MACS is a technique that allows the separation of healthy spermatozoa from spermatozoa that will soon die due to apoptosis. This technique is based on the application of magnetic fields, from which it gets its name (Magnetic Activated Cell Sorting), and on the use of annexin V.
This type of spermatozoa selection cannot be done with traditional methods, as apparently these spermatozoa that have started the apoptotic process do not differ from healthy spermatozoa. Therefore, the aim of the MACS technique is to perform a better sperm selection, discarding apoptotic spermatozoa that will probably not give rise to a viable embryo and pregnancy.
In this way, the MACS technique ultimately aims to increase the probability of obtaining a pregnancy and thus improve the results of assisted reproduction techniques.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 4.7.
- 5.
- 6.
- 7.
- 8.
Methods of sperm selection and fertility
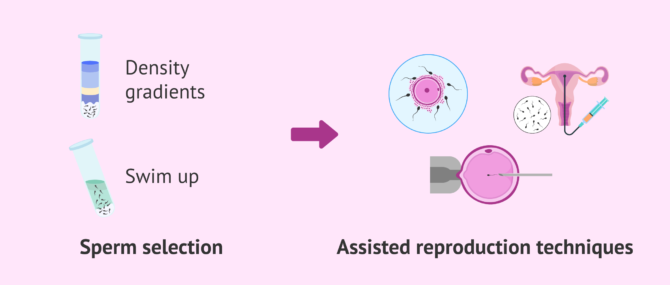
Before using any semen sample during a fertility treatment, the semen quality is analyzed by means of a semen analysis, and a sperm selection is carried out to rule out spermatozoa possessing the worst quality.
The most common methods are density gradients and swim-up and both are based primarily on choosing the best motile sperm for treatment.
However, the fact that a spermatozoon has good motility is not always an indication that it is capable of correctly fertilizing the egg. In some cases, there are genetic alterations that do not alter motility but can affect both fertilization and subsequent embryonic development.
Therefore, even if the result of the seminogram is good and the processed sample also shows adequate concentration and motility, some of the spermatozoa selected by traditional methods may not be of as good quality as expected.
For all these reasons, in recent years efforts are being made to find new methods of sperm selection that will allow sperm to be separated more precisely. In doing so, the aim is to improve the results of assisted reproduction techniques.
Assisted procreation, as any other medical treatment, requires that you rely on the professionalism of the doctors and staff of the clinic you choose. Obviously, each clinic is different. Get now your Fertility Report, which will select several clinics for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
What is the MACS technique?
The MACS sperm selection technique is used to separate spermatozoa that are entering apoptosis from healthy spermatozoa. Therefore, to understand this method, we must first be clear about apoptosis, which is programmed cell death.
Apoptosis
Apoptosis is our body's mechanism for getting rid of damaged or defective cells. This ensures that these cells will not compromise the function of healthy cells in our body.
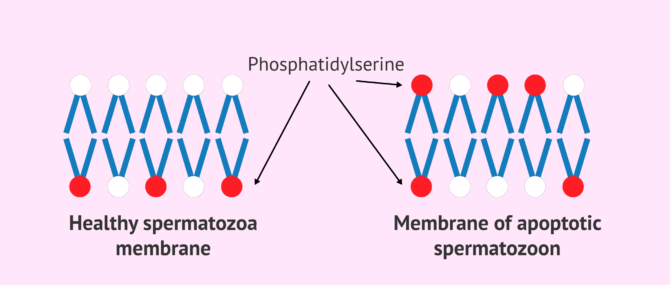
In order to carry out this process of apoptosis, the cells must undergo a series of changes, as it must be perfectly regulated. One of these changes is the externalisation of some molecules to the surface.
Phosphatidylserine is one such molecule, a phospholipid that healthy spermatozoa possess inside their membrane. This marker is externalised in the early stages of apoptosis, before sperm motility is affected. Therefore, by analysing this molecule, we can detect which sperm will die earlier than with conventional sperm selection methods. This will avoid fertilising the egg with a sperm that was already destined to die.
Annexin V columns
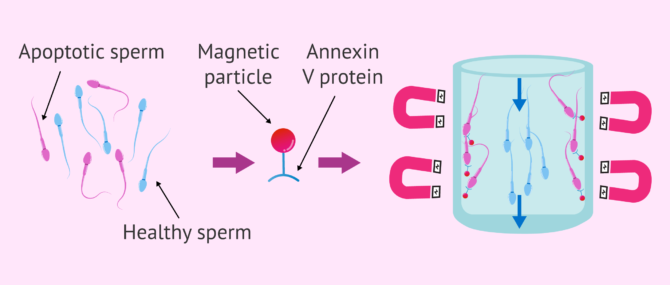
To detect phosphatidylserine, we have annexin V. This is a protein that specifically and with high affinity recognises the phosphatidylserine that has been externalised by these apoptotic spermatozoa. Thanks to this characteristic, by attaching annexin V to magnetic microspheres, we can separate spermatozoa that have entered apoptosis using a magnet.
The rationale for the magnetic selection of spermatozoa with annexin V consists of:
- Add annexin V bound to magnetic beads to the semen sample. Annexin V will bind to phosphatidylserine from those apoptotic sperm that have externalised it.
- Introduce the semen sample through a small column attached to a magnet. Apoptotic spermatozoa bound to annexin V will be retained in the magnetised column. This is because, as explained above, annexin V is in turn bound to the magnetic microspheres.
In this way, sperm that have not been trapped in the spine (and are therefore not apoptotic) will eventually be used for assisted reproductive techniques.
Advantages and disadvantages
The main benefit of this technique is that it allows for the discarding of apoptotic spermatozoa, which may not be detected by conventional sperm selection methods. Therefore, it is possible to separate the best quality spermatozoa at an early stage.
Several studies have confirmed that thanks to the MACS technique with annexin V, pregnancy rates improved.
However, it should be kept in mind that when annexin columns are used, the concentration of the sperm sample decreases considerably, since only healthy sperm will be present in the final sample. This means that the sample resulting from this procedure, in most cases, can only be used for ICSI, as the concentration is insufficient to perform artificial insemination or conventional in vitro fertilization (IVF).
Another disadvantage of this technique is that it is more expensive and laborious than traditional methods. Therefore, it is only recommended to use it in patients where it is indicated.
In which patients is MACS used?
The couples that can benefit most from this method of sperm selection are those in which the cause of sterility is the male factor or inexplained infertility. This technique is indicated in the following cases:
- High percentage of sperm with fragmented DNA.
- Recurrent failures in previous treatments, such as recurrent miscarriages with unknown cause.
- Low fertilization rate.
- Poor embryo quality.
- Sterility of unknown origin.
- Patients who underwent chemotherapy and/or radiotherapy.
In addition, the MACS technique could also be used for repeat miscarriages where the cause is unknown.
FAQs from users
From how many failed cycles is it recommended to use the MACS technique?
MACS should be used whenever a higher than normal level of apoptosis is detected in a semen sample, in order to avoid cell-damaged sperm. Therefore, it is indicated in cases of: severe male factor, implantation failure (usually we talk about two transfers with high quality embryos, which have not generated pregnancy) and those previous IVF cycles in which fertilization or embryo development has not been as expected, despite the fact that the semen sample was normal or almost normal.
Read more
What percentage of sperm selection using adnexin V columns increases the probability of successful treatment?
The selection of spermatozoa using adnexin columns substantially improves the chances of success in those cases where it is indicated.
The percentage of improvement will depend on the percentage of spermatozoa with fragmented DNA in the seminal sample, since this will allow us to select healthy spermatozoa, thus increasing the possibility of having good quality embryos.
Can MACS be performed with sperm obtained through testicular biopsy?
No, because the sperm obtained by this technique are scarce. Therefore, when they are passed through the columns of adnexin V, it is very likely that there will not be enough to carry out the treatment.
Is a minimum semen volume required to make MACs?
The most important thing to perform a MACs technique is the sperm concentration, as well as the fluidity of the semen sample.
Read more
When is MACS recommended?
The MACS technique can be used in any situation, but is particularly recommended in the following cases:
- DNA with a high fragmentation rate.
- Previous IVF cycles characterised by low fertilisation rate or poor embryo quality, despite good egg quality.
- Severe seminal infertility.
- Patients undergoing radiotherapy or chemotherapy.
- Repeated miscarriages with no other identified cause.

Are Annex V columns an alternative to density gradients?
No, the most advisable thing is to pass the sample through density gradients to eliminate spermatozoa with poor mobility and to make the sample cleaner. In this way, it is easier to make the subsequent magnetic selection more efficient.
Can sex be selected using this technique?
No. This technique is based on a marker that is in the sperm cell membrane. To date, there is no known external marker that allows us to separate the sperm with the X sex chromosome (fetus will be XX, female) from those with the Y sex chromosome (fetus will be XY, male).
Suggested for you
As we have seen, patients with a DNA fragmentation index can benefit from the use of this new technique. You can find more information about this disorder in the following article: What is sperm DNA fragmentation?
In addition to the MACS technique, there are also other new sperm selection methods, such as IMSI and PICSI. IMSI (Intracytoplasmic Morphologically Selected Sperm Injection) consists of choosing the sperm to be used in ICSI using a more powerful microscope that allows a better visualization of the morphology. If you want to delve deeper into this topic, we recommend you to visit this article: What is IMSI?
On the other hand, PICSI (physiological ICSI) consists of selecting the spermatozoa that would be capable of fertilizing the egg under physiological conditions, i.e. in the mother's body. In the following article, you can read more about this technique: What is PICSI?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Gil M, Sar-Shalom V, Melendez Sivira Y, Carreras R, Checa MA. Sperm selection using magnetic activated cell sorting (MACS) in assisted reproduction: a systematic review and meta-analysis. J Assist Reprod Genet. 2013 Apr;30(4):479-85 (View)
Lee TH, Liu CH, Shih YT, Tsao HM, Huang CC, Chen HH, Lee MS. Magnetic-activated cell sorting for sperm preparation reduces spermatozoa with apoptotic markers and improves the acrosome reaction in couples with unexplained infertility. Hum Reprod. 2010 Apr;25(4):839-46 (View)
Lepine S, McDowell S, Searle LM, Kroon B, Glujovsky D, Yazdani A. Advanced sperm selection techniques for assisted reproduction. Cochrane Database Syst Rev. 2019 Jul 30;7(7):CD010461 (View)
Makker K, Agarwal A, Sharma RK. Magnetic activated cell sorting (MACS): utility in assisted reproduction. Indian J Exp Biol. 2008 Jul;46(7):491-7.
Oseguera-López I, Ruiz-Díaz S, Ramos-Ibeas P, Pérez-Cerezales S. Novel Techniques of Sperm Selection for Improving IVF and ICSI Outcomes. Front Cell Dev Biol. 2019 Nov 29;7:298 (View)
Paasch U, Grunewald S, Glander HJ. Sperm selection in assisted reproductive techniques. Soc Reprod Fertil Suppl. 2007;65:515-25.
Pacheco A, Blanco A, Bronet F, Cruz M, García-Fernández J, García-Velasco JA. Magnetic-Activated Cell Sorting (MACS): A Useful Sperm-Selection Technique in Cases of High Levels of Sperm DNA Fragmentation. J Clin Med. 2020 Dec 8;9(12):3976 (View)
Pedrosa ML, Furtado MH, Ferreira MCF, Carneiro MM. Sperm selection in IVF: the long and winding road from bench to bedside. JBRA Assist Reprod. 2020 Jul 14;24(3):332-339 (View)
Romany L, Garrido N, Cobo A, Aparicio-Ruiz B, Serra V, Meseguer M. Obstetric and perinatal outcome of babies born from sperm selected by MACS from a randomized controlled trial. J Assist Reprod Genet. 2017 Feb;34(2):201-207 (View)
Sánchez-Martín P, Dorado-Silva M, Sánchez-Martín F, González Martínez M, Johnston SD, Gosálvez J. Magnetic cell sorting of semen containing spermatozoa with high DNA fragmentation in ICSI cycles decreases miscarriage rate. Reprod Biomed Online. 2017 May;34(5):506-512 (View)
Ziarati N, Tavalaee M, Bahadorani M, Nasr Esfahani MH. Clinical outcomes of magnetic activated sperm sorting in infertile men candidate for ICSI. Hum Fertil (Camb). 2019 Jun;22(2):118-125 (View)
FAQs from users: 'From how many failed cycles is it recommended to use the MACS technique?', 'What percentage of sperm selection using adnexin V columns increases the probability of successful treatment?', 'Can MACS be performed with sperm obtained through testicular biopsy?', 'Is a minimum semen volume required to make MACs?', 'When is MACS recommended?', 'Are Annex V columns an alternative to density gradients?' and 'Can sex be selected using this technique?'.
Authors and contributors