The sperm vitality test is a test performed during the seminogram in which the percentage of live and dead spermatozoa in a semen sample is calculated.
Although motility indicates vitality, not all immotile sperm are dead. The vitality index is not measured in all spermograms; only in those cases in which there are more than 40% of immotile spermatozoa.
The main reason for this is that when a sperm does not move, we cannot know whether the sperm is alive or not. It is possible that the absence of motility is due to a failure of its ciliary machinery, which is responsible for movement, or because the sperm is dead.
Provided below is an index with the 7 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 2.
- 2.1.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 3.5.
- 4.
- 5.
- 6.
- 7.
Determination of live and dead spermatozoa
When a seminal sample has a high percentage of immotile spermatozoa, it is necessary to determine whether they are alive or not, that is, to assess sperm vitality.
Even though sperm have no motility, it does not mean that they are dead. Therefore, the study of sperm vitality is essential.
Therefore, the objective of the sperm vitality test is to determine the number of live spermatozoa in a semen sample, regardless of whether they are immotile.
Two types of methodologies for assessing sperm vitality are detailed below.
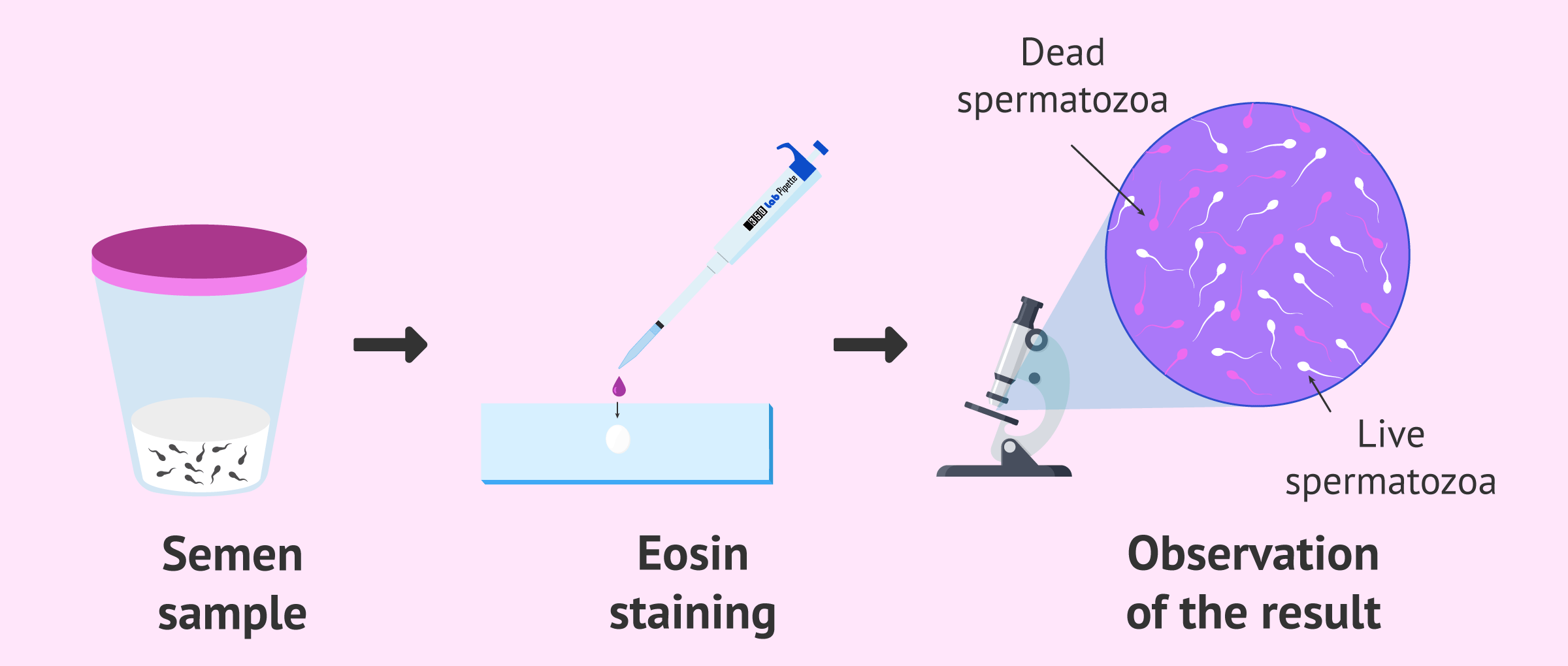
Eosin staining
Currently, the most commonly used sperm vitality test in assisted reproduction centers is the eosin test, also known as the Williams Pollack test williams Pollack test.
To carry out this methodology and determine the percentage of spermatozoa that are alive in a semen sample, an eosin stain is performed on the spermatozoa. It should be noted that the male will obtain the semen sample by masturbation without exceeding the abstinence period of 2-5 days. In this way, the results obtained from the test will be reliable.
A characteristic of dead spermatozoa in the presence of perforations and holes in their membranes, making them permeable to the eosin dye. So, when the staining is performed and the sample is observed under the microscope, the dead sperm will appear stained.
In contrast, eosin will not be able to penetrate living spermatozoa since their membrane is intact. For this reason, live sperm will appear white.
Hypoosmotic test
To a lesser extent, another sperm vitality study used is the hypoosmotic test. This test is based on the integrity of the sperm membrane of the sperm.
Spermatozoa are diluted with a hypotonic solution, which produces an osmotic imbalance between the extracellular and intracellular medium. Thanks to the reaction of the spermatozoa to this solution, it can be distinguished:
- Live spermatozoa
- try to regulate the imbalance caused by the hypotonic solution between the external environment and the interior of the spermatozoon by incorporating water into the interior. This causes an increase in the volume of the sperm and the tail of the sperm will coil into a helix shape.
- Dead spermatozoa
- hypotonic solution has no effect on dead spermatozoa. In this case, the tail will not curl and no water will enter the sperm.
The advantage of this technique is that it does not kill spermatozoa, so it can be used for fertility treatment. Therefore, the hyposmotic test is a good option for semen samples with low sperm concentration.
Sperm vitality index results
Once the methodology to be applied to assess sperm vitality has been determined, it is essential to know that at least 200 spermatozoa must be evaluated to obtain reliable results.
The World Health Organisation (WHO) published an update of the Laboratory Manual for Semen Testing and Processing in 2021 (the sixth edition). However, the criteria of the fifth edition (2010) are still the most common.
In view of this, the WHO dictates that from 58% of live spermatozoa the semen sample is considered normal. On the other hand, if the vitality index is less than 58%, sperm vitality is altered and the semen sample has a high number of dead spermatozoa.
Therefore, when the percentage of dead spermatozoa in a sperm sample is greater than 42%, it is referred to as necrozoospermia.
Considering undergoing a fertility treatment? By getting your individual Fertility Report your will see different clinics especially selected for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
Necrozoospermia
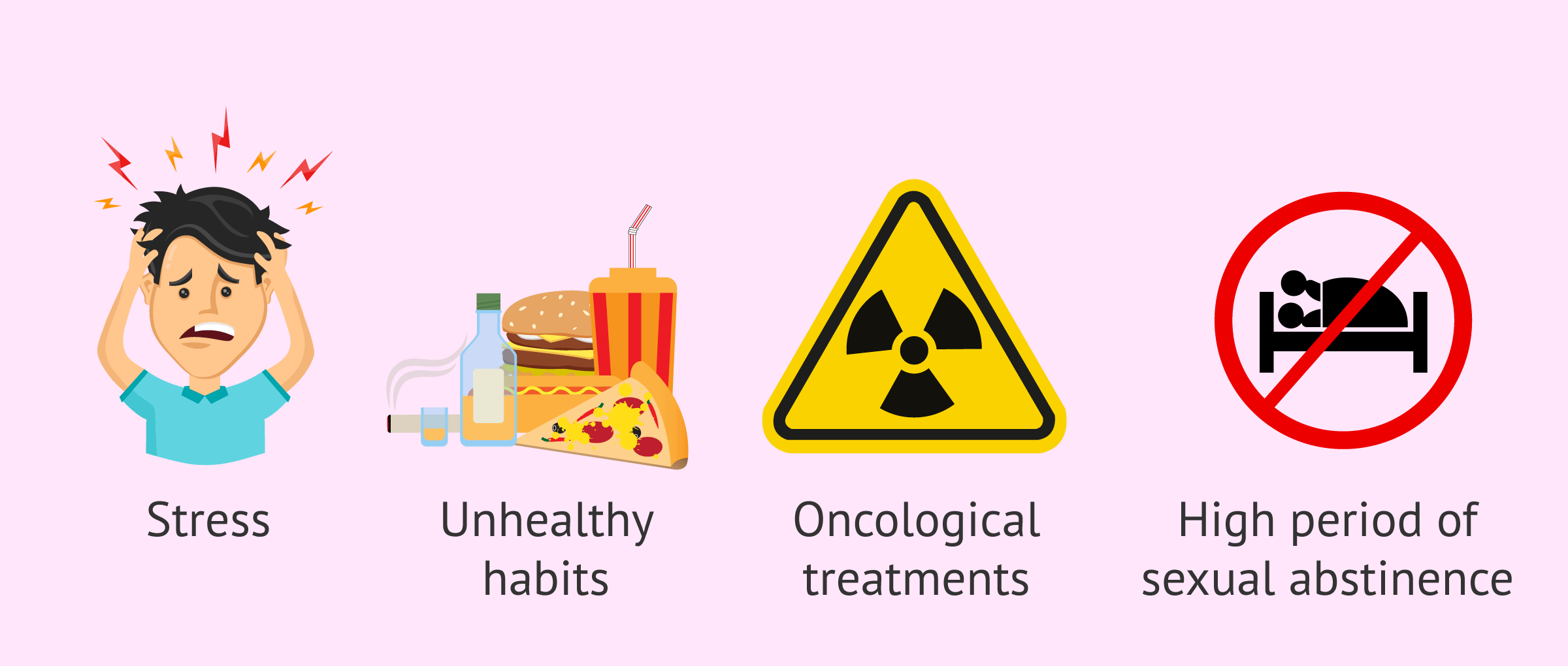
It is one of the main causes of male sterility due to a sperm factor. The most frequent causes of necrozoospermia are listed below:
- Stress.
- Consumption of alcohol, drugs or poor diet.
- Oncological treatments.
- Urinary tract infections.
- Hormonal disorders.
- Long period of sexual abstinence.
Necrozoospermia has no specific treatment to prevent sperm death. However, men are always advised to lead an appropriate lifestyle, reduce the withdrawal period, or even take dietary supplements.
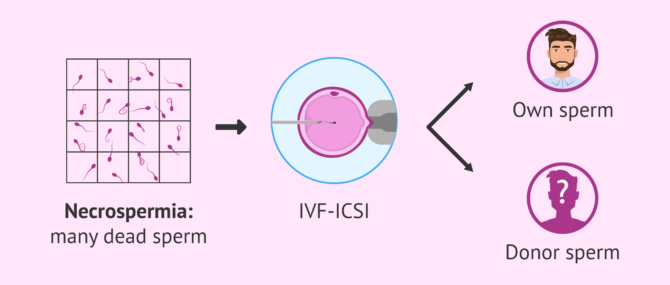
For those patients with necrozoospermia who wish to become parents, in vitro fertilization (IVF) with intracytoplasmic embryo injection (ICSI) is recommended to achieve gestation. In this way, only a small amount of live sperm will be needed.
If the IVF-ICSI treatment is not positive, it would be the time to consider assisted reproduction treatment with sperm donation.
If you would like to learn more about this semen alteration, we recommend you visit the following article: Spermatozoa with necrospermia: definition, causes, and treatment.
FAQs from users
Can sperm vitality be improved?
Yes, healthy habits are the best way, as well as avoiding toxins (tobacco, plastics, etc.). In addition, the intake of trace elements and antioxidants can improve sperm motility. In particular, nuts, tomatoes and asparagus are good foods to achieve this.
On the other hand, there are multiple polyvitamins on the market aimed at improving sperm vitality and they are readily available in pharmacies.
How is sperm vitality determined?
Sperm vitality is the test that indicates the number of live sperm present in an ejaculate sample.
Mainly, the analysis of sperm vitality is carried out through two methodologies:
- Eosin staining
- the most widespread analysis among most assisted reproduction units. It consists of, through a series of fixation and coloration processes, distinguishing live sperm from those that are not through the color they present. The rationale is based on the absorption of different dyes, eosin in this case, by dead cells, so that when counting we will observe non-stained (live) sperm and stained (dead) sperm, expressing said result as a percentage after having counted at least 200 cells.
- Hypo-osmotic test
- based on the semi-permeability characteristic of the membranes and its variations in media of different osmolarity.
When one technique or another has been performed and the number of live or dead spermatozoa is obtained, the result can be established. If the percentage of live sperm is equal to or greater than 58%, sperm vitality is considered to be correct.
Read more
How long do sperm cells last alive in the female body?
After vaginal ejaculation, sperm can survive in the woman's body for a maximum of 4-5 days. The conditions in the female are similar to those in the male and therefore the sperm can survive.
How long do live sperm last in the condom or in the hand?
The external conditions are not favorable to the sperm requirements and therefore if the ejaculation is external, the spermatozoa die within a few hours. For this reason, it is so important to try to maintain the temperature and light conditions during the collection of the semen sample for a semen analysis or an assisted reproduction treatment.
What is the price of the semen vitality test?
As mentioned above, vitality testing is not routinely performed on a semen analysis. However, if the semen analysis yields an altered motility result, the test will be included in the spermiogram tests, usually at no additional cost.
Recommended readings
In addition to sperm vitality, it is important to study other factors in the semen analysis. If you wish to obtain more information on this topic, we recommend that you continue reading here: How are the results of the semen analysis and its values interpreted?
On the other hand, IVF-ICSI is an option to achieve gestation in those males who suffer from necrozoospermia. For more information about this assisted reproduction treatment, you can visit the following article: Sperm Microinjection: What is ICSI and how much does it cost?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
A De Bantel, J Fleury-Feith, C Poirot, I Berthaut, C Garcin, P Landais, C Ravel. Simultaneous vitality and DNA-fragmentation measurement in spermatozoa of smokers and non-smokers. Cytometry B Clin Cytom. 2015 Mar;88(2):120-4. doi: 10.1002/cyto.b.21185. Epub 2014 Sep 13.
Byron Asimakopoulos, Aggeliki Tiptiri-Kourpeti, Chryssa Metalinou. Erythropoitein Increases In Vitro Motility and Vitality of Human Spermatozoa. In Vivo. 2021 Sep-Oct;35(5):2669-2673. doi: 10.21873/invivo.12550 (View)
Khayamabed R, Tavalaee M, Taherian SS, Nasr-Esfahani MH. Effect of recombinant β-defensin 1 protein on human sperm motility and viability. Andrologia. 2020 Feb;52(1):e13455. doi: 10.1111/and.13455. Epub 2019 Oct 27 (View)
Moskovtsev SI, Librach CL. Methods of sperm vitality assessment. Methods Mol Biol. 2013;927:13-9.
Saleem A Banihani, Reema M Shatnawi. Aspirin decreases human sperm motility and vitality, chelates seminal calcium, but insignificantly reduces seminal nitric oxide production. Andrologia. 2020 Nov;52(10):e13776. doi: 10.1111/and.13776. Epub 2020 Jul 29 (View)
Sapozhkova ZY, Eremin KI. Updates in protocol for human semen examination. Klin Lab Diagn. 2020;65(2):106-110. doi: 10.18821/0869-2084-2020-65-2-106-110.
World HEalth Organization. WHO Laboratory manual for the examination and processing of human semen, 5º ed. Geneve: World Health Organization, 2010 (View)
Zhou H, Li Q, Guo LY, Yuan JR, Liu M, Zhao XT, Ye GD. Hamilton-Thorne Integrated Visual Optical System Ⅰ (IVOSⅠ) versus IVOS Ⅱ for human sperm analysis. Zhonghua Nan Ke Xue. 2019 Apr;25(5):315-321.
FAQs from users: 'Can sperm vitality be improved?', 'How is sperm vitality determined?', 'How long do sperm cells last alive in the female body?', 'How long do live sperm last in the condom or in the hand?' and 'What is the price of the semen vitality test?'.
Authors and contributors
More information about Cristina Algarra Goosman







Hi, my husband was told that he had all immotile or dead sperm, I am not very clear. Is there any chance of getting pregnant naturally?
Hello Bella,
If your husband has a sperm condition, either the presence of dead sperm (necrospermia) or immotile sperm (asthenozoospermia) pregnancy naturally will be complicated or even impossible. The best technique that professionals recommend for this kind of diagnosis is IVF-ICSI which would increase your chances of getting pregnant. If you want to learn more about this technique read the following article: What is ICSI tecnique?
Therefore, it is important that you go to your medical specialist so that he/she can establish the appropriate diagnosis and treatment for your condition.
I hope I have helped you,
Best regards
Hi, my husband has been found to have 30% normal sperm but the rest have malformations or are missing the tail or things like that, having a 30% chance we could get pregnant? Thank you
Hello Ariana1992,
Finding pregnancy with a sperm condition reduces the possibility of pregnancy. If there are 30% of sperm, the most normal thing is that if they fertilize the egg they will be healthy sperm, since fertilization requires having the optimal qualities to fertilize the egg.
Based on the general guidelines this would be a healthy amount of functional sperm cells and shouldn´t have trouble conceiving. If after 6 months of trying, or a year if you are under 35, and you haven’t conceived then I would encourage you to seek professional help.
You could go to a fertility clinic so that they can explain to you how to proceed. Here is our Directory of Clinics where you can locate the clinics closest to you.
I hope I have helped you,
Best regards