The procedure of egg donation is an alternative option to IVF with own eggs. In this case, a woman becomes an egg donor for an infertile intended mother that cannot use her own oocytes. The success rates of donor-egg IVF are lower in women over 40. The donor baby will not have the genes of the birth mother but those of the donor, i.e. the biological mother.
The pros and cons of having a baby with donor eggs, whether fresh or frozen, should be weighed before making a hasty decision. Factors such as the cost, which is higher than a normal IVF procedure, and the risks involved are of utmost importance. The following is a comprehensive guide to this fertility option.
Provided below is an index with the 10 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 2.4.
- 3.
- 4.
- 5.
- 6.
- 6.1.
- 6.2.
- 6.3.
- 6.4.
- 6.5.
- 6.6.
- 6.7.
- 6.8.
- 6.9.
- 6.10.
- 6.11.
- 6.12.
- 6.13.
- 6.14.
- 6.15.
- 6.16.
- 6.17.
- 6.18.
- 6.19.
- 6.20.
- 6.21.
- 7.
- 8.
- 9.
- 10.
Definition of 'egg donation'
Egg donation is an option for infertile women willing to have a baby. It involves the presence of two main parties: the recipient or intended mother, and the egg donor. When using donated oocytes, in vitro fertilization (IVF) is the only treatment of choice.
Broadly speaking, the following are the main pros and cons of egg donation:
Pros: the woman can go through all the stages of pregnancy, have a baby, and give birth as if it was a natural pregnancy. Also, the baby has a genetic connection to the male partner.
Cons: the first one is that the child will not have any biological connection to the mother.
Secondly, egg donation cycles are expensive, although it depends on the country.
There exist many synonyms used to refer to it, including egg cell donation, oocyte donation, ovum donation, ova donation or ovary donation. It is also commonly described as selling eggs.
The history of this treatment goes back to 1984 and was especially aimed at those women who have fertility problems due to early menopause, surgery for ovarian cysts, or malignant diseases, and until then saw themselves with the impossibility of becoming pregnant.
Who is a good candidate?
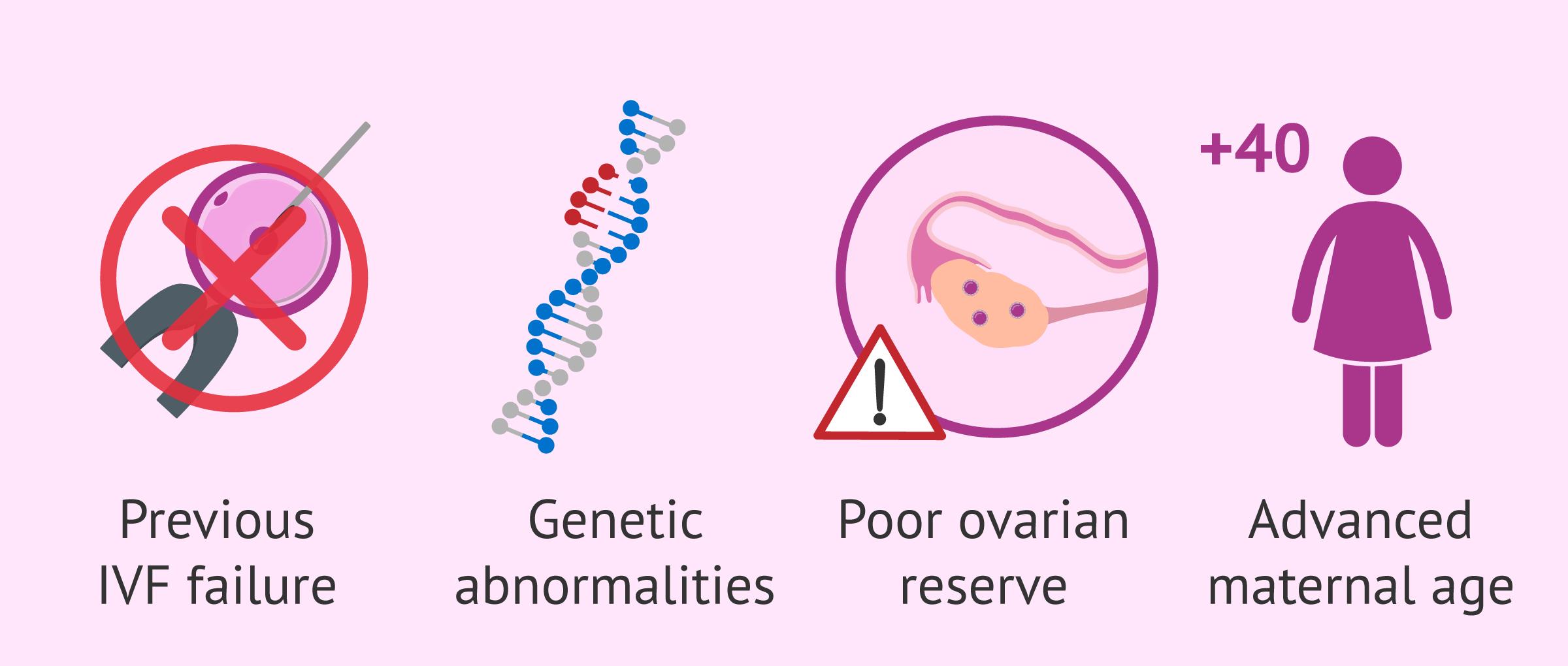
The use of donor eggs is especially indicated for women who find themselves in any of the following situations:
Previous IVF failure with own eggs: poor response to ovarian stimulation drugs, low egg and/or embryo quality, fertilization and/or implantation failure, or recurrent miscarriage are the most common reasons why a woman might not be able to get pregnant via IVF.
Women with a genetic alteration that is likely to be inherited by offspring, and is not detectable by means of preimplantation genetic diagnosis (PGD)
Poor ovarian reserve or absence of ovarian function: either due to primary ovarian insufficiency, premature ovarian failure, menopause, or surgery in the ovaries.
Women of advanced maternal age, even those who already have a biological child, often consider using donor eggs, especially those over 40 years old. From this age onwards, chromosomal alterations in the fetus and are more likely to appear. Also, the miscarriage rate increases at this point.
As a matter of fact, advances maternal age is the most frequent cause among patients who move to donor eggs.
As a woman ages, the quality of her eggs becomes poorer, and her ovarian reserve keeps on diminishing. Today, the phenomenon known as delayed motherhood is a major reason leading to an increase in the demand for IVF with donor eggs among women over 35-40.
In these cases, the chances of getting pregnant with own eggs are very low. For this reason, donated eggs might be the reproductive solution for these women to have the opportunity to become mothers.
The eggs from a donor can be used exclusively for the IVF cycle of a single recipient. However, in order to reduce the overall cost of the treatment, recipients choose egg sharing or shared egg donation, an option by which, as the name suggests, the oocytes collected from a single donor are used by two recipients.
Collecting the eggs from the donor
Donor eggs are obtained by follicle puncture or ovum pick-up (OPU), a transvaginal, ultrasound-guided surgical procedure that is done under sedation.
It involves the aspiration of the fluid from the follicles in the ovaries, which is where we will find the oocytes that are about to be harvested.
When this fluid is taken to the laboratory, the eggs contained within are aspirated and kept under optimal culture conditions up until in vitro fertilization (IVF) is done, if it is a fresh cycle, or frozen for later use.
Fertilization and embryo culture
Only the mature eggs will be fertilized at the laboratory. It can be done either by means of conventional IVF or via Intracytoplasmic Sperm Injection (ICSI), being the latter the most commonly used in these cases.
For fertilization, either sperm from the husband or from a sperm donor can be used. In case the latter is the option of choice, the treatment is known as double-donor IVF.
Embryos are obtained with IVF, and then cultured under conditions that promote their optimal development. Then, their evolution is monitored up until the day of the embryo transfer.
This close and thorough follow-up allows the specialist to select only the best embryos for the transfer, that is, those with the highest implantation potential.
Embryo transfer
Once the donor's eggs are retrieved, your partner or sperm donor has to provide a semen sample on the day of the ovum pick-up, so that the eggs are inseminated for the creation of human embryos.
The embryos are left in culture until they reach the proper stage for transfer, usually on day 3. That is the moment when recipients have to return to the clinic for transfer to the uterus.
Patients have to decide how many embryos to transfer. Although experts typically recommend single embryo transfers (SETs) to reduce the chances of multiple births, it is a topic for discussion with the doctor.
Once the endometrium acquires the ideal thickness, that is, trilaminar appearance and an 8 mm lining, the embryos will be transferred and their implantation awaited.
Embryo transfer (ET) is a simple, painless procedure after which the only thing left to do is waiting for embryo implantation. In other words, pregnancy is what every woman expects after performing an ET.
Pregnancy test and fetal monitoring
A woman can find out whether she is pregnant within 10 days by means of a quantitative beta-hCG blood test. For the result of this test to be accurate, recipients should wait at least 14 days or more after fertilization.
Should you get a positive result, the first ultrasound scan will be scheduled. This is the moment when you will be able to hear the fetal heart rate, and find out whether it is a singleton or a multiple pregnancies.
Success rates
Donor eggs are from the highest quality since they have been donated by young, healthy women who do not suffer from any fertility problem. To be accepted as donors, they must undergo a series of thorough medical tests to ensure their optimum state of health.
Bearing this in mind, it is only logical that IVF cycles using donor eggs usually present higher success rates than those cycles that are performed using the patient’s own eggs.
The following statistical data should be taken into account when deciding to use donor eggs:
Recipient's age: Women over 40 have lower implantation rates, live birth rates, and clinical pregnancy rates. Subsequently, the miscarriage rate is higher.
Uterine receptivity: It declines with advanced maternal age, especially if there is history of pathological conditions in the uterus such as myomas or polyps.
Hypertension: Along with other systemic disorders, it is more common in older women, something that might contribute to reduce the implantation potential.
Chances of getting pregnant with donor eggs may vary depending on other factors such as the recipient's anatomy of the uterus, using frozen versus fresh eggs, the ages of the donor and the recipient, what is causing infertility on the recipient, etc.
If you want to read further information about the success rates, see also: Pregnancy success rates with donor eggs.
Risks and psychological effects
The number of side effects recipients may experience during and after undergoing an IVF cycle with donor eggs is considerably lower than that expected for donors.
Since recipients do not undergo ovarian stimulation or egg retrieval, they are not exposed to the risks of these procedures, such as the ovarian hyperstimulation syndrome (OHSS).
Having a multiple pregnancy is the principal risk of egg donation for the recipient. This may occur when multiple embryo transfers are carried out, because the fact that donors are young women increases the pregnancy success rate.
Experts do recommend to limit the number of embryos to transfer, generally to no more than 2 or 3 for day 2-3 transfers. If the embryo is transferred on day 5 (blastocyst stage), a single or two embryo transfer.
Using donor eggs means the intended mother has to say "no" to her own DNA. For some intended parents, coping with the idea that they will not share their genetic load with that of their children might not be easy to accept. For this reason, many patients need psychological support before, during and even after the process in order to deal with it.
Those who decide to become parents via egg donation should be sure what is the meaning of being a mother. In this sense, motherhood is defined as the desire to see the birth of your child, as well as bringing him up, educating and taking care of him, putting aside the genetic load.
Another aspect to keep in mind is that it is not all about genetics. Even though the child might not be genetically related to the recipient of donor eggs, as they do not share the same genetic information, the baby is going to be influenced by the epigenetic changes that take place in her the uterine lining.
Interview with Dr. Maria Arqué
In this video, fertility specialist Dr. Maria Arqué talks about the steps and requirements of Egg donation IVF.
FAQs from users
When is egg donation required?
IVF with egg donation is not usually the first option when a woman or couple comes to a fertility clinic, as patients generally prefer to try to achieve pregnancy with their own gametes first. However, the situations in which egg donation is clearly indicated are the following:
- Patients with no ovarian function, whether due to premature ovarian insufficiency, absence of ovaries, menopause, etc.
- Patients who have ovarian function but cannot use their own eggs due to transmissible genetic abnormalities.
Egg donation may also be indicated after repeated failures in previous IVF cycles and when the woman is over 40 years old. This last indication is quite common, since egg quality decreases with age. As a result, the likelihood increases that the embryos obtained will have chromosomal abnormalities that compromise their viability and may lead to miscarriage or to the birth of a baby with conditions such as Down syndrome.
How does Donor egg IVF work?
The first step for IVF with egg donation depends on the couple, and in many cases, it is a difficult decision. Once the initiative is taken, patients should visit a trustworthy center to begin the entire treatment.
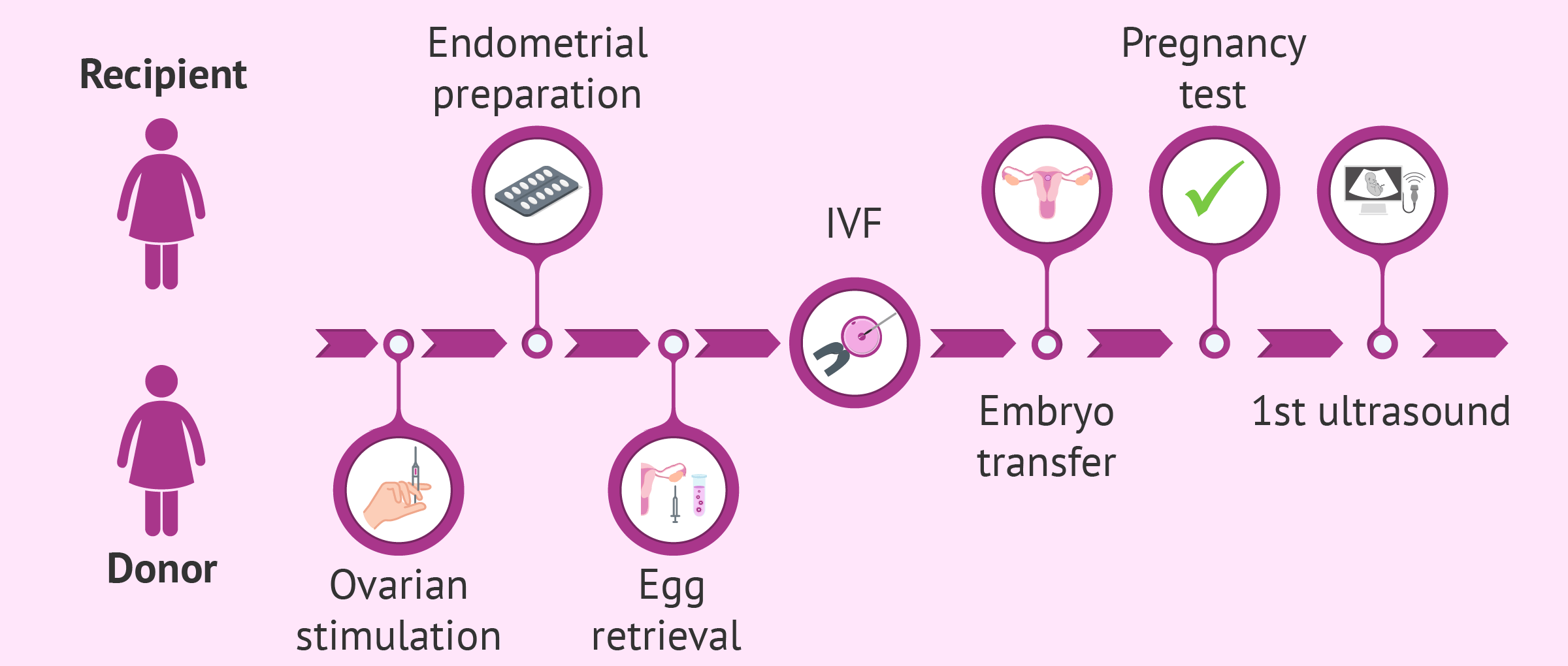
The professional at the center will be in charge of selecting the most suitable egg donor, stimulating the ovaries of the egg donor, preparing the endometrium of the recipient woman to whom the transfer of the embryos generated in the laboratory and the transfer itself will be made.
Read more
How many IVF cycles should you do before using donor eggs?
This is an extremely difficult question to answer because Fertility is a physical, emotional, and financial investment. Unless a woman is in menopause, one can never definitively provide a 0% chance for pregnancy using her eggs. However, as a woman ages, particularly above age 39 along with very poor ovarian age testing (ultra low AMH and/or elevated FSH), the prognosis for success with IVF becomes very poor.
So, there is no absolute number of IVF cycles to recommend undergoing before moving to egg donation. Nevertheless, one should consider egg donation if her IVF cycle was cancelled due to a poor response or a low number of eggs were retrieved despite a high dose of stimulation with poor embryo development.
What are the risks of egg donation?
Many donors, before getting involved in the process of oocyte donation, are afraid of the consequences that this technique may have, since it is believed to be a dangerous procedure that can even cause cancer.
However, oocyte donation is a safe process with very few side effects, of which the donor is informed before starting it in any clinic. One of them is ovarian hyperstimulation syndrome, which is increasingly rare.
In the following link there is more detailed information about this: Health risks and side effects for donors.
Donor-egg IVF vs. adoption, which one is better?
Both donor assistance and adoption offer the pleasures of parenting, so it is up to you. Prospective parents should focus on long-term aspects such as how this decision could affect their family life.
If I use donor eggs, will the baby look like me?
When matching an egg donor to a recipient, fertility clinics take into account that there is compatibility between them and that they share as many phenotype and immunological characteristics as possible. So, theoretically, yes, a baby conceived with donor eggs is likely to look like the birth mother.
However, it is important to note that the biological mother of the baby will be the egg donor, so in terms of genetic inheritance, the answer to this questions is no, the baby will not look like the recipient, since he or she does not share the genetic load with her.
Does a donor egg have my DNA?
No, donated eggs contain the DNA of the donor. The fact that it is later fertilized in the laboratory and transferred to the recipient's uterus does not modify the original genetic code of the egg. The embryo, therefore, contains the donor's genetic material.
What are the success rates with donor eggs in women over 40?
With donor eggs, the chances of getting pregnant stand at 50-70% per cycle for women in their forties. It should be kept in mind that uterine receptivity might decline with advanced age. The reasons behind it might include biochemical and/or molecular aberrations of the endometrial lining, incidence of pathological conditions in the uterus (e.g. polyps, myomas...), hypertension, etc.
How can I prepare for IVF with donor eggs?
From the medical point of view, the recipient has to get her body ready to receive the embryo that has been created using donor eggs in order to maximize the chances of implantation.
If fresh donor eggs are used, then synchronization between the cycles of the donor and the recipient is required. Inversely, this step is not needed when frozen donor eggs are used.
The recipient has to prepare her body for donor-egg IVF by means of endometrial preparation, which makes the uterus to grow its lining so that it is prepared for the embryo to implant successfully after the transfer (ET). To this end, the patient has to follow a strict drug protocol.
Why does donor-egg IVF fail?
Several complications not necessarily related to egg quality can lead to IVF failure or the impossibility to carry the pregnancy to term in spite of having used donor eggs, including:
- Genetic abnormalities, which might lead to embryonic arrest at any point of embryo development
- Uterine alterations that might prevent the embryo from continuing its development and cause the woman to miscarry
- Implantation failure due to poor endometrial receptivity
Can you get pregnant with donor eggs after menopause?
Yes, it is possible to have a baby after menopause, a phenomenon known as postmenopausal pregnancy. Menopause is defined as the cessation of menstruation, which means the loss of ovarian activity. However, this does not affect the uterus, which is still functional, and able to carry a pregnancy. This is perfectly possible with either donor eggs from a young girl, the woman's own previously frozen eggs, or the couple's frozen embryos, if any.
Do babies from egg donation share genes with the birth mother?
Egg donor babies do not share the genetic load of the birth mother, but that of the egg donor, who is in fact the biological mother.
Nevertheless, recent studies have shown that recipients of donor eggs still pass some traits of their DNA through a phenomenon called epigenetics, a branch of Biology that studies the influence of a person's lifestyle on who he or she is, regardless of the gene expression.
So, factors such as the mother's diet during pregnancy could affect the development of the baby-to-be's gene expression.
If I use donor eggs, will the baby be mine?
Absolutely. Having a child is not only about sharing your DNA with him or her, but about educating, bringing up and enjoying life together as a family. Women who become mothers via egg donation love the baby exactly as any other female who got pregnant naturally with her own eggs would do. Having a child, no matter how you do it, is one of the most gratifying and rewarding experiences in life.
So, those women who are afraid of developing feelings of regrets once pregnant or after the birth of the child should know that this idea will disappear eventually.
How successful is IVF with donor eggs?
In general, the use of donor eggs makes an IVF treatment more likely to succeed, as the oocytes have been donated by young, healthy girls who enjoy a good ovarian reserve, features that make the quality of the eggs they produce optimal.
In comparison, if the normal pregnancy rate of IVF with own eggs stands at 35-34% on average, with donor eggs it increases to up to 55-63% approximately. These figures, however, depend on the uterine receptivity of the patient.
Visit the following article to learn more: Pregnancy success rates with donor eggs.
What are the miscarriage rates with donor eggs?
While in women younger than 45, the implantation rate is 45% on average, it drops to 35% in women from the 45-50 age group. Subsequently, the miscarriage rates increase with age in spite of using donor eggs: while they are less than 10% when the woman is 45 or less, they stand at 16% on average for women over 45. As explained above, a decline in endometrial receptivity is usually the reason behind this.
Can I use donor eggs from my sister?
It depends on the country where the process is taking place. In the United States, for instance, the answer to this question would be yes, as egg donor recipients can choose a known, semi-known, or anonymous donor depending on their preferences.
In Spain, Cyprus, Ukraine, the Czech Republic, etc., donors must remain anonymous by law. In the UK, since April 2005, anonymous are not required to be anonymous in accordance with the HFE Act. All donor-conceived children have the chance to know the identity of their donor if they wish to after turning 18.
Are you interested in learning more about this? Do not miss this article: Egg donation to a family member.
How can recipients cope with feelings of regret after using donor eggs?
The loss of one's own genetics is a dramatic step in many women's lives. The good news is that grieving the use of one's own egg cells is a normal part of the process, and many women understand that parenting is not 100% about genetics after a few months.
Remember that the donor may be the genetic DNA source, but she is not the mother. You are the one who is going to be a mom, regardless of whether it is a donor-conceived or biological child.
More info here: Telling children about their conception by gamete or embryo donation.
What are the most common pregnancy symptoms with donor eggs?
Firstly, it should be noted that, when a woman gets pregnant using donated ova, pregnancy develops as any normal, natural pregnancy would do. However, the symptoms can vary a little bit due to the medications egg donor recipients have to take. In short, nausea and vomiting, frequent urination, exhaustion, extreme hunger or loss of appetite, heightened sense of smell, etc., among others, are the most common early pregnancy symptoms.
See also: Pregnancy symptoms after DE-IVF.
What is the relationship between epigenetics and egg donation?
Epigenetics is the study of physiological phenotypic characteristics in babies that result from environmental factors. Such variations have an influence on how cells express genes.
In this sense, women who regret having used donor eggs because they do not share their genetic expression with the baby should know that, during pregnancy, the metabolism of the pregnant woman may have an influence on the baby's future behavioral patterns.
Does a baby conceived via donor eggs resemble birth mom?
Keeping in mind that egg donors should be compatible with recipients, so that they share certain characteristics such as the hair, eye, and skin color, ethnicity, height, etc., the donor-conceived baby will share certain physical traits with her.
I used donor eggs, when should I tell my child?
Deciding when to tell your child depends on your preferences, though experts are in favor of disclosure at some point in the child's life. Telling earlier may help them absorb the information more easily over time.
Suggested for you
Once a pregnancy is achieved through egg donation, the gestation evolves in the same way as a pregnancy with one's own eggs. The woman may present the same symptoms and the pregnancy follow-up is also the same. You can read more about this here: Having a Baby through Egg Donation - Early Pregnancy Signs.
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
FAQs from users: 'When is egg donation required?', 'How does Donor egg IVF work?', 'How many IVF cycles should you do before using donor eggs?', 'What are the risks of egg donation?', 'Donor-egg IVF vs. adoption, which one is better?', 'If I use donor eggs, will the baby look like me?', 'Does a donor egg have my DNA?', 'What are the success rates with donor eggs in women over 40?', 'How can I prepare for IVF with donor eggs?', 'Why does donor-egg IVF fail?', 'Can you get pregnant with donor eggs after menopause?', 'Do babies from egg donation share genes with the birth mother?', 'If I use donor eggs, will the baby be mine?', 'How successful is IVF with donor eggs?', 'What are the miscarriage rates with donor eggs?', 'Can I use donor eggs from my sister?', 'How can recipients cope with feelings of regret after using donor eggs?', 'What are the most common pregnancy symptoms with donor eggs?', 'What is the relationship between epigenetics and egg donation?', 'Does a baby conceived via donor eggs resemble birth mom?' and 'I used donor eggs, when should I tell my child?'.
Authors and contributors










How old is the cut off for egg donation? I have 4 kids. I’m very fertile.
Hello Trac,
It depends on the country you’re interested in. Each country has its own regulations on egg donation, and the age factor may vary. Can I ask in which one are you interested?
Regards
Ladies, me and my boyfriend have decided to try egg donation abroad, have any of you experienced that? We’re considering Ukraine, Czech Republic and Spain to date, but haven’t made made our mind up yet… Any advice?
Hello bOOba,
If you’re interested in traveling abroad for egg donation, that’s good news, because we’ve created a Calculator especially for patients in your situation. It’s very easy to complete, and will only take you a few minutes. After filling out a private questionnaire to let us know about your situation. Most importantly, it’s free. Once you finish the questionnaire, you will receive detailed estimates from different fertility clinics according to the options you’ve chosen (e.g. destinations of your preference, family type, situation, etc.). Just click here: Calculator.
I hope this helps and you could share your experience with us!
Regards
Hi there,
I’m 45, have been through 2 unsuccessful IVF cycles with own eggs and now I’ve been advised to use donor eggs because of my advanced age which is kinda upsetting but i’ve to face reality. today i’m ready to accept this path mainly because my niece has offered to be my egg donor, she’s 23, has one kid of her own. i think there would be some kind of family connection between me and the baby if i accept my niece’s eggs rather than those of an anonymous donor, what do ya think? i feel i have to do this, but at the same time i’m rather scared… of course, we would tell our son or daughter about his/her origins early because otherwise keeping that secret would kill me.
Please, share your experiences or opinions on this. That would be very helpful.
Thank you very much, this article’s been so helpful!
Dear Elsa,
Using a family member as your egg donor, whether she’s your sister, cousin or niece, is fine as long as both of you accept it and are sure you want to actually do it. Otherwise, my advice is that you use an anonymous donor. I assume you’re a resident in a country where this is possible, such as the United States, aren’t you?
Take a look at the following post for more information on intrafamilial egg donation: Egg donation to a family member for IVF.
I hope this helps,
Best of luck!
hey there! I will share my friend’s experience with you. She used an unknown donor’s eggs and very much satisfied with the results she had both the times. See, if you use your own niece’s eggs, that tells you that your kid will have his/her cousin as their mother biologically and that will make them awkward. Also, not only for them but also for you won’t you think that your niece who donates would be around you guys whole your life and you sometimes would become insecure of them that they may own your child although this procedure is contract based, still the inner feelings never follow contracts.So it is better to have donor eggs.For that the clinics have their own donors, you may choose the donor of your own choice and traits you have many options don’t make things awkward for your soon to be child.Good Luck!
Hello, I have a diagnosis of endometriosis, so I was wondering if donor eggs could be appropriate for me. To be precise, I’ve stage 3 endometriosis, and have done 2 artificial insemination and 3 IVF cycles previously with no luck. What do u think ladies?
Hello Anne-Marie,
Endometriosis is not usually a reason for using donor eggs, as it does not affect egg production in principle. However, if you’ve been struggling with endometriosis for a long time, egg quality might have been compromised due to the environment that endometriosis generates around the ovary. Also, if your age is not adequate for getting a natural pregnancy, and after various failed IVF attempts, then using donor eggs could be an option for you. The most severe cases of endometriosis (e.g. stage 4) often require surrogacy, as the patient is unable to carry a pregnancy to term.
I hope this helps,
Best
Hi i’m going through ivf egg donation. i’m post 16 day today yesterday i had a test nd my hcg level was 647.. i had my transfer on 24th feb .. i’m tensed about my sonography date is on 24th of march. is everything gonna be alright as i’m not having any symptoms now…?
Dear savita,
As long as your hCG levels are doubling every 48 hours, everything should be fine. In fact, your hCG levels are a bit high keeping in mind that you’re not 4 weeks yet. As for the fact that you don’t have symptoms at all, it’s not a concerning issue. Some women do not have any pregnancy symptoms, and it doesn’t mean that there’s something wrong.
I hope this helps,
Best
Ty☺️
Only 1 embryo was transferred..