Testicular biopsy consists of a minor surgery that allows the extraction of tissue from the testicles and its observation under a microscope. The main objective of a testicular biopsy is to find sperm when they do not appear naturally in the semen expelled during ejaculation. For many men, this step represents the opportunity to be able to use their own sperm to have a child.
Regarding the procedure, the testicular biopsy can be performed by opening the skin of the scrotum or by puncturing and aspirating with a special needle. For this, local or general anesthesia is administered in the area, so the testicular biopsy does not cause pain.
Normally, a testicular biopsy does not cause serious complications. Among the most common risks associated with this intervention in men are wound infection or slight discomfort in the hours following the procedure.
Provided below is an index with the 11 points we are going to expand on in this article.
- 1.
- 1.1.
- 2.
- 3.
- 4.
- 4.1.
- 4.2.
- 5.
- 6.
- 6.1.
- 7.
- 7.1.
- 7.2.
- 7.3.
- 7.4.
- 7.5.
- 7.6.
- 8.
- 9.
- 10.
- 11.
What does it consist of?
Testicular biopsy is a superficial surgical procedure based on the removal of one or more portions of tissue through small incisions in the testicles. These incisions are sutured with stitches that fall out or are reabsorbed.
The portions of the tissue are then looked at under a microscope to detect the presence or absence of sperm. Thus, the tissue of the testicles can also be studied.
The procedure for obtaining sperm in the laboratory is very delicate. In the seminiferous tubules (tubes inside the testicle) there are spermatozoa, but also other types of cells that can make it difficult to visualize them. Therefore, this surgical test is performed by a specialist physician (urologist) supported by a biologist.
In general, it is a simple and painless technique because it is performed under anesthesia.
40% of sterility cases in couples are of male origin, either because of alterations in the quality of the semen or because of ejaculation problems.
Testicular biopsy is a relatively modern procedure that allows couples to achieve a pregnancy through IVF treatment with intracytoplasmic sperm injection (ICSI), without the need for donor sperm.
What is the purpose of a testicular biopsy?
Thanks to this surgery, it is possible to determine whether spermatogenesis (sperm production) occurs normally in the testicle.
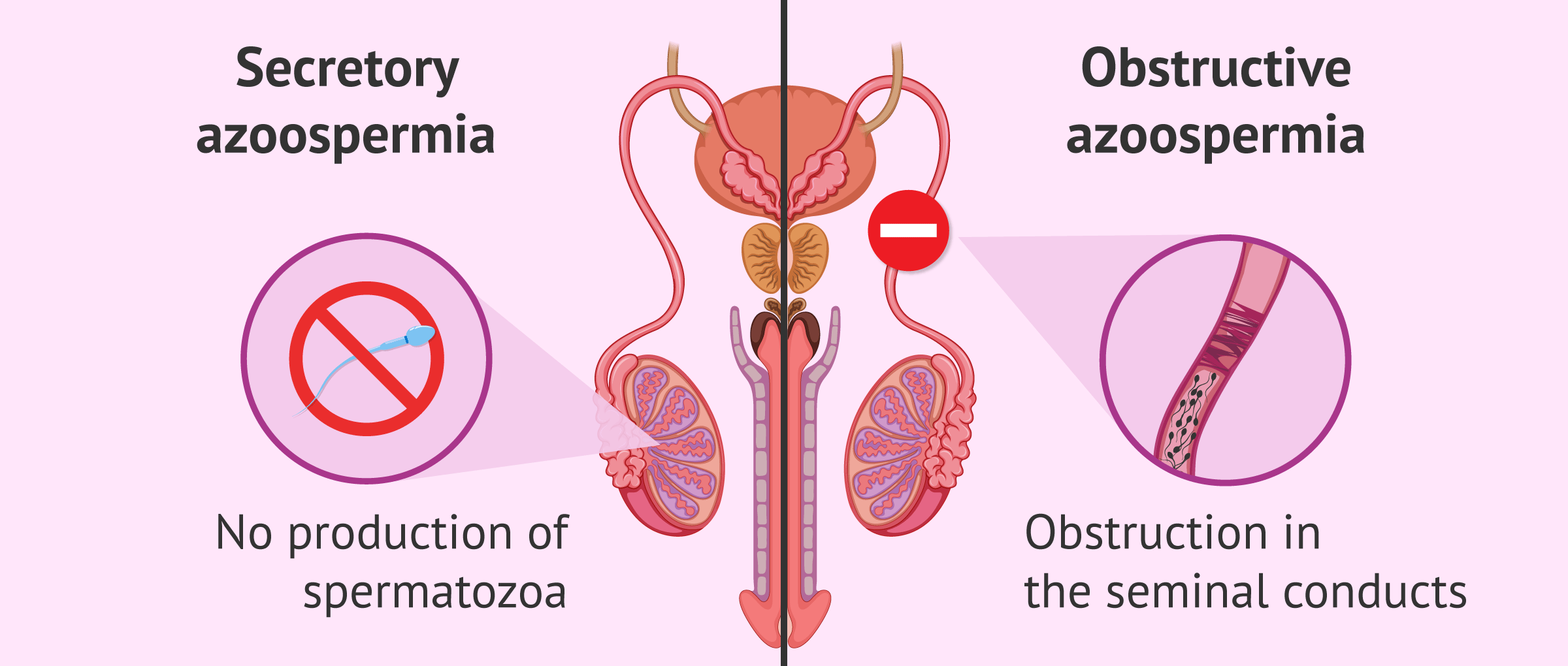
Therefore, testicular biopsy allows us to distinguish between a pathology:
- of obstructive type: if the seminal ducts that allow the semen to exit are blocked. This type of pathology is known as obstructive azoospermia.
- of secretory type: the production of spermatozoa does not exist or the spermatozoa do not finish their maturation process. That refers to the secretory azoospermia.
This diagnostic purpose allows us to say what kind of problem the patient is suffering from and to evaluate the origin of male infertility. Thus, the specialist proposes the most appropriate treatment.
Another objective of this test is the spermatozoa retrieval directly from the testicle. This is done when no sperm are found in the ejaculate. In this way, sperm are obtained to be frozen and/or used fresh later in an ICSI fertility treatment.
It should be noted that only as many sperm as eggs are needed for ICSI. For this reason, this technique can be performed with poor quality seminal samples or samples recovered from the testicle.
Assisted procreation, as any other medical treatment, requires that you rely on the professionalism of the doctors and staff of the clinic you choose. Obviously, each clinic is different. Get now your Fertility Report, which will select several clinics for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
Indications of testicular biopsy
Testicular biopsy is usually done to find the cause of male infertility when a seminogram shows abnormal results. This technique is recommended in cases of azoospermia, oligospermia, and severe alterations of seminal quality.
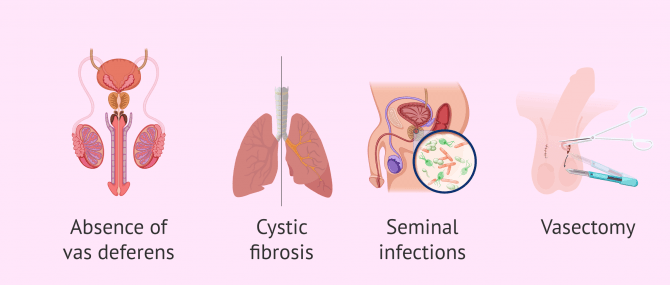
It is also indicated in cases of obstruction of the seminal duct, which have different causes:
- Absence of vas deferens.
- Cystic Fibrosis.
- Infections.
- Vasectomy.
On the other hand, a testicular biopsy can be performed in the presence of a tumor to determine its status.
Testicular biopsy should not be performed when the absence of sperm is caused by hormonal disorders or there is clear evidence of their absence in the testicles.
Types of testicular biopsies
The method of biopsy to be performed will depend on the reason for the exam. Your doctor will discuss your options.
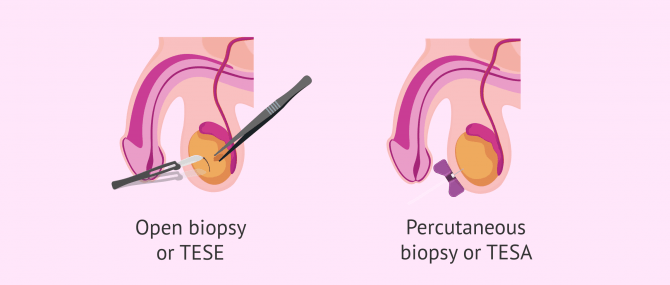
In general, there are two techniques for obtaining sperm from the testicle:
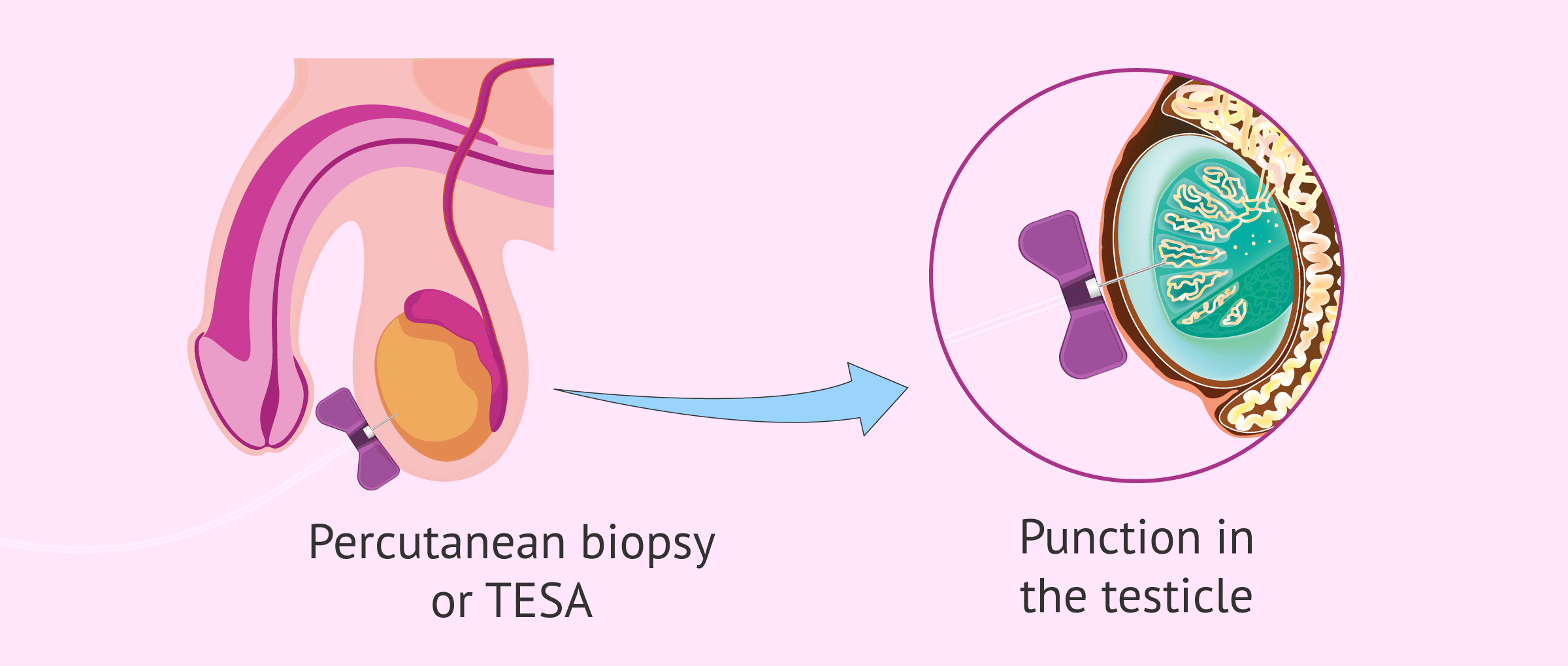
- Testicular sperm extraction (TESE), also called open biopsy, is the biopsy itself. Although TESE is indicated in patients with obstructive azoospermia, it is also applied in some situations of secretory azoospermia.
- Testicular sperm aspiration (TESA): also known as percutaneous biopsy. This method is less invasive than TESE and is useful for men who have sterility problems caused by a blockage in sperm ejaculation.
The aim of both procedures is to obtain spermatozoa for subsequent use in in vitro fertilisation (IVF) treatment. Although they have the same purpose, the decision to apply one method or the other will depend on the patient's particular situation.
It is recommended that sexual activity be avoided for 1-2 weeks after the testicular biopsy.
What is the procedure for a testicular biopsy?
Testicular biopsy does not require hospital admission since it is a simple technique. However, it is an unpleasant test for the man compared to a seminogram or blood test.
Depending on the type of testicular biopsy to be performed (TESE or TESA), the method performed is different.
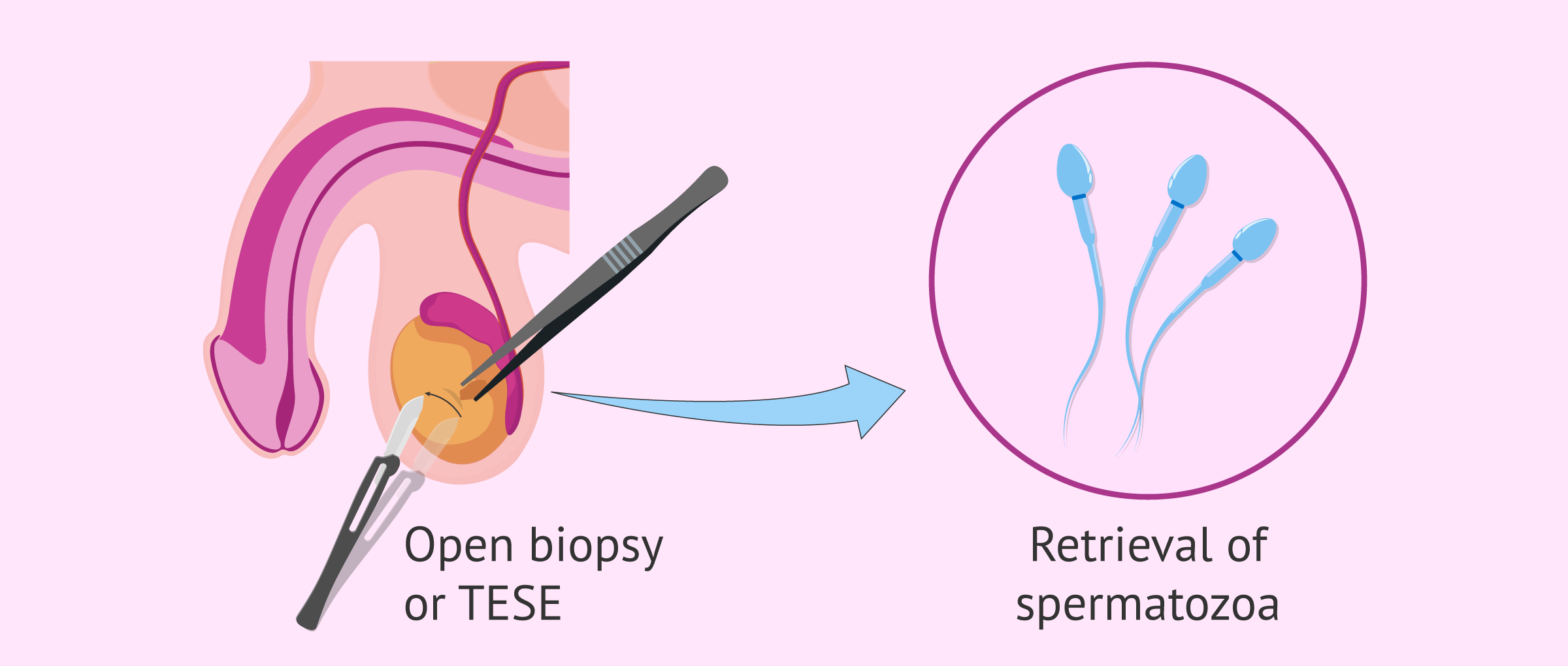
Open testicular biopsy or TESE
The surgical procedure of an open biopsy is performed under local anesthesia and sometimes combined with sedation. The duration of the procedure is approximately 15 to 20 minutes.
The process consists of removing small fragments of the testicle to be evaluated under a microscope to look for sperm. To do this, a small incision of 2-3 cm is made in the skin of the scrotum and another in the testicle. In the end, stitches are placed to close the wound and it is covered with a simple dressing. The technique is repeated on the other testicle if necessary.
The removed tissue is fractionated in the laboratory and observed under the microscope. In this way, part of the tissue is used for the recovery of viable sperm, and another part is used to establish a diagnosis of the cause of infertility.
Once the sperm are obtained, they can be frozen in liquid nitrogen at -196ºC or used directly to fertilize the woman's eggs extracted by ovarian puncture during an IVF treatment.
Percutaneous testicular biopsy or TESA
This model of testicular biopsy consists of making a puncture in the testicle with the help of a special needle attached to a syringe. This is a less aggressive methodology compared to open biopsy.
However, TESA also has several disadvantages over TESE:
- Few sperm may be obtained and the patient may have to undergo another open testicular biopsy.
- Increased likelihood of complications and side effects.
Therefore, a percutaneous biopsy is not frequently used for sperm aspiration. In these cases, sperm aspiration is usually used in the epididymis.
Complementary studies
Once the testicular tissue is obtained, the process does not end in the operating room. In addition to looking for viable sperm for in vitro fertilization, a small portion of that tissue can be sent to the laboratory for deeper medical analysis.
These additional studies are key to understanding at a cellular level why the testicle is not functioning correctly. To obtain a definitive diagnosis, the most prominent complementary analyses include:
- Histology study: is performed when the seminogram shows a concentration of spermatozoa below the limits of normality (oligozoospermia) or if there are no spermatozoa in the ejaculate (azoospermia). Here the testicular tissue and its ability to produce sperm are analyzed, as well as finding out at what point in the spermatogenesis this production is interrupted.
- Meiosis or cytogenetic study: evaluates the structure, composition and chromosome arrangement at the different stages of sperm formation. This test is performed when there are previous repeated miscarriages or low sperm mobility (asthenozoospermia). The use of a testicular biopsy for a meiotic study is quite controversial since there are no clear parameters for this analysis.
Thanks to this valuable information, the medical team can outline a much more precise strategy and offer real alternatives, avoiding the emotional toll of repeating treatments that are not going to work.
Postoperative advice after a testicular biopsy
After the intervention, the man will be able to return home on the same day as the testicular biopsy after previously spending some time under observation. It is normal to feel a slight discomfort or a feeling of heaviness in the testicular area, which disappears in a couple of days with common painkillers. For everything to heal perfectly and to have a proper recovery after the biopsy of the testicle, it is essential to follow these steps:
- Wear brief-style underwear that keeps the area supported and without movement.
- Apply some local cold (protected with a cloth) to reduce possible inflammation.
- Keep the area clean and dry, washing carefully.
- Avoid heavy exertion, lifting weights, or having sexual intercourse during the first week after the testicular biopsy.
Following these postoperative guidelines, most patients feel fully recovered in a very few days.
Complications and risks of testicular biopsy
Complications and risks associated with testicular biopsy are rare. However, since it is a surgical procedure, complications may arise from the anesthesia. In any case, these complications will be referred to as the treatment that the specialist doctor decides.
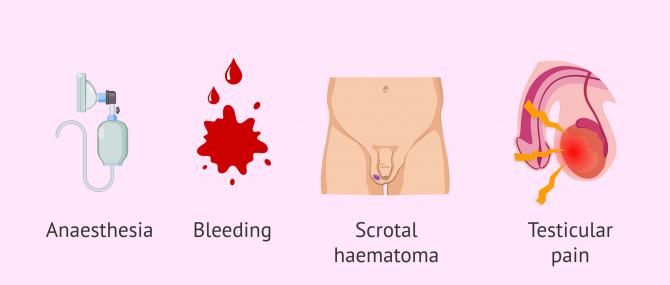
Other side effects of testicular biopsy, although uncommon, are the following:
- Bleedings.
- Wound infection.
- Bruise on the skin of the scrotum.
- Intratesticular hematoma accompanied by persistent pain of the testicles. This bruise is usually reabsorbed within a few weeks.
- Swelling of the testicle that stops with the administration of analgesics and anti-inflammatories.
On the other hand, the assisted reproduction treatment can also be canceled if no sperm are recovered in the biopsy. In this situation, the eggs retrieved in the woman's follicular puncture would be frozen, while waiting to decide whether to repeat the biopsy or opt for donor sperm.
Waiting for the results of the biopsy may create a situation of anxiety in the couple. For this reason, specialists advice to seek psychological support.
FAQs from users
Can sexual intercourse take place before testicular biopsy?
Testicular biopsy is used to obtain sperm when sperm cannot be obtained by ejaculation. It is indicated in cases of azoospermia, when sperm have been obtained without sperm in the semen sample or to achieve pregnancy after a vasectomy.
In cases of azoospermia, sperm will be retrieved if the cause is an obstruction (obstructive azoospermia). In case the problem is in sperm production, if a sperm-producing focus of the testicle is not located, it is very difficult to find sperm in the biopsy as well.
Since the seminal sample does not contain sperm (which is the reason why biopsy is usually indicated), having sexual intercourse before the biopsy will not influence the results of the procedure.
Does a testicular biopsy hurt?
No. Open testicular biopsy or TESE can be performed under local or general anesthesia. The most common method is to sedate the patient, so he or she will not notice anything.
In percutaneous biopsy or TESA, local anesthesia is usually used, so the patient may feel some pressure but no pain.
Is sexual intercourse possible after a testicular biopsy?
A period of sexual abstinence of 1 to 2 weeks is recommended. After this time, the patient can return to normal sexual activity.
Can sperm obtained from a testicular biopsy be used to perform artificial insemination?
No. The amount of sperm obtained in a testicular biopsy is very small, so artificial insemination is not possible.
In these cases, the recommended technique is ICSI.
How much does a testicular biopsy cost?
The price of a testicular biopsy ranges from approximately 2,500-6,000 dollars, depending on the center where it is performed and the method used.
Does a testicular biopsy always yield spermatozoa?
No. The probability of finding spermatozoa with a testicular biopsy is high, but it is not 100%. The cause of the absence of sperm in the ejaculate is important to predict the probability of success of the technique.
Suggested for you
If you wish to obtain information about the normal values of a seminogram in man, I encourage you to click on the following link: Sperm Test Results Explained- Interpretation & Normal Values.
Azoospermia is one of the leading causes of testicular biopsy. Therefore, I invite you to continue reading this article: Azoospermia- Can a Man Actually Have Zero Sperm Count?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Amer MK, Ahmed AR, Hamid AAA, GamalEl Din SF. Factors determining the sperm retrieval rate in fresh versus salvage micro-TESE: a comparative cohort study. Int Urol Nephrol. 2019 Mar;51(3):401-408. doi: 10.1007/s11255-019-02086-5 (View)
Bouker A, Halouani L, Kharouf M, Latrous H, Makni M, Marrakchi O, Zouari R, Fourati S. Step-by-step loupes-mTESE in non-obstructive azoospermic men, a retrospective study. Basic Clin Androl. 2019 Jul 15;29:11. doi: 10.1186/s12610-019-0091-9 (View)
Cisneros J.B, Navarro C, Castro A.E, Vásquez C, Bonilla M.A, Navas T.P. Microdisección testicular para la obtención de espermatozoides (m-TESE): nueva modalidad terapéutica en pacientes con azoospermia no obstructiva y niveles elevados de hormona folículo estimulante. Reporte de un caso. Revista Mexicana de Urología 2014. Vol 74 (6) 375-378.
Mehmood S, Aldaweesh S, Junejo NN, Altaweel WM, Kattan SA, Alhathal N. Microdissection testicular sperm extraction: Overall results and impact of preoperative testosterone level on sperm retrieval rate in patients with nonobstructive azoospermia. Urol Ann. 2019 Jul-Sep;11(3):287-293. doi: 10.4103/UA.UA_36_18 (View)
Pilatz A, Kilb J, Kaplan H, Fietz D, Hossain H, Schüttler CG, Diemer T, Bergmann M, Domann E, Weidner W, Wagenlehner F, Schuppe HC.High prevalence of urogenital infection/inflammation in patients with azoospermia does not impede surgical sperm retrieval. Andrologia. 2019 Aug 27:e13401. doi: 10.1111/and.13401 (View)
Taitson PF, Mourthé A Filho, Radaelli MRM. Testicular sperm extraction in men with sertoli cell-only testicular histology - 1680 cases. JBRA Assist Reprod. 2019 Aug 22;23(3):246-249. doi: 10.5935/1518-0557.20190023 (View)
FAQs from users: 'Can sexual intercourse take place before testicular biopsy?', 'How many sperm need to be obtained in a testicular biopsy?', 'Does a testicular biopsy hurt?', 'Is sexual intercourse possible after a testicular biopsy?', 'Can sperm obtained from a testicular biopsy be used to perform artificial insemination?', 'How much does a testicular biopsy cost?' and 'Does a testicular biopsy always yield spermatozoa?'.





My husband will get a testicular biopsy performed. How much is this treatment in the u.k?
Hi Caroline,
a testicular biopsy will cost around £1,900.00. However, the total cost depends on the clinic and if complementary techniques, such as sperm freezing, are required.
Hope this helps,
Best
Hello, I would like to know how many days of sexual abstinence you have to keep when you are going to have a testicular biopsy. I have a varicocele and hormonal and genetic problems have been ruled out. Also, I would like to know if I have to prepare in any way, that is, if I have to wear panties or briefs and days of abstinence. Thank you very much.
Hi, my boyfriend had his vasectomy done ten years ago. If he had the surgery again, would it be effective in getting me pregnant? How much does a reconstruction operation cost? I’m waiting for your answer. Thank you.
Hi, this is Thomas. I went through vasectomy two years ago, but now I’m with another person and we want to become parents. The thing is, I’ve been told I should undergo testicular biopsy in order to check if I have any level of sperm concentration on my testes to be able to make my partner pregnant. I would appreciate it if someone that has gone through this whole process could tell me about it. Thanks.