The menstrual cycle is a period of approximately 28 days in which a woman experiences changes in her body, especially in the uterus and ovaries of her reproductive system, by the action of female sex hormones.
All of these changes are aimed at preparing women for a possible pregnancy, from the beginning of their reproductive stage with the first menstruation until menopause.
The length of the cycle can vary between 23 and 35 days depending on the woman, as some have shorter or longer cycles. However, the stages of the menstrual cycle that we are going to discuss are the same in all cases.
Provided below is an index with the 7 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 2.4.
- 2.5.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 3.5.
- 4.
- 5.
- 6.
- 7.
Female hormones
In order to understand how the menstrual cycle works, it is first necessary to know the female sex hormones, as they are responsible for regulating this entire process.
A woman's sex hormones are produced in her pituitary gland (FSH and LH) and in her ovaries (estrogen and progesterone). In the following section we are going to to comment on each of them:
- FSH
- follicle-stimulating hormone. It begins to secrete at the beginning of the sexual cycle and its function is to stimulate the ovary so that the primordial follicles develop. Follicles are fluid-filled structures that contain eggs at different stages of maturation.
- LH
- luteinizing hormone. It is responsible for triggering ovulation once the follicle containing the egg has fully matured.
- Estrogen
- are hormones secreted by the ovary as follicles develop. They have a regulating function of the entire menstrual cycle, in addition to intervening in the sexual development of women.
- Progesterone
- is secreted by the ovary after ovulation. Its main function is to increase the endometrial thickness so that the embryo can implant and pregnancy takes place.
If you are interested in knowing the normal values of these hormones, we recommend reading the following article: Female hormone analysis: what should normal hormone levels be?
Phases of the menstrual cycle.
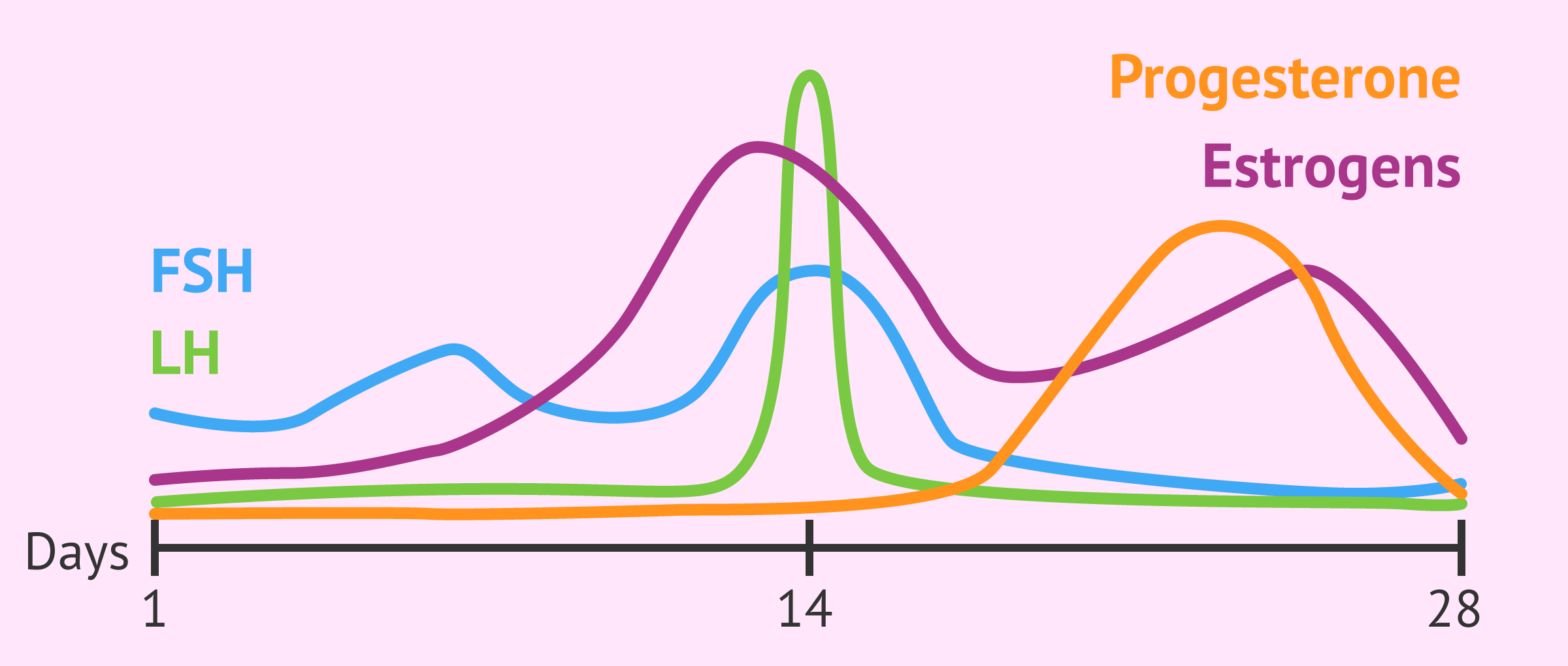
At the beginning of the menstrual cycle, the sex hormones are in basal state, i.e. with a minimal concentration, as they have not yet begun to be produced.
From now on, it will be possible to differentiate between several stages within the menstrual cycle depending on hormone levels and the process that occurs.
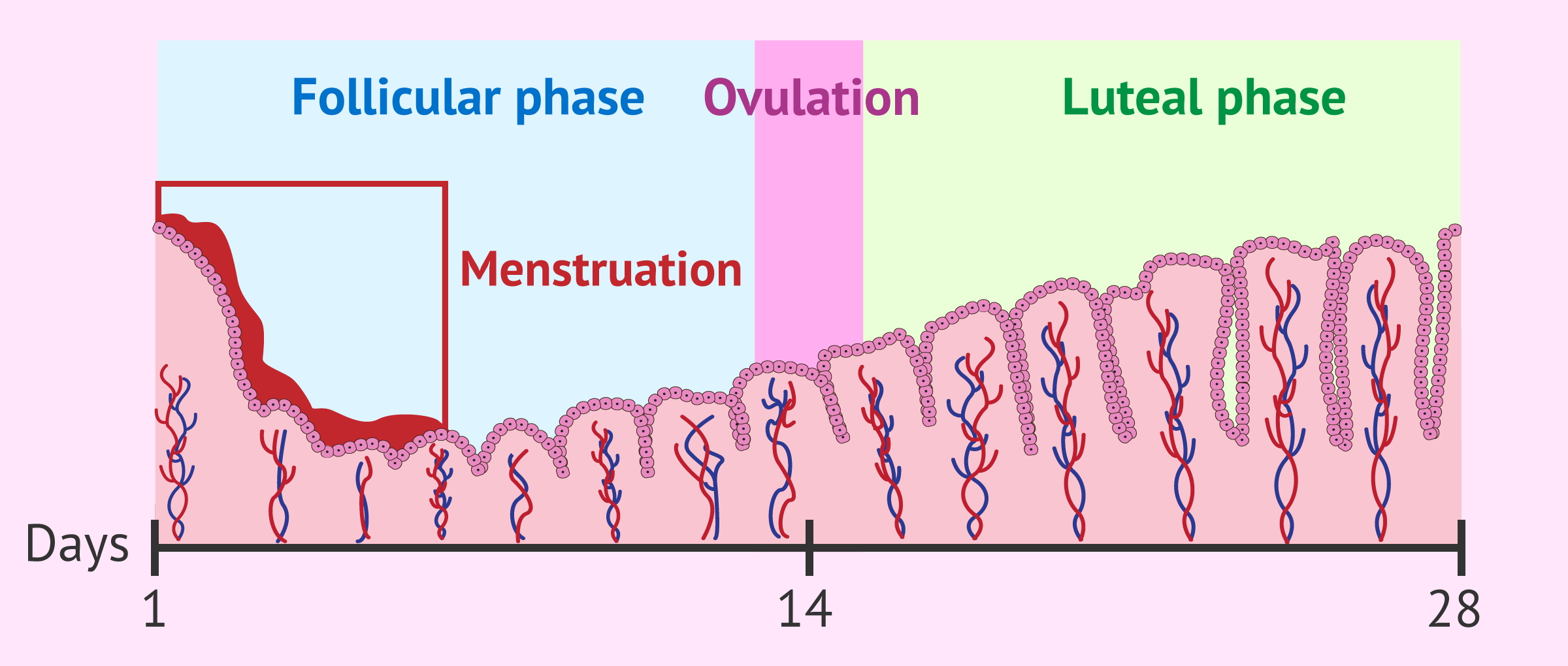
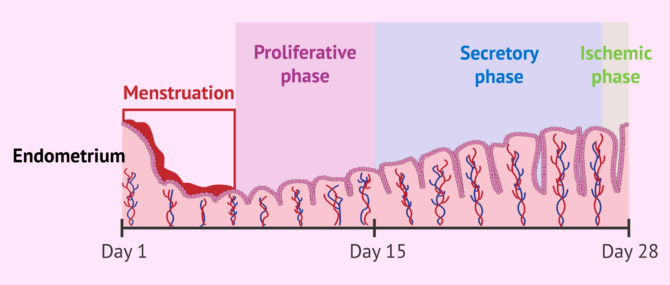
Menstruation
The menstrual cycle begins with the beginnung of the menstruation. The menstruational bleeding is attributed to the shedding of the uterine lining when the ovulated egg is not fertilized.
The endometrium is the innermost layer of the uterus, which is renewed in each menstrual cycle in order to accommodate the embryo during pregnancy.
If you want to know more about this topic, we recommend you read the following post: What is the Role of the Endometrium?
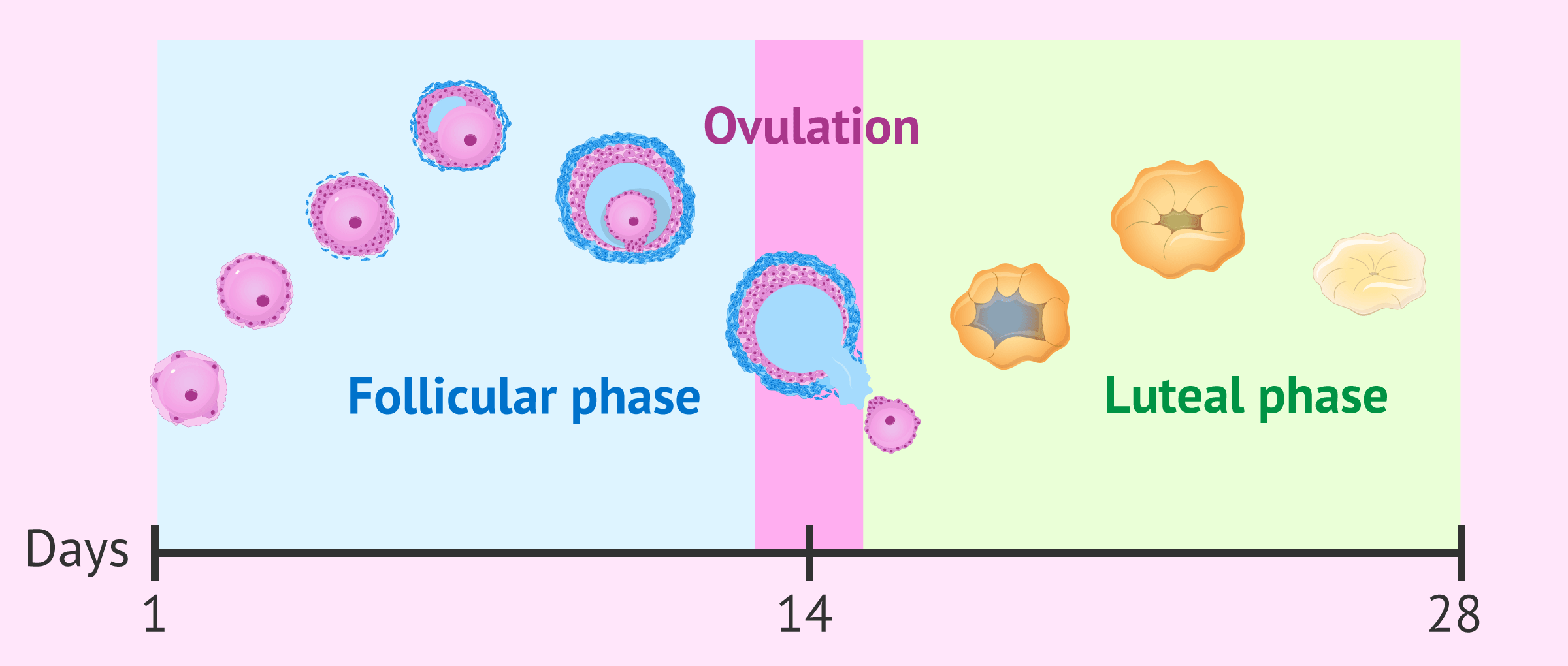
Follicular Phase
The follicular phase, also known as the proliferative or preovulatory phase, consists of a process of growth of the ovarian follicles from the beginning of menstruation until ovulation.
When a woman reaches puberty, she has an ovarian reserve of about 500,000 primary follicles in her ovaries. They remain dormant, waiting to be selected to develop in each menstrual cycle.
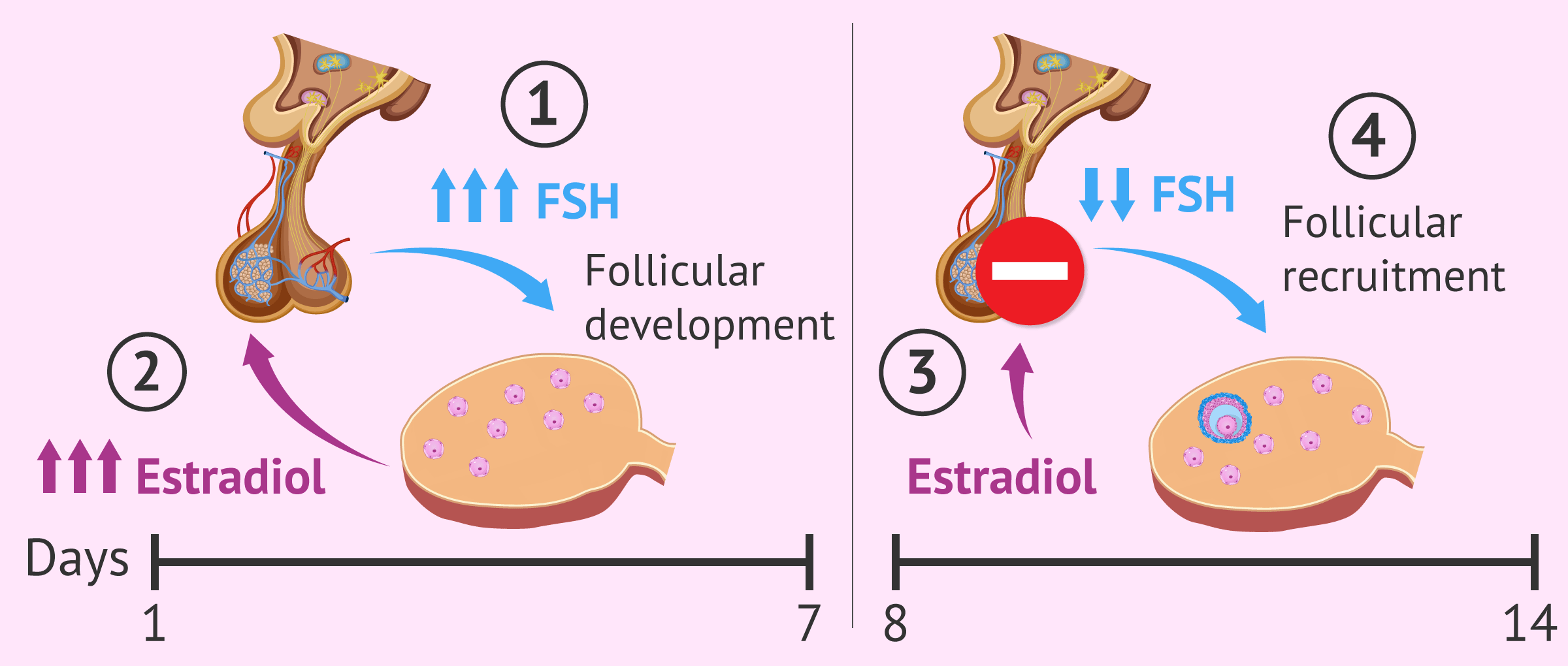
The increase in FSH causes several of these follicles to begin to grow and migrate towards the surface of the ovary, constituting a follicular cohort.
The development of the follicular cohort causes the synthesis and secretion of estradiol, whose regulatory function is to block the production of FSH by the pituitary gland.
The consequence of this is follicular recruitment: as the FSH level decreases, the ovarian follicles are not able to survive and to continue their development. Only one of them will fully mature and become a final preovulatory follicle.
This dominant follicle is called the Graafian follicle which measures about 18 mm before ovulation. The rest of the follicles will be blocked and degenerate.
Moreover, estrogens produced during this proliferative phase also contribute to the emergence of more aqueous and elastic cervical mucus, which favors the entry of sperm. The estrogens also act on the endometrium, favoring its thickening.
Ovulation phase
Around day 14 of the menstrual cycle, the pituitary gland produces a rise in LH levels, known as LH peakand causes ovulation.
Ovulation is the process by which the Graafian follicle ruptures and the mature egg inside it is released into the fallopian tube.
The fertile days are those close to ovulation, that is, they are located towards the middle of the menstrual cycle. During this period, you are more likely to become pregnant if you have unprotected sex.
Usually, in each menstrual cycle, a single mature egg is expelled into one of the fallopian tubes. Occasionally, two follicles may ovulate, increasing the chance of having a twin pregnancy.
The egg that is now in the fallopian tube will remain waiting for a sperm that can fertilize it if there has been sexual intercourse. If this does not happen within 24 hours of ovulation, the egg will age and can no longer be fertilized.
To detect if ovulation has taken place when a couple is trying for pregnancy, there are tests that detect the peak of LH in the urine.
Luteal phase
The luteal phase, also called the secretory or post-ovulatory phase, is the phase that begins just after ovulation and lasts until the end of the menstrual cycle, i.e. until menstrual bleeding returns.
The ruptured follicle is transformed into a yellowish body called the yellow body or corpus luteum. This body is responsible for producing estrogen and progesterone, the two hormones that will act on the endometrium.
At this time, progesterone is now in charge of modifying the cervical mucus so that it becomes impenetrable again by the sperm.
Progesterone also acts on the endometrium, which becomes thicker and spongy as a result of increased blood supply. This makes the endometrium receptive for the embryo to implant.
If pregnancy occurs, the corpus luteum continues to produce estrogen and progesterone until the eighth week. From this moment on, the placenta will be in charge of continuing with its synthesis.
Ischemic phase and start of a new cycle
If the released egg is not fertilized by a sperm, the corpus luteum disappears. As a result, estrogen and progesterone production gradually decreases in what is known as the ischemic phase of the menstrual cycle.
The decrease in sex hormones causes the endometrium to flake off and be eliminated through the vagina, producing menstruation again.
The first day of menstrual bleeding already corresponds to the first day of the next menstrual cycle, because the sex hormones will increase again from this moment and they will start a new follicular proliferation.
FAQs from users
Is pregnancy with luteal phase insufficiency possible?
Antonio Forgiarini, gynaecologist at Next Fertility Valencia, explains in this video whether it is possible to achieve a pregnancy despite an insufficient luteal phase:
Yes it's possible, especially because we don't know if luteal insufficiency is a real problem or not, especially in natural cycle because they are very variable. Normally, when we suspect this problem we can add progesterone. Progesterone is the principal hormone during the lutal phase, so we can add it during the second phase of the menstrual cycle in a natural cycle or after a reproductive treatment we usually always add progesterone during the lutal phase.
What are the benefits of evening primrose oil?
Basically, evening primrose oil is an oil of vegetable origin obtained directly from this plant.
Evening primrose oil is rich in phytoestrogens, compounds similar to female hormones of vegetable origin, so it is used to improve symptoms of menopause, especially in mild cases.
In addition, it has been described that evening primrose oil can be useful for the treatment of premenstrual symptoms (feeling of swelling of the lower abdomen, headache, irritability ...)
Evening primrose oil has also been described as a long-term treatment that may be helpful in regulating the menstrual cycle.
As far as reproductive medicine is concerned, there is no evidence that this medicine improves a woman's state of fertility, except in the case of a patient who manages to regularise her previously anovulatory cycles with evening primrose oil.
What are the fases of the endometrial cylce?
Since the endometrium develops as a function of the hormones that act throughout the menstrual cycle, estrogen and progesterone, it also has two different phases:
- Proliferative endometrium: its thickness increases little by little thanks to the effect of estrogens.
- Secretory endometrium: it matures and becomes receptive thanks to progesterone secreted by the corpus luteum.
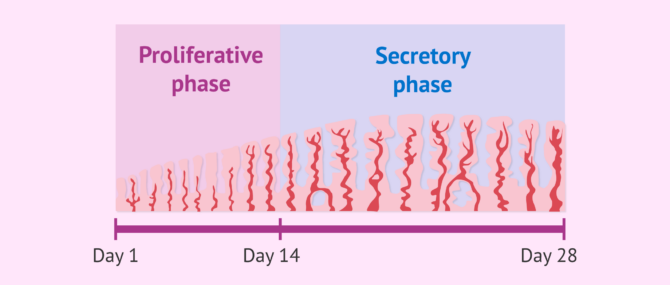
An ultrasound can be used to measure the endometrial thickness and find out what stage it is in.
What symptoms appear in the different phases of the menstrual cycle?
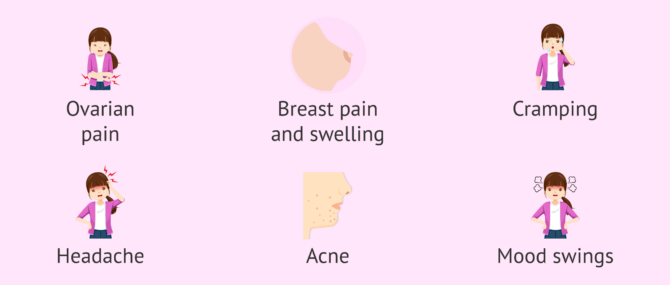
It is true that each phase of the menstrual cycle may have different symptoms that may be more or less evident depending on the woman. However, those symptoms that women suffer the most are the so-called premenstrual symptoms, which appear just before the beginning of their period and are maintained during their first days. These are discussed below:
- Ovarian and abdominal pain
- Swollen and painful breasts
- Colic
- Fluid retention
- Headache
- Acne
- Changes in mood
The ovulation phase may also result in minor discomfort such as very mild spotting and pain in the ovaries.
When can I get pregnant during the menstrual cycle?
The fertile days of the woman, that is to say, those in which the probability of pregnancy is much greater, are those that correspond to the ovulatory stage. Ovulation takes place at about the middle of the menstrual cycle, on days 13, 14, or 15, provided the woman has regular 28-day menstrual cycles.
Suggested for you
Women seeking pregnancy must keep track of their menstrual cycle in order to achieve their purpose. In the following article we explain what natural pregnancy is: How can I get pregnant naturally?
Similarly, those women who are not considering becoming mothers should also know their menstrual cycle and take steps to avoid pregnancy yet. We recommend read more about this in the following article: Contraceptive methods.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Baerwald A, Pierson R. Ovarian follicular waves during the menstrual cycle: physiologic insights into novel approaches for ovarian stimulation. Fertil Steril. 2020 Sep;114(3):443-457. doi: 10.1016/j.fertnstert.2020.07.008. PMID: 32912608. (View)
Bull JR, Rowland SP, Scherwitzl EB, Scherwitzl R, Danielsson KG, Harper J. Real-world menstrual cycle characteristics of more than 600,000 menstrual cycles. NPJ Digit Med. 2019 Aug 27;2:83. doi: 10.1038/s41746-019-0152-7. PMID: 31482137; PMCID: PMC6710244. (View)
Duncan WC. The inadequate corpus luteum. Reprod Fertil. 2021 Feb 26;2(1):C1-C7. doi: 10.1530/RAF-20-0044. PMID: 35128435; PMCID: PMC8812462. (View)
FAQs from users: 'Is pregnancy with luteal phase insufficiency possible?', 'What are the benefits of evening primrose oil?', 'What are the fases of the endometrial cylce?', 'What symptoms appear in the different phases of the menstrual cycle?' and 'When can I get pregnant during the menstrual cycle?'.
Authors and contributors
Find the latest news on assisted reproduction in our channels.