According to WHO (World Health Organization) data, more than half a million women die each year due to complications arising during pregnancy or childbirth.
Among these complications, postpartum hemorrhage is the leading cause of maternal mortality, accounting for more than 35% of all maternal deaths per year. However, these data are mainly associated with developing countries.
The reasons for postpartum hemorrhage are grouped by the 4T rule: tone, trauma, tissue and thrombin. Depending on the severity of the obstetric hemorrhage, specialists will apply different treatments to control the bleeding.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 3.
- 4.
- 4.1.
- 4.2.
- 5.
- 6.
- 7.
- 8.
What is postpartum hemorrhage?
Postpartum hemorrhage (PPH) is defined as the loss of 500 ml of blood or more during a vaginal delivery or within 24 hours after the third stage of labor. There are also those who add to this definition the loss of 1000 ml of blood after cesarean section. However, there is no consensus on the definition of postpartum hemorrhage; there are several definitions depending on the estimated blood loss.
There are two general types of postpartum hemorrhage:
- Primary
- occurs within 24 hours after delivery.
- Secondary
- occur between 24 hours and 6 months after delivery.
It should be noted that it is normal to have bleeding after childbirth. However, the gestational complication of postpartum hemorrhage occurs when the amount of blood released is greater than usual.
Why does postpartum hemorrhage occur?
There are multiple causes of postpartum hemorrhage, although they are usually grouped into the four T's: tone, trauma, tissue and thrombin.
Therefore, the reasons at the level of the uterus that can cause postpartum hemorrhage with the following:
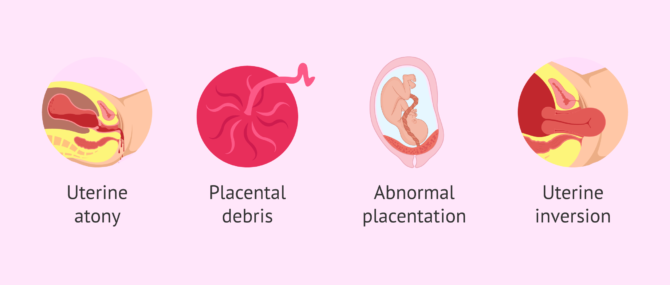
- Uterine atony: inability of the uterus to contract. It is the most common cause of bleeding after childbirth.
- Placental remains: when portions of placenta or fetus remain attached. It is the most common cause of late postpartum hemorrhage.
- Abnormal placentation: when the placenta invades beyond the endometrium into the muscle wall or other neighboring organs such as the bladder.
- Uterine inversion: inversion of the uterus within its own cavity, descending through the vagina until it emerges through the vulva. It occurs immediately after delivery and seriously endangers the mother's life. It can be a complete or incomplete inversion depending on its degree of inversion and depending on the acute or chronic duration.
- Uterine rupture: usually caused by the existence of a scar in the wall of the uterus. Sometimes, however, there may be a tearing of the uterus during pregnancy or the dilation phase.
However, there are also non-uterine causes of bleeding after childbirth such as hematomas, uterine tract injuries or coagulation problems associated with severe preeclampsia and placental abruption.
Risk Factors
Although the causes of postpartum bleeding are diverse, many of them can be prevented and/or treated to avoid endangering a woman's health. In addition, some risk factors are known to increase the likelihood of postpartum bleeding. Some of these factors are listed below:
- Excess amniotic fluid or polyhydramnios.
- Being a woman over 35 years.
- Twin pregnancy.
- Previous uterine curettage.
- Presence of uterine fibroids.
- Prolonged labor.
- Maternal pathologies such as diabetes, lupus, anemia, etc.
However, not all women in any of these situations will experience postpartum hemorrhage. They are only factors that may be associated with an increased tendency to bleed after childbirth.
Treatment of postpartum hemorrhage
First of all, it is essential to detect possible risk factors to try to prevent exaggerated bleeding from occurring after childbirth. If, despite having control, hemorrhage occurs after delivery, the next step would be to monitor the mother. The specialists will try to stabilize the mother hemodynamically.
Sometimes, bleeding after childbirth ends after a massage on the uterus. However, at other times it is necessary to resort to pharmacological treatment. In these cases, oxytocin, misoprostol, ergometrine or other synthetic prostaglandins are usually used.
When pharmacological treatment does not work and fails to stop the bleeding, the following options would be:
- Intrauterine balloon or Bakri balloon
- is a non-invasive technique that helps treat uterine atony. Therefore, it is a strategy to be applied when there is obstetric hemorrhage. It is a silicone balloon with a channel at the end of a catheter to drain uterine debris.
- Selective arterial embolization
- consists of introducing a catheter into the femoral artery until it reaches, for example, the uterine artery and a vascular occlusion is performed.
- Placement of hypogastric artery ligation
- is the most conservative option before going on to hysterectomy, so it would be convenient to apply in women with reproductive desire in the future after childbirth.
The last therapeutic resort if the bleeding cannot be stopped after delivery would be to perform a hysterectomy, that is, to remove the woman's uterus. However, this is not usually the case, except if none of the above treatments work.
FAQs from users
What do the 4Ts of postpartum haemorrhage refer to?
The 4Ts with the causes of bleeding that occur after childbirth. Specifically, this term refers to: tone, trauma, tissue and thrombin.
Tone or uterine atony is the most common cause of obstetric haemorrhage and is usually caused by overdistension of the uterus. Thus, multiple pregnancy is a risk factor for uterine atony.
Trauma accounts for 20% of cases of postpartum haemorrhage and is due to tearing of the birth canal, inversion of the uterus or uterine rupture.
Nine per cent of postpartum haemorrhages are due to retained placental tissue or placental abnormalities.
Finally, the remaining 1% are due to coagulation or thrombin abnormalities.
Can postpartum haemorrhage be prevented?
Sometimes postpartum haemorrhage is caused by some unknown factor and cannot be prevented. However, the World Health Organisation (WHO) advises the use of uterotonic agents such as oxytocin to prevent postpartum haemorrhage.
Another example of a recommended uterotonic medication during childbirth is misoprostol. In addition, it is important to carry out controlled umbilical cord traction and to monitor uterine tone at all times.
Suggested for you
If you are interested in knowing how to prepare for the moment of delivery and be more relaxed, we recommend you to visit the following article: How to prepare for childbirth - Theory and practice.
Also, if what you would like to know is when your period will return after giving birth, then we invite you to continue reading here: Menstruation after childbirth: how long does it take to come down?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
A. Aldo Solari, G. Caterina Solari, F. Alex Wash, G. Marcos Guerrero, G. Omar Enríquez. Hemorragia del postparto. Principales etiologías, su prevención, diagnóstico y tratamiento. REV. MED. CLIN. CONDES - 2014; 25(6) 993-1003] (View)
Franklin J. Espitia de la Hoz, Oscar E. Zuluaga Cortés, Lilian Orozco Santiago. Ligadura de arterias hipogástricas en hemorragia postparto severa. CES Med. vol.30 no.1 Medellín Jan./June 2016 (View)
Hernández-Morales MA, García-de la Torre JI. Factores de riesgo de hemorragia obstétrica. Ginecol Obstet Mex. 2016 dic;84(12):757-764 (View)
Recomendaciones de la OMS para la prevención y el tratamiento de la hemorragia posparto. ISBN 978 92 4 354850 0 (View)
Texto de capacitación Materno-Infantil. Hemorragia Postparto IV. Ministerio de Salud (View)
FAQs from users: 'What do the 4Ts of postpartum haemorrhage refer to?' and 'Can postpartum haemorrhage be prevented?'.
Author
Find the latest news on assisted reproduction in our channels.