Implantation failure refers to a situation in which a woman wishes to become pregnant but she is unable to fulfill her dream despite having unprotected sexual intercourse on a regular basis.
The main problems these couples face is that they actually don't know if theirs is a case of Repeated Implantation Failure (RIF), or if their gametes are actually unable to meet each other and subsequently fertilization never occurs.
A diagnosis of RIF can only be confirmed after several failed IVF attempts, which is to say if an embryo has been cultured and placed into the uterus of the mother-to-be but has not lead to an ongoing pregnancy.
Provided below is an index with the 10 points we are going to expand on in this article.
- 1.
- 2.
- 3.
- 3.1.
- 3.2.
- 3.3.
- 4.
- 4.1.
- 4.2.
- 4.3.
- 4.4.
- 4.5.
- 4.6.
- 4.7.
- 5.
- 6.
- 6.1.
- 6.2.
- 6.3.
- 6.4.
- 6.5.
- 6.6.
- 6.7.
- 6.8.
- 6.9.
- 7.
- 8.
- 9.
- 10.
What is embryo implantation?
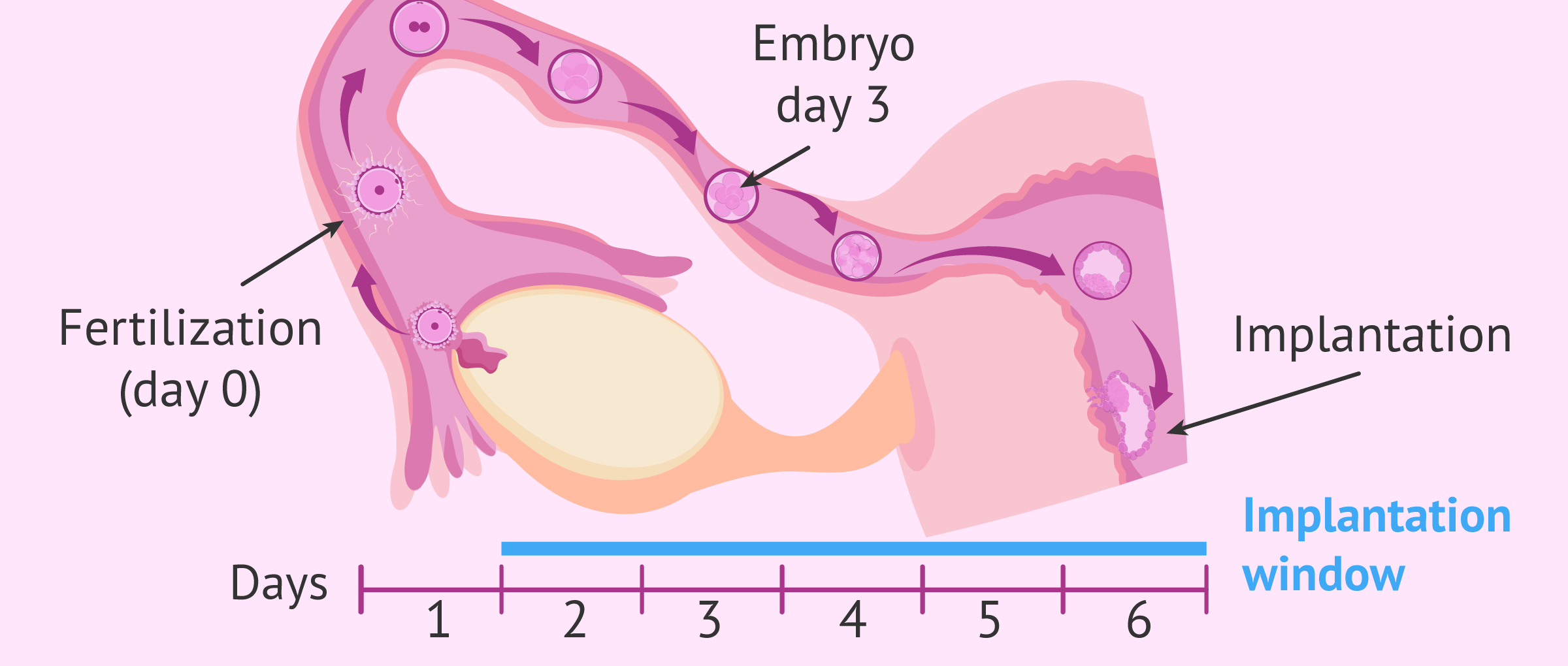
Implantation is the process whereby the embryo attaches to the uterine lining during the implantation window of the woman. It takes place within 6-7 days after fertilization, thereby giving rise to a new pregnancy.
The implantation window of females is a period of 2 to 6 days during which the uterus is receptive for implantation, which is to say, it has the optimum conditions to receive the embryos and allow them to attach. The ideal characteristics of the endometrium to facilitate embryo implantation are a thickness of 7-9 mm and a trilaminar appearance.
The embryo implantation process can be split into two phases:
- Pre-implantation stage
- It encompasses the preparation of the endometrial lining, early embryonic cleavage, and apposition.
- Implantation stage
- Once at blastocyst stage, the embryo attaches to the uterine lining.
As one shall see, embryo implantation is a challenging process that requires a healthy embryo and a receptive uterus in order for synchronization between them to occur effectively.
Implantation failure signs
We can begin to suspect implantation failure has taken place when a patient hasn't achieved an ongoing pregnancy after 3 IVF cycles using own eggs, or after 2 donor-egg cycles, as long as:
- Only good quality embryos were transferred
- No technical difficulties were encountered during the embryo transfer procedure
- No evidence of uterine abnormalities exists
In these cases, we recommend that patients consider undergoing other treatment options in order to increase implantation rates.
What causes implantation problems?
There exist several causes that may lead to embryo implantation failure, either related to the embryo, the uterine lining of the patient, or specific diseases.
Each of the possible causes of implementation failures is described below.
Embryonic causes
They are fundamentally due to genetic alterations in the embryo or the reproductive cells of the parents (the egg and/or sperm).
Also, some embryos present abnormalities in the zona pellucida (ZP), which prevent them from breaking out of the ZP and detaching from it.
The zona pellucida (ZP) is a glycoprotein sphere that surrounds the egg cell. It can be found around the embryo following fertilization as well.
Uterine causes
There are certain factors that decrease endometrial receptivity, such as those mentioned below:
- Chronic asymptomatic infections of the endometrium (endometritis).
- Endocavitary alterations such as polyps, certain fibroids, septa, or adhesions.
- Anomalies in the implantation window, such as its displacement before or after the 5-7 days post-ovulation.
Antibiotics and probiotics may be necessary to treat endometritis. On the other hand, some uterine alterations can be resolved using techniques such as surgical hysteroscopy. Additionally, there are tests, such as the ERA test, that can determine if the implantation window is displaced and the best time to perform the embryo transfer.
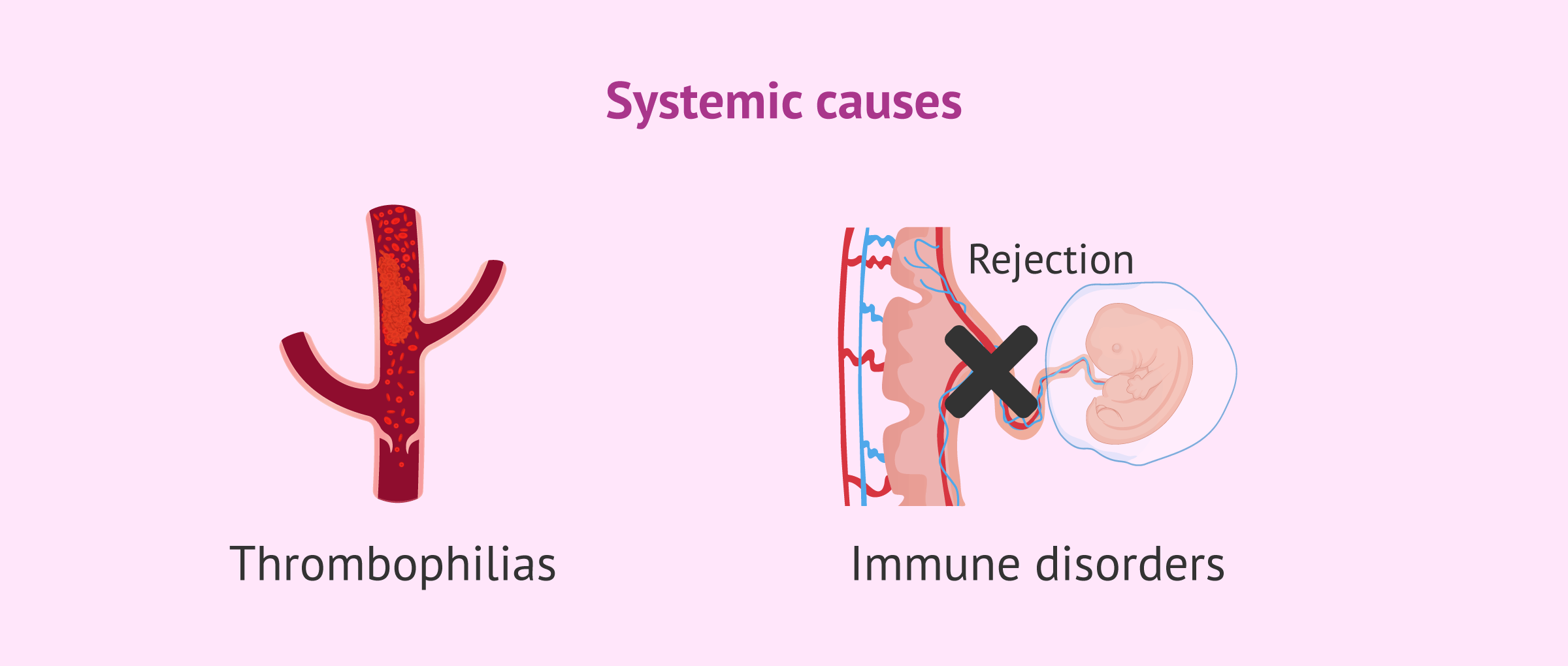
Systemic causes
Occasionally, the problems causing implantation failure stem from alterations in the functioning of systems not directly related to the reproductive system, such as:
- Thrombophilias
- alterations in blood clotting processes. Despite being a cause of implantation failure, coagulation problems can also lead to recurrent miscarriages.
- Immune system disorders
- rejection of the embryo by identifying it as foreign. An example would be antiphospholipid syndrome, as the woman's immune system is highly active and damages the embryonic cells. This causes the rejection of the embryo's implantation in the woman's uterus.
The exact mechanism by which these causes affect embryo implantation is unknown, but they are factors to be considered in order to prescribe appropriate treatment and try to improve the possibility of embryo implantation.
Solutions for Implantation Failure
The possible treatments or ways to address embryonic implantation failure are listed in the following sections.
Extended culture to blastocyst stage
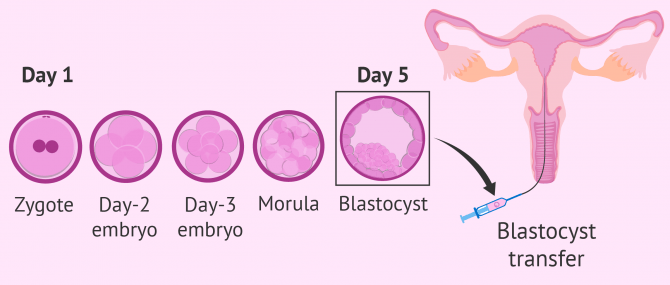
In in vitro fertilization (IVF), embryologists evaluate the early development of the obtained embryos in the laboratory. It is possible to observe the entire development until the embryo reaches the blastocyst stage (day 5 or day 6) or, conversely, to see if the embryo stops its development at an earlier stage.
Extending the culture to the blastocyst stage allows for better embryo selection and, additionally, since the transfer will take place on day 5, there will be better embryo-endometrial synchronization.
Learn more: What Is Blastocyst Culture & Transfer?
Preimplantation Genetic Diagnosis (PGD)
The chances for implantation failure increase with advanced maternal age due to the presence of an increased number of chromosomal abnormalities in the egg cell. Nowadays, it is possible to select healthy embryos in the laboratory thanks to the use of Preimplantation Genetic Diagnosis (PGD), now known as Preimplantation Genetic Testing (PGT).
This complementary technique consists of the genetic analysis of the embryo, based on an embryo biopsy, without this affecting its development.
See this for more: What Is PGD or Preimplantation Genetic Diagnosis?
Heparin administration
Some women with a risk of thrombophilia are prescribed aspirin and heparin, an option that is usually very effective to deal with RIF. This treatment should be started before pregnancy and continued until the baby is born.
Heparin is a natural anticoagulant (blood thinner) that can be found in various tissues of the human body.
Endometrial Receptivity Analysis (ERA)
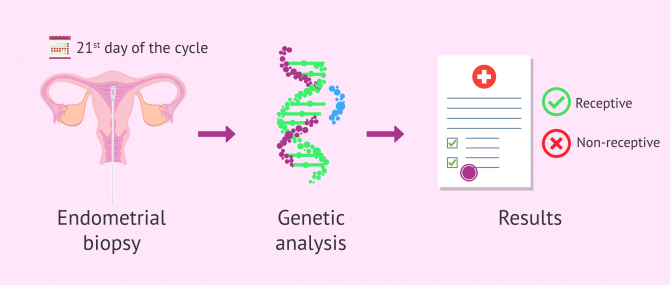
The Endometrial Receptivity Analysis (ERA), also called Endometrial Receptivity Array, is a molecular diagnostic tool that allows us to examine the expression of a set of genes that are closely linked to the endometrium. In other words, ERA provides us with information about endometrial receptivity with just a biopsy.
Moreover, ERA is able to detect abnormalities in the implantation window, if any. Should this be the cause, patients are recommended to opt for embryo vitrification. IVF embryo transfer can be postponed up until the moment when their endometrium is more receptive.
Related topic: Endometrial Receptivity Array (ERA): Procedure and Success Rates.
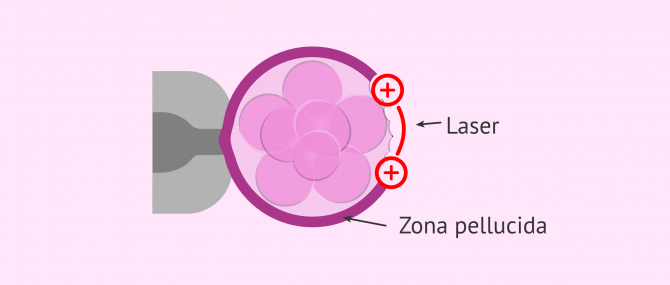
Assisted Hatching
With assisted hatching, the embryologist creates a small hole in the zona pellucida of the embryo through which the embryonic cells can hatch out.
This technique is highly effective because it allows the embryos with a thick zona pellucida to be able to implant. To give you an idea, when thickening is present in embryos, they resemble a flattened olive.
Get more information about this procedure here: Assisted Hatching Before Embryo Transfer.
Egg and sperm donation
Egg donation may be the best solution in cases of repeated implantation failure when the uterus and the endometrial lining are normal. Implantation rates are excellent in patients who use donor eggs, given that embryo quality is significantly higher.
Embryos created in the laboratory using eggs from young and healthy women are normally of good quality. This is the reason why egg donation IVF has higher success rates. Nevertheless, the characteristics of the woman's endometrium have to be considered as well when it comes to transferring the embryo into the uterus.
However, a diagnosis of a severe masculine factor in the male can also influence embryo implantation. Therefore, sperm donation IVF would be the best solution in these cases.
Surrogacy
When there are several unexplained implantation failures and none of the aforementioned solutions have been effective, the final possible option is to resort to surrogacy. In this case, it could be attempted using the woman's own eggs, provided it has been observed that they produce high-quality embryos.
However, surrogacy is not permitted and is illegal in Spain. Therefore, patients who wish to pursue this will need to travel to countries where surrogacy is recognized by their legislation.
More on this story: What Is Surrogacy & How Does It Work? – Everything You Should Know.
How to calculate the costs
The possible infertility treatment options to deal with recurrent implantation failure are expensive, especially if pregnancy is not achieved the first time.
In the case of IVF, the average cost of single cycle IVF packages ranges between $8,500 and $12,000. More often than not, this price range doesn't include the cost of fertility drugs, which add a considerable amount to this sum. PGD or ERA, if needed, are additional techniques that shoot up the price of IVF.
In case none of these options works and you decide to move on to donor eggs, a complete egg donation cycle typically costs $26,000 on average, which includes the donor's fee ($7,000 approximately) plus $400 for short-term medical insurance for the egg donor.
As regards surrogacy, it can cost up to $90,000-$130,000 or more, depending on the US state where it takes place and the particular circumstances of each case.
Should you think about going to a fertility clinic, it is important that you ask first for possible discounts should you undergo two or more cycles. Also, keep in mind which techniques are included in the initial budget in order to gain an idea of the overall costs you will have to face.
In order to know what costs you should expect, we recommend you this post as a guide: What are the average costs of IVF?
Assisted procreation, as any other medical treatment, requires that you rely on the professionalism of the doctors and staff of the clinic you choose. Obviously, each clinic is different. Get now your Fertility Report, which will select several clinics for you out of the pool of clinics that meet our strict quality criteria. Moreover, it will offer you a comparison between the fees and conditions each clinic offers in order for you to make a well informed choice.
FAQs from users
Does vitamin D affect embryo implantation?
Although traditionally only the role of vitamin D in bone health has been emphasized, its potential role in fertility is becoming increasingly important. This hormone has receptors throughout the body, including the ovary, endometrium, and placenta, and has been linked to reproductive and obstetric outcomes.
Studies have shown that optimal levels of vitamin D improve the chance of pregnancy. However, the mechanism by which the rate of gestation increases is not yet very clear.
In a study carried out on donor egg recipients, where it is assumed all the embryos will have a good quality, it was observed that those patients with correct vitamin D levels had a greater chance of becoming pregnant. However, in another study carried out with the transfer of euploid (chromosomally healthy) embryos, this effect was not observed. Thus, although the evidence seems to indicate that vitamin D does improve endometrial receptivity, its role is probably more complex than it appears at first glance.
Another possible mechanism by which vitamin D may increase pregnancy rates is by improving egg quality. Blood levels of vitamin D have been shown to be proportional to levels in follicular fluid, and it is believed that vitamin D may palliate ovarian aging, although it has not been possible to study it directly in eggs.
Do low progesterone levels cause implantation failure?
Yes. Progesterone has a key role in maturing the uterine lining for embryo implantation. Low levels of progesterone after ovulation (i.e. luteal phase deficiency) might lead to implantation failure.
At how many implantation failures do I know when it's time to resort to egg donation?
We speak of repeated implantation failure when pregnany has not occured after having transferred 10 or more embryos of good quality throughourt assisted reproductive treatments carried out by the patient, or when 3 or more embryo transfers have been carried out with embryos of good quality.
It takes two for implantation, the embryo and the endometrium. So it would be appropriate to assess both.
What are the main causes that hinder embryo implantation in an ART cycle?
There are several types of causes that can hinder the correct implantation of the embryo:
- Uterine problems. The presence of a uterine pathology can condition the implantation of the embryos. It is always a question of ruling out the existence of the same (polyps, myomas, intrauterine adhesions...) before carrying out a reproduction treatment.
- The intrinsic quality of the embryos transferred. Higher quality embryos are more likely to implant.
- Problems arising from the execution of assisted reproduction treatments. The clearest example is the significant elevation (more than 3000 pg/mL) of estradiol levels in the blood.
Which treatment is the most effective for a successfull embryo implantation?
The ideal treatment is the one that manages to generate good quality embryos, with no circumstances that diminish their chances of implantation. In addition, it is necessary to count on a correct transference of the same ones to the interior of the uterus.
It is important to point out that nowadays, due to the great advances in cryobiology (vitrification of oocytes and/or embryos), it has been achieved that the negative impact that the circumstances derived from controlled ovarian hyperstimulation can have is minor, given that the transfer of the embryos to a natural cycle can be deferred instead of transferring in circumstances of high levels of estrogens, a more physiological environment for embryo implantation and for which implantation in the human organism is designed.
Can implantation failures be avoided when performing PGD in a blastocyst transfer?
We speak of implantation failure when a patient has not achieved pregnancy after 3 cycles of IVF/ICSI with her eggs, or after 2 egg donation cycles,provided that good quality embryos have been transferred, there have been no technical problems during the embryo transfer and there are no obvious problems in the uterus.
One of the treatments for couples with implantation failure is preimplantation genetic diagnosis (PGD) or preimplantation genetic screening (PGS) to rule out chromosomal abnormalities. In these cases, embryos that do not present any chromosomal anomaly that could be the cause of the implantation failures would be transferred to the uterus, that is, it reduces the number of transfers of altered embryos and the number of transfers making the treatment more bearable without so many negatives, besides reducing abortion rates.
Why does implantation failure occur with donor eggs?
In spite of having high-quality embryos with a normal development rate, unfortunately some egg donor cycles fail when the uterus is not receptive. Implantation will never take place in a non-receptive uterus.
Do frozen embryos provoke implantation failure?
Not necessarily. The implantation rate of frozen embryos is similar to that of fresh embryos. The embryo vitrification process is well developed and safe, so it would not affect embryo viability.
I have several implantation failure behind me. Am I elegible for surrogacy?
No. Surrogacy is not legal in Spain under any circumstances. If surrogacy is necessary, patients will have to travel to a country where it is permitted by law.
Suggested for you
We have explained that implantation failure occurs after embryo transfer in IVF cycles. To learn more about this technique step by step, click here: What Is In Vitro Fertilization (IVF)? – Process, Cost & Success Rates.
To gain a much deeper insight on the process of implantation, we recommend that you visit the following post: What Is Embryo Implantation?
What are the earliest signs of embryo implantation? Get more info by clicking the following link: What Are the First Signs & Symptoms of Embryo Implantation?
Community and Support
At inviTRA we work to make monthly and rigorous information accessible to everyone. If this article has helped you, consider supporting us so we can continue accompanying more people on their journey to parenthood.
References
Bashiri A, Halper KI, Orvieto R. Recurrent Implantation Failure-update overview on etiology, diagnosis, treatment and future directions. Reprod Biol Endocrinol. 2018 Dec 5;16(1):121. doi: 10.1186/s12958-018-0414-2. PMID: 30518389; PMCID: PMC6282265. (View)
Benkhalifa M, Joao F, Duval C, Montjean D, Bouricha M, Cabry R, Bélanger MC, Bahri H, Miron P, Benkhalifa M. Endometrium Immunomodulation to Prevent Recurrent Implantation Failure in Assisted Reproductive Technology. Int J Mol Sci. 2022 Oct 24;23(21):12787. doi: 10.3390/ijms232112787. PMID: 36361577; PMCID: PMC9654171. (View)
Boivin J, Griffiths E, Venetis CA. Emotional distress in infertile women and failure of assisted reproductive technologies: meta-analysis of prospective psychosocial studies. BMJ. 2011 Feb 23;342:d223. doi: 10.1136/bmj.d223. PMID: 21345903; PMCID: PMC3043530. (View)
Coughlan C, Ledger W, Wang Q, Liu F, Demirol A, Gurgan T, Cutting R, Ong K, Sallam H, Li TC. Recurrent implantation failure: definition and management. Reprod Biomed Online. 2014 Jan;28(1):14-38. doi: 10.1016/j.rbmo.2013.08.011. Epub 2013 Sep 14. PMID: 24269084. (View)
Franasiak JM, Alecsandru D, Forman EJ, Gemmell LC, Goldberg JM, Llarena N, Margolis C, Laven J, Schoenmakers S, Seli E. A review of the pathophysiology of recurrent implantation failure. Fertil Steril. 2021 Dec;116(6):1436-1448. doi: 10.1016/j.fertnstert.2021.09.014. Epub 2021 Oct 19. Erratum in: Fertil Steril. 2022 Mar;117(3):653. doi: 10.1016/j.fertnstert.2022.01.002. PMID: 34674825. (View)
He Y, Shi S, Su X, Chen G, Zhao X. Incidence of pregnancy outcomes among patients with recurrent implantation failure: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2025 Nov 10;25(1):1184. doi: 10.1186/s12884-025-08372-8. PMID: 41214571; PMCID: PMC12604203. (View)
Macklon NS. The true incidence of recurrent implantation failure. Curr Opin Obstet Gynecol. 2022 Jun 1;34(3):147-150. doi: 10.1097/GCO.0000000000000781. PMID: 35645013. (View)
Pantos K, Grigoriadis S, Maziotis E, Pistola K, Xystra P, Pantou A, Kokkali G, Pappas A, Lambropoulou M, Sfakianoudis K, Simopoulou M. The Role of Interleukins in Recurrent Implantation Failure: A Comprehensive Review of the Literature. Int J Mol Sci. 2022 Feb 16;23(4):2198. doi: 10.3390/ijms23042198. PMID: 35216313; PMCID: PMC8875813. (View)
Pirtea P, Scott RT Jr, de Ziegler D, Ayoubi JM. Recurrent implantation failure: how common is it? Curr Opin Obstet Gynecol. 2021 Jun 1;33(3):207-212. doi: 10.1097/GCO.0000000000000698. PMID: 33896917. (View)
Shaulov T, Sierra S, Sylvestre C. Recurrent implantation failure in IVF: A Canadian Fertility and Andrology Society Clinical Practice Guideline. Reprod Biomed Online. 2020 Nov;41(5):819-833. doi: 10.1016/j.rbmo.2020.08.007. Epub 2020 Aug 20. PMID: 32962928. (View)
Su W, Gong C, Zhong H, Yang H, Chen Y, Wu X, Jin J, Xi H, Zhao J. Vaginal and endometrial microbiome dysbiosis associated with adverse embryo transfer outcomes. Reprod Biol Endocrinol. 2024 Aug 28;22(1):111. doi: 10.1186/s12958-024-01274-y. PMID: 39198832; PMCID: PMC11351450. (View)
(The writing group) for the participants to the 2022 Lugano RIF Workshop; Pirtea P, Cedars MI, Devine K, Ata B, Franasiak J, Racowsky C, Toner J, Scott RT, de Ziegler D, Barnhart KT. Recurrent implantation failure: reality or a statistical mirage?: Consensus statement from the July 1, 2022 Lugano Workshop on recurrent implantation failure. Fertil Steril. 2023 Jul;120(1):45-59. doi: 10.1016/j.fertnstert.2023.02.014. Epub 2023 Feb 22. PMID: 36822566. (View)
Wang Q, Sun Y, Fan R, Wang M, Ren C, Jiang A, Yang T. Role of inflammatory factors in the etiology and treatment of recurrent implantation failure. Reprod Biol. 2022 Dec;22(4):100698. doi: 10.1016/j.repbio.2022.100698. Epub 2022 Sep 23. PMID: 36162310. (View)
FAQs from users: 'Does vitamin D affect embryo implantation?', 'Do low progesterone levels cause implantation failure?', 'At how many implantation failures do I know when it's time to resort to egg donation?', 'What are the main causes that hinder embryo implantation in an ART cycle?', 'Which treatment is the most effective for a successfull embryo implantation?', 'Can implantation failures be avoided when performing PGD in a blastocyst transfer?', 'Why does implantation failure occur with donor eggs?', 'Do frozen embryos provoke implantation failure?' and 'I have several implantation failure behind me. Am I elegible for surrogacy?'.











After having two failed embryo implantation, my doctor told me to have an endometrial biopsy done. Does this hurt? How reliable is this procedure? We already have spent so much money, I want to make sure that this time everything goes well.
Good morning Maybebaby,
The ERA test is frequently used in women with implantation failure and offers very good results. It is not always the best solution since the causes of implantation failure are diverse, but above all it helps to know if the implantation window is displaced.
The endometrial biopsy is a simple practice that is performed in the same office without anesthesia. It might simply cause some discomfort when the cannula is inserted.
Hope this helps,
all the best.
How do I know if I suffer from implantation failure? I’m about to start my first IVF cycle but this article makes me a little insecure about the possible outcomes and worst case scenario.