Throughout gestation, the woman has the possibility of performing some prenatal diagnostic tests to make sure that the baby on the way is healthy and does not suffer any genetic alteration or congenital malformation.
These prenatal studies differ basically in two types:
- Non-invasive tests
- are very simple to do and do not pose any risk to the mother or fetus.
- Invasive tests
- involve making a puncture to reach the gestational sac and taking a sample. Therefore, there is a risk of pregnancy loss.
Which method you chose depends on your and your partner’s medical history, your age, and the possible risks to the baby.
Provided below is an index with the 7 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 2.
- 2.1.
- 2.2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 3.5.
- 4.
- 5.
- 6.
- 7.
Non-invasive prenatal test
They are tests that help establish the risk of chromosomal alterations in the fetus without entering the uterine cavity, so they do not pose a risk of miscarriage or infection.
Another advantage of non-invasive tests is that they are performed during the first trimester. Therefore, in case of a bad result, the woman has a margin of time to decide whether to continue with the pregnancy or to make a voluntary pregnancy interruption.
Currently, there are two main types of noninvasive prenatal genetic diagnosis tests:
Analysis of cell-free DNA in maternal blood
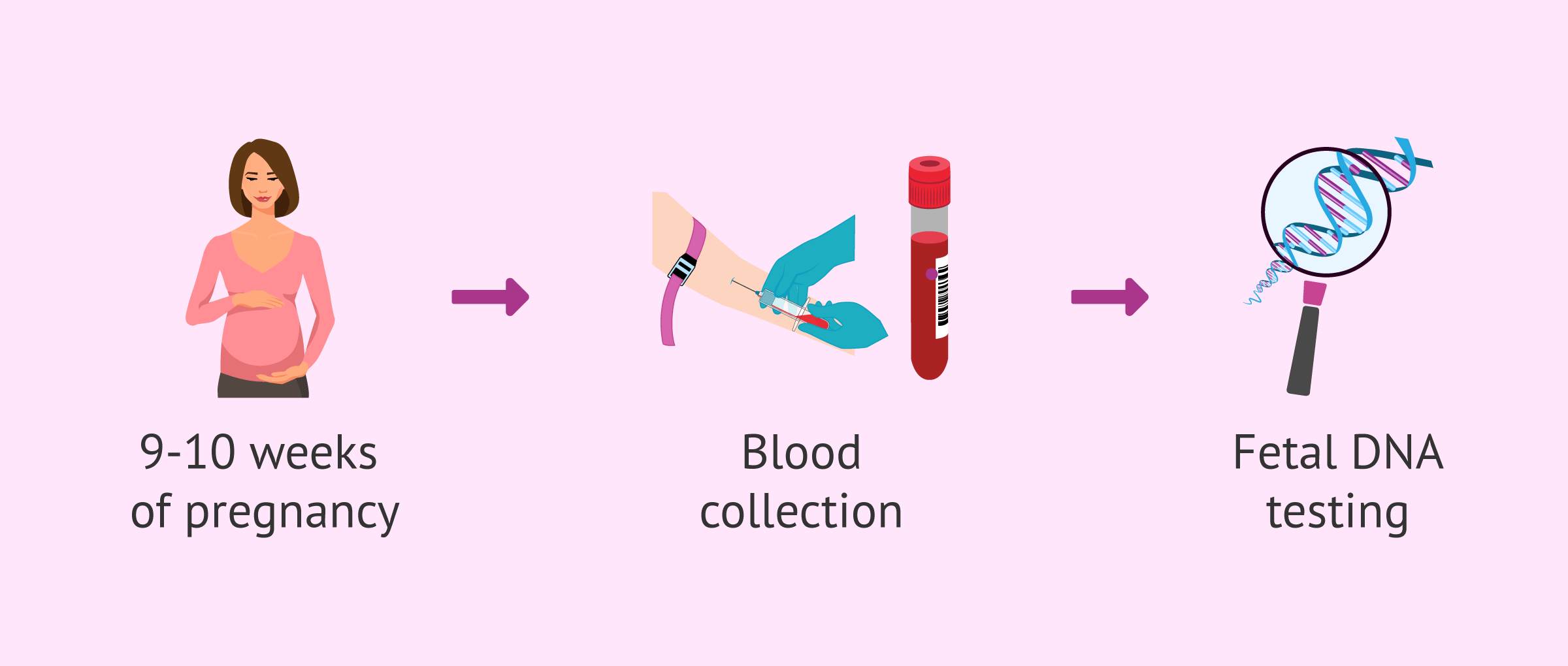
This is a test that can be performed from the 9th or 10th week of pregnancy onwards, when it is possible to detect DNA from the fetus in the mother's blood.
To perform a fetal DNA test in maternal blood only requires the collection of a blood sample and its analysis.
Although the diagnostic capacity of this test is limited, it does detect the most frequent genetic anomalies in the population:
- Down syndrome (trisomy 21)
- Edwards syndrome (trisomy 18)
- Patau syndrome (trisomy 13)
- Aneuploidy on sex chromosomes: Turner syndrome (monosomies X0), Klinefelter syndrome (trisomy XXY), etc.
Besides, there is a type of advanced non-invasive prenatal test that can also identify some specific mutations that cause pathologies such as DiGeorge syndrome, Angelman syndrome or cri-du-chat syndrome, among others.
The high detection rate of this test, its safety and the speed at which the results are obtained mean that more and more people are deciding to carry it out. However, it has the disadvantage of being expensive.
First Trimester Screening
This prenatal test, also known as triple screening, consists of linking a series of ultrasound and biochemical markers to obtain as a result a probability of risk that the fetus has some chromosomal alteration.
For the test to be carried out, the following tests and data collection are needed around the 11th or 12th week of pregnancy:
- First trimester ultrasound
- Nuchal translucency measurement
- Blood tests
- determination of free PAPP-A and beta-hCG markers.
- Other parameters
- mother's age, weight, number of fetuses, weeks of pregnancy, etc.
Triple screening is not a diagnostic technique as such, but rather an estimate of the risk of genetic disease to the fetus. Therefore, this test has a high degree of error and, in the event of a high risk result, this should always be confirmed by amniocentesis or chorionic biopsy.
Despite this, combined first-trimester screening continues to be routinely performed as a control test in almost all pregnancies.
Invasive prenatal tests
Invasive prenatal diagnostic techniques directly analyze fetal cells obtained through a vaginal or abdominal puncture to access the amniotic cavity.
This implies a small risk of fetal damage or gestational loss, although today it is less than 1%. For this reason, specialists recommend invasive tests only if you have obtained a poor result in the triple screening or fetal DNA test. They are also advisable in cases of advanced maternal age or a history of genetic diseases.
The advantage of invasive prenatal testing is that it is conclusive and allows a reliable diagnosis of the following birth defects:
- Chromosomal abnormalities
- Hereditary genetic diseases
- Fetal malformations
- Infections
Below, we are going to describe the two types of invasive prenatal testing most commonly used today, although there are others as well.
Chorionic villus sampling
A chorionic biopsy or chorionic biopsy consists of obtaining cells from the placenta in order to analyze them and detect possible abnormalities in the fetus.
The sample may be taken transcervically or transabdominally and should be taken between the 10th and 14th week of pregnancy.
With chorionic villus sampling it is possible to rule out more than 200 pathologies in the fetus and, in addition, the results are obtained earlier than in amniocentesis.
Amniocentesis
This well-known diagnostic test consists of obtaining a sample of amniotic fluid through a transabdominal puncture and analyzing the fetal cells suspended in it.
Amniocentesis is usually done between the 15th and 20th week of pregnancy since there is not enough amniotic fluid to perform it before.
Once the amniotic fluid sample has been obtained, there are several techniques for analyzing it and obtaining results:
- Study of the prenatal karyotype
- analyzes all 23 pairs of chromosomes, including the pair of sex chromosomes. The result takes about 4 weeks.
- QF-PCR
- is a molecular technique that allows the analysis of chromosomes 13, 18, 21, X and Y, whose alteration causes more than 90% of the aneuploidies. The result is obtained in 2 days.
- Array CGH prenatal
- allows the detection of genetic and chromosomal alterations responsible for 124 genetic syndromes with a resolution 10 times higher than that of the conventional karyotype. It is fast, reliable and does not require cell culture. The result is obtained in 5 days.
You can continue reading and learn more about this topic in the following article: Amniocentesis: Why it is done and what are the possible risks?
FAQs from users
What type of prenatal diagnostic is recommended for a woman who has become pregnant through IVF?
Normally, pregnancy follow-up after IVF is exactly the same as a spontaneous pregnancy, but it must be kept in mind that many of the women who undergo assisted reproduction treatments are over 35 and even 40 years old. In other words, the risks derived from chromosomal alterations will be increased. Nowadays, thanks to prenatal blood diagnosis techniques in the first weeks of pregnancy, we can detect chromosomal alterations even before performing the first trimester ultrasound. We will recommend this type of analysis to older women who have achieved pregnancy with their own eggs.
Which prenatal diagnostic test is best suited to detect Down syndrome?
Which prenatal diagnostic test is best suited to detect Down syndrome?
The simplest test that poses no risk to the mother or the fetus is the maternal blood fetal DNA test. This test is very accurate in detecting the trisomy of chromosome 21, which is responsible for Down syndrome.
However, the cost of the test is around 500-600€, so if there is no high risk of chromosomal anomalies, future parents usually only do the combined screening of the first trimester.
Finally, invasive prenatal diagnostic tests also detect pathologies such as Down syndrome with very high reliability.
What happens if I get bad results with a chorionic biopsy?
If the chorionic villus analysis shows that the fetus is affected by some genetic malformation or abnormality, the woman or couple will have to decide whether to continue the pregnancy or perform a therapeutic abortion.
Depending on each case, the doctor may recommend amniocentesis at a later date to confirm the result.
However, it should be borne in mind that voluntary termination of pregnancy will be easier when it is done earlier.
How are genetic diseases detected in a fetus?
Women who are already pregnant and are at risk of transmitting a genetic disease to offspring, can find out whether the fetus has inherited it or not with an amnio test or chorion biopsy.
Once the result is ready, if it confirms that the fetus has a genetic disease, the woman or couple will have to decide whether they wish to continue with the pregnancy ir terminate it.
What is prenatal diagnosis?
Prenatal diagnosis is a set of tests that provide information about possible abnormalities in the fetus during gestation. There are different types of tests, some invasive and others non-invasive. Depending on the week of pregnancy and the situation of each woman, the specialist will choose one prenatal test or another.
Suggested for you
If you want to know all the prenatal tests that are performed month by month throughout pregnancy, we recommend you read the following post: Prenatal pregnancy control.
On the other hand, if you are interested in knowing what preimplantation diagnosis of embryos is, you can access the following article: What is PGD?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Control prenatal del embarazo normal. PROTOCOLOS SEGO. Progresos de Obstetricia y Ginecología 2011;54(6): 330-349 (View)
Badenas C, Rodríguez-Revenga L, Morales C, Mediano C, Plaja A, Pérez-Iribarne MM, Soler A, Clusellas N, Borrell A, Sánchez MÁ, Miró E, Sánchez A, Milà M, Jiménez W. Assessment of QF-PCR as the first approach in prenatal diagnosis. J Mol Diagn. 2010 Nov;12(6):828-34 (View)
Beaudet AL. Using fetal cells for prenatal diagnosis: History and recent progress. Am J Med Genet C Semin Med Genet. 2016 Jun;172(2):123-7 (View)
Cheng WL, Hsiao CH, Tseng HW, Lee TP. Noninvasive prenatal diagnosis. Taiwan J Obstet Gynecol. 2015 Aug;54(4):343-9 (View)
de Jong A, Maya I, van Lith JM. Prenatal screening: current practice, new developments, ethical challenges. Bioethics. 2015 Jan;29(1):1-8 (View)
FAQs from users: 'What type of prenatal diagnostic is recommended for a woman who has become pregnant through IVF?', 'Which prenatal diagnostic test is best suited to detect Down syndrome?', 'What happens if I get bad results with a chorionic biopsy?', 'How are genetic diseases detected in a fetus?' and 'What is prenatal diagnosis?'.