The cervix is the lower part of the uterus and the channel for sperm to enter the uterine cavity. Due to its location and structure, it can act as a barrier to the entry of bacteria and pathogens.
The cervix measures between 3 to 4 cm in length and 2.5 cm in diameter. However, at the time of delivery it may undergo an increase of up to 10 cm in the process of dilatation.
Cervical mucus or cervical mucus is a secretion produced inside the cervix. This mucus usually occurs approximately 5 days before ovulation and its appearance indicates to the woman that she is in her fertile period and, therefore, can become pregnant.
In this article, we will see the function of cervical mucus, and we will analyze the causes that generate abnormalities in the cervical mucus.
Provided below is an index with the 8 points we are going to expand on in this article.
- 1.
- 2.
- 2.1.
- 2.2.
- 2.3.
- 2.4.
- 2.5.
- 3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 5.
- 6.
- 7.
- 8.
What is uterine mucus used for?
The different hormones of the female menstrual cycle produce changes in the consistency and color of the cervical mucus.
The mucus has a thick, white texture that becomes lighter and more abundant as the days of ovulation approach. As the day approaches, the mucus changes its structure and becomes more fluid and elastic. These modifications facilitate and allow the ascent of spermatozoa through the cervix.
This versatility in the structural change of the cervical mucus gives the cervix a function as a biological custom , allowing the passage of spermatozoa at certain times of the menstrual cycle and not at others.
Therefore, its low quality, excessive viscosity, or small quantity can constitute a factor of female sterility by being an obstacle to the passage of spermatozoa.
Causes of cervical mucus abnormalities
There are some problems related to cervical mucus that can cause secondary infertility in women. These alterations in the cervical mucus are collected under the name of hostile cervical mucus and all these causes are based on a deficiency in the mucus-semen interaction.
Low estrogen levels
Estrogen is the hormone responsible for producing the changes necessary for the mucus to become abundant, elastic, and permeable to sperm. If the woman does not have sufficient estrogen levels, she will have scanty and inelastic mucus:
- Deficiencies in hormone levels
- changes in mucus structure and quantity in the days prior to ovulation are due to the elevated estrogen levels that occur during this phase of the cycle. During ovulation, the mucus has a fluid and elastic structure reminiscent of egg white. If estrogen levels are insufficient, the mucus will not have the structure and fluidity necessary to allow sperm to pass into the uterine cavity.
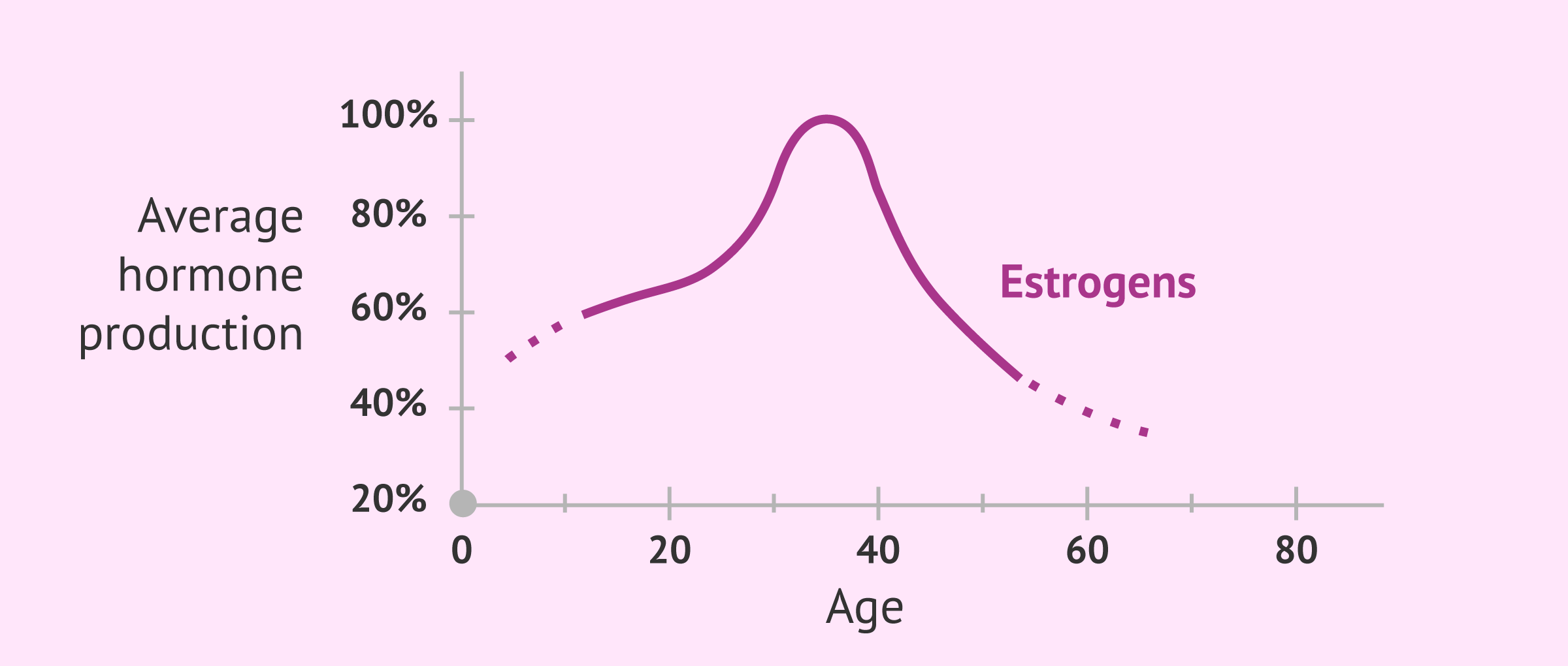
- Age
- during a woman's fertile life, her hormonal cycles and cervical mucus undergo significant changes. In the first stage of childbearing age, the quality of cervical mucus at the time of ovulation is much more watery and can last up to 5 days. As the woman's age advances, these days when optimal mucus is present for fertilization are reduced, and with them the options for achieving pregnancy.
On the other hand, women in menopause have a compact and inelastic cervical mucus. In addition, many of them have problems of vaginal dryness and irritation due to deficient lubrication of the cervical secretory glands.
These hormonal changes, which are detected throughout a woman's fertile life, influence the quality of the mucus. As a woman ages, her sex hormones decline. As we have seen before, this decrease in female hormones has an impact on cervical mucus.
Inflammations in the cervix area
Sexually transmitted infections such as Chlamydia or Gonorrhea can cause inflammation in the cells of the cervix. This inflammation can cause the cells to become altered and increase the number of leukocytes (white blood cells of the immune system) in the affected area. As a result, this infection can cause problems in the passage of sperm through the cervical canal.
Other bacterial infections may cause discomfort and pain in the affected area. In addition, the patient may have changes in the color and odor of her cervical mucus that may alert her to the presence of infection. This type of anomaly can produce cervicitis, a type of pathology in the cervical area that can, among many other things, alter the normal state of the mucus.
Human papillomavirus (HPV) is a sexually transmitted infection characterized by different strains of the virus with different symptomatology. Some strains of this virus can produce genital warts in both men and women.
Other much more aggressive strains of this virus can go unnoticed in the external sex organs but produce cervical cancer. This is why the treatment in cases where the infection is very advanced is surgery of the affected area. Among the most common surgical treatments performed in the cervical area due to HPV is conification, which is based on the removal of the first layers of the cervical mucosa affected by HPV. This intervention may alter mucocervical segregation.
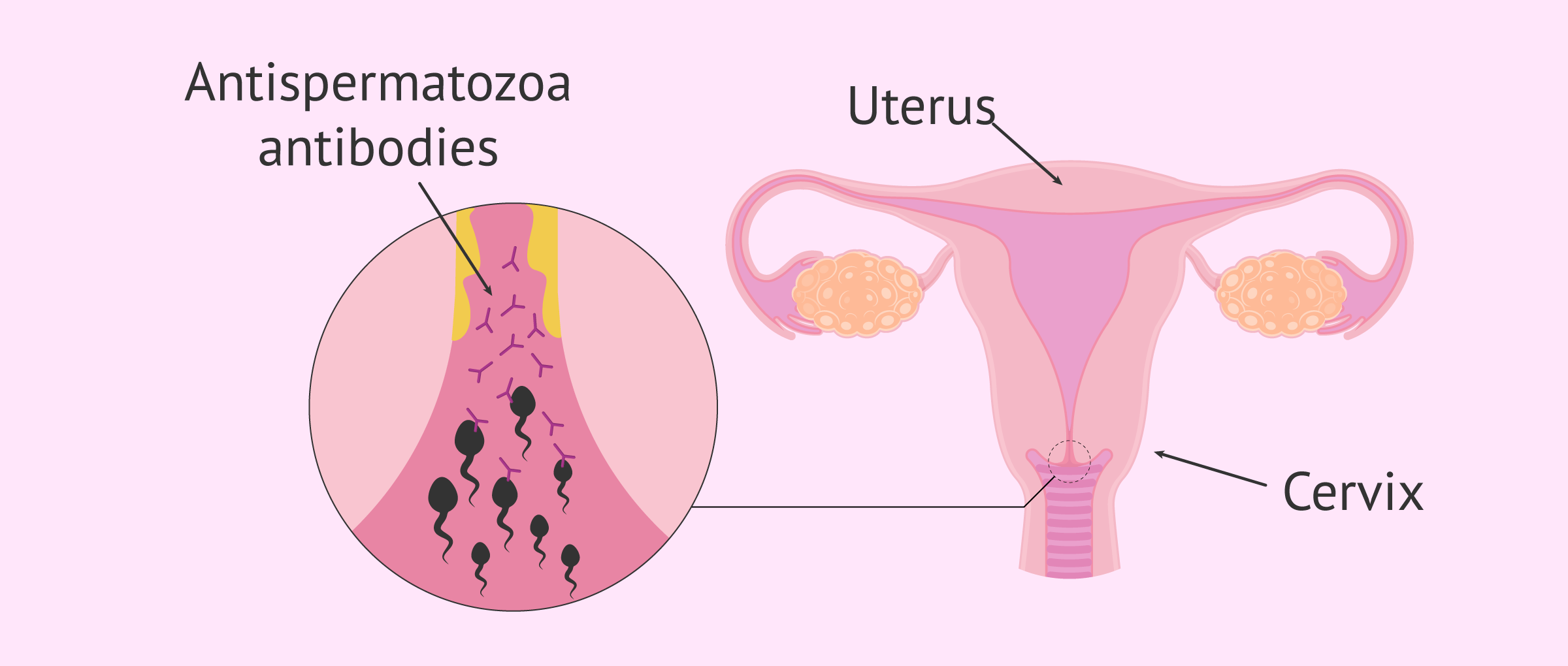
Occurrence of antisperm antibodies in the mucus
Antibodies are small molecules that act as the body's protective agents. These antibodies are created by the immune system to detect and defend the body against foreign particles, such as viruses and bacteria. Once the invading cell is located, it will be eliminated.
An abnormality in the functioning of the human body's defense system can detect sperm as invading and dangerous cells. For this reason, the body can create antisperm antibodies that bind to the male cell so that it is eliminated.
These antisperm antibodies can be found in the cervical mucus of some women with this type of immune problem. As a result, the sperm does not manage to pass through the cervical canal, as they are attacked by the defense system of the woman's organism.
Assisted procreation, as any other medical treatment, requires that you rely on the professionalism of the doctors and staff of the clinic you choose. Obviously, each clinic is different. Get now your Fertility Report, which will select several clinics for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
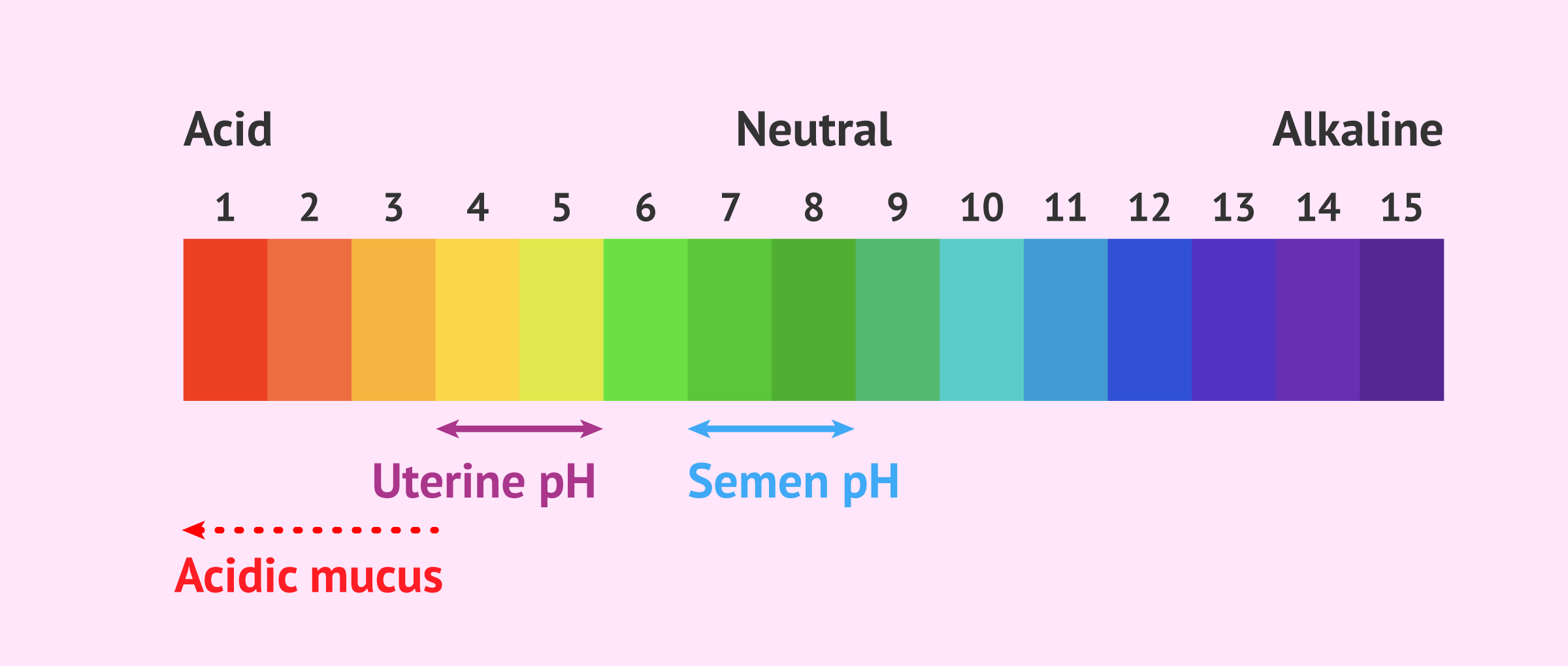
Acid mucus
Under normal conditions, semen has a pH of about 7. This neutral environment allows spermatozoa to survive in it for long periods of time.
However, the female uterus has a much more acidic pH, which is around 4.5. This acidic environment naturally found in the female tract makes it difficult for sperm to survive.
In conditions where the cervical mucus is altered by having a pH that is too acidic, it can create an environment that is too hostile for sperm to survive in.
Side effects of certain medications
Some drugs can have an impact on the quality of cervical mucus. The best known, because of their impact on the cervix, are the following:
- Antihistamines and cold medicines
- these medications are intended to reduce nasal mucus secretions. However, the secretory cells of the cervix may be affected by this type of medication. In spite of this, its relationship with infertility is in between said, since its use is reduced to short periods of time. It can be said that, despite the reduction of lubrication in the female tract, these drugs do not have a great impact on female fertility.
- Antidepressants
- can make the cervix drier and reduce mucus secretion. In addition, its use can also reduce libido and, with it, the frequency and quality of sexual intercourse.
- Clomiphene citrate
- this drug that is so frequently used in ovulation induction treatments can cause dryness of the cervix if used in very high doses. Assisted reproduction experts indicate that the benefit of this drug in anovulatory women is greater than the harm caused by the reduction of cervical mucus. Moreover, this problem can be solved by adjusting the treatment to lower doses.
Treatments for cervical mucus problems
Treatments to improve cervical mucus are as varied as the causes that alter it, such as:
- Insufficient estrogen supply can be addressed by supplementing the patient with medications containing estrogen variants. This promotes the production of mucus.
- Changes due to vaginal or cervical infections should be treated with antibiotics or antifungals that restore the proper functioning of the cervical secretory cells.
- The low secretions that some women have, can be solved with the help of lubricants to alleviate the discomfort generated during sexual intercourse. It should be noted that if there is a sexually transmitted infection or antisperm antibodies, it is recommended that they see a gynecologist help them solve these problems.
- The presence of hostile cervical mucus due to acidic mucus or antisperm antibodies, which may kill male cells. In these cases, a postcoital test (PCT) is recommended. This method observes the state of the spermatozoa in the mucus and whether or not they are able to survive. It also analyzes the characteristics of the mucus.
- The presence of antisperm antibodies and other types of hostile mucus that prevent pregnancy naturally can be overcome by artificial intrauterine insemination.
In intrauterine artificial insemination, the sperm are placed directly into the cavity of the uterus, precisely so that they do not have to pass through the cervical canal and cervical mucus.
FAQs from users
Are there any alterations in a woman's cervical mucus that may affect her fertility?
There has been talk that certain configurations of cervical mucus either by density or by acidity of the medium could affect fertility. The reality is that at present there is no evidence that these parameters can significantly affect the possibility of having a pregnancy.
In any case, if in specific cases these parameters could affect the couple's fertility, they would be very easily solved with the fertility techniques that are currently used, either Artificial Insemination or In Vitro Fertilization, so there are no major studies on the subject.
Can alterations in the cervical mucus lead to female infertility?
Yes, alterations in the cervical mucus can are a common cause of female infertility. The cervical mucus is a secretion produced before ovulation and it disappears after the woman ovulates. It has a sticky texture, and its mission is to pave the way for sperm. It is, in fact, a good indicator of female fertility.
How should cervical mucus be during fertile days?
There are birth control methods that are based on the observation of cervical mucus precisely because it varies greatly in each phase of the cycle.
At the end of the menstrual period, the cervical mucus is thin and clear (or whitish). Normally in the ovulatory phase (in the days immediately before ovulation and one day after ovulation) its characteristics change to facilitate the entry of sperm into the uterus and fertilization of the egg.
On those days it is usually whiter and above all it changes consistency, it is less dense and more filamentous. This can help to identify the most fertile days (which are those preceding ovulation up to 24 hours after it has taken place).
Can I get pregnant if I have hostile cervical mucus?
Alterations in the cervical mucus, due to its quantity, structure or quality can make it difficult for the sperm to reach the egg. Therefore, this problem can be a cause of infertility.
A solution to all these problems generated in the cervix can be artificial insemination. Through this technique, the fastest and best quality sperm are selected in the laboratory and placed inside the uterine cavity. In this way, the passage of sperm through the cervix and hostile mucus is avoided.
What does the fern leaf-shaped mucus mean?
This definition refers to the pattern left by the spreading and drying of the mucus in the fertile stage, i.e., the days close to ovulation.
This fern leaf-shaped pattern creates channels through which the sperm can pass. The passage of male cells through these ducts is essential for their capacitation and activation.
Recommended readings
If you want to read more about the cervical factor, we recommend the article: Cervical factor: female sterility due to cervical abnormalities.
Cervical mucus is changeable. Its structure and fluidity vary depending on the time of the woman's menstrual cycle. In this way, the woman may be able to detect and predict the most fertile days of her cycle. If you want to know more about the mucus of the cervix and how to detect your ovulation period be sure to read the following article: How is the cervical mucus in the fertile period?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Cortes E, Montero B, Yuguero O. Chlamydia trachomatis Infection Could Be a Risk Factor for Infertility in Women: A Prospective Descriptive Study. Cureus. 2022 Oct 26;14(10):e30697. doi: 10.7759/cureus.30697. PMID: 36457637; PMCID: PMC9704856. (View)
Helmerhorst FM, Van Vliet HA, Gornas T, Finken MJ, Grimes DA. Intra-uterine insemination versus timed intercourse for cervical hostility in subfertile couples. Cochrane Database Syst Rev. 2005 Oct 19;2005(4):CD002809. doi: 10.1002/14651858.CD002809.pub2. PMID: 16235303; PMCID: PMC6599852. (View)
Hur CE, Goldberg JM. Laparoscopic transfundal approach to cervical dilation: a novel treatment for cervical stenosis and cervical factor infertility. Fertil Steril. 2024 May;121(5):890-891. doi: 10.1016/j.fertnstert.2024.02.005. Epub 2024 Feb 9. PMID: 38342370. (View)
Jose-Miller AB, Boyden JW, Frey KA. Infertility. Am Fam Physician. 2007 Mar 15;75(6):849-56. PMID: 17390595. (View)
Kossakowski J, Stephenson M, Smith H. Intrauterine insemination with husband's sperm: comparison of pregnancy rates in couples with cervical factor, male factor, immunological factor and idiopathic infertility. Aust N Z J Obstet Gynaecol. 1993 May;33(2):183-6. doi: 10.1111/j.1479-828x.1993.tb02389.x. PMID: 8216122. (View)
Najmabadi S, Schliep KC, Simonsen SE, Porucznik CA, Egger MJ, Stanford JB. Cervical mucus patterns and the fertile window in women without known subfertility: a pooled analysis of three cohorts. Hum Reprod. 2021 Jun 18;36(7):1784-1795. doi: 10.1093/humrep/deab049. PMID: 33990841; PMCID: PMC8487651. (View)
Poon WW, McCoshen JA. Variances in mucus architecture as a cause of cervical factor infertility. Fertil Steril. 1985 Sep;44(3):361-5. doi: 10.1016/s0015-0282(16)48861-8. PMID: 4029424. (View)
Scholten I, Moolenaar LM, Gianotten J, van der Veen F, Hompes PG, Mol BW, Steures P. Long term outcome in subfertile couples with isolated cervical factor. Eur J Obstet Gynecol Reprod Biol. 2013 Oct;170(2):429-33. doi: 10.1016/j.ejogrb.2013.06.042. Epub 2013 Aug 3. PMID: 23921361. (View)
Scott JZ, Nakamura RM, Mutch J, Davajan V. The cervical factor in infertility: diagnosis and treatment. Fertil Steril. 1977 Dec;28(12):1289-94. doi: 10.1016/s0015-0282(16)42971-7. PMID: 590536. (View)
FAQs from users: 'Are there any alterations in a woman's cervical mucus that may affect her fertility?', 'Can alterations in the cervical mucus lead to female infertility?', 'How should cervical mucus be during fertile days?', 'Can I get pregnant if I have hostile cervical mucus?' and 'What does the fern leaf-shaped mucus mean?'.
Authors and contributors
More information about Cristina Algarra Goosman











Hi, there are times in my cycle that I have a lot of vaginal discharge, I am worried that it is not normal, it has no odor and is transparent.
Hello Myldred,
The amount, as well as the color of cervical mucus, can vary throughout the cycle. If it is clear and odorless you should not worry. The amount also varies throughout the cycle, if it does not cause you a problem or discomfort you should not worry. If it is an impediment you could go to the doctor to see if he/she can help you.
I hope I have helped you,
Best regards
Hi, my cervical mucus has always been clear or at many times a little whitish. Since a few days ago I have had yellowish secretions and my vagina itches, I don’t know what’s wrong with me, what should I do?
Hello kamie,
Clear or even whitish color is normal for cervical mucus, on the contrary, yellowish cervical mucus denotes the presence of some bacterial infection. Especially if it is accompanied by itching or burning.
I recommend that you go to your doctor so that he/she can prescribe an antibiotic to eliminate the infection and finally restore your vaginal wellness.
I hope I have helped you
Best regards