Like all other assisted reproductive techniques, artificial insemination (AI) has certain advantages and also some disadvantages.
Artificial insemination is considered a low-complexity technique, so its main advantage is that it is a simple and minimally invasive procedure.
However, certain requirements are needed to achieve pregnancy by AI and the succes rates achieved from it are not as good as those from in vitro fertilization (IVF).
Provided below is an index with the 7 points we are going to expand on in this article.
- 1.
- 1.1.
- 1.2.
- 1.3.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 3.4.
- 4.
- 5.
- 6.
- 7.
Advantages of artificial insemination
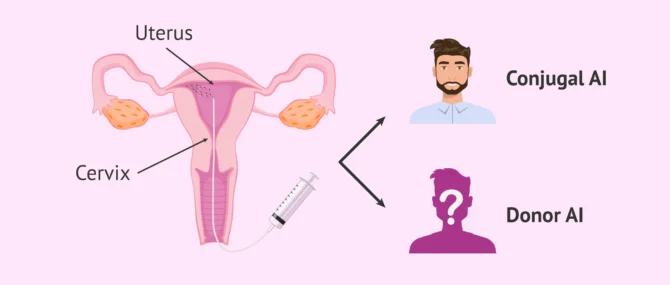
Although there are several types of AI depending on the site where the sperm are deposited, the most common is intrauterine insemination (IUI) and, for this reason, is the one we refer to when we speak simply of AI.
The process of intrauterine insemination is very simple and consists of introducing the sperm directly into the woman's uterus, through the cervix, with the help of a cannula.
The semen sample for IUI is preprocessed in the laboratory and can come from the male partner or from a sperm donor.
The following are the main benefits or advantages of artificial insemination.
Similarity with natural conception
AI is the assisted reproductive technique that most closely resembles natural conception. Unlike IVF cycles (where the patient's eggs are extracted by follicular puncture and subsequently fertilized in the laboratory), in artificial insemination, fertilization occurs inside the woman's body.
Furthermore, although it is true that in AI the sperm is artificially introduced into the patient's uterus to facilitate their journey, there is a natural selection in the female reproductive tract of the sperm that will eventually fertilize the egg.
Simplicity and low cost
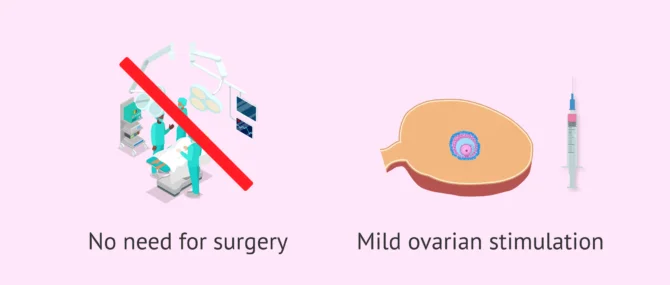
Artifical insemination can be performed in the gynecologist's office itself, without the need to go to the operating room. It is a very simple, fast and comfortable technique for the patient.
The process of introducing the cannula through the cervix to perform AI is painless and does not require anesthesia.
On the other hand, the ovarian stimulation performed prior to AI is milder than that required for IVF treatment, since only 1-2 follicles are sought for maturation. This reduces the side effects, the risks caused by hormone treatment and the costs associated with this medication.
In addition, because AI does not require too much personnel intervention, nor an operating room, nor embryo culture with complex maintenance and handling systems, its cost is lower than that of IVF treatments.
Advantages derived from the technique itself
In addition to the benefits discussed above, AI also has advantages that are characteristic of the insemination process itself:
- It increases the chances of gestation compared to natural conception due to the slight ovarian stimulation, the control to perform the insemination close to the ovulatory period, the processing of the semen sample and the introduction of the sperm directly into the uterus.
- It allows single women and couples formed by two women to become mothers through sperm donation.
Assisted procreation, as any other medical treatment, requires that you rely on the professionalism of the doctors and staff of the clinic you choose. Obviously, each clinic is different. Get now your Fertility Report, which will select several clinics for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
For all these reasons, AI is a widely used technique and should be the first choice for assisted reproduction in couples who do not have any factors that make it inadvisable.
Disadvantages of artificial insemination
Even with all the advantages mentioned above, the simplicity of the AI procedure implies certain requirements for the couple and influences the success rates. In addition, AI may have certain risks.
Requirements
AI is not an appropriate technique for all women or couples attending a fertility clinic. The specialist will be the one to assess and explain to the couple which assisted reproduction treatment may be the most appropriate in their case.
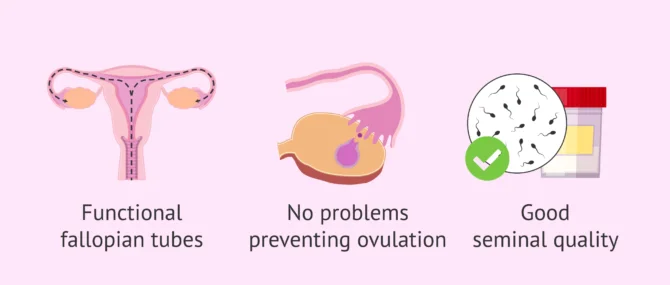
In order to achieve a pregnancy with the AI technique, the following conditions are required in the couple:
- The woman's Fallopian tubes must be functional, as this is where fertilization will occur.
- The woman must not have any problems that prevent her from ovulating spontaneously or induced by hormonal medication
- The quality of the spermatozoa must be good and present favorable results, or only slight alterations, in the semen analysis. In addition, a REM (motile sperm count) greater than 3 million progressive motile sperm is recommended after processing of the semen sample.
On the other hand, AI is usually used in young women with a maximum age of 35-37 years to have an acceptable chance of success.
Success rate
AI requires less human intervention than IVF. This also results in significantly lower success rates.
In the latest National Activity Registry of the Spanish Fertility Society (SEF) for 2022, the gestation rate (per cycle) for AI stands at 18.0% in women under 35 years of age. However, the delivery rate (per cycle) is 14.0% for women of the same age group.
Statistical data in this article shall not be used to imply or predict an outcome certainty to a specific individual within a population at risk.
For this reason, several AIs are usually performed to achieve gestation. It is usual to make 4 attempts with AI before opting for another assisted reproductive technique. Thus, the cumulative pregnancy rate amounts to approximately 60%. After the fourth AI attempt, the cumulative rate does not increase, so it is not advisable to continue seeking pregnancy by this technique.
If you wish to obtain more detailed information on the subject, we recommend you to visit the following article: What is the probability of success of artificial insemination?
Risks
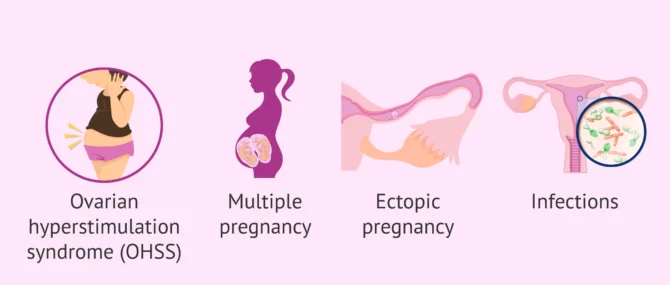
Despite its simplicity, AI is not without certain risks, such as those mentioned below:
- Ovarian hyperstimulation syndrome (OHSS). This syndrome is not very frequent in AI, since ovarian stimulation is mild.
- Multiple pregnancy, due to the maturation of more than 1 egg after ovarian stimulation. Multiple gestations are associated with increased obstetric risk during pregnancy and delivery.
- Ectopic pregnancy
- Infections or allergic reactions. Although very infrequent, such problems can occur after AI.
You can read more about these AI risks by clicking on the following link: Risks and consequences of artificial insemination.
FAQs from users
What are the advantages of AI for women under 35?
When a couple or a single patient comes to our fertility clinic, the first thing we do is a detailed study of both of them or of her if the woman comes alone.
The technique of artificial insemination or AI can be performed with the couple's sperm or with donor sperm when the woman comes alone or when the man has an absence of sperm.
AI is a simple and much less aggressive technique than in vitro fertilization (IVF). Its costs are much lower than those of IVF and the hormonal dose used is lower, which also reduces treatment costs.

After a period of hormonal stimulation of approximately 10 days and 2 previous ultrasound controls, the sperm is introduced into the uterine cavity by means of a cannula which is completely painless. It can even be performed in the gynecology office.
AI is advisable in cases of short-term sterility, with a male with normal results. One of the cases where it is also a very effective technique is in patients with polycystic ovary syndrome, since by stimulating ovulation we get the egg and sperm to unite.
Before performing an insemination you must have at least one permeable tube.
The chances of pregnancy, with respect to natural conception, will increase because during ovarian stimulation is controlled at what time is the most appropriate for the introduction of the semen sample.
Finally, it is important to emphasize that pregnancy rates are not high and that sometimes it is necessary to perform more than one insemination to achieve success.
What are the advantages of donor AI over spousal AI?
Conjugal insemination (CAI) is indicated when there is a mild fertility problem, either due to an ovulatory factor, mild endometriosis, mild male factor or idiopathic cause. Within the mild male causes, there may be a mild decrease in sperm concentration or motility, but most of the time there is already a cause of infertility.
In the case of inseminations with donor sperm, we use a totally normal sperm (donor) and with a good fertilizing capacity and, generally, there are no fertility problems in the woman. There may be cases of single women, couples of women or severe male factors such as secretory azoospermia that require a male gamete change. This means that the reproductive prognosis or the possibilities of success are slightly higher with donor sperm.
On the other hand, the use of donor sperm allows us to have a little more security due to the numerous medical, analytical and genetic tests that are performed on donors in order to avoid the birth of a sick child or the transmission of any genetic or infectious disease.
What are the advantages of AI ovarian stimulation over IVF?
The advantages of ovarian stimulation prior to AI, compared to that performed before IVF, are:
- Fewer side effects associated with hormonal treatment.
- Less risk of ovarian hyperstimulation syndrome (OHSS).
- Less cost associated with medication.

All these advantages are related to the lower amount of gonadotropins required in AI, since only 1-2 follicles are being matured.
Is it inconvenient to have a tubal ligation to perform an AI?
Yes, in order to perform an artificial insemination, it is necessary that the fallopian tubes are functional. Having the tubes tied will prevent the egg and sperm from meeting and, therefore, fertilization will not be possible.
However, in vitro fertilization (IVF) treatments do not have this requirement, since fertilization takes place outside the woman's body, that is, in the laboratory.
Recommended reading
If you want to continue reading and would like more in-depth information about the process of artificial insemination, you can visit the following link: How is artificial insemination done step by step?
If what you need is information about IVF treatments, we recommend reading this article: In vitro fertilization (IVF): What is it and how much does it cost?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Cohlen B, Bijkerk A, Van der Poel S, Ombelet W. IUI: review and systematic assessment of the evidence that supports global recommendations. Hum Reprod Update. 2018 May 1;24(3):300-319 (View)
Ejzenberg D, Gomes TJO, Monteleone PAA, Serafini PC, Soares-Jr JM, Baracat EC. Prognostic factors for pregnancy after intrauterine insemination. Int J Gynaecol Obstet. 2019 Oct;147(1):65-72 (View)
Evans MB, Stentz NC, Richter KS, Schexnayder B, Connell M, Healy MW, Devine K, Widra E, Stillman R, DeCherney AH, Hill MJ. Mature Follicle Count and Multiple Gestation Risk Based on Patient Age in Intrauterine Insemination Cycles With Ovarian Stimulation. Obstet Gynecol. 2020 May;135(5):1005-1014 (View)
Matorras R, Rubio K, Iglesias M, Vara I, Expósito A. Risk of pelvic inflammatory disease after intrauterine insemination: a systematic review. Reprod Biomed Online. 2018 Feb;36(2):164-171 (View)
Sociedad Española de Fertilidad. Registro Nacional de Actividad 2021-Registro SEF (View)
FAQs from users: 'What are the advantages of AI for women under 35?', 'What are the advantages of donor AI over spousal AI?', 'What are the advantages of AI ovarian stimulation over IVF?' and 'Is it inconvenient to have a tubal ligation to perform an AI?'.
Authors and contributors
More information about Cristina Algarra Goosman

More information about Michelle Lorraine Embleton






Hi, we have been trying to get pregnant for several years and we are having a hard time, we have done an AI but it was negative. Wouldn’t it be better to go directly to IVF and not repeat another AI, I have been told to repeat the AI.
Hello Linsdey,
Performing several cycles of Artificial Insemination is recommended for patients who have no need to perform a more complex procedure such as IVF.
Generally based on success rates it is recommended to perform 4 cycles of AI before attempting IVF, after this, the accumulative percentage of success greatly declines. In addition, the AI procedure is more economical and less invasive than IVF so it is advisable to explore this technique.
I recommend that you talk to your doctors to explain the rationale for continuing with AI and the advantages and disadvantages of IVF based on your medical history and reproductive desires.
I hope I have helped you.
Best regards.
Hello, I had a tubal ligation and now I want to try to be a mother again, I was recommended an assisted reproduction technique or an operation to untie my tubes, it is better to perform an AI, isn’t it?
Hello Aina43,
In the case of tubal ligation, there are effectively two options, to perform a reversal in which functional tubal patency would be attempted to restore (this procedures is not 100% effective), so that a natural pregnancy could be obtained or even use a basic assisted reproductive technique such as AI.
On the other hand, a reproductive technique that does not require the functionality of the fallopian tubes, an IVF, can be performed.
It would not be possible to perform an AI as you mentioned, since it is necessary for the egg to travel through the tubes to the uterus, where it would be fertilized and subsequently implanted.
I recommend that you go to a reproductive clinic where they can explain the advantages and disadvantages of the two options presented to you. I leave you our directory of clinics where you can find out about the best clinics in your area.
I hope I have helped you.
Best regards.