A savior sibling or savior baby is a child that has been conceived using Assisted Reproductive Technology (ART) in order to be genetically compatible with an older sibling that is affected by a fatal disease. The savior sibling will provide his older sibling with an organ transplant to save his or her life.
The concept of savior siblings has been the subject of intense ethical and scientific debate. While a great number of associations fight agains fatal diseases like beta thalassemia or Fanconi anemia are in favor of savior siblings, the Catholic church and pro-life groups are against allowing parents to use savior siblings.
Provided below is an index with the 9 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 3.
- 4.
- 5.
- 5.1.
- 5.2.
- 6.
- 7.
- 8.
- 9.
Usage of savior siblings
The creation of a savior sibling is a valid option available for parents when an older sibling is affected with a fatal disease, either congenital or acquired, and requires a hematopoietic stem cell (HSCs) transplantation.
In the case of congenital diseases (the baby is born ill), the most common ones are those due to mutations in a single gene and are inherited from one of the parents:
- Beta thalassemia
- Fanconi anemia
- Diamond-Blackfan anemia
On the other hand, a savior sibling can be created to treat a case of leucemia as well. In these cases, given that leucemia is not a genetic disease, the only requirement for the siblings is to be compatible so that the transplant is successful, without risk of rejection.
Depending on each particular case, it may be treated using cord blood right after the birth of the savior sibling. In case this option was not possible, a standard bone marrow transplantation would be required.
How are savior siblings created?
The assisted reproduction technique used to create savior siblings is called Preimplantation Genetic Diagnosis (PGD). Particularly, it is a type of PGD with human leukocyte antigen (HLA) typing.
This technique is used for two purposes:
- Having a healthy child, that is, free from a hereditary genetic disease that affects his older brother or sister.
- Having a child that is histocompatible with the older child that is affected with a fatal disease.
To this end, intended parents have to undergo an In Vitro Fertilization (IVF) cycle firstly. Once the embryos are created in the lab, they will be examined genetically by means of PGD with HLA typing. Finally, healthy embryos that are compatible with the affected sibling will be transferred to the intended mother's womb.
As explained above, in the case of leucemia, the purpose is that the savior baby has the HLA of his older brother or sister. Conversely, in cases of monogenetic disorders, the savior sibling must be free from this disorder as well.
What is HLA typing?
Human leukocyte antigens (HLAs) are proteins that can be found on the surface of almost all cells in the human body, especially on the surface of white blood cells.
The function of HLAs is to serve as recognition molecules in the initiation of an immune response, that is, it allows cells from the immune system to differentiate between own tissues and external substances.
It was after the discovery of the HLA system in the 70s when the procedures for cell, tissue and organ transplantation were improved, thereby reducing the rejection rates to a large extent.
HLA typing is a form of genetic analysis used to study the particular HLAs of each individual person or embryo likely to be transferred in order to become a savior sibling.
Success rates
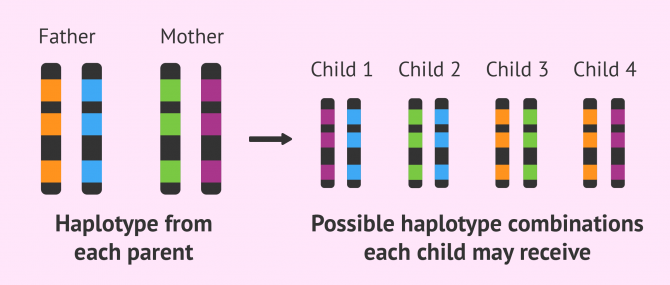
Children inherit their HLA system from their parents in the form of haplotypes (group of genes), one from the mother, and one from the father. Each parent can provide two possible types of haplotypes to their offspring, which can result in 4 possible combinations that will give rise to a new HLA system.
The importance of this type of inheritance is that both siblings can share both haplotypes, which would make them compatible for a transplant: in 50% of the cases, siblings will share one haplotype; in 25%, they will share none; and the remaining 25% will have both haplotypes equal.
Moreover, the analysis of haplotypes HLA must be combined with the study of a genetic disease that is present in the family, if any.
If the genetic disease present is a recessive one, the chances of finding a normal embryo using PGD are 75%, a percentage that decreases dramatically if we combine both analyses.
In short, the likelihood of finding a healthy embryo that is compatible when there is a hereditary genetic disease is 19% approximately.
Given that it is a technically challenging process, the quality of the IVF with PGD cycle should be an optimal one in each step of the process—including ovarian stimulation, fertilization rate, blastomere biopsy, PGD, and pregnancy rate—in order to increase the overall success rates.
Considering undergoing a fertility treatment? By getting your individual Fertility Report your will see different clinics especially selected for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
Savior sibling cases
There have been many cases of babies created to be savior siblings in the history of reproductive medicine since the birth of Adam Nash back in August 29, 2000. Adam was the first genetically designed savior sibling via In Vitro Fertilization (IVF). He was created to save his sister Molly, who was born with Fanconi anemia.
In 2001, Shahana Hashmi knew that she was a carrier of the genetic mutation that causes beta thalassaemia. For this reason, she used PGD to conceive her first child in order to ensure that he or she would be born completely healthy, but unfortunately PGD was unsuccessful and her first son, Zain, was born with the condition.
Shahana and her husband, Raj, had four further children, but sadly none of them were a tissue match for Zain. The Hashmis decided to apply to the HFEA for permission to use PGD to select an embryo that would be finally free of the disease and be able to donate life-saving cord blood to older brother Zain. The Court of Appeal and the House of Lords finally ruled that it was an acceptable practice.
Also, in 2002, an Australian couple from Victoria was given permission to use IVF in order to screen an embryo to create a savior sibling for their old daughter Christina, who was affected with Fanconi anemia as well.
Jamie Whitaker was born in 2004 at the Royal Hallamshire Hospital to save his older brother Charlie, aged 4, who has affected with Diamond-Blackfan anemia. Their parents sought permission for the procedure in the UK, but it was denied by the HFEA. They then went to the United States in order to provide a match for Charlie.
Ethical issues
The concept of savior sibling is surrounded by many ethical concerns and questions that have created arguments for and against. The main question here is whether the benefit to the sick child of having a savior sibling outweighs the potential harm done to the savior sibling. In this sense, there are many potential issues that could arise in the future, including that the savior child may feel neglected from his/her family.
Those against savior siblings would argue that the pain to the savior sibling is too much, as hospital treatment is required and it will somehow affect his or her health, which can cause them not to live a "normal life" in the future. Conversely, those who support savior siblings would argue that saving the life of a brother or sister justifies the harm in all cases.
The following is a quote by savior sibling Jamie Whitaker supporting savior siblings:
I know I was born to do that instead of being just born for me. It makes me feel closer to Charlie (Daily Mail).
There are many psychological issues involved in the idea of savior siblings. Some would argue that parents tend to view the savior child as a medical device to make the sick child better, and for this reason they will focus more of their attention on that one child. Others would however argue that being a savior sibling is actually beneficial for him/her, as they will have a sense of pride that he/she was able to save someone's life by simply existing.
Also, it has been argued that creating savior siblings may jeopardize the autonomy of the parents, as they may decide to have further children to save a sick son or daughter when this was not their intention at first. Autonomy of the children may be affected as well. Some detractors consider that the future child's autonomy is violated when her or she is born to be a savior sibling.
For some, the idea of savior siblings is different to a normal birth, as they are born for a purpose as soon as they enter the world. This could be harmful for the savior baby, as his/her future has been planned out for him/her.
Finally, another ethical concern that is considered affected with the idea of savior siblings is nonmaleficence, that is, the idea of doing no harm to others. The main ethical questions that arises here is: Are parents inflicting harm upon the savior sibling? Indeed, parents should consider whether the harm being done to the savior child justifies or exceeds the benefit that the sick child will receive.
FAQs from users
How many savior siblings are born each year?
There is no official statistical data as regards the number of savior babies that are born each year. However, it is estimated that up to 1 percent of PGD in the United States is used to create embryos that are tissue matches for their siblings.
Is the creation of savior siblings a practice regulated by law?
It varies by country. For example, in the UK, the HFEA has ruled that it is lawful to use modern reproductive technologies to create savior babies. In Australia, the Infertility Treatment Authority reviews applications for the use of PGD with HLA typing on a case-by-case basis.
Suggested for you
Preimplantation Genetic Diagnosis (PGD) is a technique used to screen embryos genetically, hence that it is used to create savior siblings, as we have explained throughout this post. Get more info by clicking the following link: What Is PGD or Preimplantation Genetic Diagnosis?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.