The third month of pregnancy marks the end of the first trimester. It covers from weeks 9 to 12 of pregnancy, and is a time period that involves great changes.
Symptoms for the pregnant woman start being noticeable to the naked eye, since the belly and breasts have increased in size. On the other hand, fetal development is completed, and now the fetus is growing unstoppably.
Several prenatal visits to your doctor are required during this month in order to gather information on fetal health. Moreover, after the first three months, the risk of miscarriage drops dramatically, and you will start enjoying your pregnancy above all.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 1.3.
- 1.4.
- 2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 5.
- 6.
- 7.
- 8.
How does the baby change?
At 3 months, the embryonic period finishes, marking the beginning of the fetal period. The embryo is now called fetus.
The vital organs of the unborn child are now fully formed, and some of them start working. However, specialization and differentiation of each system continues during the following weeks.
The following are the most remarkable events taking place this month:
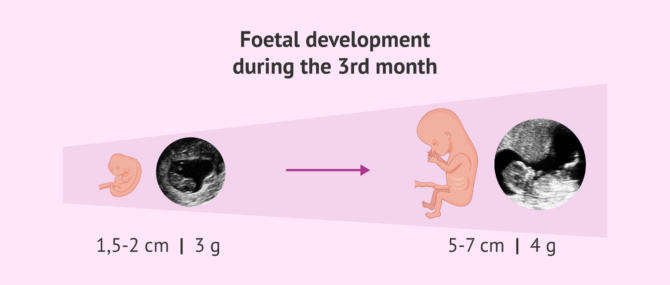
- The fetus grows from 1.5-2 cm at the end of month two to 5-7 cm long by the end of month three.
- The weight varies from 3 to 14 g approximately as the fetus continues its development.
- Male or female genitalia start their formation, although the gender is not visible through ultrasound scan yet.
- The fetus resembles a human being now: facial features are more evident, the limbs get longer, hands and feet are more defined, and the toes and fingers have separated.
What follows are the main changes that occur to the unborn baby by week.
One should note that fetal development does not work as a mathematical operation. Thus, the changes and factors explained herein are just general information. Differences can be found by week depending on each woman and pregnancy.
Week 9
When the third month of pregnancy begins, the embryo measures between 2.5 and 4 3 cm. As one can imagine, it is still very small, but the appearance is more human-like than in the second month.
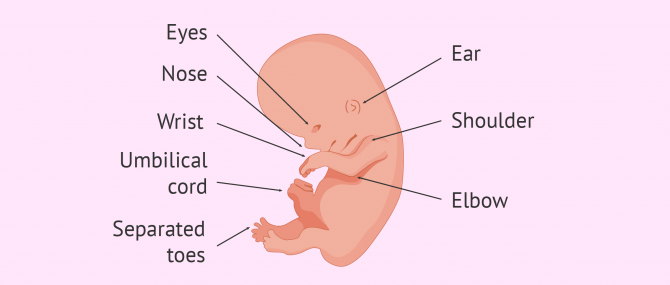
Fetal development occurs faster now: the legs and arms grow longer, and we can distinguish the hands and feet with fingers and toes formed, the shape of the head can be distinguished thanks to the formation of the nose and ears, etc.
The eyes, which have migrated to the frontal part of the face, develop with eyelids, although they will remain shut until later.
Week 9 is the last week of the embryonic period. Learn more: The Ninth Week of Pregnancy.
Week 10
At this point, the fetus already measures between 3-4 cm and weighs 5 grams approximately. The fact that fetal growth occurs so rapidly causes your uterus to expand, and therefore you may feel your belly more bloated.
Typically, the fetus starts moving from this moment onwards: he can open and shut his mouth, hands, and feet. It is likely that you start noticing the first baby kicks, medically known as patellar reflex or knee-jerk. This is a biological resource that prepares us for being able to walk.
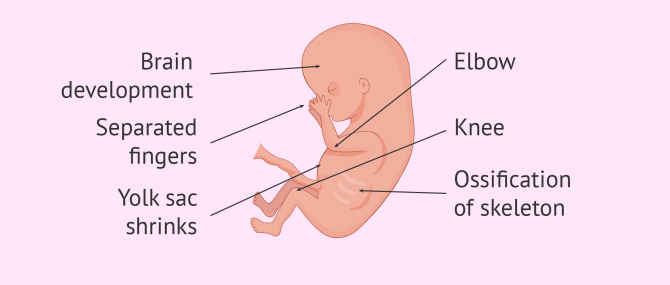
Other changes include the formation of the tongue and palate, the appearance of the elbows and knees, the growth of about 250,000 neurons per minute, growth of lanugo (fetal hair), the formation of the anus, etc.
Moreover, the yolk sac is progressively shrinking, since the placenta feeds your baby now.
Get more info by clicking the following link: The Tenth Week of Pregnancy.
Week 11
At week 11th, fetal measures are 4-5 cm, and the weight can be as high as 7-8 g approximately. Although the skin is still very thin and transparent, the body has acquired a more elongated form now.
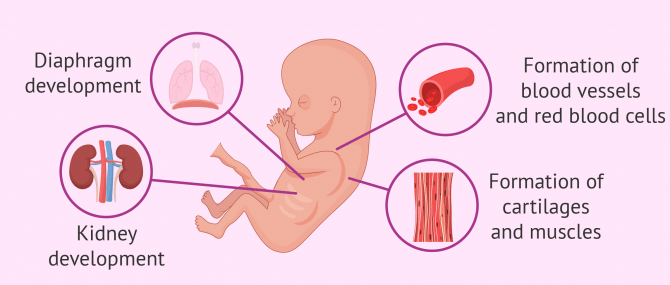
Vital organs like the liver, kidneys, and stomach are fully formed, and some of them have even started working.
For instance, the fetus generates own red blood cells now. Moreover, he or she is capable of expelling urine, which mixes with amniotic fluid. Male fetuses produce testosterone, which contributes to sexual differentiation.
Diaphragm formation occurs at this point, too. From this moment on, the fetus may hiccup while in the womb.
You may like: The Eleventh Week of Pregnancy.
Week 12
The head is slowly acquiring a round-shape and the expected size. The neck is longer now, and the ears are located in an adequate position, at both sides of the head.
The following are average fetal measurements and weight on week 12 of pregnancy: between 5 and 6 cm, and 8-14 grams, respectively.
Also, the organs and main systems are fully developed, and each one can be found on the expected location (stomach, liver, lungs, pancreas, and intestines). However, more specialization and development is still required.
A major change during week 12 is the formation of the genitalia. However, they cannot be distinguished via ultrasound scan yet.
Aside from all this, the fetus moves energetically, and continues developing different reflexes. Although it is still unnoticeable by the mother, the fetus is able to react to little stimuli like rubbing your belly.
The sucking reflex starts during this week as well. The fetus is capable of inserting a finger on the mouth, thereby learning to suck and getting ready for breastfeeding.
Further reading: The Twelfth Week of Pregnancy.
Mother's symptoms
Fortunately, the most unpleasant symptoms of pregnancy, like nausea and vomiting, start to disappear this month. However, you are still likely to experience them throughout the whole month up until the beginning of month 4 approximately.
In essence, the most remarkable symptoms of pregnancy during month 3 include:
- Increased breast size. Areolas become harder and darken. Also, you will notice the appearance of darkened veins along your breasts.
- Your belly starts showing. Uterine size increases and starts growing out of the pelvis. By the end of month 3, pregnancy is visible to others.
- It is normal that you gain between 1 and 2 kg during this month. It is likely that you need maternity clothes from now on.
- Abdominal cramps due to the placenta and pelvic muscles expanding.
- Your skin will become softer and brighter due to increased blood and hormone levels. You may have acne as well.
- Melasma, also known as chloasma faciei, or the mask of pregnancy, may occur as well. It characterizes by the appearance of macules and/or patches in the skin. Using high-level sun protection is strongly recommended.
- Increased blood flow and dilation of capillary vessels may cause spider veins to pop out, especially in breast and legs.
- Nails and hair growth faster and stronger.
- Gastrointestinal (GI) issues: heartburn, acidity, flatulence, and/or constipation.
- Leg cramps due to the uterus pressing on certain nerves
As regards your emotions during this stage of pregnancy, it is likely that you are oversensitive due to hormonal changes. It is common for pregnant women to have sudden mood changes, cries for no apparent reason, is extremely tired or more sleepy than usual.
Moreover, the mother-to-be feels more intensely the presence of the baby inside her, even though she does not feel him or her moving yet.
Screenings & tests
In the third month, you will have the first of the many prenatal checkups that you will have throughout the course of pregnancy.
Sometimes, the first visit is done in the second month of pregnancy. However, many women do not find out that they are expecting until week 8.
In any case, your doctor will conduct a weight and blood pressure check to start monitoring your pregnancy. Also, he or she will carry a vaginal and breast examination, as well as a pap smear in case you the last one was performed more than a year ago.
Your doctor will ask you a series of questions concerning your clinical history: date of the last menstrual period, previous pregnancies, potential miscarriages or abortions, remarkable symptoms, etc.
Moreover, you will be asked to undergo the following tests:
Urine & blood tests
Urine tests carried out during pregnancy are used to detect the presence of potential urinary tract infections (UTIs). Also, it is also a useful tool for the diagnosis of certain obstetric complications, such as gestational diabetes or preeclampsia.
As for the bloodwork, it provides information about the following parameters:
- Blood type and maternal Rh factor
- Antibodies that work against certain viruses, such as hepatitis, toxoplasmosis, rubeola... infectious diseases that can lead to pregnancy complications.
- Iron levels to detect anemia
- Beta-hCG and PAPP-A protein levels to perform the triple test of the first trimester
Urine and blood tests are repeated every three months during the course of pregnancy.
Ultrasound scan
The ultrasound scan of week 12 is one of the most important screenings carried out when a woman is pregnant, since it provides us with relevant information regarding the baby's health, which is highly reassuring for the parents-to-be.
Amongst the many parameters this ultrasound allows us to examine, the following are fundamental:
- Fetal heartbeat
- Number of fetuses and gestational sacs to determine if it is a singleton or multiple pregnancy
- Fetal measurements and anatomical structures
- Nuchal translucency (NT) scan and fetal nasal bone length measurement, vital tests to dismiss the presence of genetic abnormalities
Nuchal translucency (NT) is the medical term to refer to a collection of fluid under the skin located at the back of the baby's skin, which should be less than 3 mm.
Triple screen test
The triple marker test or just triple test is a specific test done during the first trimester of pregnancy that is used to determine the risk of chromosomal abnormalities in the fetus.
To conduct this test, the following parameters are examined:
- PAPP-A: pregnancy associated plasma protein
- Free β-hCG
- Nuchal translucency as determined by ultrasound scan
Based on the results obtained with each one of these tests, along with maternal age and weight, the doctor determines the risk for the fetus to develop a chromosomal abnormality, like the Down's, Edwards, or Patau syndromes.
If the value is too elevated, the risk of your baby having some kind of anomaly is high. For this reason, you will be required to undergo an amnio test, chorionic biopsy, or chromosomal testing of maternal blood to confirm the diagnosis.
If you are interested in this topic and want to read more information, we recommend you to visit the following article: Nuchal translucency and combined first trimester screening.
FAQs from users
Is a triple test always done during pregnancy?
The triple test or triple screen is a universal test that is done in all women when they are pregnant, particularly around week 12 of pregnancy. It pays special attention to the risk of Down's syndrome in the fetus by combining two markers from the first trimester ultrasound with two hormones examined in pregnant women (BHCG + AFP) along with her age.
In case your OB/GYN refers you directly to invasive tests (amnio test or chorionic villus sampling) because you've been pregnant before and chromosomal abnormalities were detected in the fetus, then a triple test would be unnecessary.
How many weeks are 3 months pregnant?
Being 3 months pregnant equals 12 weeks out of the total 40 weeks of gestation. Particularly, month 3 of pregnancy covers from week 9 to week 12. Moreover, the third month of pregnancy marks the end of first trimester, the stage of pregnancy with the highest miscarriage rates.
Can you sleep on your stomach when 3 months pregnant?
Absolutely yes, since at this stage of pregnancy, the size of your belly is not so big, and therefore it won't be uncomfortable for you. However, we recommend that you start getting used to sleeping on your back or side to be more comfortable in more advances stages of pregnancy.
Can you feel the baby at 3 months?
During the third month of pregnancy, fetal movement is increasingly active, including kicking, rotating ankles and wrists, reaching his/her arms out, bending his/her fingers upwards and downwards, wrinkling the forehead, pressing the lips together, and other facial movements.
However, even though you will notice the common symptoms of pregnancy, it is still too early for you to feel these movements.
Is it safe to dye my hair at 3 months?
Most studies indicate that colorants and hair dyes do not harm the fetus or affect fetal development. However, as a preventive measure, many women prefer to use natural hair dyes or temporary hair colors, which do not penetrate into the cuticle layer, allowing only a coating action. Others prefer to avoid hair dyes until the end of the first trimester, which configures the most vulnerable period for the fetus.
Is it possible to have an abortion at 3 months of pregnancy?
It is possible. However, once you reach 3 months' gestation, the likelihood of miscarriage is reduced.
However, if there are any warning signs of a possible miscarriage, it is best to report it to a medical specialist.
Suggested for you
Month 4 is just around the corner, which translates into the entrance of the second trimester, a joyful stage for most parents-to-be. Read more: What Happens During the 4th Month of Pregnancy?
At this stage of pregnancy, it is also advisable to take care of yourself. Exercising is one of the best ways to achieve this goal. Recommended reading: Physical Activity and Exercise During Pregnancy.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Alcolea Flores, S., Mohamed Mohamed D. Guía de cuidados en el embarazo. Consejos de su matrona. Hospital Universitario de Ceuta (Dirección Territorial de Ceuta e Instituto Nacional de Gestión Sanitaria (ed.). Colección Editorial de Publicaciones del INGESA. ISBN: 978-84-351-0408-1 (View)
Consejería de Salud de la Junta de Andalucía (2002). Proceso Asistencial Integrado: Embarazo, Parto y Puerperio. Consejería de Salud, Junta de Andalucía. Sevilla (View)
Cunningham F, MacDonald P, Gant N et al. (1996). Adaptación maternal al embarazo. Masson SA. Cunningham F, MacDonald P, Gant N, et al. 4ª ed, Barcelona; pp. 201-237
Duyff, R.L. (2002). American Dietetic Association Complete Food and Nutrition Guide (2nd Ed.). Hoboken, New Jersey: John Wiley & Sons, Inc.
Eugene S, Bonapace MD, Robert S, Fisher MD. (1998). Constipation and diarrhea in pregnancy. Gastroenterol Clin North Am; 27: 197- 211 (View)
Gary F, Mc Donald P. (1996). Adaptación materna al embarazo. En: Gary F, MacDonald P, Grant N Lereso K, Gilstrap L, editores. Williams. Obstetricia (4.a ed.). Barcelona: Masson.
González Merlo J. (1992). Modificaciones fisiológicas producidas en el organismo materno por el embarazo. En: Williams. Obstetricia (4.a ed.). Barcelona: Masón (View)
Grupos de trabajo de la Guía de Embarazo y Parto, Guía de Salud Oral, y Guía de Lactancia Materna. Consejería de Sanidad, Dirección General de Salud Pública y Servicio de Salud del Principado de Asturias. Octubre de 2015.
March of Dimes, Pregnancy & Newborn Health Education Center. Exercise during Pregnancy. Retrieved March 11, 2008
National Health Service (NHS) (UK) (2009). The Pregnancy Book. Your complete guide to: A healthy pregnancy, Labour and childbirth, The first weeks with your new baby. Crown copyright 2009. Produced by COI for the Department of Health.
Obstetricia 4ª edición. J. González Merlo. Ed. Masson. Barcelona, 2003
Ramírez García O, Martín Martínez A, García Hernández JA. (2003). Duración del embarazo. Modificaciones de los órganos genitales y de las mamas. Molestias comunes del embarazo normal. Panamericana Ed. Tratado de Ginecología, Obstetricia y Medicina de la Reproducción. Cabero Roura L, Madrid.
The American College of Obstetricians and Gynecologists. (2005). Your Pregnancy and Birth (4th ed.). Washington, DC: Meredith Books.
The American Dietetic Association. (2008) Position of the American Dietetic Association: Nutrition and Lifestyle for a Healthy Pregnancy Outcome. Journal of the American Dietetic Association. 108:553-561.
U.S. Food and Drug Administration (FDA). Food Safety for Moms-To-Be. Retrieved April 09, 2010
FAQs from users: 'Is a triple test always done during pregnancy?', 'How many weeks are 3 months pregnant?', 'Can you sleep on your stomach when 3 months pregnant?', 'Can you feel the baby at 3 months?', 'Is it safe to dye my hair at 3 months?' and 'Is it possible to have an abortion at 3 months of pregnancy?'.