PMID: 34353481; PMCID: PMC8943685. (View)
Tuddenham S, Hamill MM, Ghanem KG. Diagnosis and Treatment of Sexually Transmitted Infections: A Review. JAMA. 2022 Jan 11;327(2):161-172. doi: 10.1001/jama.2021.23487. PMID: 35015033. (View)
Workowski KA, Bachmann LH, Chan PA, et al. Sexually Transmitted Infections Treatment Guidelines, 2021. MMWR Recomm Rep 2021;70(No. RR-4):1–187. DOI: http://dx.doi.org/10.15585/mmwr.rr7004a1. (View)
Zhu S, Viejo-Borbolla A. Pathogenesis and virulence of herpes simplex virus. Virulence. 2021 Dec;12(1):2670-2702. doi: 10.1080/21505594.2021.1982373. PMID: 34676800; PMCID: PMC8923070. (View)
FAQs from users: 'Is there an increased risk of HIV infection if you have genital herpes?' and 'Can oral herpes lead to genital herpes?'.
Author
Find the latest news on assisted reproduction in our channels.