Obesity in pregnant women is associated with an increased risk of certain obstetric complications such as gestational diabetes or preeclampsia. However, elevated body mass index (BMI) in pregnant women has also been linked to the risk of miscarriage.
Although the causes of obesity leading to this increased miscarriage rate are unclear, the uterine inflammatory environment may be related.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 4.
- 4.1.
- 4.2.
- 5.
- 6.
- 7.
- 8.
Obesity and female fertility
Obesity has been linked to infertility in women, as the associated hormonal alterations can cause problems for ovulation to occur correctly and menstrual imbalances.
However, the reproductive potential of these women would be reduced even with normal menstrual cycles. This means that obesity would lead to a longer time to pregnancy, but not only because of the ovulatory problems mentioned above.
Therefore, the oocytes, embryos, and/or endometrium could also be affected if the woman suffers from obesity.
On the other hand, the results of assisted reproduction techniques are also worse in the case of obese patients, with a lower live birth rate.
Obesity and pregnancy
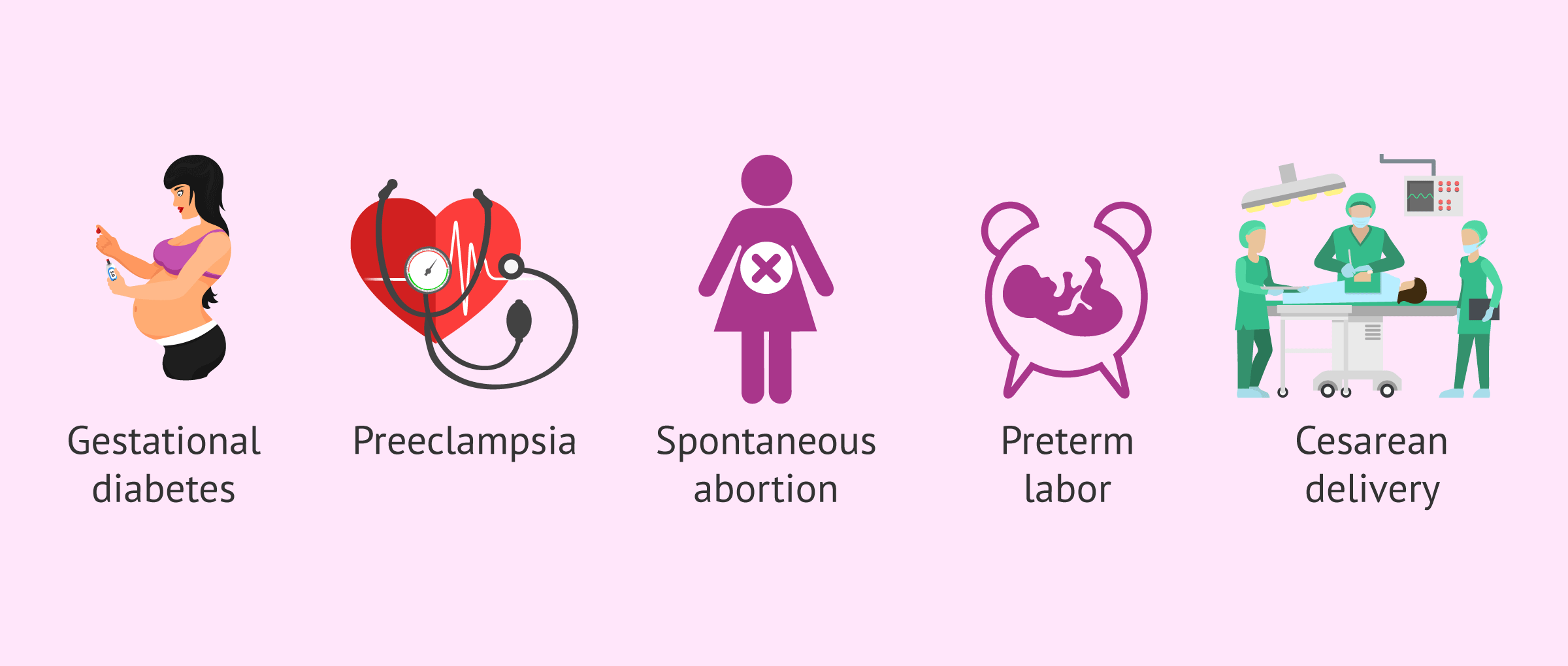
Once pregnancy is achieved, if the woman has a high BMI, she may present a greater number of complications. Among them, we can mention the following:
- Gestational diabetes
- Preeclampsia and hypertension problems
- Spontaneous abortion
- Premature delivery
Additionally, the risk of cesarean delivery would also be increased in these patients.
Effects on offspring
Notwithstanding the above, obesity in pregnant women can also have effects on their offspring. Children born to a woman with a high BMI may be more likely to suffer:
- Obesity
- Diabetes
- Hypertension
On the other hand, maternal obesity may increase the risk of certain congenital anomalies and of having a larger or high birth weight baby(macrosomia).
Obesity and abortion
As we have mentioned, overweight and obesity are associated with an increased risk of miscarriage, whether pregnancy has been achieved naturally or with the help of assisted reproductive techniques.
In addition, obesity seems to increase the risk of miscarriage independently of whether the woman has polycystic ovarian syndrome(PCOS) or not.
Causes
The causes for obesity to influence this increased risk of miscarriage have not been clarified. It has been proposed that obesity would lead to an affectation of the oocytes and, therefore, of the embryo. However, the involvement of the uterine environment could also play an important role.
Women with obesity problems have been found to have a higher rate of miscarriage after the transfer of euploid embryos (with the correct number of chromosomes).
This suggests that embryonic aneuploidy is not the factor responsible for the increased risk of miscarriage in obese patients.
Therefore, all this leads to think of a possible uterine or placental alteration that leads to the interruption of embryonic development.
Repeated miscarriage
Repeat miscarriage, although there has been some controversy in its definition, is the loss of two or more previous pregnancies.
Although there are certain known causes for this condition, obesity may also be related to recurrent miscarriage. For women with a history of repeat miscarriage, a BMI greater than 30 increases the risk of miscarriage for a future pregnancy.
Because obesity is associated with chronic inflammation, the immune system may be involved in the increased number of obstetric complications in these patients.
Risk reduction
Due to all the obstetric complications, we have mentioned that can occur when a woman becomes pregnant with obesity, one of the main measures to adopt would be to lose weight before seeking gestation.
A Mediterranean diet based on vegetables, fruits, cereals, legumes, and fish could help to keep weight under control, as well as be associated with low levels of inflammation.
On the other hand, it is equally important to control weight gain during pregnancy so that it is not excessive. However, losing weight or gaining too little is also not ideal during pregnancy.
Finally, it should be noted that if the woman has high postpartum weight retention, it may increase the risk of obstetric complications in the next pregnancy.
FAQs from users
Is there any benefit or advantage to being overweight to avoid abortion?
No, an elevated body mass index (BMI) in pregnant women is not beneficial, as it is associated with certain obstetric complications. These include an increased risk of miscarriage.
What are the risks of obesity in pregnancy?
A woman who becomes pregnant with obesity has an increased risk of complications during pregnancy, for herself and for the baby.
If the woman has a high BMI, the risk of gestational diabetes, preeclampsia, hypertension and miscarriage is increased. In addition, the risk of cesarean delivery is also increased.
For the offspring, maternal obesity can lead to an increased risk of obesity, hypertension and diabetes, as well as certain congenital anomalies.
Recommended readings
If you are interested in knowing more about recurrent miscarriage, we recommend you to visit the following link: What is recurrent miscarriage - Causes, diagnosis, and treatment.
On the other hand, if you want to read more in-depth about the different types of miscarriage, you can visit this article: Types of miscarriage: how many are there and how do they differ?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Bellver J, Ayllón Y, Ferrando M, Melo M, Goyri E, Pellicer A, Remohí J, Meseguer M. Female obesity impairs in vitro fertilization outcome without affecting embryo quality. Fertil Steril. 2010 Feb;93(2):447-54. (See)
Bellver J, Melo MA, Bosch E, Serra V, Remohí J, Pellicer A. Obesity and poor reproductive outcome: the potential role of the endometrium. Fertil Steril. 2007 Aug;88(2):446-51. (See)
Boots C, Stephenson MD. Does obesity increase the risk of miscarriage in spontaneous conception: a systematic review. Semin Reprod Med. 2011 Nov;29(6):507-13. (See)
Broughton DE, Moley KH. Obesity and female infertility: potential mediators of obesity's impact. Fertil Steril. 2017 Apr;107(4):840-847. (See)
Cavalcante MB, Sarno M, Peixoto AB, Araujo Júnior E, Barini R. Obesity and recurrent miscarriage: A systematic review and meta-analysis. J Obstet Gynaecol Res. 2019 Jan;45(1):30-38. (See)
Cozzolino M, García-Velasco JA, Meseguer M, Pellicer A, Bellver J. Female obesity increases the risk of miscarriage of euploid embryos. Fertil Steril. 2021 Jun;115(6):1495-1502. (See)
Ginsburg ES, George JS. Weighing in: the impact of obesity on euploid miscarriage rates. Fertil Steril. 2021 Jun;115(6):1433-1434. (See)
Lashen H, Fear K, Sturdee DW. Obesity is associated with increased risk of first trimester and recurrent miscarriage: matched case-control study. Hum Reprod. 2004 Jul;19(7):1644-6. (See)
Ma RCW, Schmidt MI, Tam WH, McIntyre HD, Catalano PM. Clinical management of pregnancy in the obese mother: before conception, during pregnancy, and post partum. Lancet Diabetes Endocrinol. 2016 Dec;4(12):1037-1049. (See)
Maheshwari A, Stofberg L, Bhattacharya S. Effect of overweight and obesity on assisted reproductive technology--a systematic review. Hum Reprod Update. 2007 Sep-Oct;13(5):433-44. (See)
Metwally M, Ong KJ, Ledger WL, Li TC. Does high body mass index increase the risk of miscarriage after spontaneous and assisted conception? A meta-analysis of the evidence. Fertil Steril. 2008 Sep;90(3):714-26. (See)
Metwally M, Preece R, Thomas J, Ledger W, Li TC. A proteomic analysis of the endometrium in obese and overweight women with recurrent miscarriage: preliminary evidence for an endometrial defect. Reprod Biol Endocrinol. 2014 Aug 5;12:75. (See)
Metwally M, Saravelos SH, Ledger WL, Li TC. Body mass index and risk of miscarriage in women with recurrent miscarriage. Fertil Steril. 2010 Jun;94(1):290-5. (See)
Metwally M, Tuckerman EM, Laird SM, Ledger WL, Li TC. Impact of high body mass index on endometrial morphology and function in the peri-implantation period in women with recurrent miscarriage. Reprod Biomed Online. 2007 Mar;14(3):328-34. (See)
Poston L, Caleyachetty R, Cnattingius S, Corvalán C, Uauy R, Herring S, Gillman MW. Preconceptional and maternal obesity: epidemiology and health consequences. Lancet Diabetes Endocrinol. 2016 Dec;4(12):1025-1036. (See)
Provost MP, Acharya KS, Acharya CR, Yeh JS, Steward RG, Eaton JL, Goldfarb JM, Muasher SJ. Pregnancy outcomes decline with increasing recipient body mass index: an analysis of 22,317 fresh donor/recipient cycles from the 2008-2010 Society for Assisted Reproductive Technology Clinic Outcome Reporting System registry. Fertil Steril. 2016 Feb;105(2):364-8. (See)
Silvestris E, de Pergola G, Rosania R, Loverro G. Obesity as disruptor of the female fertility. Reprod Biol Endocrinol. 2018 Mar 9;16(1):22. (See)
Spencer L, Rollo M, Hauck Y, MacDonald-Wicks L, Wood L, Hutchesson M, Giglia R, Smith R, Collins C. The effect of weight management interventions that include a diet component on weight-related outcomes in pregnant and postpartum women: a systematic review protocol. JBI Database System Rev Implement Rep. 2015 Jan;13(1):88-98. (See)
Talmor A, Dunphy B. Female obesity and infertility. Best Pract Res Clin Obstet Gynaecol. 2015 May;29(4):498-506. (See)
FAQs from users: 'Is there any benefit or advantage to being overweight to avoid abortion?' and 'What are the risks of obesity in pregnancy?'.
Author
More information about Cristina Algarra Goosman




Hi, I have a high BMI, does that mean I will have miscarriages?
Hi MeganST,
Not at all, an elevated BMI increases the risks of miscarriage but it does not mean that all pregnancies of overweight people are destined for miscarriage.
I recommend that you keep going to your doctor’s visits and follow the recommendations to have as healthy a pregnancy as possible, and try to avoid complications.
I hope I have helped you,
Best regards.
Hi, I am starting to think about having a baby but I am a little overweight, what should I do to control it before getting pregnant?
Hello Noi,
The search for pregnancy is a period in which it is important to optimize your health as much as possible, so we recommend that you take care of both your diet and any toxic habits you may have.
Following the Mediterranean diet is a good option to try to control weight, however, if you have difficulties you can go to a nutritionist who will help you with your nutrition.
I hope I have helped you.
Best regards.