Pregnancy is a new physiological state in a woman that does not have to cause any problems for her health and that of the future baby she is expecting. However, it is very important to monitor the entire gestation period in order to detect possible alterations and prevent them in time.
Since the generalization of medical control of pregnancy and the introduction of hospital delivery, perinatal mortality has declined significantly in industrialized societies, being much lower than maternal-fetal mortality in underdeveloped or developing countries.
Therefore, it is very important that all pregnant women have an early, periodic, complete and quality prenatal check-up, according to the Spanish Society of Gynecology and Obstetrics (SEGO).
Provided below is an index with the 9 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 4.
- 4.1.
- 4.2.
- 5.
- 5.1.
- 5.2.
- 5.3.
- 5.4.
- 6.
- 7.
- 8.
- 9.
First visit
As soon as a woman discovers that she is pregnant, she should make an appointment with her gynecologist to begin prenatal care.
At the first visit, called the intake visit, the patient's medical history will be opened, which should include all this information:
- Family and partner history as detailed as possible.
- Medical history and possible pathologies that may be aggravated.
- Obstetric history: previous pregnancies, miscarriages, termination of pregnancy, childbirth, etc.
- Menstrual cycle characteristics, previous surgeries, contraceptive use, etc.
- Date of last menstrual period (LMP) to calculate weeks of pregnancy.
The gynecologist will then perform a physical examination of the patient, which is based on palpation of the genitals and breasts, measurement of weight and height to calculate the BMI, blood pressure measurement, etc.
Other possible complementary tests include the following:
- Coombs test: blood group compatibility of mother and fetus
- Urine analysis: leukocytes, glucose, albumin, etc.
- Blood tests: hemogram, blood glucose, TSH, cholesterol, iron, etc.
- Serologies: rubella, syphilis, toxoplasmosis, hepatitis B and HIV.
- Cytology
Based on all the results obtained, the gynecologist will give the woman all the nutritional recommendations and care necessary for the correct development of the pregnancy.
First trimester of pregnancy
At all subsequent pregnancy check-ups, the gynecologist will perform a physical examination and take weight and blood pressure measurements.
The first-trimester ultrasound, which in many cases is the woman's first ultrasound, should be done between 11 and 13 weeks of gestation, and is usually done vaginally. The objectives of this ultrasound are as follows:
- Identify the number of embryos and gestational sacs.
- Listen to the heartbeat of the embryo.
- Take measurements of the embryo to estimate the weeks of pregnancy together with the FUR.
- Measure the nuchal translucency.
- Observe the morphology of the embryo.
- Observe the uterus and adjoining structures.
Next, we will discuss the diagnostic tests that can be done to check that the fetus is healthy and has no chromosomal abnormalities.
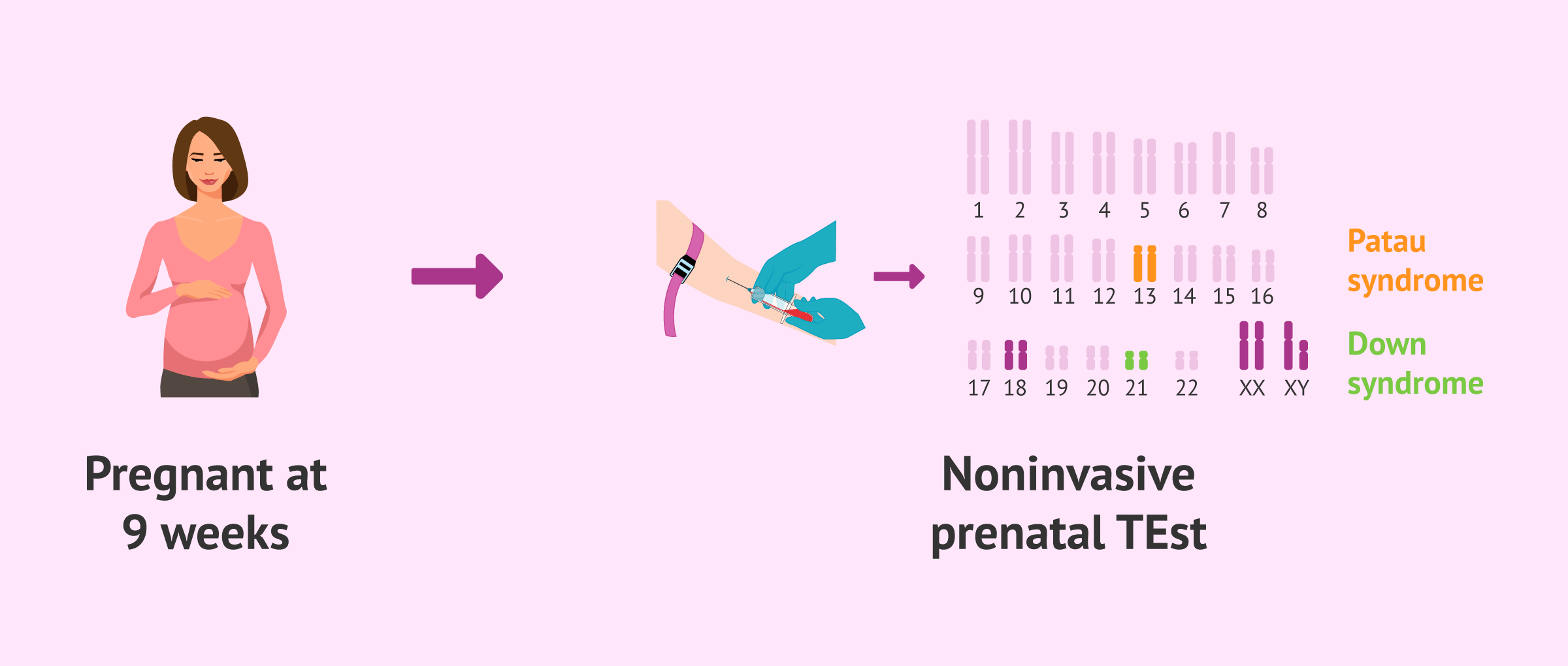
Non-invasive prenatal testing
This test consists of analyzing the DNA of the fetus obtained from a simple blood sample from the mother. It can be performed from week 9 of pregnancy and has multiple advantages.
The genetic alterations that can be detected in fetal DNA are those affecting the number of chromosomes: Down syndrome, Edwards' syndrome, Patau's syndrome, and those related to the sex chromosomes.
This non-invasive test is being increasingly used due to its simplicity and lack of risk for both the fetus and the mother. In addition, the number of invasive tests performed, such as amniocentesis, has been greatly reduced.
For more information on fetal DNA blood testing, you can continue reading here: Non-invasive prenatal test in maternal blood.
However, it should be noted that fetal DNA testing in maternal blood is not covered by Social Security or private health insurance. Therefore, women who wish to have it done will have to pay the price.
Triple screening
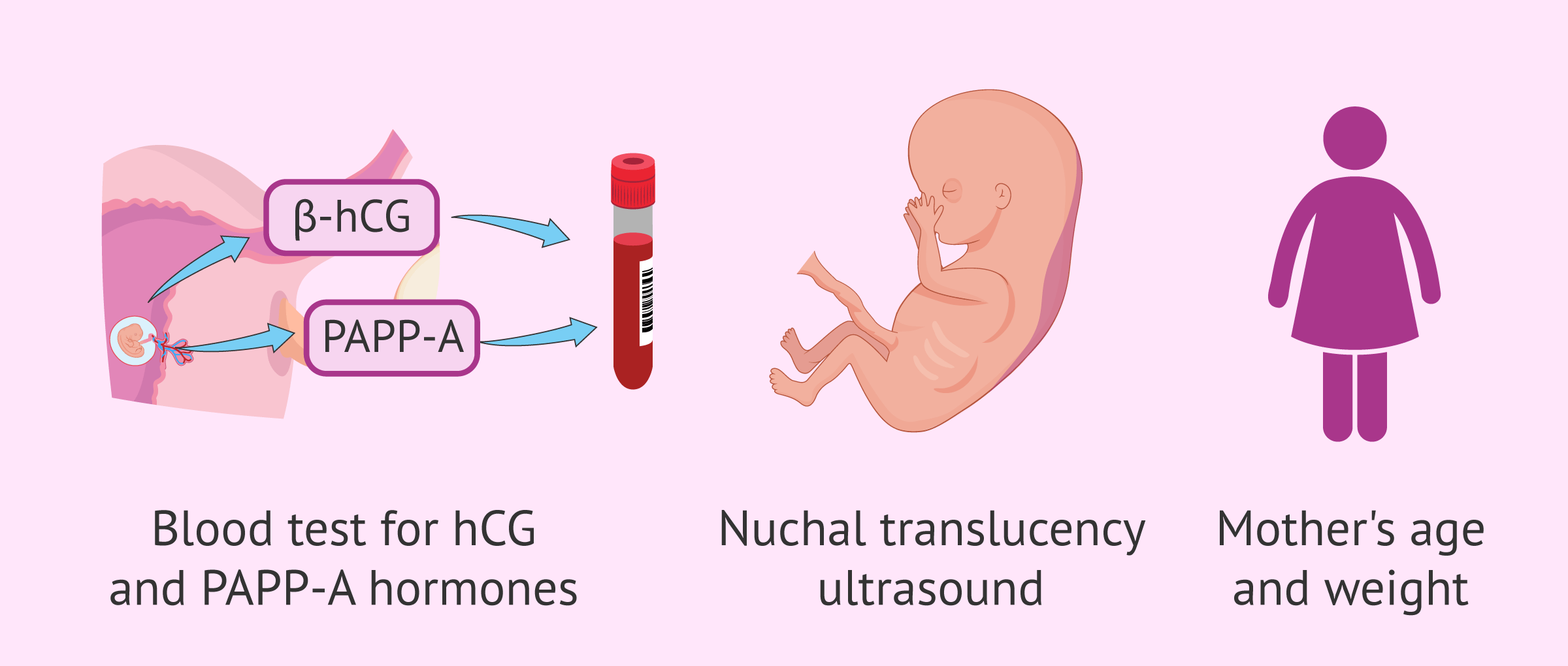
First trimester combined screening, also known as triple screening, is a biochemical test that is now routinely performed on all pregnant women to determine the risk of congenital abnormalities in the baby.
This estimate is made from the following parameters that the gynecologist obtains from the first-trimester blood test and ultrasound:
- The nuchal fold or nuchal translucency
- Biochemical markers: pregnancy-associated placental protein (PAPP-A) and free beta-hCG.
- Mother's age, weight, number of fetuses, etc.
The values obtained are compared with tables made according to a pattern of normality in relation to the week of pregnancy.
Depending on the risk index (RI) obtained in the triple screening, it will be necessary or not to perform other invasive diagnostic tests in order to rule out chromosomal alterations.
- IR ≥ 1 in 50
- there is a risk of chromosomopathies. An amniocentesis or chorionic villus sampling will be necessary to confirm the result.
- IR 1 in 50 - 1 in 250
- medium risk. It is recommended to test maternal blood for fetal DNA and, depending on the result, to perform invasive or non-invasive prenatal testing.
- IR < 1 in 250
- the risk is very low.
Once the triple screening test is passed and the pregnancy is over 12 weeks, the risk of miscarriage is much lower and the woman feels more relaxed.
Second trimester of pregnancy
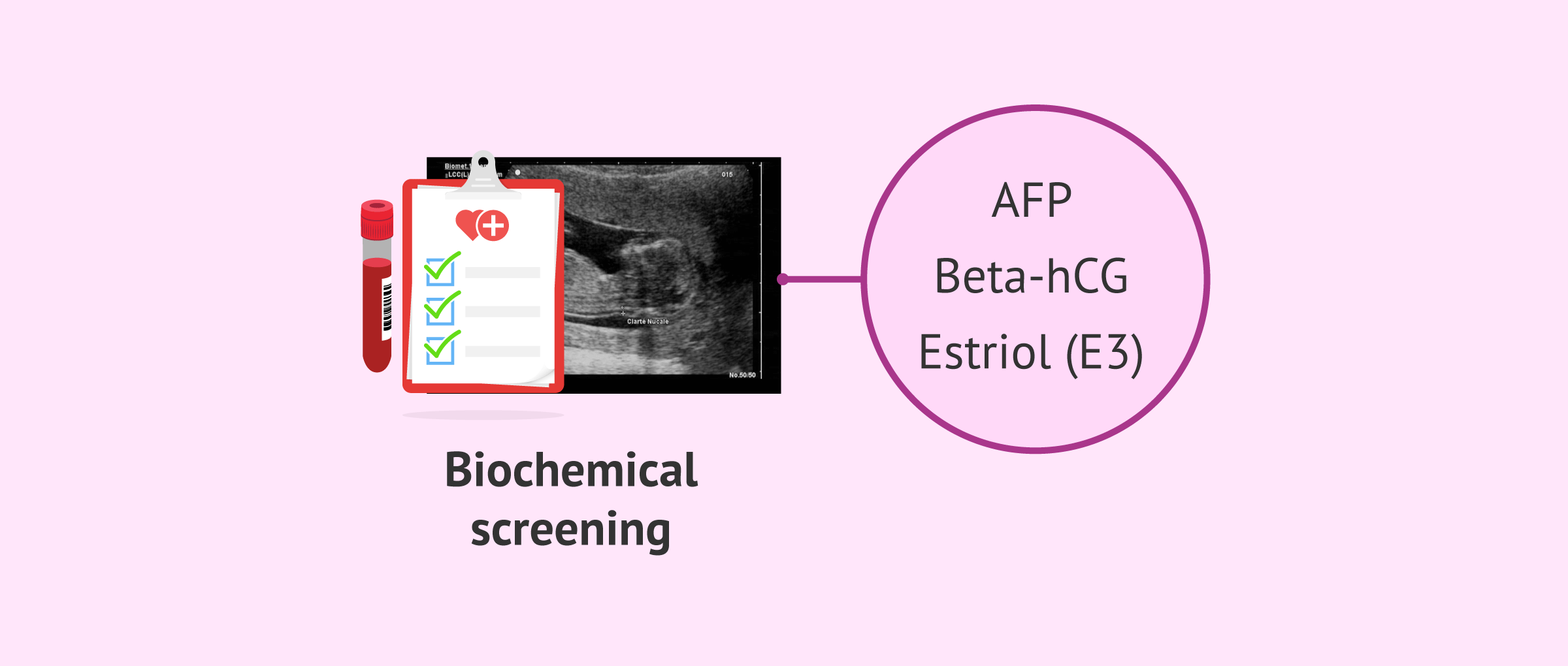
From the 15th week of pregnancy, alpha-fetoprotein (AFP), beta-hCG, and estriol (E3) values are determined in maternal blood for double or triple biochemical screening.
These parameters are indicators of possible structural abnormalities in the fetus, especially neural tube closure defects:
- High AFP values
- indicate multiple pregnancy or presence of spina bifida or anencephaly in the fetus.
- Low AFP values
- are indicative of trisomies on chromosomes 21 or 18.
- Low free or unconjugated estriol values
- the presence of alterations in chromosomes 13, 18 or 21 may be suspected.
To generalize the units of these measurements and avoid variations according to gestational age, they are measured in MoM (multiples of the median). A normal result is considered when the values are between 0.5 and 2.5 MoM. The normal value is 1 MoM, so the greater the distance from this value, the worse the result.
Problems in fetal development are suspected when the AFP and beta-hCG values are less than 0.4 or greater than 2.5, and the estriol value is less than 0.5.
Morphological ultrasound
The second trimester ultrasound, also known as a morphological ultrasound, should be performed between 18 and 22 weeks of pregnancy.
It is one of the most important ultrasounds of the entire pregnancy and its objectives are the following:
- Perform a complete morphological examination of the fetus.
- Determine male or female sex.
- Perform biometry: measure the head, abdomen and femur, etc. to check for proper fetal development.
- Study of the placenta, umbilical cord and amniotic fluid.
- Study of the heart and circulation through the uterine arteries.
With the results of this ultrasound and biochemical screening, the gynecologist will determine the need for further prenatal testing such as those discussed below.
Chorionic biopsy
Chorionic villus sampling consists of obtaining chorionic villi from the placenta vaginally or transabdominally in order to karyotype the fetal cells.
It is an invasive prenatal test but serves to confirm the diagnosis of biochemical screening or fetal DNA testing. It has also been possible to identify false positives or negatives from the above tests.
The advantage of chorion biopsy is that it can be performed before amniocentesis, between 10 and 14 weeks of gestation. However, it is a more difficult technique that involves more risks.
For more information about this prenatal diagnostic test, you can continue reading here: What is chorionic villus sampling?
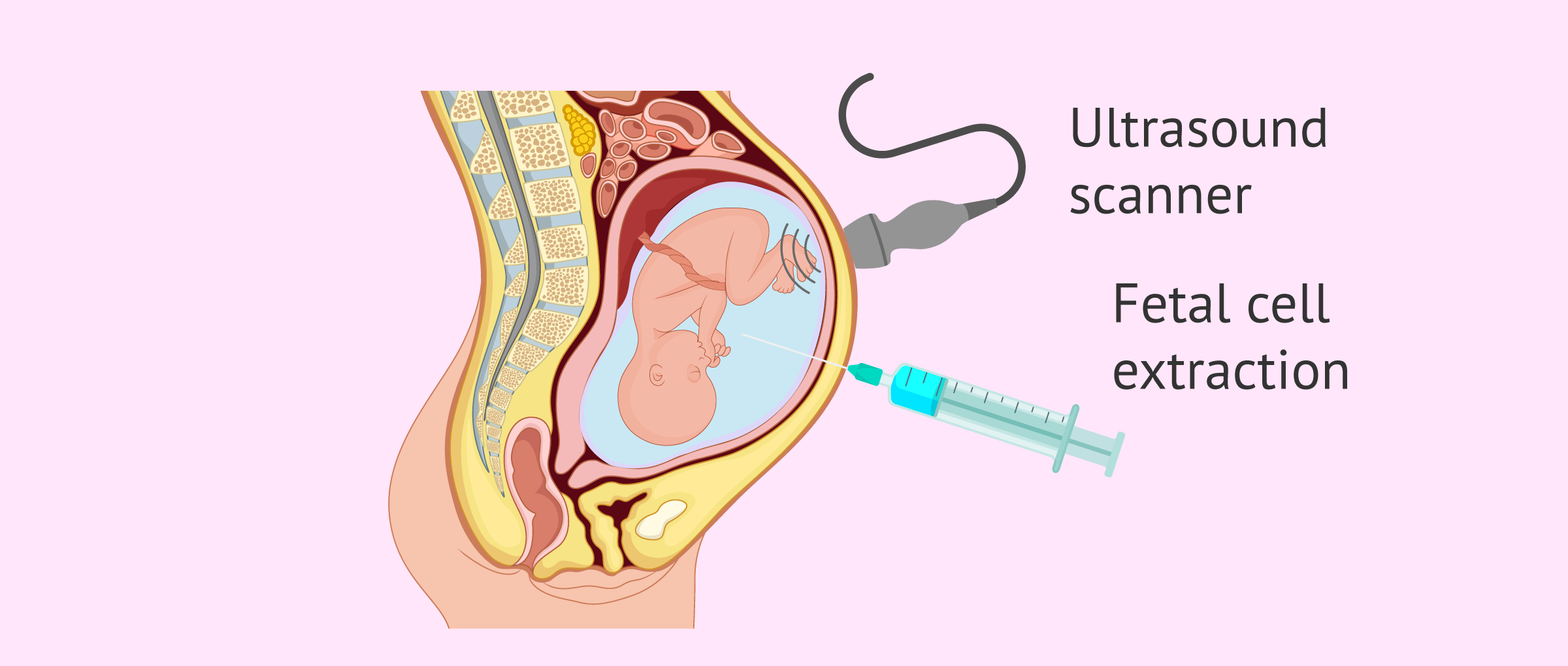
Amniocentesis
Amniocentesis is an invasive prenatal test that involves the extraction of a sample of amniotic fluid through the mother's abdominal wall using a fine needle and ultrasound monitoring.
The amniotic fluid contains fetal cells, which can be analyzed as well during chorionic biopsy to identify possible genetic alterations.
Amniocentesis is generally performed between 15 and 20 weeks of gestation in women of advanced maternal age, with a history of children with chromosomopathies, at risk of transmitting inherited genetic diseases, or when the triple screening values have been altered.
If you are interested in reading more about this topic, we recommend the following post: What is amniocentesis?
Third trimester of pregnancy
Between 34 and 36 weeks of pregnancy, the woman will need to have a third trimester ultrasound to check the following parameters:
- Identify fetal vitality and statics.
- Check the growth of the fetus and its position.
- Determine the volume of amniotic fluid and diagnose possible alterations.
- Visualize the placenta and check its location.
- Observe the umbilical cord and check that it does not encircle the baby's neck.
This ultrasound can provide information regarding the delivery: when it will be, how it will be, the precautions to be taken by the woman, etc.
O'Sullivan test
The O'Sullivan test is a test to determine the blood glucose level and diagnose whether a woman has gestational diabetes.
It is done in all pregnant women between 24 and 28 weeks of gestation, although if there are risk factors it should be done earlier.
In case of a positive result (glucose ≥ 140 mg/dl or 7.8 mmol/L), the woman will have to have a second glucose overload test to confirm the diagnosis.
You can read more about this topic here: What is gestational diabetes?
Fetal monitoring
Three to four weeks prior to the due date, the woman will need to have weekly visits to check fetal well-being.
This is known as antepartum fetal monitoring(AFM) and consists of recording the fetal heartbeat, and the rhythm and intensity of the mother's contractions.
Once 40 weeks gestation has been reached if labor does not move naturally, the physician will indicate whether it is necessary to induce labor or schedule a cesarean section at the most appropriate time.
FAQs from users
How many times is it advisable to visit a prenatal visit during a pregnancy?
According to the Spanish Society of Gynecology and Obstetrics (SEGO), women with a pregnancy that progresses without complications should go to the prenatal consultation with the following periodicity:
- Up to week 36: every 4-6 weeks.
- From week 37 to week 40: every 1-2 weeks.
- After week 40: 1 to 3 times a week.
What is combined first-trimester screening?
The triple screening does not represent a diagnosis but is a statistical test based on biochemical markers present in maternal blood that establishes a risk index.
It does not provide information on the actual condition of the baby but is based on a simple calculation of probabilities.
Read more
What tests can be performed during pregnancy to detect abnormalities in the fetus?
The most important tests to know that the pregnancy is progressing correctly and that the fetus is in good health are, firstly, the 12-week ultrasound and the triple screening, and secondly, the 20-week morphological ultrasound.
It is also important to highlight amniocentesis in women who present risk factors, since it is the only test that ensures 100% that the fetus has no genetic alterations.
Is it necessary to have any vaccinations during pregnancy?
Only in the event that the gynecologist deems it convenient for the woman to be immunized against a disease for which she has not been previously vaccinated. It should be emphasized that only vaccines with inactivated viruses, bacterial vaccines, and toxoids, such as diphtheria, tetanus, cholera, meningococcus, pneumococcus, hepatitis, rabies, poliomyelitis, etc., can be administered during pregnancy.
Influenza vaccine should also be offered to all pregnant women during the periods of the year when they are most susceptible to infection.
Recommended readings
In the following article, you will find more information about all the ultrasounds performed during pregnancy: Fetal ultrasound in the first, second, and third trimester.
Once 40 weeks of gestation have passed, the long-awaited moment of giving birth arrives. If you want to know all the details about childbirth, you can access the following post: What is childbirth like?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Control prenatal del embarazo normal. PROTOCOLOS SEGO. Progresos de Obstetricia y Ginecología 2011;54(6): 330-349 (View)
Capitán Jurado M, Cabrera Vélez R. Atención preconcepcional. La consulta preconcepcional en Atención Primaria. Evaluación de la futura gestante 2001; 11: 207-215
J M Ellings, R B Newman, N A Bowers. Prenatal care and multiple pregnancy. J Obstet Gynecol Neonatal Nurs. Jul-Aug 1998;27(4):457-65 (View)
Nola Holness. High-Risk Pregnancy. Nurs Clin North Am. 2018 Jun;53(2):241-251. doi: 10.1016/j.cnur.2018.01.010 (View)
FAQs from users: 'How many times is it advisable to visit a prenatal visit during a pregnancy?', 'What is combined first-trimester screening?', 'What tests can be performed during pregnancy to detect abnormalities in the fetus?' and 'Is it necessary to have any vaccinations during pregnancy?'.
Authors and contributors
More information about Cristina Algarra Goosman










Hi everyone!
Cytogenetic studies are only performed under the conditions you mention here? And what about if I want to undergo it but neither of that situations match with mine? I’d like to do so just as a prevention measure, is it possible or not?
Thank you very much
Dear Rose,
Cytogenetic studies entail many risks; therefore, if you’re not carrying a high risk pregnancy, there’s no need to perform any of them, because chances for miscarriage are higher.
Best wishes.